Chapter 11 Applying psychological interventions in rheumatic disease
KEY POINTS
 The theories, research and professional practice approaches used by health psychologists provide a rich basis for the development of practical interventions for people with rheumatic disease that therapists can deliver
The theories, research and professional practice approaches used by health psychologists provide a rich basis for the development of practical interventions for people with rheumatic disease that therapists can deliver There are many internet resources with information on health psychology, health and rheumatic disease (see useful websites)
There are many internet resources with information on health psychology, health and rheumatic disease (see useful websites)INTRODUCTION
In this chapter we will consider how physiotherapists, occupational therapists, nurses and other allied health professionals benefit from understanding how psychological interventions can be applied to people with rheumatic disease. We will focus on cognitive-behavioural therapy (CBT) approaches you might consider applying and provide information about assessments of stress, illness perceptions and mood you can use in practice. The role of health psychologists in rheumatology was discussed in Chapter 1 and here we will also consider how they might add breadth to multidisciplinary teams (MDTs).
This volume is timely given the changing emphasis within the healthcare system, both in the UK and internationally. Health professionals are encouraged to promote self-care (or self-management) for patients with long-term conditions (Department of Health 2006). We will outline studies demonstrating the application of psychological theory and practice to facilitating self-management by enhancing concordance between patients and health professionals, building upon Chapter 5 (Biopsychosocial care) and chapter 6 (Patient education and self-management). A recent meta-analytic review by Dixon et al (2007) identified that psychosocial interventions boost active coping efforts people with arthritis engage in. These interventions improve anxiety, joint swelling, as well as depression, functional ability and self-efficacy over pain. We will explain some of these concepts, like self-efficacy and coping in more detail (see also Chs 5 & 6). Finally, we provide some examples of practical tools to foster self-motivated behaviour change and improve outcomes of people with rheumatic diseases.
STRESS AND CHRONIC ILLNESS
The idea of effective ‘coping’ is related to how much ‘stress’ the person feels under. So we need to define these concepts and consider the theoretical background they arise from (Box 11.1).
BOX 11.1 Frequently asked question: what is ‘stress’?
In the language of the modern day we use the words ‘stress’ or ‘stressed’ to explain a feeling or emotion usually arising from a particular event or situation. We say we feel ‘stressed’ when we perceive that the demands of a situation outweigh the perceived resources that we have to meet it (Lazarus Folkman 1984). The key word here is perceived.
Stress is normal. Most of us say we feel ‘stressed’ sometimes. You may find studying or elements of your job stressful, i.e. you perceive these stimuli or events as stressors. Lazarus & Folkman (1984) described how our reactions to such stressors include cognitions, emotions, behaviours and physiological changes. Cognitions are thoughts, such as the threat of how bad the outcome could be, how challenging it is and how much control you have over the situation (Lazarus & Folkman 1984). The emotional, behavioural and physical reactions might include feeling worried, thinking about the perceived problem a lot, working longer hours to complete work and experiencing physical symptoms of anxiety, such as ‘butterflies’ in the stomach (Lazarus & Folkman 1984).
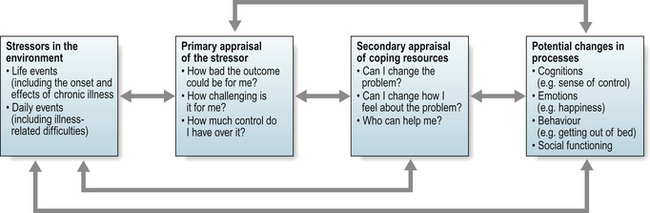
Alternatively, you might view your courses or tasks at work as exciting, challenging and feel elated by the prospect. An individual’s interpretation or perception of the stressful event and their response to it is the key element here. People experience different events, or different elements of events, as stressful or not based on their interpretation of the event. How you think about a given situation influences what you do. In reality, the experience of ‘stress’, and the ways in which we cope with it, is a process of interactions and adjustments in which we alter the impact of the stressful event or situation by making adjustments in our behaviours, cognitions and emotions (Lazarus & Folkman 1984, Fig. 11.1).
Chronic illnesses, like the rheumatic diseases, can be conceived as stressful events at both a physical and psychosocial level. They lead to coping responses from early onset (Treharne et al 2004), which are revised and adjusted throughout the disease course. This is a specific application of the stress-appraisal-coping model. People constantly appraise their coping responses for their usefulness, make adjustments and re-appraise the situation as necessary (Lazarus & Folkman 1984).
The concept of coping was introduced in Chapter 5. Coping involves a process of managing the emotional and physical demands of the stressful situation. Although coping responses used may not actually solve the problem or alter the demands of the situation per se, they may enable the individual to alter their perception of the situation and reconstruct their thinking in more positive terms. Coping responses can act in two ways to reduce psychological stress (Lazarus & Folkman 1984):
PROBLEM-FOCUSED COPING
The individual acts to alter the problem causing the stress. This is employed when a person believes that the situation is changeable and they have, or can get, the resources to help them. These beliefs can easily be facilitated by a therapist offering practical interventions and psychological support enhancing active problem-focused coping strategies, such as making a plan of action and following it. Such coping strategies are associated with better psychological outcomes and less depression among people with rheumatic disease (Hampson et al 1996, Treharne et al 2007a, Zautra & Manne 1992).
EMOTION-FOCUSED COPING
The individual acts to cope with the emotional effects of a problem. Often people engage in this type of coping when they believe they cannot alter the stressor or have insufficient resources to cope with the problem (Lazarus & Folkman 1984). These strategies often involve avoidance, which can be active in nature, such as keeping busy with some other task, or passive in nature, such as social withdrawal. Emotion-focused coping does not always involve avoidant behaviour, for example trying to see the positive side of the situation is an active emotion-focused strategy (Treharne et al 2007a).
In the UK, facilitating coping strategies is becoming increasingly relevant as the government places further onus upon individuals to take responsibility for their own health and well-being, supported in full by multidisciplinary services within the NHS and their selected partnerships (Department of Health 2006). ‘Standards of care’ have been published by the Arthritis and Musculoskeletal Alliance (ARMA) in the UK for a variety of rheumatic diseases, including back pain, connective tissue diseases, inflammatory arthritis and osteoarthritis (http://www.arma.net.uk). ARMA proposed self-management training should be available for individuals with rheumatic disease at any stage of their illness: via the Challenging Arthritis programme run by the charity Arthritis Care (see Barlow et al 1998): the generic Expert Patient Programmes, now available throughout the UK within NHS primary care trusts (see Expert Patients Programme 2009); and health professional led self management programmes. Many people will be happy to seek information and learn self-management strategies through group-based interventions, but not all are able to or comfortable with such courses (Hale et al 2006b). Ongoing individualised treatment plans by the multidisciplinary team are still required.
ASSESSING STRESS
Assessing causes of stress may form an important part of your baseline assessment, particularly if you provide relaxation therapy or other stress management interventions. Initially, psychologists assessed stress in terms of the impact of certain life events (Holmes & Rahe 1967). The death of a spouse or close family member was deemed more severe in impact than holidays, a notable stressor. The number of stressful life events, particularly recent ones, is linked to health status and onset of health problems (Holmes & Rahe 1967).
More recently, assessment has focused on impact of daily hassles, i.e. acute events having a direct daily impact (Kanner et al 1981), particularly for people with chronic illnesses like RA (Treharne et al 2002, Turner Cobb et al 1998). When these events become long-term (e.g. daily difficulties at work due to hand problems; frequent tense exchanges with a relative due to their limited understanding of the impact of rheumatic disease), the stressor becomes chronic. The impact of daily hassles can possibly be worse than some of the major life events mentioned (Pillow et al 1996).
Global assessments of stress levels can also be used without addressing the specific event causing the stress. For example, the Perceived Stress Scale (Cohen et al 1983) is a short measure of whether an individual is failing to cope with their perceived stress. This has been applied in several rheumatic disease studies. Scores predict worsening of anxiety over one year (measured using the Hospital Anxiety and Depression Scale; Zigmond & Snaith 1983) among people with rheumatoid arthritis (Treharne et al 2007a).
Assessing potentially stressful events in your patients’ daily life can include the frequency, perceived impact and severity of the stressor for that individual. This can be measured with objective instruments, such as the Daily Stress Inventory (Brantley et al 1987). Alternatively, you can ask the patient to keep a simple daily diary of events and their responses (behaviours and moods) to help you design a tailored intervention to help them meet goals for improvement they set. Such diaries can be structured to cover various aspects of daily life (e.g. going shopping; when splints are used) in as much or as little detail as required. These do not have to meet psychometric standards necessary for research if being used as a clinical tool for information gathering, enabling the person to reflect on what they are experiencing on a day-to-day (or hour-by-hour) basis.
UNDERSTANDING STRESSORS
Common long-term daily stressors include frustration with daily activities, living with pain and fatigue and potentially limited understanding of family and friends. People with such long-term daily stressors may experience psychological and social changes that may be difficult to understand and accept (Katz & Neugebauer 2001). Health professionals need to respond to patient needs (which may not always be clearly articulated) and apply a range of approaches and models of self-care support. These approaches can be individual or group based. In order to target educational and therapeutic approaches appropriately we need to understand individual beliefs and capabilities, what knowledge patients have about their condition, the degree to which they have accepted their condition, their attitude, confidence and determination to achieve a progressive positive outcome (see Ch. 6).
COGNITIVE REPRESENTATIONS OF ILLNESS
As described earlier, cognitions are thought processes a person goes through to make sense of any situation or event. People form guides about what is expected in specific contexts, such as how to behave in a restaurant or lecture (e.g. not to throw food). These guides, called schemas, incorporate the norms and values appropriate to our society. However, people have individual beliefs and experiences that underpin the subtleties of their personal schemas (Greenberger & Padesky 1995).
Some well known illnesses have clear schemas, with labels attached to them, that people consider when searching for an explanation for a group of symptoms being experienced, for example ‘influenza’ (Bishop 1991). However, illnesses presenting with an array of rare, complex, variable and confusing symptoms are less easily interpreted. Individuals turn to other lay means of sense-making, for example, asking a relative or friend with a similar experience (Hale et al 2007). When it becomes necessary or apparent that formal medical assistance is required, diagnosis is not quick and the process may involve numerous tests and uncertainties. This can be common in rheumatic diseases, especially systemic lupus erythematosus (Hale et al 2006a), RA and fibromyalgia. This procedure contributes to the formation of patients’ beliefs, attitudes and uncertainties and subsequently updates their illness schemas (see Ch. 5). Leventhal and colleagues laid much of the groundwork for our understanding of illness perceptions (Nerenz & Leventhal 1983, see Leventhal et al 2003).
Different types of information influence different responses to perceived threats to health and well-being. Leventhal and colleagues explored what adaptations and coping efforts need to be made and maintained in people experiencing chronic illness. They proposed an adaptive system model in which illness representations guide coping responses and performance of action plans followed by monitoring of the success or failure of coping efforts (Nerenz & Leventhal 1983). The model has similarities with other problem-solving behaviour theories, such as the transactional model of stress and coping described earlier (Fig. 11.1), wherein chronic illness is conceptualised as the stressful experience (Lazarus & Folkman 1984). Leventhal and colleagues described parallel thinking about the illness danger (e.g. ‘What are these pains I keep getting, is there anything I can do about them?’) and emotional control (e.g. “I am upset as my doctor said she can’t cure it, what shall I do to make myself feel better about it?”) (Nerenz & Leventhal 1983).
MEASURING ILLNESS PERCEPTIONS
Validated questionnaire measures of illness perceptions include the Revised Illness Perception Questionnaire (Moss-Morris et al 2002, see Box 11.2) and a shortened version, the Brief Illness Perception Questionnaire (Broadbent et al 2006). These can be applied in clinical practice to access patients’ beliefs about their illness’s impact and future health. These impacts include assessments about its consequences, its controllability (by the individual as a self-manager or via treatments they are prescribed), its emotional impact and its coherence (i.e. whether the symptoms and overall illness experience make sense to the patient). Moss-Morris et al (2002) describe how the patient’s ongoing perceptions of the timeline of their illness relates to whether or not they think their illness will be permanent (i.e. chronic) and go through cycles (i.e. flare and remissions), as many rheumatic diseases can do (Hill & Ryan 2000).
BOX 11.2 Illness cognitions (with example items from the Revised Illness Perception Questionnaire; Moss-Morris et al 2002)
REMODELLING ILLNESS PERCEPTIONS
By accessing patients’ illness perceptions, health professionals can tailor patient education and treatment plans to the individual emphasizing those elements causing most concern to the patient (Hale et al 2007). This helps people reassess any obviously erroneous illness beliefs they express. This can be achieved by sharing appropriate disease-related information, discussing treatment and working through any worries about potential side-effects. Patients’ plans for the future can be constructed and revised as necessary using simple principles like carrying out activities that they enjoy (within their ability range) to distract them from worry and to facilitate a sense of achievement that is easily lost in a disease that can have severe psychosocial impact.
This approach to remodelling illness perceptions was formally tested in an intervention for people who had recently had a heart attack (Petrie et al 2002). After assessing participants’ perceptions of their heart disease, an inpatient intervention provided general information about the need to avoid attributing all on-going symptoms to heart disease. A personalised approach then addressed the specific illness perceptions worrying participants (most of whom were men), as well as discussing their medications, discharge plan and importance of individual’s lifestyle risks (e.g. poor diet, lack of exercise, smoking). This aimed to improve participants’ sense of control by expanding their causal models beyond the common misconception that stress was the sole cause of their heart attack. Compared to a control group (given standard cardiac education), those receiving this personalised intervention showed improvements in perceptions of their ability to control symptoms, consequences of their heart disease and its timeline. After three months, they also felt more prepared for their discharge, had a faster rate of return to work and reported fewer symptoms of angina.
A similar approach was taken by Goodman et al (2005) among people with systemic lupus erythematosus. They used a group CBT intervention, including goal setting, writing action plans, carrying out ‘behavioural experiments’ to help challenge negative automatic thought patterns using cognitive restructuring, as well as relaxation, distraction and guided imagery. A limitation of Goodman et al (2005) study was that participants chose whether or not they were in the intervention group. This is not ideal for testing interventions because self-selection, rather than randomised allocation, means the two groups could be significantly different (for example, psychologically), even though reflective of how such interventions might be instigated in routine clinical practice (see Study activity 2). Patients reported increased perceptions that treatment could control their lupus but not in perceptions they could control their own illness. Despite this, there were decreases in perceived stress, feelings of helplessness and self-critical thinking after the intervention, demonstrating how the vicious circle of thoughts and behaviours can be broken (see Study activity 11.2).
Other group-based intervention studies have delivered patient education accessing patients’ illness perceptions as part of the educative process. Brown et al (2004) described the benefits patients obtained from the groups ‘Focus on Lupus’ and ‘Focus on Scleroderma’ using qualitative analysis, providing depth to understanding the process. Patients reported feeling more in control, although people with lupus had a more positive collective response.
DEFINING MOOD DISORDERS AND ASSESSING MOOD
Psychological outcome measures are outlined in Chapter 4. It is important to identify whether mood states meet diagnostic criteria for psychiatric conditions before planning ways to help improve mood, as some may need mental health services. It is also important to monitor ongoing daily mood of the individual, and go beyond retrospective measures (e.g. the Hospital Anxiety and Depression Scale, Zigmond & Snaith 1983).
DEPRESSION AND ANXIETY
Like the word stress, the terms depressed and anxious have been assimilated into everyday language. These conditions are based on clear medical diagnoses (American Psychiatric Association 2000). Health professionals must listen to the mood symptoms their patients are describing and map these along the parallel continuum from happiness and calmness (the ‘norm’) through occasional bouts of dejectedness and worry (a transient problem) to enduring sadness or generalised anxiety (more chronic problems).
Depression
An‘episode’ of major depression is classified by the American Psychiatric Association (2000) as at least two weeks of depressed mood or lack of interest in activities and anhedonia (the lack of pleasure from previously enjoyed activities). These problems are experienced most of the day and every day for this period. In addition to this, the individual should have four or more of the following associated problems:
(American Psychiatric Association 2000)
There is some potential overlap with the effects of fatigue and disability from rheumatic disease, but the criterion of ‘feeling slowed down’ is meant as a cognitive rather than physical problem. Frank et al (1988) applied an earlier version of these criteria to a sample of people with rheumatoid arthritis using structured clinical interviewing finding the prevalence of major depression was 17%. A recent meta-analysis has confirmed depression is more common in RA than the general population (Dickens et al 2002).
A less intense but prolonged version of depression is called dysthymic disorder or minor depression. This is classified by the American Psychiatric Association (2000) as depressed mood most of the day, more days than not for at least two years, and is probably the most common type of depressed mood you will come across in your clinical practice (Frank et al 1988).
Anxiety
Generalised anxiety disorder is distinct from phobias and pure obsessive thought disorders. The American Psychiatric Association (2000) classifies this using criteria of excessive, uncontrollable worry about several events (which could include one’s state of health) more days than not for a period of at least 6 months that has an impact on social functioning or work ability. In addition, the individual should have four or more of the following problems:
ASSESSING DEPRESSION AND ANXIETY
Muscle tension may also be experienced in rheumatic disease (Treharne et al 2007b). It is also clear that (major) depression and (generalised) anxiety overlap in their listed symptoms and associated thought processes. The forthcoming revision to the American Psychiatric Association’s criteria, due for publication in 2010, should clarify differences further (Kupfer et al 2002). Fortunately, both conditions are tackled by similar psychological therapies (Greenberger & Padesky 1995) and drug treatments (Joint Formulary Committee 2009).
Given the problems with accuracy of retrospective recall of psychological processes (Stone et al 1998), the criteria for depression and anxiety ideally require some form of daily mood assessment. Electronic completion of questionnaires is ideal given the ease of viewing questions and answer choices on-screen, saving on paper consumption and data entry time, whilst maintaining replicability of the meaning of questions (e.g. Wilson et al 2002, see Fig. 11.2).
Two classic measures of mood are the Positive and Negative Affect Schedule (Watson et al 1988, see also Crawford & Henry 2004, for normative data) and the bipolar Profile of Mood States (Lorr & McNair 1982, see also Treharne et al 2001, 2002, for applications of relevant subscales). Both these questionnaires assess depression (versus elation) and anxiety (versus calmness) but, as with assessments of stress, a diary system for recording aspects of mood can be used. Alternatively, two screening questions can be used (Arroll et al 2003):
The responses help you direct your therapeutic skills to one or both of these issues (see below), or the basis for referral to local psychological services.
PRACTICAL COGNITIVE BEHAVIOURAL METHODS
So far we have examined how illness might be perceived as stressful, and how patients’ symptoms, cognitions (i.e. thoughts), moods and behaviours combine to determine their coping responses. Appraisals of coping style and the effectiveness of that response guide further coping efforts. This applies to all of us in everyday life as well as to people with chronic illnesses. Many people find coping with the physical and the psychosocial effects of their disease difficult and may experience periods of depression and/or anxiety, which are troublesome even if they do not reach the formal criteria for a mood disorder (Lewinsohn et al 2000). This can occur at the initial stages of their disease journey (Treharne et al 2004), or any time particularly, during a flare or after a psychosocial loss like employment, a valued leisure activity or role within the home (Katz & Neugebauer 2001). It may also relate to any life event, such as a bereavement or moving house (Holmes & Rahe 1967). These kind of events (measured using inventories) relate to depression among people with RA (Turner Cobb et al 1998).
When coping becomes difficult, it is useful to understand what an individual believes about his or her disease and the likely impact of the disease. Understanding such thoughts and thought processes, the behavioural consequences of those thoughts and the physiological symptoms and reactions to those thoughts will give greater insight into those areas that might be hindering effective coping practices.
SELF-MANAGEMENT PROGRAMMES
The use of cognitive-behavioural approaches within rheumatology commenced on a large scale with the development of the Arthritis Self-Management Programme (ASMP; known as Challenging Arthritis in the UK), which facilitates effective coping within a group-based community programme led by people who have arthritis (Lorig & Holman 1989). Self-management, applying cognitive-behavioural techniques, builds upon the principle of self-efficacy (Bandura 1977) (see Chs 5 & 6). This approach aims to enhance the belief one can achieve a goal, even in the face of specific obstacles, for example, going for a walk even when feeling fatigued or when it is raining.
Participants in ASMP and Challenging Arthritis groups learn principles of self-help, i.e. taking responsibility for learning about and managing their condition. Within this, they are given disease-related information including: drug treatments; exercise; fatigue; pain management/relaxation techniques; nutrition; non-traditional treatments; problem-solving; communication skills; depression and contracting (learning to set achievable goals). Optimising the effectiveness of an intervention may require customising elements to individual difficulties and characteristics; for example, patients exhibiting heightened distress levels as opposed to those adjusting relatively well.
COGNITIVE-BEHAVIOURAL APPROACHES
Cognitive-behavioural approaches, on an individual basis or within small group settings (i.e. between 4 and 12 members), focus more specifically upon accessing those thoughts, moods and behaviours that lead to depression and anxiety (Dickens et al 2002). Classically, the type of thoughts indicative of depression focus upon loss, whereas thoughts about threat or challenge are typical in people with anxiety (Sanders & Wills 2005). Whilst there are formal measures of depression and anxiety (as outlined earlier and in Ch. 4), a flexibly structured clinical interview provides valuable information.
Cognitive approaches
People experiencing depression have a typically negative way of thinking about the self, the world and the future and may continue to appraise events in these terms, falling into a cycle of negative automatic thoughts, upon which they often ruminate, and find difficult to reconceptualise (Sanders & Wills 2005). An individual who has developed this negatively biased way of thinking will exhibit common cognitive biases, such as ‘all-or-nothing’ or ‘black-and-white’ thinking where the shades of ‘grey’ areas of life are overlooked, so that an individual might think, or even state out loud, that “I’ve completely failed, everyone else can do this”. There may be ‘catastrophic’ thinking where the worst is always predicted “I’ll never be able to do that again, I’ve lost everything.” A particular challenge for the therapist might be working with those thoughts that involve ‘gazing into a crystal ball’ where the patient anticipates the future in a typically negative way so that their prediction will be “There’s no point in trying this physiotherapy as it won’t work.” By structured questioning and listening to your patient carefully, you may be able to access the key areas of difficulty that you can work with.
Behavioural approaches
Setting acceptable staged goals that the individual can easily test that they can achieve (particularly if those goals are pleasurable) is a short-term behavioural experiment that will hopefully challenge the patient’s hypotheses of overall failure and reduce anxieties. Like the well-known mantra of Alcoholics Anonymous (AA), they need to take things ‘one day at a time’. Simple feedback, like plotting charts of achievement, exercise or activity diaries and suggesting personally-set rewards as an incentive, are useful maintenance tools the patient can use in the long-term. Such charts and diaries are best personally tailored to the needs of the individual rather than following a prescribed format. Suggestions you can use include structuring the records around various segments of the day (e.g. early morning, late morning, afternoon and evening, or before work, during work and after work) and the use of very small motivational rewards such as gold stars, which no one is too old for.
Cognitive therapy
Cognitive therapists will work to develop a ‘conceptualisation’ or ‘formulation’ that links schemas, salient or triggering events, mood, cognitions and behaviours to explain to the patient how vicious cycles arise that continue to feed negative repetitive thoughts and impact upon mood and, subsequently, behaviour. This may be beyond the scope of your practice, however, and it would be appropriate to work closely with the psychologist within your multidisciplinary team (if you work within such a team and have access to a psychologist). Occupational therapists can pursue post-graduate training in cognitive-behavioural therapy (as either short or long courses) and some essentials may be included in undergraduate courses. See Study activity 11.3 for details of an example case of a patient with systemic lupus erythematosus who experienced psychosocial difficulties.
Evidence for CBT approaches in rheumatology
CBT approaches can involve a number of broad methods focusing on breaking the cycle of thoughts and behaviours that may be perpetuating a psychological problem (Sanders & Wills 2005). Several studies have tested CBT approaches in rheumatic diseases. Sharpe et al (2001a, 2003) used the basis of the ASMP manual to deliver individually tailored one-to-one CBT sessions for people with rheumatoid arthritis. Reductions in depressed mood were found immediately after treatment and 6 and 18 months later for participants given the CBT intervention, whereas depressed mood worsened over the same period for those given just routine care (i.e. the control group). Swollen joint counts also reduced over time for the participants given CBT, more so than the control group. However, the individuals in the CBT group made significantly more coping efforts (over many strategies on an inventory where all efforts are summed) at the start of their study, therefore, the groups appeared unevenly matched for motivation to start with. It is also hard to convey a sense of what happened for individuals in the therapy sessions in a journal article. The additional report by Sharpe et al (2001b) on a series of these cases is more enlightening for select examples.
Another tailored CBT programme by Evers et al (2002) was developed for people with rheumatoid arthritis designated ‘at risk’ for psychological problems (i.e. characterised by higher levels of negative mood and anxiety, more passive coping with pain and stress, greater helplessness and less acceptance of disease and lower levels of social functioning, perceived support and network help). A selection of patient-preferred modules targeted, for example, negative mood or fatigue. People were selected in the ‘early’ stages of their disease. However, this was defined as within 8 years from diagnosis. This could be too wide a definition, providing a group with very varied experiences. Depression, helplessness and fatigue were significantly reduced post-treatment and 6 months later compared to the control group who received routine care. Furthermore, at the 6-month follow-up assessment perceived support, active coping with stress and adherence to prescribed medication had increased more in the CBT group than the control group. Of course it is not known at this stage how individualised treatments compare to more generalised CBT treatments for all people with rheumatoid arthritis or those not deemed ‘at risk’, nor how or what treatment effects might be seen in those with long-standing disease. However, although randomised controlled trials are hard to conduct, and inevitably still have limitations, the evidence currently suggests that CBT can show benefit for people with rheumatic disease, which are worth applying in practice.
CONCLUSION
Stress management, self-management programmes and using CBT approaches are all effective strategies in Rheumatology. These need to be an integral part of occupational and physiotherapists’ daily practice. Further training in CBT approaches and liaison with health and clinical psychologists to develop services is recommended.
ACKNOWLEDGEMENTS
We thank Prof. George Kitas and Mrs Yvonne Norton MBE, Chair of Lupus West Midlands, for their support. We are also grateful to Miss S for consenting to share her experiences.
Miss S is a 35-year-old single woman with a confirmed diagnosis of systemic lupus erythematosus. She frequently experiences significant skin rashes and joint discomfort. She can no longer work as she experiences periods of severe fatigue and is often confined to the house which makes her feel isolated and depressed. Miss S had difficulty obtaining a diagnosis at the onset of her disease and was hospitalised for depression at this time. She used to be a dynamic out-going young woman, hard working and successful in her career. Since her diagnosis she has had significant psychosocial losses to adjust to: loss of satisfying work and income forcing a house move; loss of social life and friends and work colleagues; the prospect of losing a relationship due to her continuing ill-health and appearance concerns.
Miss S would like to be more physically active, less dependent upon her family and work with animals at some point in the future. She continues to find it difficult to come to terms with her disease and experiences depression and anxiety about the future.
Discuss with your colleagues or fellow students how you would approach the varied aspects of this case. If you work in a multidisciplinary team, how would your colleagues from other disciplines approach these issues? (For more details about this case, and other similar cases, see Hale et al 2006a.)
The Division of Health Psychology of the British Psychological Society
http://www.health-psychology.org.uk
Patient UK: A reference website aimed at the UK public. http://www.patient.co.uk
The Birmingham Arthritis Resource Centre: a community-based educational resource centre with information on several rheumatic diseases available in different languages.
The Arthritis and Musculoskeletal Alliance
The Oxford Cognitive Therapy Centre (Warneford Hospital, Oxford, UK): details of courses, booklets and textbooks on the cognitive approach to psychological therapy.
References and further reading
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, fourth ed. Washington, DC.: text revision American Psychiatric Association; 2000. text revision
Arroll B., Khin N., Kerse N. Screening for depression in primary care with two verbally asked questions: cross sectional study. Brit. Med. J.. 2003;327(7424):1144-1146.
Bandura A. Self-efficacy: toward a unifying theory of behavioral change. Psychol. Rev.. 1977;84(2):191-215.
Barlow J., Turner A., Wright C. Long-term outcomes of an arthritis self-management programme. Brit. J. Rheumatol.. 1998;37(12):1315-1319.
Bishop G.D. Lay disease representations and responses to victims of disease. Basic Appl. Soc. Psych.. 1991;12(1):115-132.
Brantley P.J., Waggoner C.D., Jones G.N., et al. A daily stress inventory: Development, reliability, and validity. J. Behav. Med.. 1987;10(1):61-74.
Broadbent E., Petrie K.J., Main J., et al. The Brief Illness Perception Questionnaire. J. Psychosom. Res.. 2006;60(6):631-637.
Brown S.J., Somerset M.E., McCabe C.S., et al. The impact of group education on participants’ management of their disease in lupus and scleroderma. Musculoskeletal Care. 2004;2(4):207-217.
Cohen S., Kamarck T., Mermelstein R. A global measure of perceived stress. J. Health Soc. Behav.. 1983;24(4):385-396.
Crawford J.R., Henry J.D. The Positive and Negative Affect Schedule (PANAS): construct validity, measurement properties and normative data in a large non-clinical sample. Brit. J. Clin. Psychol.. 2004;43(3):245-265.
Department of Health. Supporting People with Long-Term Conditions to Self-Care: A Guide to Developing Local Strategies and Good Practice. London: Department of Health; 24 February, 2006. Online. Available: http://www.dh.gov.uk/en/Publicationsandstatistics/Publications/PublicationsPolicyAndGuidance/DH_4130725/22.10.2008.
Dickens C., McGowan L., Clark-Carter D., Creed F. Depression in rheumatoid arthritis: A systematic review of the literature with meta-analysis. Psychosom. Med.. 2002;64(1):52-60.
Dixon K.E., Keefe F.J., Scipio C.D., et al. Psychological interventions for arthritis pain management in adults: a meta-analysis. Health Psychol.. 2007;26(3):241-250.
Evers A.W.M., Kraaimaat F.W., van Riel P.L.C.M., et al. Tailored cognitive-behavioral therapy in early rheumatoid arthritis for patients at risk: a randomized controlled trial. Pain. 2002;100(1-2):141-153.
Expert Patients Programme. 2009. Find a course. Online. Available: http://www.expertpatients.co.uk/public/default.aspx?load=SearchCourses/ Accessed 6.9.09.
Frank R.G., Beck N.C., Parker J.C., et al. Depression in rheumatoid arthritis. J. Rheumatol.. 1988;15(6):920-925.
Goodman D., Morrissey S., Graham D., et al. The application of cognitive-behaviour therapy in altering illness representations of systemic lupus erythematosus. Behav. Change. 2005;22(3):156-171.
Greenberger D., Padesky C.A. Mind over Mood: Change How You Feel by Changing the Way You Think. New York: Guilford, 1995.
Hale E.D., Treharne G.J., Kitas G.D. The common-sense model of self-regulation of health and illness: how can we use it to understand and respond to our patients’ needs? Rheumatology. 2007;46(6):904-906.
Hale E.D., Treharne G.J., Lyons A.C., et al. “Joining-the-dots” for systemic lupus erythematosus patients: personal perspectives of healthcare from a qualitative study. Ann. Rheum. Dis.. 2006;65(5):585-589.
Hale E.D., Treharne G.J., Macey S.J., et al. ‘Big boys don’t cry’: a qualitative study of gender differences in self-management and coping with arthritis. Abstract. Rheumatology, 45. 2006;Suppl. 1:i14.
Hampson S.E., Glasgow R.E., Zeiss A.M. Coping with osteoarthritis by older adults. Arthritis Care Res.. 1996;9(2):133-141.
Hill J., Ryan S. Rheumatology: A Handbook for Community Nurses. London: Whurr; 2000.
Holmes T.H., Rahe R.H. The social readjustment rating scale. J. Psychosom. Res.. 1967;11(2):213-218.
Joint Formulary Committee, March 2009. British National Formulary, 57th ed. British Medical Association and Royal Pharmaceutical Society of Great Britain, London Online. Available: http://bnf.org/bnf/.
Kanner A.D., Coyne J.C., Schaefer C., et al. Comparison of two modes of stress measurement: daily hassles and uplifts versus major life events. J. Behav. Med.. 1981;4(1):1-39.
Katz P.P., Neugebauer A. Does satisfaction with abilities mediate the relationship between the impact of rheumatoid arthritis on valued activities and depressive symptoms? Arthritis Care Res.. 2001;45(3):263-269.
Kupfer D.J., First M.B., Regier D.A. A Research Agenda for DSM-V. Washington, DC: American Psychiatric Association, 2002.
Lazarus R.S., Folkman S. Stress, Appraisal, and Coping. New York: Springer; 1984.
Leventhal H., Brissette I., Leventhal E.A. The common-sense model of self-regulation of health and illness. In: Cameron L.D., Leventhal H., editors. The Self-Regulation of Health and Illness Behaviour. London: Routledge; 2003:42-65.
Lewinsohn P.M., Solomon A., Seeley J.R., et al. Clinical implications of “subthreshold” depressive symptoms. J. Abnorm. Psychol.. 2000;109(2):345-351.
Lorig K., Holman H. Long-term outcomes of an arthritis self-management study: effects of reinforcement efforts. Soc. Sci. Med.. 1989;29(2):221-224.
Lorr M., McNair D. Profile of Mood States: Bi-Polar Form. San Diego: Educational and Industrial Testing Service; 1982.
Moss-Morris R., Weinman J., Petrie K., et al. The revised illness perceptions questionnaire (IPQ-R). Psychol. Health. 2002;17(1):1-16.
Nerenz D., Leventhal H. Self-regulation in chronic illness. In: Burish T.G., Bradley L.A., editors. Coping with Chronic Disease: Research and Applications. New York: Academic Press; 1983:13-37.
Petrie K., Cameron L., Ellis C., et al. Changing illness perceptions after myocardial infarction: an early intervention randomized controlled trial. Psychosom. Med.. 2002;64(4):580-586.
Pillow D.R., Zautra A.J., Sandler I. Major life events and minor stressors: identifying mediational links in the stress process. J. Pers. Soc. Psychol.. 1996;70(2):381-394.
Sanders D., Wills F. Cognitive Therapy: An Introduction, second ed. London: Sage, 2005.
Sharpe L., Sensky T., Timberlake N., et al. A blind, randomized, controlled trial of cognitive-behavioural intervention for patients with recent onset rheumatoid arthritis: preventing psychological and physical morbidity. Pain. 2001;89(2–3):275-283.
Sharpe L., Sensky T., Timberlake N., et al. The role of cognitive behavioural therapy in facilitating adaptation to rheumatoid arthritis: a case series. Behav. Cogn. Psychoth.. 2001;29(3):303-309.
Sharpe L., Sensky T., Timberlake N., et al. Long-term efficacy of a cognitive behavioural treatment from a randomized controlled trial for patients recently diagnosed with rheumatoid arthritis. Rheumatology. 2003;42(3):435-441.
Stone A.A., Schwartz J.E., Neale J.M., et al. A comparison of coping assessed by ecological momentary assessment and retrospective recall. J. Pers. Soc. Psychol.. 1998;74(6):1670-1680.
Treharne G.J., Lyons A.C., Tupling R.E. The effects of optimism, pessimism, social support, and mood on the lagged relationship between daily stress and symptoms. Online. Curr. Res. Soc. Psychol., 7. 2001;5:60-81. Online Available: http://www.uiowa.edu/~grpproc/crisp/crisp.7.5.htm/
Treharne G.J., Lyons A.C., Booth D.A., et al. Daily stress, coping, and helpful support in relation to symptoms and mood in rheumatoid arthritis (RA) patients. Rheumatology. 2002;41(Suppl.):73. Abstract
Treharne G.J., Lyons A.C., Booth D.A., et al. Reactions to disability in patients with early versus established rheumatoid arthritis. Scand. J. Rheumatol.. 2004;33(1):30-38.
Treharne G.J., Lyons A.C., Booth D.A., et al. Psychological well-being across 1 year with rheumatoid arthritis: coping resources as buffers of perceived stress. Brit. J. Health Psychol.. 2007;12(3):323-345.
Treharne G.J., Lyons A.C., Hale E.D., et al. Sleep disruption frequency in rheumatoid arthritis: predictors of change over 1 year and its impact on outcomes. Musculoskeletal Care. 2007;5(1):51-64.
Turner Cobb J.M., Steptoe A., Perry L., Axford J. Adjustment in patients with rheumatoid arthritis and their children. J. Rheumatol.. 1998;25(3):565-571.
Watson D., Clark L.A., Tellegen A. Development and validation of brief measures of positive and negative affect: the PANAS scales. J. Pers. Soc. Psychol.. 1988;54(6):1063-1070.
Wilson A.S., Kitas G.D., Carruthers D.M., et al. Computerised information gathering in two specialist rheumatology clinics: an evaluation of an initial electronic version of the Short Form 36. Rheumatology. 2002;41(3):268-273.
Zautra A.J., Manne S.L. Coping with rheumatoid arthritis: a review of a decade of research. Ann. Behav. Med.. 1992;14(1):31-39.
Zigmond A.S., Snaith R.P. The hospital anxiety and depression scale. Acta Psychiat. Scand.. 1983;67(6):361-370.