CHAPTER 1 Properties and Overview of Immune Responses
The term immunity is derived from the Latin word immunitas, which referred to the protection from legal prosecution offered to Roman senators during their tenures in office. Historically, immunity meant protection from disease and, more specifically, infectious disease. The cells and molecules responsible for immunity constitute the immune system, and their collective and coordinated response to the introduction of foreign substances is called the immune response.
The physiologic function of the immune system is defense against infectious microbes. However, even noninfectious foreign substances can elicit immune responses. Furthermore, mechanisms that normally protect individuals from infection and eliminate foreign substances are also capable of causing tissue injury and disease in some situations. Therefore, a more inclusive definition of the immune response is a reaction to components of microbes as well as to macromolecules, such as proteins and polysaccharides, and small chemicals that are recognized as foreign, regardless of the physiologic or pathologic consequence of such a reaction. Under some situations, even self molecules can elicit immune responses (so-called autoimmune responses). Immunology is the study of immune responses in this broader sense and of the cellular and molecular events that occur after an organism encounters microbes and other foreign macromolecules.
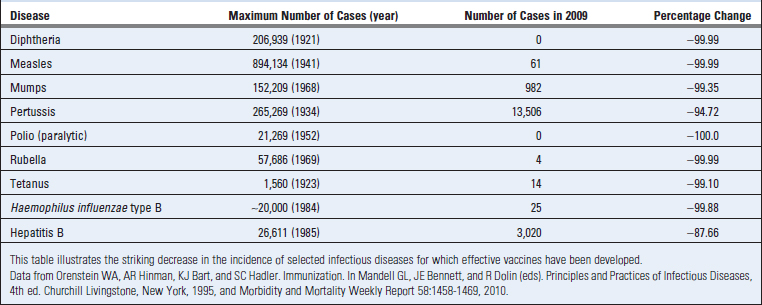
Historians often credit Thucydides, in the fifth century bc in Athens, as having first mentioned immunity to an infection that he called plague (but that was probably not the bubonic plague we recognize today). The concept of protective immunity may have existed long before, as suggested by the ancient Chinese custom of making children resistant to smallpox by having them inhale powders made from the skin lesions of patients recovering from the disease. Immunology, in its modern form, is an experimental science, in which explanations of immunologic phenomena are based on experimental observations and the conclusions drawn from them. The evolution of immunology as an experimental discipline has depended on our ability to manipulate the function of the immune system under controlled conditions. Historically, the first clear example of this manipulation, and one that remains among the most dramatic ever recorded, was Edward Jenner’s successful vaccination against smallpox. Jenner, an English physician, noticed that milkmaids who had recovered from cowpox never contracted the more serious smallpox. On the basis of this observation, he injected the material from a cowpox pustule into the arm of an 8-year-old boy. When this boy was later intentionally inoculated with smallpox, the disease did not develop. Jenner’s landmark treatise on vaccination (Latin vaccinus, of or from cows) was published in 1798. It led to the widespread acceptance of this method for inducing immunity to infectious diseases, and vaccination remains the most effective method for preventing infections (Table 1-1). An eloquent testament to the importance of immunology was the announcement by the World Health Organization in 1980 that smallpox was the first disease that had been eradicated worldwide by a program of vaccination.
Since the 1960s, there has been a remarkable transformation in our understanding of the immune system and its functions. Advances in cell culture techniques (including monoclonal antibody production), immunochemistry, recombinant DNA methodology, and x-ray crystallography and the creation of genetically altered animals (especially transgenic and knockout mice) have changed immunology from a largely descriptive science into one in which diverse immune phenomena can be explained in structural and biochemical terms. In this chapter, we outline the general features of immune responses and introduce the concepts that form the cornerstones of modern immunology and that recur throughout this book.
Innate and Adaptive Immunity
Defense against microbes is mediated by the early reactions of innate immunity and the later responses of adaptive immunity (Fig. 1-1 and Table 1-2). Innate immunity (also called natural or native immunity) provides the early line of defense against microbes. It consists of cellular and biochemical defense mechanisms that are in place even before infection and are poised to respond rapidly to infections. These mechanisms react to microbes and to the products of injured cells, and they respond in essentially the same way to repeated infections. The principal components of innate immunity are (1) physical and chemical barriers, such as epithelia and antimicrobial chemicals produced at epithelial surfaces; (2) phagocytic cells (neutrophils, macrophages), dendritic cells, and natural killer (NK) cells; (3) blood proteins, including members of the complement system and other mediators of inflammation; and (4) proteins called cytokines that regulate and coordinate many of the activities of the cells of innate immunity. The mechanisms of innate immunity are specific for structures that are common to groups of related microbes and may not distinguish fine differences between microbes.
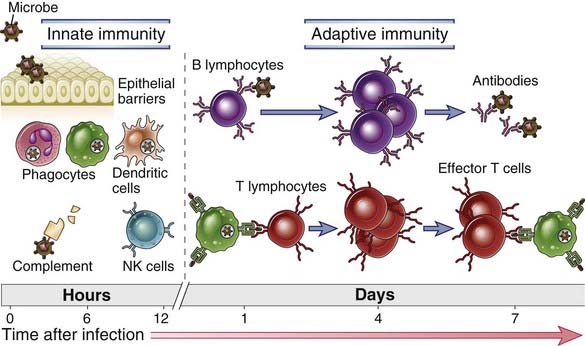
FIGURE 1–1 Innate and adaptive immunity.
The mechanisms of innate immunity provide the initial defense against infections. Adaptive immune responses develop later and consist of activation of lymphocytes. The kinetics of the innate and adaptive immune responses are approximations and may vary in different infections.
TABLE 1–2 Features of Innate and Adaptive Immunity
| Innate | Adaptive | |
|---|---|---|
| Characteristics | ||
| Specificity | For molecules shared by groups of related microbes and molecules produced by damaged host cells | For microbial and nonmicrobial antigens |
| Diversity | Limited; germline encoded | Very large; receptors are produced by somatic recombination of gene segments |
| Memory | None | Yes |
| Nonreactivity to self | Yes | Yes |
| Components | ||
| Cellular and chemical barriers | Skin, mucosal epithelia; antimicrobial molecules | Lymphocytes in epithelia; antibodies secreted at epithelial surfaces |
| Blood proteins | Complement, others | Antibodies |
| Cells | Phagocytes (macrophages, neutrophils), natural killer cells | Lymphocytes |
In contrast to innate immunity, there are other immune responses that are stimulated by exposure to infectious agents and increase in magnitude and defensive capabilities with each successive exposure to a particular microbe. Because this form of immunity develops as a response to infection and adapts to the infection, it is called adaptive immunity. The defining characteristics of adaptive immunity are exquisite specificity for distinct molecules and an ability to “remember” and respond more vigorously to repeated exposures to the same microbe. The adaptive immune system is able to recognize and react to a large number of microbial and nonmicrobial substances. In addition, it has an extraordinary capacity to distinguish between different, even closely related, microbes and molecules, and for this reason it is also called specific immunity. It is also sometimes called acquired immunity, to emphasize that potent protective responses are “acquired” by experience. The main components of adaptive immunity are cells called lymphocytes and their secreted products, such as antibodies. Foreign substances that induce specific immune responses or are recognized by lymphocytes or antibodies are called antigens.
Mechanisms for defending the host against microbes are present in some form in all multicellular organisms. These mechanisms constitute innate immunity. The more specialized defense mechanisms that constitute adaptive immunity are found in vertebrates only. Two functionally similar but molecularly distinct adaptive immune systems developed at different times in evolution. About 500 million years ago, jawless fish, such as lampreys and hagfish, developed a unique immune system containing diverse lymphocyte-like cells that may function like lymphocytes in more advanced species and even responded to immunization. The antigen receptors on these cells were variable leucine-rich receptors that were capable of recognizing many antigens but were distinct from the antibodies and T cell receptors that appeared later in evolution. Most of the components of the adaptive immune system, including lymphocytes with highly diverse antigen receptors, antibodies, and specialized lymphoid tissues, evolved coordinately within a short time in jawed vertebrates (e.g., sharks), about 360 million years ago. The immune system has also become increasingly specialized with evolution.
Innate and adaptive immune responses are components of an integrated system of host defense in which numerous cells and molecules function cooperatively. The mechanisms of innate immunity provide effective initial defense against infections. However, many pathogenic microbes have evolved to resist innate immunity, and their elimination requires the more powerful mechanisms of adaptive immunity. There are many connections between the innate and adaptive immune systems. The innate immune response to microbes stimulates adaptive immune responses and influences the nature of the adaptive responses. Conversely, adaptive immune responses often work by enhancing the protective mechanisms of innate immunity, making them capable of effectively combating pathogenic microbes.
Types of Adaptive Immune Responses
There are two types of adaptive immune responses, called humoral immunity and cell-mediated immunity, that are mediated by different components of the immune system and function to eliminate different types of microbes (Fig. 1-2). Humoral immunity is mediated by molecules in the blood and mucosal secretions, called antibodies, which are produced by cells called B lymphocytes (also called B cells). Antibodies recognize microbial antigens, neutralize the infectivity of the microbes, and target microbes for elimination by various effector mechanisms. Humoral immunity is the principal defense mechanism against extracellular microbes and their toxins because secreted antibodies can bind to these microbes and toxins and assist in their elimination. Antibodies themselves are specialized and may activate different effector mechanisms. For example, different types of antibodies promote the ingestion of microbes by host cells (phagocytosis), bind to and trigger the release of inflammatory mediators from cells, and are actively transported into the lumens of mucosal organs and through the placenta to provide defense against ingested and inhaled microbes and against infections of the newborn, respectively. Cell-mediated immunity, also called cellular immunity, is mediated by T lymphocytes (also called T cells). Intracellular microbes, such as viruses and some bacteria, survive and proliferate inside phagocytes and other host cells, where they are inaccessible to circulating antibodies. Defense against such infections is a function of cell-mediated immunity, which promotes the destruction of microbes residing in phagocytes or the killing of infected cells to eliminate reservoirs of infection.
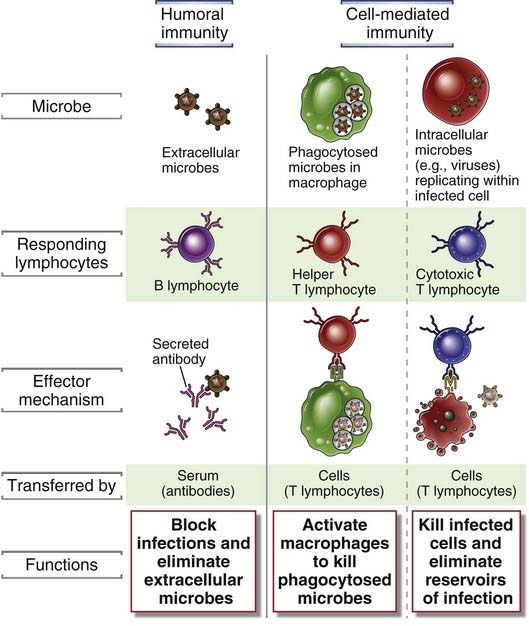
FIGURE 1–2 Types of adaptive immunity.
In humoral immunity, B lymphocytes secrete antibodies that prevent infections by and eliminate extracellular microbes. In cell-mediated immunity, helper T lymphocytes activate macrophages to kill phagocytosed microbes or cytotoxic T lymphocytes directly destroy infected cells.
Protective immunity against a microbe is usually induced by the host’s response to the microbe (Fig. 1-3). The form of immunity that is induced by exposure to a foreign antigen is called active immunity because the immunized individual plays an active role in responding to the antigen. Individuals and lymphocytes that have not encountered a particular antigen are said to be naive, implying that they are immunologically inexperienced. Individuals who have responded to a microbial antigen and are protected from subsequent exposures to that microbe are said to be immune.
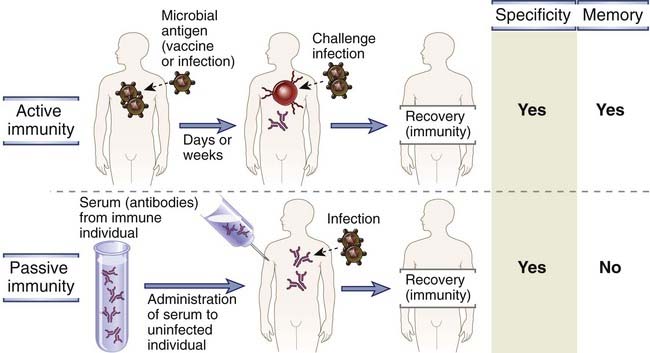
FIGURE 1–3 Active and passive immunity.
Active immunity is conferred by a host response to a microbe or microbial antigen, whereas passive immunity is conferred by adoptive transfer of antibodies or T lymphocytes specific for the microbe. Both forms of immunity provide resistance to infection and are specific for microbial antigens, but only active immune responses generate immunologic memory. Cell transfers can be done only between genetically identical donor and recipient (e.g., inbred mice) to avoid rejection of the transferred cells.
Immunity can also be conferred on an individual by transferring serum or lymphocytes from a specifically immunized individual, a process known as adoptive transfer in experimental situations (see Fig. 1-3). The recipient of such a transfer becomes immune to the particular antigen without ever having been exposed to or having responded to that antigen. Therefore, this form of immunity is called passive immunity. Passive immunization is a useful method for conferring resistance rapidly, without having to wait for an active immune response to develop. A physiologically important example of passive immunity is the transfer of maternal antibodies to the fetus, which enables newborns to combat infections before they develop the ability to produce antibodies themselves. Passive immunization against toxins by the administration of antibodies from immunized animals is a lifesaving treatment for potentially lethal infections, such as tetanus, and snake bites. The technique of adoptive transfer has also made it possible to define the various cells and molecules that are responsible for mediating specific immunity. In fact, humoral immunity was originally defined as the type of immunity that could be transferred to unimmunized, or naive, individuals by antibody-containing cell-free portions of the blood (i.e., plasma or serum) obtained from previously immunized individuals. Similarly, cell-mediated immunity was defined as the form of immunity that can be transferred to naive animals with cells (T lymphocytes) from immunized animals but not with plasma or serum.
The first experimental demonstration of humoral immunity was provided by Emil von Behring and Shibasaburo Kitasato in 1890. They showed that if serum from animals that had recovered from diphtheria infection was transferred to naive animals, the recipients became specifically resistant to diphtheria infection. The active components of the serum were called antitoxins because they neutralized the pathologic effects of the diphtheria toxin. This result led to the treatment of otherwise lethal diphtheria infection by the administration of antitoxin, an achievement that was recognized by the award of the first Nobel Prize in Physiology or Medicine to von Behring. In the early 1900s, Paul Ehrlich postulated that immune cells use receptors, which he called side chains, to recognize microbial toxins and subsequently secrete these receptors to combat microbes. He also coined the term antibodies (antikörper in German) for the serum proteins that bound toxins, and substances that stimulated the production of antibodies were called antigens. The modern definition of antigens includes substances that bind to specific lymphocyte receptors, whether or not they stimulate immune responses. According to strict definitions, substances that stimulate immune responses are called immunogens. The properties of antibodies and antigens are described in Chapter 5. Ehrlich’s concepts are a remarkably prescient model for the function of B cells in humoral immunity. This early emphasis on antibodies led to the general acceptance of the humoral theory of immunity, according to which host defense against infections is mediated by substances present in body fluids (once called humors).
The cellular theory of immunity, which stated that host cells are the principal mediators of immunity, was championed initially by Elie Metchnikoff. His demonstration of phagocytes surrounding a thorn stuck into a translucent starfish larva, published in 1883, was perhaps the first experimental evidence that cells respond to foreign invaders. Ehrlich and Metchnikoff shared the Nobel Prize in 1908, in recognition of their contributions to establishing these fundamental principles of immunity. Sir Almroth Wright’s observation in the early 1900s that factors in immune serum enhanced the phagocytosis of bacteria by coating the bacteria, a process known as opsonization, lent support to the belief that antibodies prepared microbes for ingestion by phagocytes. These early “cellularists” were unable to prove that specific immunity to microbes could be mediated by cells. The cellular theory of immunity became firmly established in the 1950s, when it was shown that resistance to an intracellular bacterium, Listeria monocytogenes, could be adoptively transferred with cells but not with serum. We now know that the specificity of cell-mediated immunity is due to lymphocytes, which often function in concert with other cells, such as phagocytes, to eliminate microbes.
In the clinical setting, immunity to a previously encountered microbe is measured indirectly, either by assaying for the presence of products of immune responses (such as serum antibodies specific for microbial antigens) or by administering substances purified from the microbe and measuring reactions to these substances. A reaction to a microbial antigen is detectable only in individuals who have previously encountered the antigen; these individuals are said to be “sensitized” to the antigen, and the reaction is an indication of “sensitivity.” Although the reaction to the purified antigen has no protective function, it implies that the sensitized individual is capable of mounting a protective immune response to the microbe.
Cardinal Features of Adaptive Immune Responses
All humoral and cell-mediated immune responses to foreign antigens have a number of fundamental properties that reflect the properties of the lymphocytes that mediate these responses (Table 1-3).
TABLE 1–3 Cardinal Features of Adaptive Immune Responses
| Feature | Functional Significance |
|---|---|
| Specificity | Ensures that the immune response to a microbe (or nonmicrobial antigen) is targeted to that microbe (or antigen) |
| Diversity | Enables immune system to respond to a large variety of antigens |
| Memory | Increases ability to combat repeat infections by the same microbe |
| Clonal expansion | Increases number of antigen-specific lymphocytes to keep pace with microbes |
| Specialization | Generates responses that are optimal for defense against different types of microbes |
| Contraction and homeostasis | Allows immune system to recover from one response so that it can effectively respond to newly encountered antigens |
| Nonreactivity to self | Prevents injury to host during responses to foreign antigens |
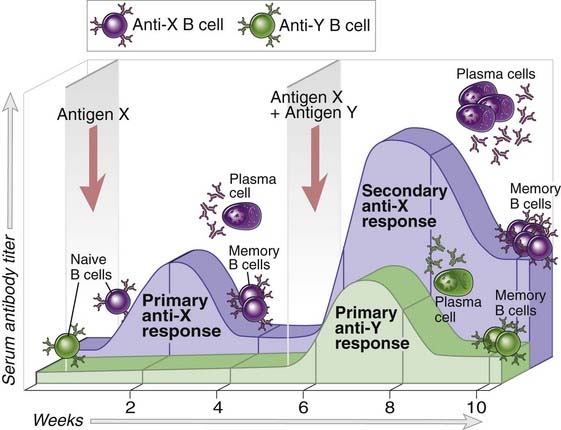
FIGURE 1–4 Specificity, memory, and contraction of adaptive immune responses.
Antigens X and Y induce the production of different antibodies (specificity). The secondary response to antigen X is more rapid and larger than the primary response (memory). Antibody levels decline with time after each immunization (contraction, the process that maintains homeostasis). The same features are seen in cell-mediated immune responses.
The total number of antigenic specificities of the lymphocytes in an individual, called the lymphocyte repertoire, is extremely large. It is estimated that the immune system of an individual can discriminate 107 to 109 distinct antigenic determinants. This ability of the lymphocyte repertoire to recognize a very large number of antigens is the result of variability in the structures of the antigen-binding sites of lymphocyte receptors for antigens, called diversity. In other words, there are many different clones of lymphocytes that differ in the structures of their antigen receptors and therefore in their specificity for antigens, contributing to a total repertoire that is extremely diverse. The variation of antigen receptors among different clones of T and B cells is the reason that these receptors are said to be “clonally distributed.” The molecular mechanisms that generate such diverse antigen receptors are discussed in Chapter 8.
These features of adaptive immunity are necessary if the immune system is to perform its normal function of host defense (see Table 1-3). Specificity and memory enable the immune system to mount heightened responses to persistent or recurring exposure to the same antigen and thus to combat infections that are prolonged or occur repeatedly. Diversity is essential if the immune system is to defend individuals against the many potential pathogens in the environment. Specialization enables the host to “custom design” responses to best combat different types of microbes. Contraction of the response allows the system to return to a state of rest after it eliminates each foreign antigen and to be prepared to respond to other antigens. Self-tolerance is vital for preventing harmful reactions against one’s own cells and tissues while maintaining a diverse repertoire of lymphocytes specific for foreign antigens.
Immune responses are regulated by a system of positive feedback loops that amplify the reaction and by control mechanisms that prevent inappropriate or pathologic reactions. When lymphocytes are activated, they trigger mechanisms that further increase the magnitude of the response. This positive feedback is important to enable the small number of lymphocytes that are specific for any microbe to generate the response needed to eradicate that infection. Many control mechanisms become active in immune responses to prevent excessive activation of lymphocytes, which may cause collateral damage to normal tissues, and to avoid responses against self antigens. In fact, a balance between activating and inhibitory signals is characteristic of all immune responses. We will mention specific examples of these fundamental features of the immune system throughout the book.
Cellular Components of the Adaptive Immune System
The principal cells of the immune system are lymphocytes, antigen-presenting cells, and effector cells. Lymphocytes are the cells that specifically recognize and respond to foreign antigens and are therefore the mediators of humoral and cellular immunity. There are distinct subpopulations of lymphocytes that differ in how they recognize antigens and in their functions (Fig. 1-5). B lymphocytes are the only cells capable of producing antibodies. They recognize extracellular (including cell surface) antigens and differentiate into antibody-secreting plasma cells, thus functioning as the mediators of humoral immunity. T lymphocytes, the cells of cell-mediated immunity, recognize the antigens of intracellular microbes and either help phagocytes to destroy these microbes or directly kill the infected cells. T cells do not produce antibody molecules. Their antigen receptors are membrane molecules distinct from but structurally related to antibodies (see Chapter 7). T lymphocytes have a restricted specificity for antigens; they recognize peptides derived from foreign proteins that are bound to host proteins called major histocompatibility complex (MHC) molecules, which are expressed on the surfaces of other cells. As a result, these T cells recognize and respond to cell surface–associated but not soluble antigens (see Chapter 6). T lymphocytes consist of functionally distinct populations, the best defined of which are helper T cells and cytotoxic (or cytolytic) T lymphocytes (CTLs). In response to antigenic stimulation, helper T cells secrete proteins called cytokines, which are responsible for many of the cellular responses of innate and adaptive immunity and thus function as the “messenger molecules” of the immune system. The cytokines secreted by helper T lymphocytes stimulate the proliferation and differentiation of the T cells themselves and activate other cells, including B cells, macrophages, and other leukocytes. CTLs kill cells that produce foreign antigens, such as cells infected by viruses and other intracellular microbes. Some T lymphocytes, which are called regulatory T cells, function mainly to inhibit immune responses. A third class of lymphocytes, natural killer (NK) cells, is involved in innate immunity against viruses and other intracellular microbes. A small population of T lymphocytes that express a cell surface protein found on NK cells are called NKT cells; their specificities and role in host defense are not well understood. We will return to a more detailed discussion of the properties of lymphocytes in Chapter 2 and in later chapters. Different classes of lymphocytes can be distinguished by the expression of surface proteins that are named CD molecules and numbered (see Chapter 2).
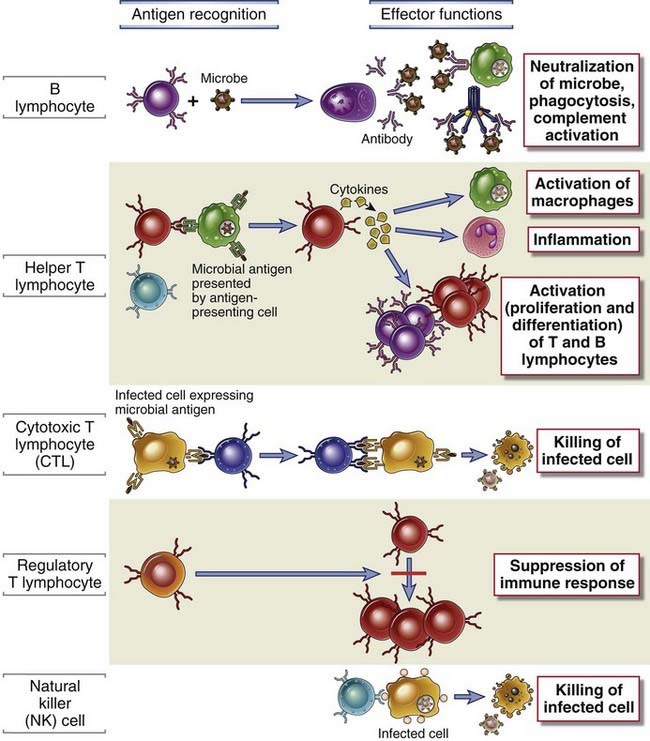
FIGURE 1–5 Classes of lymphocytes.
B lymphocytes recognize soluble antigens and develop into antibody-secreting cells. Helper T lymphocytes recognize antigens on the surfaces of antigen-presenting cells and secrete cytokines, which stimulate different mechanisms of immunity and inflammation. Cytotoxic T lymphocytes recognize antigens on infected cells and kill these cells. Regulatory T cells suppress and prevent immune response (e.g., to self antigens). NK cells use receptors with more limited diversity than T or B cell antigen receptors to recognize and kill their targets, such as infected cells.
The initiation and development of adaptive immune responses require that antigens be captured and displayed to specific lymphocytes. The cells that serve this role are called antigen-presenting cells (APCs). The most specialized APCs are dendritic cells, which capture microbial antigens that enter from the external environment, transport these antigens to lymphoid organs, and present the antigens to naive T lymphocytes to initiate immune responses. Other cell types function as APCs at different stages of cell-mediated and humoral immune responses. We will describe the functions of APCs in Chapter 6.
The activation of lymphocytes by antigen leads to the generation of numerous mechanisms that function to eliminate the antigen. Antigen elimination often requires the participation of cells that are called effector cells because they mediate the final effect of the immune response, which is to get rid of the microbes. Activated T lymphocytes, mononuclear phagocytes, and other leukocytes function as effector cells in different immune responses.
Lymphocytes and APCs are concentrated in anatomically discrete lymphoid organs, where they interact with one another to initiate immune responses. Lymphocytes are also present in the blood; from the blood, they can recirculate through lymphoid tissues and home to peripheral tissue sites of antigen exposure to eliminate the antigen (see Chapter 3).
The cells of innate immunity interact with one another and with other host cells during the initiation and effector stages of innate and adaptive immune responses. Many of these interactions are mediated by secreted proteins called cytokines. We will describe the properties and functions of individual cytokines when we discuss immune responses in which these proteins play important roles. We summarize some of the general features and functional categories of cytokines below.
Cytokines, Soluble Mediators of the Immune System
Cytokines, a large and heterogeneous group of secreted proteins produced by many different cell types, mediate and regulate all aspects of innate and adaptive immunity. The human genome contains about 180 genes that may encode proteins with the structural characteristics of cytokines. The nomenclature of cytokines is somewhat haphazard, with many cytokines arbitrarily named on the basis of one of the biologic activities they were discovered to have (e.g., tumor necrosis factor, interferons) and others called interleukins, with a number suffix, because cytokines were thought to be made by and to act on leukocytes.
Cytokines are not usually stored as preformed molecules, and their synthesis is initiated by new gene transcription as a result of cellular activation. Such transcriptional activation is transient, and the messenger RNAs encoding most cytokines are unstable and often rapidly degraded, so cytokine synthesis is also transient. The production of some cytokines may additionally be regulated by RNA processing and by post-translational mechanisms, such as proteolytic release of an active product from an inactive precursor. Once synthesized, cytokines are rapidly secreted, resulting in a burst of release when needed.
Cytokines share many other general properties. One cytokine can act on diverse cell types and have multiple biologic effects, a property that is referred to as pleiotropism. Conversely, multiple cytokines may have the same action, and are said to be redundant. One cytokine can stimulate or inhibit the production of others, and cytokines may antagonize one another or produce additive or synergistic effects.
Most cytokines act close to where they are produced, either on the same cell that secretes the cytokine (autocrine action) or on a nearby cell (paracrine action). T cells often secrete cytokines at the site of contact with APCs, the so-called immune synapse (see Chapter 9). This may be one reason that cytokines often act on cells that are in contact with the cytokine producers. When produced in large amounts, cytokines may enter the circulation and act at a distance from the site of production (endocrine action). Tumor necrosis factor (TNF) is an example of a cytokine that has important local and distant (systemic) effects.
Some cytokines are mediators and regulators of innate immunity. They are produced by innate immune cells such as dendritic cells, macrophages, and mast cells, and they drive the process of inflammation or contribute to defense against viral infections. Other cytokines, especially those produced by helper T cell subsets, contribute to host defense mediated by the adaptive immune system and also regulate immune responses. Members of this category of cytokines are also responsible for the activation and differentiation of T cells and B cells. Some cytokines are growth factors for hematopoiesis and regulate the generation of different types of immune cells from precursors in the bone marrow.
In general, the cytokines of innate and adaptive immunity are produced by different cell populations, act on different target cells, and have other distinct properties. However, these distinctions are not absolute because the same cytokine may be produced during innate and adaptive immune reactions, and different cytokines produced during such reactions may have overlapping actions.
Overview of Immune Responses to Microbes
Now that we have introduced the major components of the immune system and their properties, it is useful to summarize the principles of immune responses to different types of microbes. Such a summary will be a foundation for the topics that are discussed throughout the book. The immune system has to combat many and diverse microbes. As we shall see shortly, immune responses to all infectious pathogens share some common features, and responses to different classes of these microbes may also have unique features. How these adaptive immune reactions are initiated, orchestrated, and controlled are the fundamental questions of immunology. We start with a discussion of the innate immune response.
The Early Innate Immune Response to Microbes
The innate immune system blocks the entry of microbes and eliminates or limits the growth of many microbes that are able to colonize tissues. The main sites of interaction between individuals and their environment—the skin and gastrointestinal and respiratory tracts—are lined by continuous epithelia, which serve as barriers to prevent the entry of microbes from the external environment. If microbes successfully breach the epithelial barriers, they encounter the cells of innate immunity. The cellular innate immune response to microbes consists of two main types of reactions—inflammation and antiviral defense. Inflammation is the process of recruitment of leukocytes and plasma proteins from the blood, their accumulation in tissues, and their activation to destroy the microbes. Many of these reactions involve cytokines, which are produced by dendritic cells, macrophages, and other types of cells during innate immune reactions. The major leukocytes that are recruited in inflammation are the phagocytes, neutrophils (which have short life spans in tissues), and monocytes (which develop into tissue macrophages). These phagocytes express on their surfaces receptors that bind and ingest microbes and other receptors that recognize different microbial molecules and activate the cells. On engagement of these receptors, the phagocytes produce reactive oxygen and nitrogen species and lysosomal enzymes, which destroy the microbes that have been ingested. Resident macrophages in the tissues serve much the same functions. Antiviral defense consists of a cytokine-mediated reaction in which cells acquire resistance to viral infection and killing of virus-infected cells by NK cells.
Microbes that are able to withstand these defense reactions in the tissues may enter the blood, where they are recognized by the circulating proteins of innate immunity. Among the most important plasma proteins of innate immunity are the components of the alternative pathway of the complement system. When this pathway is activated by microbial surfaces, proteolytic cleavage products are generated that mediate inflammatory responses, coat the microbes for enhanced phagocytosis, and directly lyse microbes. (As we shall discuss later, complement can also be activated by antibodies—called the classical pathway, for historical reasons—with the same functional consequences.) Many of the circulating proteins enter sites of infection during inflammatory reactions and thus help combat microbes in extravascular tissues.
The reactions of innate immunity are effective at controlling and even eradicating infections. However, a hallmark of many pathogenic microbes is that they have evolved to resist innate immunity. Defense against these pathogens requires the more powerful and specialized mechanisms of adaptive immunity, which prevents them from invading and replicating in the cells and tissues of the host.
The Adaptive Immune Response
The adaptive immune system uses three main strategies to combat most microbes.
The goal of the adaptive response is to activate one or more of these defense mechanisms against diverse microbes that may be in different anatomic locations, such as intestinal lumens, the circulation, or inside cells.
All adaptive immune responses develop in steps, each of which corresponds to particular reactions of lymphocytes (Fig. 1-6). We start this overview of adaptive immunity with the first step, which is the recognition of antigens.
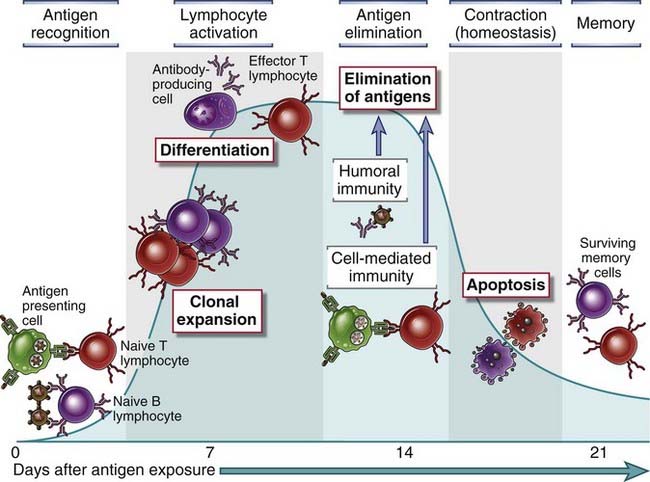
FIGURE 1–6 Phases of adaptive immune responses.
Adaptive immune responses consist of distinct phases, the first three being the recognition of antigen, the activation of lymphocytes, and the elimination of antigen (the effector phase). The response contracts (declines) as antigen-stimulated lymphocytes die by apoptosis, restoring homeostasis, and the antigen-specific cells that survive are responsible for memory. The duration of each phase may vary in different immune responses. The y-axis represents an arbitrary measure of the magnitude of the response. These principles apply to humoral immunity (mediated by B lymphocytes) and cell-mediated immunity (mediated by T lymphocytes).
The Capture and Display of Microbial Antigens
Because the number of naive lymphocytes specific for any antigen is very small (on the order of 1 in 105 or 106 lymphocytes) and the quantity of the available antigen may also be small, special mechanisms are needed to capture microbes, to concentrate their antigens in the correct location, and to deliver the antigens to specific lymphocytes. Dendritic cells are the APCs that display microbial peptides to naive CD4+ and CD8+ T lymphocytes and initiate adaptive immune responses to protein antigens. Dendritic cells located in epithelia and connective tissues capture microbes, digest their proteins into peptides, and express on their surface peptides bound to MHC molecules, the specialized peptide display molecules of the adaptive immune system. Dendritic cells carry their antigenic cargo to draining lymph nodes and take up residence in the same regions of the nodes through which naive T lymphocytes continuously recirculate. Thus, the chance of a lymphocyte with receptors for an antigen finding that antigen is greatly increased by concentrating the antigen in recognizable form in the correct anatomic location. Dendritic cells also display the peptides of microbes that enter other lymphoid tissues, such as the spleen.
Intact microbes or microbial antigens that enter lymph nodes and spleen are recognized in unprocessed (native) form by specific B lymphocytes. There are also specialized APCs that display antigens to B lymphocytes.
Antigen Recognition by Lymphocytes
Lymphocytes specific for a large number of antigens exist before exposure to the antigen, and when an antigen enters, it selects the specific cells and activates them (Fig. 1-7). This fundamental concept is called the clonal selection hypothesis. It was first suggested by Niels Jerne in 1955, and most clearly enunciated by Macfarlane Burnet in 1957, as a hypothesis to explain how the immune system could respond to a large number and variety of antigens. According to this hypothesis, antigen-specific clones of lymphocytes develop before and independent of exposure to antigen. A “clone” refers to a lymphocyte of one specificity and its progeny. A characteristic of the immune system is that a very large number of clones is generated during the maturation of lymphocytes, thus maximizing the potential for recognizing diverse microbes.
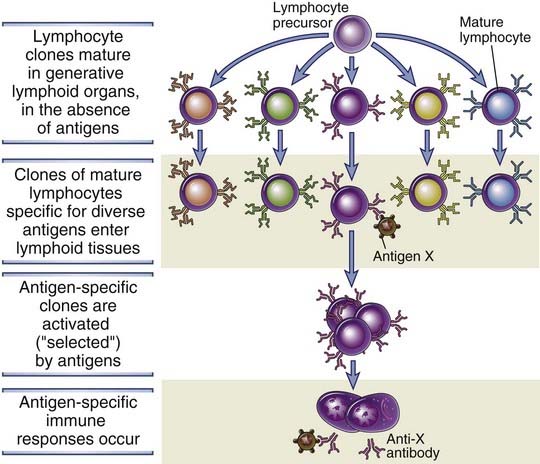
FIGURE 1–7 The clonal selection hypothesis.
Each antigen (X or Y) selects a preexisting clone of specific lymphocytes and stimulates the proliferation and differentiation of that clone. The diagram shows only B lymphocytes giving rise to antibody-secreting effector cells, but the same principle applies to T lymphocytes.
The activation of naive T lymphocytes requires recognition of peptide-MHC complexes presented on dendritic cells. The nature of the antigen that activates T cells (i.e., peptides bound to MHC molecules) ensures that these lymphocytes can interact only with other cells (because MHC molecules are cell surface proteins) and not with free antigen. This feature is necessary because all the functions of T lymphocytes are dependent on their physical interactions with other cells. To respond, the T cells need to recognize not only antigens but also other molecules, called costimulators, which are induced on the APCs by microbes. Antigen recognition provides specificity to the immune response, and the need for costimulation ensures that T cells respond to microbes (the inducers of costimulatory molecules) and not to harmless substances.
B lymphocytes use their antigen receptors (membrane-bound antibody molecules) to recognize antigens of many different chemical types.
Engagement of antigen receptors and other signals trigger lymphocyte proliferation and differentiation. The reactions and functions of T and B lymphocytes differ in important ways and are best considered separately.
Cell-Mediated Immunity: Activation of T Lymphocytes and Elimination of Intracellular Microbes
Activated CD4+ helper T lymphocytes proliferate and differentiate into effector cells whose functions are mediated largely by secreted cytokines. One of the earliest responses of CD4+ helper T cells is secretion of the cytokine interleukin-2 (IL-2). IL-2 is a growth factor that acts on the antigen-activated lymphocytes and stimulates their proliferation (clonal expansion). Some of the progeny differentiate into effector cells that can secrete different sets of cytokines and thus perform different functions. Many of these effector cells leave the lymphoid organs where they were generated and migrate to sites of infection and accompanying inflammation. When these differentiated effectors again encounter cell-associated microbes, they are activated to perform the functions that are responsible for elimination of the microbes. Some effector T cells of the CD4+ helper cell lineage secrete cytokines that recruit leukocytes and stimulate production of microbicidal substances in phagocytes. Thus, these helper T cells help the phagocytes kill the infectious pathogens. Other CD4+ effector T cells secrete cytokines that stimulate the production of a special class of antibody called immunoglobulin E (IgE) and activate leukocytes called eosinophils, which are able to kill parasites that may be too large to be phagocytosed. As we discuss next, some CD4+ helper T cells stay in the lymphoid organs and stimulate B cell responses.
Activated CD8+ lymphocytes proliferate and differentiate into CTLs that kill cells harboring microbes in the cytoplasm. These microbes may be viruses that infect many cell types or bacteria that are ingested by macrophages but escape from phagocytic vesicles into the cytoplasm (where they are inaccessible to the killing machinery of phagocytes, which is largely confined to vesicles). By destroying the infected cells, CTLs eliminate the reservoirs of infection.
Humoral Immunity: Activation of B Lymphocytes and Elimination of Extracellular Microbes
On activation, B lymphocytes proliferate and differentiate into cells that secrete different classes of antibodies with distinct functions. The response of B cells to protein antigens requires activating signals (“help”) from CD4+ T cells (which is the historical reason for calling these T cells “helper” cells). B cells can respond to many nonprotein antigens without the participation of other cells.
Some of the progeny of the expanded B cell clones differentiate into antibody-secreting plasma cells. Each plasma cell secretes antibodies that have the same antigen-binding site as the cell surface antibodies (B cell receptors) that first recognized the antigen. Polysaccharides and lipids stimulate secretion mainly of the antibody class called IgM. Protein antigens induce the production of antibodies of functionally different classes (IgG, IgA, IgE) from a single clone of B cells. The production of these different antibodies, all with the same specificity, is called class switching and requires the action of helper T cells; it provides plasticity in the antibody response, enabling it to serve many functions. Helper T cells also stimulate the production of antibodies with increased affinity for the antigen. This process, called affinity maturation, improves the quality of the humoral immune response.
The humoral immune response combats microbes in many ways. Antibodies bind to microbes and prevent them from infecting cells, thus “neutralizing” the microbes and blocking their ability to infect host cells or to colonize tissues. In fact, antibodies are the only mechanisms of adaptive immunity that prevent an infection from becoming established; this is why eliciting the production of potent antibodies is a key goal of vaccination. IgG antibodies coat microbes and target them for phagocytosis because phagocytes (neutrophils and macrophages) express receptors for the tails of IgG. IgG and IgM activate the complement system, by the classical pathway, and complement products promote phagocytosis and destruction of microbes. Some antibodies serve special roles at particular anatomic sites. IgA is secreted from mucosal epithelia and neutralizes microbes in the lumens of the respiratory and gastrointestinal tracts (and other mucosal tissues). Maternal IgG is actively transported across the placenta and protects the newborn until the baby’s immune system becomes mature. Most antibodies have half-lives of a few days, but some IgG antibodies have half-lives of about 3 weeks. Some antibody-secreting plasma cells migrate to the bone marrow and live for years, continuing to produce low levels of antibodies. The antibodies that are secreted by these long-lived plasma cells provide immediate protection if the microbe returns to infect the individual. More effective protection is provided by memory cells that are activated by the microbe and rapidly differentiate to generate large numbers of plasma cells.
Immunologic Memory
An effective immune response eliminates the microbes that initiated the response. This is followed by a contraction phase, in which the expanded lymphocyte clones die and homeostasis is restored.
The initial activation of lymphocytes generates long-lived memory cells, which may survive for years after the infection. Memory cells are more effective in combating microbes than are naive lymphocytes because, as mentioned earlier, memory cells represent an expanded pool of antigen-specific lymphocytes (more numerous than naive cells specific for the antigen), and memory cells respond faster and more effectively against the antigen than do naive cells. This is why generating memory responses is another important goal of vaccination. We will discuss the properties of memory lymphocytes in later chapters.
In the remainder of the book, we describe in detail the recognition, activation, regulation, and effector phases of innate and adaptive immune responses. The principles introduced in this chapter recur throughout the book.
Summary
Burnet FM. A modification of Jerne’s theory of antibody production using the concept of clonal selection. Australian Journal of Science. 1957;20:67-69.
Flajnik MF, du Pasquier L. Evolution of innate and adaptive immunity: can we draw a line? Trends in Immunology. 2004;25:640-644.
Jerne NK. The natural-selection theory of antibody formation. Proceedings of the National Academy of Sciences U S A. 1955;41:849-857.
Litman GW, Rast JP, Fugmann SD. The origins of vertebrate adaptive immunity. Nature Reviews Immunology. 2010;10:543-553.
Silverstein AM. Paul Ehrlich’s Receptor Immunology: The Magnificent Obsession. New York: Academic Press; 2001.
Silverstein AM. Cellular versus humoral immunology: a century-long dispute. Nature Immunology. 2003;4:425-428.