Chapter 1 Overview of the aims and management of rheumatological conditions
The multidisciplinary approach
1.1 Rheumatology and the rheumatologist
Krysia Dziedzic PhD MCSP Arthritis Research Campaign National Primary Care Centre, Primary Care Sciences, Keele University, Keele, UK
Peter Dawes MBChB FRCP Haywood Hospital, Stoke on Trent NHS Primary Care Trust, Staffordshire, UK
INTRODUCTION
There are over 200 musculoskeletal conditions affecting millions of adults and children, and it is estimated that up to 30% of all general practice consultations are about musculoskeletal complaints (Department of Health 2006). The ageing population will further increase the demand for treatment of age-related disorders such as osteoarthritis and osteoporosis (Department of Health 2006). Rheumatology is an exciting and expanding field (BHPR 2004). Its profile has risen dramatically with improved understanding of inflammatory and non-inflammatory conditions, and the availability of powerful and expensive treatments, e.g. anti-TNF therapies.
People with musculoskeletal conditions need a wide range of high-quality support and treatment from simple advice to highly specialised treatments. The Musculoskeletal Services Framework (MSF) (Department of Health 2006) describes best practice, built around evidence and experience. It promotes ‘redesign of services, and full exploitation of skills and new roles of all healthcare professionals’; and ‘better outcomes for people with musculoskeletal conditions through a more actively managed patient pathway, with explicit sharing of information and responsibility, agreed between all stakeholders in all sectors – patients; the NHS and local authorities; and voluntary/community organisations’. Multidisciplinary services are central to the framework, offering triage, assessment, diagnosis, treatment or rapid referral to other specialists.
THE ROLE OF THE MULTIDISCIPLINARY TEAM
The multidisciplinary team has been shown to be effective in optimising management of patients with arthritis (Vliet Vlieland et al 1997). All patients should have opportunities to access a range of health care professionals (SIGN 2000), including rheumatologist, general practitioner, nurse specialist, physiotherapist, occupational therapist, dietician, podiatrist, health psychologist, social worker and pharmacist. The next section will summarise the individual roles of many of these health care professionals. Following this, the most important member of the rheumatology team, the patient as an expert in living with the condition, will describe their journey (see Ch. 2). Throughout the book members of the multidisciplinary team have contributed chapters on their specific area of specialty, e.g. Chapter 14 on diet and complementary therapies.
THE RHEUMATOLOGIST
Rheumatologists have general medical knowledge, and have additional training and experience in the diagnosis and treatment of arthritis and other diseases of the musculoskeletal system. As well as an empathic approach to patients and the ability to work well within a multidisciplinary team the rheumatologist will often be the team leader. They develop good communication skills and above all the ability to work closely with other health professionals. The team approach to providing care is highly valued by rheumatologists because rheumatology manages longstanding and often incurable conditions.
The majority of musculoskeletal diseases are managed in primary care and rheumatology is mainly an outpatient speciality. Some rheumatology departments hold out-reach clinics in general practice, and some are now sited in primary care trusts. However, there are real advantages for patients with inflammatory arthritis or connective tissue disease in seeing a rheumatologist (BHPR 2004), as some of these are very serious diseases that can be difficult to diagnose and treat. Timing of pharmacological interventions and their safe monitoring is a pre-requisite for managing inflammatory arthritis. Rheumatologists undertake many practical procedures. All would do joint aspiration and injection whilst some develop an interest in ultrasound, nerve conduction studies, arthroscopies, muscle biopsies etc. (BHPR 2004). Others develop expertise in management, research or education.
Some rheumatic diseases are complex requiring monitoring to determine a diagnosis and follow-up to assess change over time. Rheumatologists work closely with patients and the rheumatology team to identify problems, design individualised treatment programmes and help patients and their families cope with the impact of the disease.
Rheumatologists also work closely with orthopaedic surgeons, radiologists, anaesthetists (pain service), and neurosurgeons, and keep the patient’s own general practitioner fully informed of progress.
1.2 Nursing
Sarah Ryan RGN PhD MSc BSc FRCN Haywood Hospital, Stoke on Trent NHS Primary Care Trust, Staffordshire, UK
THE RHEUMATOLOGY NURSE
THE ROLE OF THE RHEUMATOLOGY NURSE
The role of the rheumatology nurse has developed from the collection of clinical measurements during drug trials in the 1970’s (Bird 1983), to encompass a much broader spectrum of activities. These activities include patient education and counselling, the monitoring of drug therapy, running specialist clinics, patient assessment and management and recommending treatment changes to the rheumatologist and general practitioner (Carr 2001).
Patients are often referred to a rheumatology nurse following diagnosis of an inflammatory rheumatological condition, most commonly rheumatoid arthritis (RA) to commence disease modifying drugs, begin the process of patient education, to obtain symptom control and receive emotional support. At the time of diagnosis the patient can experience a plethora of emotions including anger, shock, grief and denial.
Shaul (1995) demonstrated that in the early stages, women with rheumatoid arthritis needed to have their symptoms explained and managed before they could begin the process of learning coping strategies. The nurse consultation enables partnership, intimacy and reciprocity to evolve, and provides the forum to identify the patient’s priorities, providing care that has meaning and relevance to the patient. The key functions of nursing, as described by Wilson Barnett (1985) (Box 1.2.1) will be incorporated into the consultation to promote adaptation to the condition. Education and support will also be offered to family members, if the family does not appreciate the value of the management being advocated, for example exercise to assist with pain, stiffness and fatigue, then the individual may find it difficult to engage in this activity, without the endorsement of their family.
BOX 1.2.1 The key functions of nursing (Wilson Barnett 1985)
CHARACTERISTICS OF NURSE-LED CLINICS
Hill (1992) describes the characteristics of a nurse led clinic as
A survey of practice in nurse led clinics for patients with RA (Ryan & Hill 2004) demonstrated that nurses are engaged in
The model for clinics for patients with RA has been replicated to other conditions including connective tissue disorders, osteoporosis and chronic pain.
COMMUNITY NURSE LED CLINICS
Nurse led clinics have been replicated in the community and GP practices to provide similar functions including:
Arthur and Clifford (2004) compared the satisfaction of patients attending drug monitoring within primary and secondary care locations. They found patients reported a higher level of satisfaction with secondary care based drug monitoring. Empathy, specialist knowledge, information provision, technical aspects, time and continuity of care were identified as important attributes contributing to the satisfaction experienced by patients attending secondary care drug monitoring.
THE EFFECTIVENESS OF NURSING INTERVENTIONS
Hill et al (1994) demonstrated the value of a clinic run on true nursing principles. This study was an evaluation of the effectiveness, safety and acceptability of a nurse practitioner in a rheumatology outpatient clinic. Seventy patients with RA were randomly allocated to either the nurse practitioner clinic or a consultant rheumatologist clinic and seen on six occasions over 12 months. On study entry the groups were well matched. At week 48 there was no significant difference between the two groups with both groups showing significant improvement in disease activity. However, the patients in the nurse practitioner cohort showed additional improvements not mirrored in the consultant group. The improvement was in levels of pain, morning stiffness, psychological status and satisfaction with care. One of the most noticeable aspects of the research was the marked difference in the referral patterns of the two practitioners, with the nurse practitioner making greater use of other members of the multi-disciplinary team, such as the physiotherapist. Hill’s work demonstrated that the nurse can add something extra to the management of patients with RA, and that extra is something that is valued by the patient.
A randomised controlled trial by Ryan et al (2006) examined the hypothesis that consultation with a consultant nurse specialist in a drug monitor clinic would have a measurable impact on the wellbeing of 71 patients with rheumatoid arthritis. Patients were randomised into two groups over a 3-year period. The intervention group was monitored by the consultant nurse specialist and an outpatient staff nurse reviewed the control group. Patients reviewed by the consultant nurse specialist reported a greater perception of being able to control their arthritis than those managed by the staff nurse. The role of the consultant nurse specialist in helping patients cope with their symptoms through goal setting, pacing, addressing low mood state and advocating exercise may be the nursing tools and expertise through which the ‘added value’ in influencing control perceptions was achieved. Ten patients from this study were interviewed by an independent researcher to explore ways of coping. The importance of nurse support in relation to enhancing positive control perceptions emerged as a clear theme in the intervention group (Hooper et al 2004).
PROVIDING TELEPHONE ADVICE
Telephone advice lines have become an integral part of rheumatology care and are traditionally run by rheumatology nurses or other health professionals in extended roles (Thwaites 2004). The telephone advice line provides patients with the means of contacting the rheumatology nurse directly involved in their care and is accessed to provide advice of drug therapy and symptom management.
CONCLUSION
The rheumatology nurse utilises specialist knowledge and skills to help the patient address the impact of their condition on a physical, psychological and social level. This is usually achieved through nurse led clinics where the process of education, symptom management and emotional support can commence.
1.3 General practice
Christian David Mallen BMedSci BMBS DRCOG DFFP MMedSci MPhil MPCGP PhD Arthritis Research Campaign National Primary Care Centre, Primary Care Sciences, Keele University, Keele, UK
GENERAL PRACTICE
GENERAL PRACTICE AND THE ROLE OF TRIAGE
Almost all people in the UK are registered with a GP who typically provides treatment for both acute and chronic illnesses as well as providing preventive care and health education. Traditionally, GPs have also acted as gatekeepers to more specialist services, such as those provided in secondary care or by allied health professionals. Over the past few years, however, this model has started to change with the introduction of innovative services such as community matrons and primary care nurse practitioners. Despite significant reorganisation in the health service resulting in the provision of alternative providers of primary care such as NHS Direct and NHS walk-in centres, over 90% of primary care patient contacts still occur in general practice.
Rheumatological conditions are extremely common in general practice, where they account for an estimated one in five consultations (McCormick et al 1995). Consultation rates for musculoskeletal disorders rise with increasing age, with women of all ages consulting more frequently than men. Low back pain is the most frequent reason for consulting a GP in younger age groups and remains a leading cause of work absence, whereas osteoarthritis (particularly of the hip and knee) is the dominant condition managed in older adults (Jordan et al 2007, McCormick et al 1995) accounting for more than two million consultations per year. Referral to secondary care is relatively unusual occurring in approximately 5% of all consultations.
GPs are by name, and training, generalists making it impossible to have in-depth knowledge in all areas, yet given the large workload generated by rheumatological conditions in primary care, it is perhaps surprising that formal clinical training in rheumatology, rehabilitation or orthopaedics does not commonly feature as part of general practice training schemes (Hosie 2000). These unmet educational needs are currently being addressed with the introduction of the first formal curriculum for general practice in 2007. Core competencies for rheumatological disorders have been identified that should be met by all GPs in training (full details are available at www.rcgp.org.uk).
Two recent developments in primary care that have the potential to significantly impact on the delivery of musculoskeletal services in the community are the introduction of GPs with a special interest in rheumatology and practice-based commissioning. These will be discussed in more detail below.
GENERAL PRACTITIONERS WITH A SPECIAL INTEREST
One of the key components of the NHS Plan (2000) was the formal introduction of General Practitioners with a Special Interest (GPwSI). A GPwSI is defined as a general practitioner who supplements their core professional role and undertakes advanced procedures not normally undertaken by their peers (Hay et al 2007). In order to work as a GPwSI, GPs have to first demonstrate that they have the appropriate skills and competencies to deliver an enhanced rheumatological service within a defined quality framework. This enables them to accept direct referrals from other GPs, which has the potential to reduce demand for more specialised secondary care services. Services are provided at a local level, and may include areas such as more specialised joint injection and the management of patients with inflammatory arthropathies.
PRACTICE BASED COMMISSIONING
Another recent development in primary care has been the implementation of practice based commissioning. Practice based commissioning, which is currently only implemented in England, refers to the devolution of commissioning for health related services to GPs (or more usually groups of GPs within a defined geographical area such as a Primary Care Trust (PCT)). GPs, with the support of their local PCTs, have the potential to hold specific budgets and to be responsible for commissioning key services (a scheme not dissimilar to ‘fund holding’ which formed the cornerstone of NHS reform in the 1990s). It is envisaged that this will encourage a greater variety of services, from an increased number of providers, in settings that are both closer to home and more convenient for patients and their families. If successful, this scheme has the potential to reduce referrals to secondary care, improve co-ordination of patient services and improve collaboration between local GP practices (Greener et al 2006), however, uptake of practice based commissioning is currently low in many areas and its impact on the provision of services has yet to be evaluated.
TRIAGE
Over the past decade, there has been a dramatic increase in the use of triage (particularly by telephone) in general practice. The term triage refers to the process where calls are received, assessed and managed by giving advice or by referral to a more appropriate service (Lattimer et al 1996). In general practice this is a role typically (although not exclusively) performed by practice nurses.
This system allows practices to prioritise their workload and to fully utilise the clinical skills and experience of the wider primary health care team where appropriate. It is estimated that up to 50% of calls from patients can be handled by telephone advice alone (range 25.5–72.2%) and that triage has the potential to reduce immediate GP surgery consultations and home visits (Bunn 2004). Many practices have introduced a system of telephone triage where patients with a ‘new’ problem (such as acute low back pain, respiratory tract infection) speak to the practice nurse who gives advice, offers treatment or referral to an appropriate health professional (e.g. GP, physiotherapist, occupational therapist, nurse practitioner) within a predetermined protocol. Although these systems have increased in popularity further research is needed to fully evaluate aspects of safety, cost and patient satisfaction (Bunn et al 2005).
An alterative triage system for patients with rheumatological complaints has been developed by organisations such as Physio Direct (http://www.csp.org.uk/). This system allows patients direct access by telephone to a senior physiotherapist who uses a combination of computerised protocols and their clinical experience to make a diagnosis, discuss management and make an appropriate treatment plan. It also provides patients with the convenience and flexibility of self-referral, and utilises health care professionals with experience and expertise in managing rheumatological disorders. Given the prolonged waits often encountered by patients waiting for physiotherapy, and the benefits associated with prompt treatment, this system has several clear advantages, which also including the potential to reduce GP appointments, reduce non-attendance to physiotherapy clinics and enhanced patient satisfaction, however, its use is currently not universal and it has yet to be fully evaluated.
Over 90% of primary care patient contacts still occur in general practice, and rheumatological conditions are extremely common in primary care. In recent years there has been a dramatic rise in the use of triage and other approaches of direct and self- referral. Future years will see further evaluation of the cost effectiveness of these new initiatives compared with traditional approaches in primary care.
1.4 Physiotherapy
Kay Stevenson M.Phil Grad Dip Phys University Hospital of North Staffordshire, Stoke on Trent, Staffordshire, UK
BACKGROUND
Today many physiotherapists are working at the forefront of services for patients. Extended roles, new ways of working and changing professional boundaries have given physiotherapists greater opportunities than ever before to practice autonomously. This section will discuss some of the opportunities and challenges that physiotherapists may face currently and in the future.
CURRENT CLIMATE
Services for patients are subject to government reforms, which demand improved quality of care and access. The NHS plan for reform (Department of Health 2000) highlighted that services should be delivered locally, have excellent outcomes, and should be delivered by the most appropriate professional.
Approximately 30% of patients consulting their general practitioner (GP) present with a musculoskeletal condition (DOH 2006a). Physiotherapists have excellent diagnostic and treatment skills for this group of patients, which could be utilised to a greater extent to provide timely management and to assist in the delivery of the ‘18 week pathway’. This Pathway recommends that patients will be seen and treated within 18 weeks from point of referral to definitive care (Department of Health 2006b). Practice Based Commissioning allows clusters of GP practices to purchase services from their locality. The monies saved from purchasing services locally will then be reinvested to improve services further. Physiotherapists working in primary care will have opportunities to engage with local clusters to influence how and where physiotherapy is delivered.
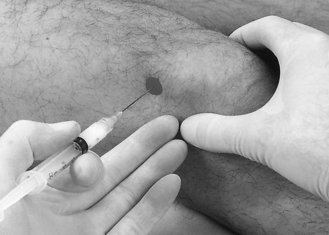
The Musculoskeletal Strategy – doing it differently (Department of Health 2006a) aims to guide where care should be provided. One of the founding principles is that of the ‘Multidisciplinary interface clinic’. This type of clinic acts as a gate-keeper for onward referral to secondary care. Patients are assessed, investigated, diagnosed and referred for treatment, mostly within primary care. Physiotherapists are already working in ‘interface’ style clinics assessing a range of conditions (Stevenson & Hay 2004). They give opportunities for extended clinical reasoning and the development of additional techniques such as injection therapy (Fig. 1.4.1), prescribing and the use of investigations.
OPPORTUNITIES
There are many opportunities for physiotherapists to improve care for their patients and extend professional boundaries (CSP 2008). Ten High Impact Changes (Department of Health 2004a) encouraged the extension of roles and working differently. Directives such as Modernising Medical Careers (Department of Health 2003a, Department of Health 2003b) and European Working Time Directive (Department of Health 2004b) will result in further reduction in doctors’ hours and provide additional opportunities for physiotherapists.
Physiotherapists have been continually extending their skills and scope and in 2001, Consultant Physiotherapy posts were introduced in recognition of this. These posts combined expert clinical practice, leadership, research and education (Department of Health 2001). The posts are one example of combining aspects of different roles to gain the best care for patients. They have been concerned with delivering expert care, service re-design and integrating research into practice (Department of Health 2001). Post holders work across professional boundaries and utilise the best from each to move services forward. Transformational leadership and facilitating change are key aspects of such posts (Manley 2000).
Physiotherapy now has an increasing body of evidence to support practice (e.g. NICE 2008). Evidence for physiotherapy intervention in rheumatoid arthritis suggests hand exercises and joint protection can improve arm function and hand grip (O’ Brien et al 2006). Physiotherapists treating patients with knee osteoarthritis can now be reassured that supervised exercises can improve pain and function when compared to usual care (Hay et al 2006). Where good quality evidence does not exist innovative approaches have been used to engage clinicians in asking appropriate clinical questions, searching the evidence and feeding results back into clinical practice (Stevenson et al 2007). Gaps in the evidence are then highlighted to researchers for consideration for future grant applications.
CHALLENGES
To gain the very best for our patients and be able to develop the services we need to have a great understanding of the political framework within which we sit. More autonomy is being devolved to a local level and it is crucial we understand how to influence local key decision makers around the benefits of physiotherapy and provide them with information that will assist them in their decision making processes. It is clear we need to have good outcome data and robust research evidence to highlight the benefits of our intervention.
In summary, these are both exciting and challenging times for all heath care professionals providing care for patients. Greater political awareness, robust research and patient involvement are key to future success.
1.5 Occupational therapy
Alison Hammond PhD MSc BSc(Hons) DipCOT FCOT Centre for Rehabilitation and Human Performance Research, University of Salford, Greater Manchester and Derby City General Hospital, Derby Hospitals NHS, Foundation Trust, Derby, UK
OCCUPATIONAL THERAPY
The aims of occupational therapy are to:
Occupational therapists (OTs) work collaboratively with clients to achieve ‘occupational balance’ (i.e. a balanced lifestyle) within the context of the person’s illness, disability or other limitations. Rheumatology provides the opportunity to apply the full range of OT physical, functional, environmental, psychological and social interventions.
A major focus is self-management education. Many people with arthritis emphasise the frustration arising from pain, fatigue and difficulty performing daily activities and roles. A community survey of older people with osteoarthritis showed 43% had difficulty with household activities and 33% with hobbies and leisure activities (Jordan et al 2000). Within two years of diagnosis 60% of people with rheumatoid arthritis (RA) have difficulties with household, leisure and social activities (Young et al 2000). Over 50% of people with RA will have difficulty with work (reduced hours, difficulty with work roles, long-term sick leave or giving up) by 10 years, with potentially serious personal and financial consequences (Verstappen et al 2004). Hand function in women with RA is only 40% of normal function within 6 months of diagnosis (Hammond et al 2000). Adjusting to living with arthritis or chronic pain conditions, such as fibromyalgia, and adapting roles and lifestyle can lead to differing emotional reactions (e.g. stress, depression, anger) and impact on relationships.
Interventions focus on: maintaining and improving upper limb function through joint protection, hand exercises, assistive devices and splinting; fatigue management; activity and environmental modifications; activities of daily living training; transport and mobility assessment and advice, benefits and community resources advice; and pain and mood management, e.g. through stress management and relaxation training (NICE 2009). Because work problems occur early, OTs should ensure these are systematically identified by the team and timely OT referrals made for ergonomic assessment and vocational rehabilitation to reduce long-term personal, health and social costs. Clients’ time use and balance of meaningful activities should be explored and avocational counselling also provided (i.e. advice and practical assistance with leisure, voluntary work and adult education opportunities). Loss of valued activities is associated with poorer psychological status, functional and disease outcomes (Katz & Yelin 1994). People with RA performing fewer valued activities (at work, leisure or in the home) are significantly more likely to be depressed, a predictor for poor outcome (and thus higher health costs) (Katz & Neugebauer 2001).
OTs should provide interventions within the context of individual clients’ readiness to make changes in their lives. This can require psychological interventions such as counselling, stress management (e.g. addressing negative thinking), using cognitive-behavioural and motivational strategies, enabling people to explore feelings and beliefs about their condition, its lifestyle impact, their abilities and clarifying goals, to enable concordance with physical and functional interventions. Such approaches are proven effective (NICE 2009). Using a cognitive-behavioural approach is more effective in enabling people to self-manage (Hammond 2004, Hammond & Freeman 2007, Hammond et al 2008, Luqmani et al 2009).
Recent clinical guidelines emphasise skilled rheumatology OT should be available to people with rheumatic conditions (Luqmani et al 2006, 2009, NICE 2009, Scott et al 1998, SIGN 2000, Zhang et al 2007). Rheumatology OT is in short supply nationally. Increasing pressure to reduce time with clients for waiting list management means OTs must ensure evidence-based, effective, efficient practice, such as group cognitive-behavioural patient education programmes, provided collaboratively with physiotherapists and nurses (Hammond et al 2008).
The changing nature of Rheumatology services provides both opportunities and threats. Increasing numbers of clinical specialist posts provide opportunities to: collaborate with academic rheumatology OT researchers furthering the evidence base for rheumatology OT; in developing guidelines; and disseminating specialist practice in ‘hub-and-spoke’ networks working closely with primary care-based OTs. The growth of OT extended role practice can further enhance team care, identifying and addressing clients’ occupational needs rapidly. The increasing shift to primary care-based services poses a risk of losing specialist skills, so all OTs must actively lobby for the continuing need for specialist rheumatology OT, wherever it is located, to enable people with arthritis to lead more meaningful lives.
1.6 Podiatry
Jim Woodburn PhD MPhil BSc FcPod Med School of Health & Social Care, Glasgow Caledonian University, Glasgow, UK
Deborah E. Turner PhD PGCert Medical Ultrasound BSc (Hons) FCPod Med School of Health & Social Care, Glasgow Caledonian University, Glasgow, UK
PODIATRY
The burden of foot disease in rheumatological conditions such as rheumatoid arthritis can be substantial and impact negatively on health related quality of life (ARMA 2007). Impairments such as pain and deformity may be associated directly with primary disease mechanisms such as synovitis and enthesopathy, but complications such as vasculitis also lead to disabling foot problems including ulceration and infection (ARMA 2007). The podiatrist is regarded as a valuable member of the multidisciplinary team however their services are often scarce and poorly accessed (ARMA 2007). Furthermore, foot problems are often neglected during routine clinical assessments further compounding the problem. Requests for podiatry and comfortable footwear are high on priority lists for unmet care for many of these patients (ARMA 2007).
Podiatrists are well-placed to assess, advise and treat patients with foot problems. The overall aims and management can be illustrated by summarising eight patient cases presenting to a typical clinical session in a busy rheumatology outpatient clinic. The first patient is Mrs White, a middle-aged lady with rheumatoid arthritis who presents with well established foot impairments including forefoot pain and deformity and moderately severe flat-footedness, all acquired since the onset of her arthritis. Mrs White attends for routine follow up and has the painful callus overlying her metatarsal heads debrided (removal of tissue to improve the healing potential of the remaining healthy tissue) and her new therapeutic footwear fitted. Mrs White reports immediate improvement in her symptoms as she leaves the clinic.
The next patient is Mr Smith a gentleman with seronegative spondylarthopathy presenting with bilateral plantar heel pain related to enthesopathy. He has responded well to an ultrasound-guided corticosteroid injection and night splint and today is being fitted for a custom made shoe insert. Mr Edwards follows. He is an elderly gentleman with persistent and disabling foot pain associated with hallux rigidus resulting from osteoarthritis at the 1st metatarsophalangeal joint (MTP). On reviewing the case the podiatrist feels he is non responsive to conservative care including orthotics and therapeutic shoes, and non-steroidal antiinflammatory drugs. The podiatrist discusses alternative approaches including surgery and a referral is made to the foot and ankle orthopaedic surgeon.
Before the next patient is seen, one of the rheumatologists brings in Mrs Jones, for an unscheduled consultation. The patient has severe and active RA and is about to start biologic therapy. However, Mrs Jones has a troublesome hammer toe which has a thick callus over the interphalangeal joint. Exquisitely painful the patient has never had this treated. The podiatrist carefully debrides the callused lesion to reveal a small underlying pressure ulcer and, recognising the risks posed by skin infection in patients treated with biologic therapy, recommends delay to systemic therapy until the ulcer is healed. A care plan is developed and the patient booked for follow up foot care.
Mrs Black brings in her 14-year-old daughter, Allison who has polyarticular juvenile idiopathic arthritis. Allison has a troublesome right ankle and is clearly limping as she walks. Following assessment, the podiatrist in consultation with the physiotherapist and paediatric rheumatologist initiates a care plan involving an intra-articular corticosteroid injection to the ankle joint along with joint mobilisation and muscle strengthening, and orthotics to stabilise and control the ankle joint during walking.
The next patient, Mrs Wilson, has been newly diagnosed with RA. Mrs Wilson has just started her methotrexate treatment so has many active joints including those of the feet. The podiatrist carefully provides some personalised advice on joint protection strategies for the feet and dispenses temporary orthoses. The patient’s partner is taught how to assist with daily hygiene including nail and skin care. Mrs Wilson is requested to attend for review after her disease is optimally controlled by medication for follow up care if indicated. To reinforce the advice given in clinic, patient information leaflets on foot problems and care are provided. Our podiatrist finishes her list by carrying out a minor surgical procedure for an RA patient with a chronic painful in growing toenail.
During the clinical session our podiatrist, who works as specialist in rheumatology practice, assists the consultant rheumatologist to undertake an ultrasound guided corticosteroid injection to the subtalar joint. They discuss the merits of entering the joint via the sinus tarsi over a medial approach, as well as indications and contra-indications of the technique. This takes place as part of a clinical mentoring scheme as the podiatrist is undertaking training on ultrasound and intra-articular joint injections as part of extended scope practice whilst working towards a consultant grade post.
Underpinning all of these cases are the primary aims of podiatry care to relieve pain, maintain or improve function and to maintain optimal tissue viability and provide wound management. In our examples above our podiatrist is working effectively as part of the multidisciplinary team and is advancing their own knowledge and skills to provide better and more effective patient care. Podiatrists are experts in assessing and evaluating mechanical foot problems and gait as well as understanding underlying systemic and local disease factors that manifest in the feet as part of the rheumatic diseases. They provide physical treatment strategies including orthotics and footwear, nail-care, callus debridement and wound management, injection therapy and minor surgical techniques. Patient education is an integral part of foot care for patients with rheumatic diseases and podiatrists are able to provide advice as well as assistance and training to adapt, self-manage and cope with disabling foot pain. Podiatry, Biomechanics and the rheumatology foot is further detailed in Chapter 13.
1.7 Health psychology
Elizabeth D. Hale BA(Hons), MSc, CPsychol Dudley Group of Hospitals NHS Trust, Russells Hall Hospital, Dudley and University of Birmingham, School of Sport and Exercise Sciences, Birmingham, UK
Gareth J. Treharne BSc (Hons), PhD University of Otago, Aotearoa/New Zealand and Dudley Group of Hospitals NHS Trust Russells Hall Hospital Dudley, UK
HEALTH PSYCHOLOGY
WHAT IS PSYCHOLOGY? AND WHAT IS HEALTH PSYCHOLOGY SPECIFICALLY?
The purview of psychology has been defined in many ways over the years. A dictionary of psychology states that ‘psychology simply cannot be defined’ (Reber 1985). Those who have attempted to define this elusive subject use phrasings akin to ‘the science of mind and behaviour’ (Gross 1992). The role of psychologists is still commonly misunderstood by health professionals and the general public alike, often provoking mistrust.
This experience of working or studying within a misunderstood discipline might be something that you identify with given that physiotherapy, occupational therapy and advanced specialist nursing are commonly misconstrued professions (see Study activity). One thing that is certain is that the question “And what do you do?” is one which we try to avoid answering at social gatherings. Answering “I’m a psychologist” is usually followed by “Oh, I’d better be careful then!” or “So can you tell what I’m thinking?” To lay these contentions to rest, we are not ‘analysing’ your behaviour and we are not ‘mind readers’. The serious point that this issue raises is that it is very relevant to understand the confusion and possible discomfort that your patients may feel when you suggest they could benefit from a referral to a psychologist, or if you mention that you will be applying a psychologically-based intervention yourself.
The formal discipline of psychology is over 130 years old. The first psychology laboratory was founded in 1875 at Harvard University in the USA by William James (Kim 2006). Four years later a further psychology laboratory was founded in Leipzig (Germany) by Wilhelm Wundt, who is usually credited as the founding father of modern psychology (Kim 2006). Interestingly, although both Wundt and James were trained in medicine, the application of psychological theory and methods to health and illness is relatively new, particularly in the UK (Division of Health Psychology 2009). In the US the two fields called behavioural medicine and health psychology were formed as recently as the 1970s. Behavioural medicine considers the role of psychology in medicine and includes a wide range of disciplines in its membership and research (Sarafino 1990). Health psychology is a subfield of psychology concerned with physical health. In the UK, health psychology only became officially recognised as a full Division of The British Psychological Society in 1998 when the British Psychological Society’s Special Interest Group in Health Psychology was redesignated the Division of Health Psychology and became responsible for the accreditation of courses and training for health psychologists, that is, those psychologists wanting to specialise in aspects of physical health and health promotion (Division of Health Psychology 2009), as detailed in Box 1.7.1.
BOX 1.7.1 Frequently asked question: what is a health psychologist?
In the UK a health psychologist is someone who specialises in the psychology of physical health, having completed accredited undergraduate, masters and doctoral degree programmes (or equivalent). Additionally, evidence of competency in several specified areas (e.g. research, intervention, consultancy) will lead to the title Chartered Health Psychologist and the titular suffix CPsychol, denoting someone who can practice health psychology without further directive supervision. (The need for professional support supervision is, of course, on-going). More information about the role of Health Psychologists is presented by the Division of Health Psychology (2009) and Hale et al (2007).
The interests and scope of health psychology in the UK remains similar to those originally formulated in the US nearly 30 years earlier; health psychologists apply psychological research and methods to:
APPLYING HEALTH PSYCHOLOGY RESEARCH
There are currently over 650 active chartered psychologists in the UK who list health as one of their subspecialties (if not their only one; see British Psychological Society 2009). To our knowledge only a few health psychologists have a special interest in rheumatology and even fewer who work in an integrated role combining formal research and clinical practice. The generation and application of health psychology research and practice should be an interdisciplinary and collaborative enterprise, utilising a variety of research methodologies. For example, we have had input on a project by a rheumatology nurse specialist colleague of ours who investigated the experiences of women with rheumatoid arthritis (RA) and how this impacts upon their role as a young mother (Mitton et al 2007). Other such collaborations are in action, for example between a team including psychologists, a physiotherapist, a biostatistician and a medical doctor who have used their joint expertise to examine the illness perceptions associated with health and behavioural outcomes in people with musculoskeletal hand problems (Hill et al 2007).
As indicated in our brief background to psychology, psychologists have been concerned from the very start that the discipline should be taken seriously and on a par with the natural sciences, hence the early establishment of psychological ‘laboratories’. The emphasis was, and continues to be, largely focused upon objective measurement and quantification (Hale et al 2008). The difficulties for psychologists have always been in how to measure something that you cannot objectively see, like motivation, anxiety or depression. Applying the same rigour and methodology as seen in the natural sciences, psychologists continue to find novel, reliable and validated ways of measuring these concepts. Psychology is not ‘mind reading’; there are no tricks or special skills that allow us to know how patients are thinking or are likely to behave, unless there is good research evidence to support it. Although it is true to say that psychological research has been dominated by this quantitative approach, there has recently been a growth of interest in the qualitative methodologies, particularly within health psychology and health based research (Hale et al 2008). Adopting the same rigorous approach to research whilst using, for example, structured or semi-structured interviews can provide in-depth perspectives of an experience which might provide knowledge that helps to illuminate a problem or re-shape healthcare policy or practice (Hale et al 2008). In essence practitioners need to critically read and evaluate the existing research literature (the evidence) on the problem they are addressing or the intervention they are intending to implement. New local practice might arise from this evaluation and synthesis. For example, a recent meta-analytic review by Dixon et al (2007) suggested that psychosocial interventions can boost the active coping efforts that people with arthritis engage in. They used the technique called meta-analysis, where the statistical effects seen across several different studies are combined, and found that these interventions are most effective for improving anxiety and joint swelling (recorded as joint counts). Furthermore, they found that depression, functional ability and pain self-efficacy can be improved by psychological intervention but not as consistently across the studies they reviewed. Information on measuring patient reported outcomes such as these can be seen in Chapter 4. We will go on to explain some of these concepts, like anxiety and coping in more detail (see Chs 4-6).
This section has introduced psychology and more specifically health psychology and its role in rheumatology. Concepts and interventions used are explained in more detail in Chapter 11.
1.8 A brief introduction to evidence-based medicine
Adrian White MA MD BM Bch General Practice and Primary Care, Peninsula Medical School, Plymouth, UK
A BRIEF INTRODUCTION TO EVIDENCE-BASED MEDICINE
Patients should receive the best possible treatment that is available for their condition. Evidence based medicine (EBM) is a particular way of deciding what is best. It was first described in the early 1990s and has come to dominate medical practice. While the EBM approach is clearly ‘correct’, it does have its limitations, and it should not be applied on its own without considering the context, particularly the needs of the individual patient. We shall briefly discuss what EBM involves, and make some suggestions on how it is best applied.
The essential process in choosing a treatment for a patient is: look for the highest quality of evidence on which of the available treatments offer the greatest benefits compared with its harms. The different types of study can be arranged in a hierarchy of their ‘quality’ (Box 1.8.1), which is based on the scientific rigour of the study. A study that is ‘rigorous’ is done in a way that the results are not influenced by what the researchers believed beforehand. The most rigorous design is the randomised controlled trial (RCT) and this is regarded as the ‘gold standard’.
Box 1.8.1 Hierarchy of evidence
 Moderate evidence: one relevant, high quality randomized controlled trial and one or more relevant, low quality randomized controlled trials
Moderate evidence: one relevant, high quality randomized controlled trial and one or more relevant, low quality randomized controlled trialsThere are various ways of grading the evidence according to the amount of evidence and its quality, for making decisions. For example, in one system evidence from systematic reviews is graded as level 1a, evidence from one randomized controlled trial as level 1b, down to evidence from expert committee reports which is level IV (Bombadier et al 2003). However, health care is not a soulless process that depends purely on reading systematic reviews. When it comes to putting EBM into practice, other factors must be taken into account, particularly the wishes of the patient and the practitioner’s clinical judgement in this particular case.
Some of the limitations of EBM are obvious. It will take a huge amount of work to produce randomized controlled trials, let alone systematic reviews, for every possible treatment for every condition. Very often, high quality evidence simply is not available, and a clinical decision has to be made on less rigorous evidence. The fact that randomized controlled trials and systematic reviews have not been done on a particular treatment does not mean it does not work! This is usually summarised in the phrase: Absence of evidence of an effect is not the same as evidence of absence of an effect. When EBM is applied thoughtlessly, useful interventions are likely to be rejected, and many patients will be denied benefit. So, while waiting for the rigorous studies, the principle of EBM is to look for the highest quality evidence available – even if it is only a report from another patient who has benefitted from a particular treatment. The final decision on treatment also has to take other factors into account, such as whether its mechanism is plausible, what it costs, and its safety record.
There are other limitations to EBM. Randomized controlled trials are often done in very restricted circumstances, for example in patients within a certain age range who do not have any other medical condition. The conclusions from these randomized controlled trials may not be applicable to a different group of patients. Additionally, although systematic reviews are supposed to be consistent and reliable, sometimes different reviews reach different conclusions.
Not all decisions require the same level of evidence. For example, taxpayers will want health policies that are based on good evidence of effectiveness, safety and cost. More subtly, a clinician might judge that there is enough evidence to support or condone a patient’s choice for a particular treatment, but not enough to recommend the treatment to someone else who has not considered it. It is often said of complementary treatments that the patient’s preference might be crucial to success, but this is probably just as true of many conventional treatments that we use every day.
In summary, although EBM may be the best way in theory to choose between different treatments, in practice it will often be necessary to make a case that the ‘right’ treatment for this particular patient is not the one that is supported by the highest level of evidence. The following chapters have considered the best available evidence whenever possible.
ARMA website accessed 10/11/08 http://www.arma.uk.net.
Chartered Society of Physiotherapy accessed 10/11/08 http://www.csp.org.uk
Department of Health accessed 10/11/08 http://www.dh.gov.uk/en/index.htm.
Arthritis Research Campaign National Primary Care Web site, Critically Appraised Topics accessed 10/11/08
http://www.keele.ac.uk/research/pchs/pcmrc/dissemination/cat/index/htm.
http://www.rcgp-curriculum.org.uk. Accessed March 2009.
References and further reading
ARMA, 2007. Standards of care for people with musculoskeletal foot problems. http://www.arma.uk.net/ (accessed 10.11.08.).
Arthur V., Clifford C. Rheumatology: the expectations and preferences of patients for their follow up monitoring care: a qualitative study to determine the dimensions of patient satisfaction. J. Clin. Nurs.. 2004;13:234-242.
BHPR, 2004. The role of the rheumatologist. Roles in rheumatology British Health Professionals in Rheumatology on line resource http://www.rheumatology.org.uk/bhpr/rolesinrheum/ (accessed March 2009.).
Bird H.A. Divided rheumatology care: the advent of the rheumatology practitioner? Ann. Rheum. Dis.. 1983;42:354-355.
Bombardier, C., Bouter, L.M., de Bie, R.A., et al., 2003. Back Group. In: The Cochrane Library issue 3. UpdateSoftware, Oxford.
British Psychological Society, 2009. Register of Chartered Psychologists. Online. Available: http://www.bps.org.uk/e-services/find-a-psychologist/register.cfm/ (accessed September 2009)
Bunn, F., Byrne, G., Kendall, S., 2004. Telephone consultation and triage: effects on health care use and patient satisfaction. Cochrane Database Systematic Reviews CD004180.
Bunn F., Byrne G., Kendall S. The effects of telephone consultation and triage on healthcare use and patient satisfaction: a systematic review. Brit. J. Gen. Pract.. 2005;55:956-961.
Carr, A., 2001. Defining the extended clinical role for allied health professionals in rheumatology. Chesterfield. Arthritis Research Campaign conference proceedings no 12.
CSP, 2008. Charting the future of physiotherapy. Chartered Society of Physiotherapy 14 Bedford Row London WC1R 4ED http://www.csp.org.uk/director/members/libraryandpublications/csppublications.cfm?item_id=56853683ED91C7CC76535A867964FCE6/ (accessed March 2009.).
Department of Health. NHS Plan: A plan for investment a plan for reform. Department of Health London; 2000. http://www.dh.gov.uk/en/Publicationsandstatistics/Publications/PublicationsPolicyAndGuidance/DH_4002960/ (accessed March 2009.).
Department of Health. Advanced Letter PAM (PTA) Allied healthcare professionals consultant posts. Department of Health London; 2001. http://www.dh.gov.uk/en/Publicationsandstatistics/Lettersandcirculars/Dearcolleagueletters/DH_4005723/ (accessed March 2009.)
Department of Health. Modernising Medical Careers. Department of Health London; 2003. http://www.dh.gov.uk/en/Publicationsandstatistics/Publications/PublicationsPolicyAndGuidance/DH_4010460/ (accessed March 2009.).
Department of Health. The Foundation Committee of the Academy of Medical Royal Colleges in Co-operation with Modernising Medical Careers in the Department of Heath. Department of Health London; 2003. http://www.dh.gov.uk/en/Publicationsandstatistics/Lettersandcirculars/Dearcolleagueletters/DH_4003085/ (accessed March 2009.).
Department of Health. 10 High Impact Changes. Department of Health London; 2004. http://www.dh.gov.uk/en/Publicationsandstatistics/Bulletins/theweek/Chiefexecutivebulletin/DH_4088866/ (accessed March 2009.).
Department of Health. A Compendium of solutions to implement the working time directive for Doctors in training. Department of Health London; 2004. http://www.dh.gov.uk/en/Publicationsandstatistics/Publications/PublicationsPolicyAndGuidance/DH_4082634/ (accessed March 2009.).
Department of Health. The Musculoskeletal Services Framework A Joint responsibility: doing it differently. Department of Health London; 2006. http://www.dh.gov.uk/en/Publicationsandstatistics/Publications/PublicationsPolicyAndGuidance/DH_4138413/ (accessed March 2009.).
Department of Health. Tackling hospital waiting the 18-week patient pathway. An implementation Framework. Department of Health London; 2006. http://www.dh.gov.uk/en/Publicationsandstatistics/Publications/PublicationsPolicyAndGuidance/DH_4134668/ (accessed March 2009.).
Division of Health Psychology, 2009. What is Health Psychology? Online. Available: http://www.health-psychology.org.uk/dhp_home.cfm (accessed September 2009).
Dixon K.E., Keefe F.J., Scipio C.D., et al. Psychological interventions for arthritis pain management in adults: a meta-analysis. Health Psychol.. 2007;26(3):241-250.
Greener I., Mannion R. Does practice based commissioning avoid the problems of fundholding? Brit. Med. J.. 2006;333:1168-1170.
Gross R. Psychology: The Science of Mind and Behaviour, third ed. London: Hodder & Stoughton, 1992.
Hammond A., Kidao R., Young A. Hand Impairment and Function in early Rheumatoid Arthritis. Arthritis and Rheumatism. 2000;43(Suppl. 9):S285.
Hammond A., Freeman K. One year outcomes of a randomised controlled trial of an educational-behavioural joint protection programme for people with rheumatoid arthritis. Rheumatology. 2001;40:1044-1051.
Hammond A. What is the role of the occupational therapist? Best Pract. Res. Cl. Rh.. 2004;18:491-505.
Hammond A., Bryan J., Hardy A., et al. Effects of a modular behavioural arthritis education programme: a pragmatic parallel-group randomized controlled trial. Rheumatology. 2008;47(11):1712-1718.
Hale E.D., Treharne G.J., Peacock S., et al. Defining the role of health psychologists in rheumatology. Rheumatology. 2007;46(Suppl. 1):i148. Abstract
Hale E.D., Treharne G.J., Kitas G.D. Qualitative methodologies I: asking research questions with reflexive insight. Musculoskeletal Care. 2008;6:86-96.
Hay E., Campbell A., Linney S., et al. Musculoskeletal GPwSI Working Group. Development of a competency framework for general practitioners with a special interest in musculoskeletal/rheumatology practice. Rheumatology. 2007;46:360-362.
Hay E.M., Foster N.E., Thomas E., et al. Effectiveness of community physiotherapy and enhanced pharmacy review for knee pain in people aged over 55 presenting to primary care: pragmatic randomised trial. Brit. Med. J.. 2006;333(7576):995.
Hill J. A nurse practitioner rheumatology clinic. Nurs. Stand.. 1992;7:35-37.
Hill J., Bird H., Lawton C., et al. An evaluation of the effectiveness, safety, and acceptability of a nurse practitioner in a rheumatology outpatient clinic. Brit. J. Rh.. 1994;33:283-288.
Hill S., Dziedzic K., Thomas E., et al. The illness perceptions associated with health and behavioural outcomes in people with musculoskeletal hand problems: findings from the North Staffordshire Osteoarthritis Project (NorStOP). Rheumatology. 2007;46(6):944-951.
Hooper H., Ryan S., Hassell A. The role of social comparison in coping with rheumatoid arthritis: an interview study. Musculoskeletal Care. 2004;2:195-206.
Hosie G. Teaching rheumatology in primary care. Ann. Rheum. Dis.. 2000;59:500-503.
Jordan J.M., Bernard S.L., Callahan L.F., et al. Self-reported arthritis-related disruptions in sleep and daily life and the use of medical, complementary and self-care strategies for Arthritis: The National Survey of Self-Care and Ageing. Arch. Fam. Med.. 2000;9:143-149.
Jordan K., Clarke A., Symmons D., et al. Measuring disease prevalence: a comparison of musculoskeletal disease using four general practice consultation databases. Brit. J. Gen. Pract.. 2007;57:7-14.
Katz P.P., Neugebauer A. Does satisfaction with abilities mediate the relationship between the impact of rheumatoid arthritis on valued activities and depression? Arthrit. Care Res.. 2001;45:263-269.
Katz P., Yelin E.H. Life activities of persons with rheumatoid arthritis with and without depressive symptoms. Arthrit. Care Res.. 1994;7:69-77.
Kim A., 2006 Wilhelm Maximilian Wundt. Stanford Encyclopedia of Philosophy. Online. Available: http://www.plato.stanford.edu/entries/wilhelm-wundt/ 29 Jun 2007
Lattimer V., Smith H., Hungin P., et al. Future provision of out of hours primary medical care: a survey with two general practitioner research networks. Brit. Med. J.. 1996;312:352-356.
Luqmani R., Hennel S., Estrach C., et al. British Society for Rheumatology and British Health Professionals in Rheumatology Guidelines for the management of rheumatoid arthritis (the first 2 years). Rheumatology. 2006;45(9):1167-1169.
Luqmani, R., Hennel, S., Estrach, C., et al. 2009. British Society for Rheumatology and British Health Professionals in Rheumatology Guidelines for the management of rheumatoid arthritis (after the first 2 years). Rheumatology doi:10.1093/rheumatology/ken450b
McCormick, A., Fleming, D., Charlton, J., 1995. Morbidity statistics from general practice. 4th national study 1991-1992. London, HMSO.
Manley K. Organisational culture and consultant nurse outcomes: part 1 organisational culture. Nurs. Stand.. 2000;14:34-38.
Mitton D.L., Treharne G.J., Hale E.D., et al. The health and life experiences of mothers with rheumatoid arthritis: a phenomenological study. Musculoskeletal Care. 2007;5:191-205.
Mooney, J., 1996. Audit of rheumatology nurse outreach clinics. Rheumatology in Practice. Winter 18-20.
NICE, 2008. National Institute for Health and Clinical Excellence. Osteoarthritis: national clinical guideline for care and management in adults. http://www.nice.org.uk/CG059www.nice.org.uk/CG059/ (accessed March 2009.).
NICE (National Institute of Clinical Excellence), 2009. Rheumatoid arthritis: national clinical guideline for management and treatment in adults. Ch. 6.3 Occupational Therapy. p87-94 http://www.nice.org.uk/nicemedia/pdf/CG59NICEguideline.pdf/. (accessed March 2009.).
O’Brien A.V., Jones P., Mullis R., et al. Conservative hand therapy treatments in rheumatoid arthritis–a randomized controlled trial. Rheumatology. 2006;45:577-583.
Reber A.S. Dictionary of Psychology, third ed. London: Penguin, 1985.
Ryan S., Hassell A.B., Lewis M., et al. A study into the impact of the expert nurse on the patients attending a drug monitor clinic. J. Adv. Nurs.. 2006;53:277-286.
Ryan S., Hill J. A survey of practice in nurse led rheumatoid arthritis clinics. Rheumatology. 2004;43(Suppl. 2):411.
Sarafino E.P. Health Psychology: Biopsychosocial Interactions, third ed. New York: John Wiley, 1990.
Scott D.L., Shipley M., Dawson A., et al. The Clinical Management of Rheumatoid Arthritis and Osteoarthritis: Strategies for Improving Clinical Effectiveness. Brit. J. Rheumat.. 1998;37:546-554.
Shaul M. From early twinges to mastery: the process of adjustment in living with rheumatoid arthritis. Arthrit. Care Res.. 1995;47:525-531.
SIGN, 2000. Management of Early Rheumatoid Arthritis. SIGN Publication No. 48 ISBN 1899893 37 7 http://www.sign.ac.uk/guidelines/fulltext/48/index.html/. (accessed March 2009.).
Stevenson K., Bird L., Sarigiovannis P., et al. A new multidisciplinary approach to integrating best evidence into musculoskeletal practice. J. Eval. Clin. Pract.. 2007;13:703-708.
Thwaites C. Rheumatology telephone advice lines. Musculoskeletal Care. 2004;2:120-126.
Verstappen S.M.M., Jacobs J.W.G., Verkleij H., et al. Overview of work disability in patients with rheumatoid arthritis as observed in transversal and longitudinal studies. Ann. Rheum. Dis.. 2004;51(3):488-497.
Vliet Vlieland T.P., Breedveld F.C., Hazes J.M. The two-year follow-up of a randomized comparison of in-patient multidisciplinary team care and routine out-patient care for active rheumatoid arthritis. Brit.J. Rheumat.. 1997;36(1):82-85.
Wilson Barnett J. Key functions in nursing. Lampada. 1985;2:35-39.
Young A., Dixey J., Cox N., et al. How does functional disability in early rheumatoid arthritis (RA) affect patients and their lives? Results of 5 years of follow-up in 732 patients from the Early RA Study (ERAS). Rheumatology. 2000;39:603-611.
Zhang W., Doherty M., Leeb B.F., et al. EULAR Evidence based recommendations for the management of hand osteoarthritis: report of a task force of the EULAR Standing Committee for International Clinical Studies including Therapeutics (ESCISIT). Ann. Rheum. Dis.. 2007;66:377-388.