67 Strategy of antimicrobial chemotherapy
Key points
• A central aim in choosing antimicrobial therapy is to match the most appropriate agent to the specific microbial aetiology. In practice, this is constrained by urgency of the situation, the diagnostic information available and policy decisions about antimicrobial use that are made on a local basis consistent with national policies.
• The initial decision on whether or not to give an antimicrobial and on the agent chosen is generally made before microbiological information is available but, where possible, after microbiological samples have been taken.
• In the UK, local and specific guidance is generally available for chemotherapy of common infective syndromes. The strategy reflects the likely causal agents and their local susceptibility patterns, the need to control antimicrobial resistance, and cost. This guidance is reflected in the local antibiotic policy.
• The laboratory will assist in modifying or initiating therapy by determining in vitro susceptibilities and by monitoring antimicrobial drug concentrations in specific circumstances. These analyses may lead to modification of therapy.
• Certain organisms such as streptococci and anaerobes have predictable susceptibilities, whereas others, such as enterobacteria, must be monitored continuously.
• Prophylactic antimicrobials are recommended in highly defined settings and when following precise regimens. Ad hoc usage is to be avoided.
• Antimicrobial combinations may be given to increase efficacy, extend the spectrum of cover or prevent the development of resistance during therapy.
In the previous chapter the work of the laboratory in assisting doctors in making a definitive microbiological diagnosis was described and summarized in Figure 66.1. Ideally, management of an infection should involve these stages plus choice of an appropriate antimicrobial agent (if necessary) and follow-up tests of cure. Chapter 5 listed the different classes of antimicrobial agents from which the doctor may prescribe. The objectives of an antibiotic strategy are to implement clinical guidelines that cover the treatment of an individual patient and policies based on these will have a maximum public health effect. These include cost-effectiveness and limiting the spread of antibiotic resistance.
Choice of treatment
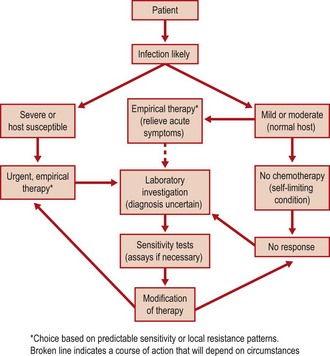
Infections are so common in general practice that it is not practical for each patient to be fully investigated and a rational choice of antimicrobial agent made on the results. Because many have a viral aetiology and most respond rapidly to simple symptomatic relief, the choice is not which agent to use but whether to prescribe at all. Many patients who make the effort to see a doctor expect drug treatment. Although the time taken to educate the public and convince the individual is often longer than that needed to write a prescription, it is important that prescribers do not yield to pressure if antibiotics are not indicated. Figure 67.1 shows a flow diagram of choice of antibiotics that is applicable to many common conditions. There are three main points in the diagram:
1. Patients may be categorized on clinical grounds into those with mild, moderate or severe infection and also into those who were previously healthy or have underlying disease that may affect their response to therapy; for example, impaired immunity or the presence of a foreign body. In the latter situation it is more important to send specimens to the laboratory and start empirical therapy to cover likely pathogens.
2. The organisms causing many common clinical syndromes have predictable antibiotic sensitivities, allowing a rational choice to be made.
3. The results of laboratory tests may lead to modification or withdrawal of chemotherapy.
Although ‘best guess’ or empirical therapy is commenced before the results of laboratory tests are available, it is wrong to argue that this approach is incorrect since early administration of an antimicrobial is sometimes life-saving.
Laboratory monitoring
Susceptibility tests
As well as providing routine tests of sensitivity on individual isolates, the laboratory should provide a general picture of the prevalence of different pathogens occurring in the local population and their pattern of resistance. Different lists should be prepared and regularly circulated to general practitioners, hospital consultants and specialized units. The methods used and limitations of susceptibility testing are outlined in Chapter 5. Sometimes individual patients will need to be monitored for the efficacy of treatment and to determine if failure has occurred due to acquired resistance or replacement with a more resistant organism. This is especially important in the assessment of new agents in clinical trials.
Antibiotic assay
Rapid methods are now available to determine the amount of antibiotic in serum and other body fluids during treatment. These assays can be used to monitor the adequacy of dosage or to avoid possible toxic effects of overdosage.
In practice, it is necessary to carry out such assays only in a small minority of patients who are seriously ill with infections such as endocarditis or those receiving potentially toxic agents such as aminoglycosides and vancomycin. Urine samples may be screened for antibacterial activity. This can be of value in determining patient compliance during therapy for tuberculosis.
The interpretation of the results of antibiotic assays may be difficult if the patient is receiving multiple antibiotics. In such cases, the power of the body fluid to inhibit or kill the infecting organism in vitro may be a more useful measurement of adequate dosage; for example, in bacterial endocarditis, the patient’s serum should kill the causative organism at a dilution of 1 in 4 or more.
It is important to know the relationship of the sample being assayed to the time of dosage: maximum or peak levels are usually measured in serum 0.5–1 h following a dose; minimum or trough levels are from a sample taken shortly before the next dose.
Assays should always be carried out in close collaboration with the microbiologist to ensure the correct timing of samples and to avoid errors of interpretation.
Clinical correlation of laboratory tests
The epithet sensitive or resistant is a clinical description; in laboratory tests it is usual to select a concentration of the agent which is known to be easily attained in serum, other body fluids or tissue after normal recommended dosage. Organisms susceptible to this, or lower concentrations, are regarded as sensitive; those able to grow are resistant. These terms relate to the minimum inhibitory concentration (MIC) of the microbe (see p. 66). The correlation between this interpretation and clinical results is generally good, but not perfect. Discrepancies may be due to a failure to attain adequate concentrations at the site of infection, resulting in clinical failure. However, there are many factors on which the outcome of the host–parasite relationship in infection depends, and it would be surprising if a complete correlation between in-vitro tests and the results of chemotherapy was observed.
Predictable sensitivity
Once the identity of an infecting organism is known, the sensitivity pattern is often predictable with a fair degree of accuracy. Not surprisingly, however, the susceptibility of common pathogens may change with time. Thus, predictable sensitivity of micro-organisms, while useful, is a changing concept and will have local variations, so that the advice of local microbiologists should be sought.
Organisms with predictable sensitivity patterns
Streptococcus pyogenes is a good example of an organism that has retained a sensitivity pattern that has changed little in 70 years. Thus, penicillin is always the drug of choice for the treatment of haemolytic streptococcal infections. Other β-lactam antibiotics are also active against Str. pyogenes. Erythromycin is an alternative if the patient cannot be given penicillin because of allergy, but an increasing number of strains in some areas show some resistance to this antibiotic in vitro.
Until recently, most strains of Str. pneumoniae were highly sensitive to penicillin. An increasing number of penicillin-resistant pneumococci are now found in cases of invasive disease in some institutions, and are posing a major problem worldwide. Fortunately, this is much rarer with strains of N.meningitidis which appear to be penicillin-sensitive in most places.
Reproducible patterns of sensitivity to antimicrobial drugs can be shown for many other groups of bacteria and offer a useful guide to the choice of chemotherapy (Table 67.1). However, exceptions to these patterns occur and resistant variants may become prevalent in some localities, particularly under the pressure of intensive antibiotic usage.
Table 67.1 Examples of organisms and antimicrobial agents for which susceptibility is usually predictable
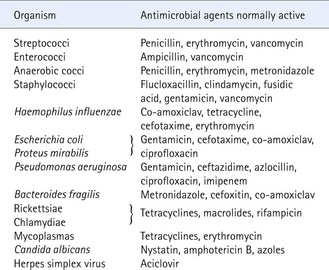
In the same way that organisms may exhibit predictable sensitivity to some agents, they may be predictably resistant. Some examples are shown in Table 67.2.
Table 67.2 Examples of organisms and antimicrobial agents for which resistance is usually predictable
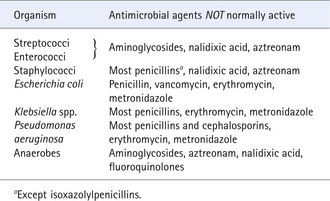
Organisms of variable sensitivity
Many groups of pathogenic bacteria, notably staphylococci and enterobacteria, vary unpredictably in their sensitivity to antimicrobial drugs. With these organisms there is a greater need to carry out sensitivity tests on individual isolates.
Staphylococci
Staphylococci, including coagulase-negative strains, show great variability in susceptibility, and this can severely limit choice of antibiotics. Four main kinds of staphylococci may be encountered:
1. Penicillin-sensitive strains. Before the widespread use of penicillin in the 1940s, most Staphylococcus aureus isolates were sensitive. Usually these strains are susceptible to other antistaphylococcal agents (macrolides, aminoglycosides and fusidic acid). Penicillin-sensitive strains now account for about 10% of isolates.
2. β-Lactamase-producing strains. Staphylococcal penicillinase confers resistance to all penicillins except methicillin, the isoxazolyl group (cloxacillin, etc.) and nafcillin. These strains usually retain susceptibility to cephalosporins. Most Staph. aureus and Staph. epidermidis strains found in clinical practice belong to this group.
3. Methicillin-resistant strains (MRSA). Methicillin, the first penicillinase-stable penicillin, is used as the test compound to identify these strains in the laboratory. Strains of Staph. aureus resistant to methicillin are also resistant to virtually all β-lactam agents. MRSA have epidemiological significance as a group and have been isolated from hospital outbreaks in different countries. Many of these epidemic strains are multiresistant, exhibiting resistance to aminoglycosides, macrolides and other antistaphylococcal agents, including the topical compound, mupirocin, which has been used to eradicate the organism from carriers of MRSA. Vancomycin, teicoplanin or linezolid may be the only agents available for treatment.
4. Other antibiotic-resistant strains. Multiple resistance to antistaphylococcal antibiotics may be seen in strains that are methicillin-sensitive. They are found in similar situations to MRSA, namely hospital units with severely debilitated patients and problems with cross-infection. Such resistance patterns are more common in coagulase-negative staphylococci.
Enterobacteria
Escherichia coli includes many strains of variable sensitivity, but among the general population in the UK half of the strains isolated from urinary tract infections are sensitive to ampicillin and amoxicillin, and an even higher proportion are sensitive to cephalosporins, co-amoxiclav (the combination of amoxicillin and clavulanic acid) and trimethoprim.
Variable sensitivity is also a feature of other enterobacteria. There has been an increase in E. coli resistant to expanded spectrum β-lactams (ESBLs) in many countries. Where these organisms are also quinolone and trimethoprim resistant, treatment with oral agents is limited. Multiresistant typhoid is a particular problem in many countries where the disease is endemic. If there is doubt about the clinical response, or the sensitivity of the strain, laboratory tests should be carried out.
Other organisms
Several pathogens which were formerly reliably sensitive to standard agents, including neisseriae, Haemophilus influenzae, pneumococci, enterococci, mycobacteria and Plasmodium falciparum, are now commonly resistant to first-line therapy. In some cases, options for treatment of infection with these organisms have become severely constrained.
Antibiotic policies and the control of resistance
The benefits of the use of antibiotics, not only in medicine but also in animal husbandry, must be taken into account in considering the merits of restrictive policies undertaken to control antibiotic resistance.
There is, without doubt, a problem of resistance among many commonly occurring micro-organisms. However, most of the problems of resistance occur among patients within closed communities such as hospitals. This is most marked in areas of intensive care, where large amounts of antibiotics are used in highly susceptible patients with low immunity to infection. In the general community, multiple resistances to antibiotics is presently not a major problem in the UK, but the spread of MRSA out of hospitals into nursing and residential homes may herald a change in this situation.
Accordingly, attention should be directed to those hospital units in which the problem of resistance is significant and which may be the most important source of spread to the general community. As resistance in bacteria has many of the features of an epidemic disease, the application of classic rules and precautions for the prevention of infection may halt this spread.
Restrictive policies
The use of antibiotics by general practitioners and clinicians is influenced by the prescribing habits of other medical colleagues and by the promotional efforts of the pharmaceutical companies. Thus, an ordered and systematic use of antimicrobial drugs might be of benefit in the general strategy of chemotherapy. Since the use of antibiotics acts as a powerful selective factor in the emergence and spread of resistant micro-organisms, restriction of use should have the opposite effect. The acceptance of this thesis has encouraged restrictive policies involving temporary bans on the use of certain antibiotics. Such policies may also lead to a reduced chance of prescription error and some cost benefits.
Rotational policies
Periodic changes of antibiotics used in treatment might also help to avoid the emergence of resistant strains by altering the selective pressures and discouraging opportunistic pathogens such as Pseudomonas and Acinetobacter species. Such a rotational policy might help to retain the therapeutic value of antibiotics over a longer period. The availability of a large range of clinically useful antibacterial substances (Table 67.3) makes this kind of policy more practicable.
Table 67.3 Main groups of antibiotics available for clinical use
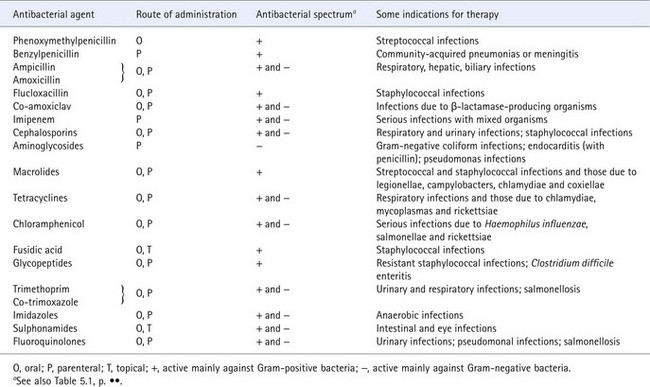
Prophylactic use of antibiotics
The unnecessary prophylactic use of antibiotics should be discouraged as this may result in increased selection of resistant variants or superinfection with resistant flora. However, there are several circumstances in which chemoprophylaxis is clearly beneficial.
A widely accepted use of antimicrobial agents for the prevention of infection is in patients who have suffered from rheumatic fever, or are thought otherwise to be at risk of rheumatic carditis to prevent further streptococcal infection. Among other indications for chemoprophylaxis are the use of peri-operative antibiotics in patients undergoing joint replacement to reduce the chance of potentially disastrous infection. Similarly, patients undergoing lower bowel resection receive peri-operative treatment with combinations of agents intended to suppress the lower bowel flora. The clinical and laboratory evidence for the benefit of these kinds of prophylaxis is now well established.
Chemoprophylaxis is also justified in preventing pneumococcal infection in splenectomized patients and pneumocystis pneumonia in people with human immunodeficiency virus (HIV). In healthy individuals who are close contacts of infectious diseases such as meningococcal meningitis, short courses of antibiotics are justified to prevent acquisition of the organism or to eradicate carrier status. Travellers to regions in which malaria is endemic should take antimalarial prophylaxis.
Host factors influencing response
In most individuals with normal immune systems an antimicrobial drug assists in a more rapid recovery from infection, but the choice of agent is often not critical providing it has some effect on the causative organisms. In very serious infections or when the patient is at a disadvantage because of impaired or absent immunity, the role of the antibiotic becomes more important and more care should be taken in its selection, dosage and administration.
Problems of toxicity
The final choice of the most appropriate antimicrobial drug may be influenced by the history and response of the patient. Known hypersensitivity to a drug such as penicillin means that neither this antibiotic nor other penicillins can be safely given and alternatives must be used. Side-effects such as nausea, vomiting, diarrhoea or pruritis may be severe enough to warrant a change in treatment. Some antibiotics have potentially serious side-effects, such as the ototoxicity of the aminoglycosides, and care must be taken to avoid these by laboratory monitoring of drug levels, as such toxicity is usually dose-related. Intercurrent disease may require modification of the dosage of certain antibiotics because of specific organ deficiency, e.g. liver failure or impaired renal function. Ototoxicity of the aminoglycosides must always be borne in mind in patients who have poor renal function.
Failure to reach the site of infection
The absorption of oral antibiotics varies widely from patient to patient and, if poor, may be a cause of treatment failure. Alternatively, infection may be localized within a large collection of pus or at an anatomical site that is penetrated by antibiotics with difficulty. Obstruction to the flow of body fluids may likewise militate against success; this is important in infections of the urinary tract, biliary system and central nervous system. In some of these cases more radical interference may be indicated to relieve the obstruction.
Alteration of normal flora
Antibiotic therapy may upset the patient’s microflora and result not only in the selection of resistant strains of commensals, such as staphylococci on the skin, or E. coli in the intestinal tract, but also colonization with species not normally present. This can lead to antibiotic-induced infection, such as candidosis. Diarrhoea is frequently associated with antibiotic therapy, and reflects disturbance of the normal bowel flora. In a few patients the clinical condition can be severe and proceed to pseudomembranous colitis associated with the toxins of Clostridium difficile (see p. 254).
Intravenous administration
When antibiotics are given intravenously, they should normally be administered directly into the vein and not added to other infusion fluids; otherwise adequate blood levels of the drug may not be attained owing to excretion outpacing administration. There is also the possibility of incompatibility between the antibiotic and the contents of the fluid. In all cases, the manufacturer’s instructions and recommendations about the administration of the drug should be closely followed.
Combinations of antibiotics
The clinical benefits of the use of combinations of antibacterial agents tend to be exaggerated. The combination of two or more agents has been long accepted in the treatment of tuberculosis, so limiting the selection of mutants resistant to the individual components. The use of β-lactam antibiotics with an aminoglycoside in the treatment of streptococcal endocarditis is also accepted, as the mixture is more bactericidal than the individual components.
A combination of a β-lactam antibiotic with a β-lactamase inhibitor may prevent destruction of the antibiotic. Thus, the enzyme inhibitor clavulanic acid in combination with amoxicillin (co-amoxiclav) restores the activity of the antibiotic against many β-lactamase-producing bacteria.
Potentiation of the antibacterial effect by combinations is referred to as synergy; some combinations exhibit a lesser effect than the individual components, and this is called antagonism. These interactions are generally displayed in vitro, and it is difficult to establish evidence of advantages or disadvantages in the patient. Thus, the combination of trimethoprim and sulphamethoxazole (co-trimoxazole) can be shown to be synergistic in the test tube, but it has been difficult to demonstrate any clinical benefit, and trimethoprim is now often used on its own to avoid the chance of toxic reactions to sulphonamides.
Antiviral therapy
An increasing number of agents are being used in the prophylaxis or treatment of viral infections (see Ch. 5).
Aciclovir is the most widely used agent at present, and is prescribed for the treatment of herpes simplex and herpes zoster. This drug can be given orally, but in severely ill patients it is administered intravenously; for example, in treating herpes encephalitis. Aciclovir is also used in the prophylaxis and treatment of varicella, particularly in immunocompromised patients. The related compound ganciclovir is available for the treatment of cytomegalovirus infection, but is associated with considerable toxicity.
Amantadine is active against influenza A virus, but not against influenza B virus. This drug, and the related rimantadine, have been chiefly used for the prophylaxis of influenza. Zanamivir and oseltamivir are active against both A and B viruses and have been used to modify infection and prevent spread of influenza.
Ribavirin (tribavirin) is useful in the treatment of respiratory syncytial virus infections in children, hepatitis B and C (in combination with interferon) and some haemorrhagic fever viruses, such as Lassa fever.
Zidovudine (azidothymidine) is an inhibitor of HIV and was the first drug used in the management of patients with acquired immune deficiency syndrome (AIDS). There are now a number of other antiretroviral agents used in combination (see Ch. 55).
Antifungal therapy
Superficial fungal infections are very common. Systematic fungal disease is relatively rare in the UK, except in patients who are immunosuppressed or otherwise compromised. There are few effective antifungal agents that can be used systemically (see Table 5.4, p. 61 and Ch. 61) and some have considerable toxicity.
For many years the chemotherapy of superficial fungal infections depended on preparations of benzoic, salicylic or undecanoic acid. More effective is griseofulvin, given orally, sometimes over long periods, for the treatment of dermatophytoses; the new allylamine, terbinafine, seems to be at least as effective in these conditions. Nystatin and other polyenes are used for the topical treatment of superficial candidosis (thrush). Imidazoles such as clotrimazole are also used in the treatment of vaginal yeast infections.
Amphotericin B is used parenterally for the treatment of systemic candidosis, cryptococccal infections and aspergillosis. Flucytosine is also active against yeasts and has been used in combination with amphotericin B. Amphotericin B is toxic and treatment has to be carefully monitored to obtain the most satisfactory clinical results. Liposomal formulations of the drug appear to be safer and more effective.
The increasing range of antifungal agents used to treat human infections are described in Chapter 61. These are being used more widely in the treatment of systemic fungal disease because of their relative lack of toxicity, although the development of resistance may be a problem. This includes ketoconazole, and triazoles such as itraconazole, fluconazole, voriconazole and posiconazole and the echinocardins (caspofungin and micafungin).
Chemotherapy of systemic infections
Serious generalized infection
Patients with serious and often overwhelming generalized infection include those with bacterial shock syndrome and others with the symptomatology of acute infection without localizing signs. These syndromes may be related to postoperative infection, to instrumentation, or to the aggravation of a previously mild infection (e.g. extension of a middle ear infection to the brain). Generalized infection may also follow a reduction in the natural resistance of the patient. Such a situation may arise in renal failure, immune deficiency states, blood dyscrasias and neoplastic disease. Specific measures used in the treatment of these diseases may further reduce resistance to infection and the clinical features characteristic of infection may be muted or absent.
Appropriate specimens should be submitted to the laboratory before treatment is begun, in an effort to isolate the causative organisms. However, these patients may require immediate treatment and often there will be little indication of the nature of the infecting organism; more than one species may be involved, especially when the source of the infection is within the abdomen. Empirical chemotherapy must therefore cover Gram-positive cocci, Gram-negative bacilli and anaerobes such as bacteroides. A combination of amoxicillin, an aminoglycoside and metronidazole is suitable. Co-amoxiclav improves the spectrum of amoxicillin and allows omission of the metronidazole. Alternatively, an expanded-spectrum cephalosporin such as cefotaxime can be used. Therapy may be subsequently changed according to the results of laboratory tests. If the patient fails to respond after treatment for 3 days, the use of alternative agents should be considered.
In some patients in intensive care and in the immunocompromised, the possibility of systematic fungal infection or activation of dormant viruses, such as cytomegalovirus, must be considered.
It must always be remembered that bacterial toxins are unaffected by antibacterial therapy. Supportive treatment will include correction of fluid and electrolyte imbalance and appropriate treatment of any co-existing organ failure. In future, immunotherapy such as the use of anti-endotoxins and drugs that alter the cytokine and clotting cascades may find a place in treatment.
Infective endocarditis
Whenever possible, treatment of endocarditis should be related to the results of sensitivity tests made on the organism isolated from the blood. Formerly, viridans streptococci were the most common isolates and penicillin was the drug of choice. Viridans streptococci are now isolated from only about one-third of patients and the organisms from the remainder are usually relatively resistant to penicillin. Bactericidal therapy with penicillin in combination with an aminoglycoside is usually indicated. It is sometimes helpful to carry out bactericidal tests against the causative organism and it may also be useful to monitor the progress of the patient by assays of the bactericidal activity of the serum against the causative organism.
After operations for the replacement of heart valves it may be difficult to isolate an organism and there may be doubt as to whether or not infection has become superimposed. The risk of withholding treatment, however, is so great that empirical treatment may be indicated, and as staphylococcal infection may occur in such circumstances, it is best to include an antistaphylococcal antibiotic. Injecting drug users are also prone to staphylococcal endocarditis.
For the prevention of bacterial endocarditis in patients at risk following dental extraction, 3 g of amoxicillin, given orally 1 h before surgery, is recommended.
Rare causes of infective endocarditis in which blood cultures are negative include infections with Coxiella burnetti or certain chlamydiae. The diagnosis of these conditions depends largely upon serological evidence as it is difficult to isolate the organisms. An aetiological diagnosis is important, as treatment with an appropriate antibiotic, usually tetracycline, may be life-saving.
Urinary tract infections
Uncomplicated cystitis
Uncomplicated urinary infections and asymptomatic bacteriuria are common in adolescent and adult women seen in general practice and maternity clinics. Most infections are due to E. coli, and most are sensitive to a wide range of drugs. In most cases eradication of the organism is achieved after a short course of therapy with an oral agent such as trimethoprim. The remainder will often respond to a second course of treatment, but if the bacteriuria still persists, fuller urological investigation is required as failure of treatment is more usually related to an abnormality of the urinary system than to resistance of the organism.
Infections following catheterization
Infection of the urinary tract sometimes occurs after instrumentation such as catheterization or cystoscopy; it is almost unavoidable if indwelling catheters are used. Often the strains causing these infections are derived from the hospital environment, and include resistant strains of Gram-negative bacilli, sometimes in mixed culture. Frequently, the patient is not greatly inconvenienced by such infection, and chemotherapy is not indicated in most areas. If therapy is required, elimination of the organisms can be difficult, particularly if there is residual pathology or a degree of urinary obstruction. Sensitivity tests must be carried out to assist in the choice of therapy. The most useful agents are cephalosporins, trimethoprim and ciprofloxacin; for more serious or refractory cases, in which there is the hazard of systemic spread of the infection, parenteral treatment with an aminoglycoside or an expanded-spectrum cephalosporin must be considered.
Recurrent infection
In chronic pyelonephritis and recurrent bacteriuria it may be important to control infection by continuous treatment with antibiotics such as trimethoprim. Unfortunately, some patients may become re-infected with resistant species so that alternative drugs must be used. Thus, long-term therapy may require periodic bacteriological reassessment and sensitivity tests on the flora isolated to indicate when changes in therapy are required.
Respiratory infections
Respiratory tract infections are extremely common, and, although many are primary virus infections, those that are more severe and prolonged usually indicate secondary bacterial invasion. Laboratory diagnosis of these conditions is important since effective treatment depends on use of an antibiotic specifically active against the causative organisms.
Upper respiratory tract infections
A number of bacteria may be associated with sore throat, pharyngitis and sinusitis, including Str. pyogenes, Str. pneumoniae, H. influenzae and Vincent’s organisms. The most important infections from the point of view of the development of sequelae are those due to Str. pyogenes, for which the treatment of choice is penicillin given for at least 7 days to ensure eradication of the organism. All the other important bacterial pathogens will also respond to this treatment, with the exception of H. influenzae, for which treatment with amoxicillin, tetracycline, co-trimoxazole or erythromycin is appropriate.
If for some reason penicillin cannot be prescribed, the antibiotic of choice is erythromycin or co-trimoxazole. Ampicillin and amoxicillin should be avoided if there is any likelihood of glandular fever because these antibiotics tend to cause a rash and prolong the disease. Tetracyclines should be avoided in young children because of the risk of discoloration of developing teeth.
Lower respiratory tract infections
Lobar pneumonia is most frequently caused by pneumococci and penicillin is the drug of choice; erthyromycin or cefotaxime are good alternatives as are some of the newer fluoroquinolones such as levofloxacin. Infections due to klebsiellae or other organisms will require treatment with antibiotics according to the results of sensitivity tests; cefotaxime or cefuroxime are usually effective if laboratory confirmation is not available. Other coliform bacilli are rarely involved in pulmonary infections although they often colonize the upper respiratory tract; they seldom require specific treatment.
Among atypical pneumonias, mycoplasma infections respond best to a tetracycline or erythromycin; legionella infections respond to macrolides, alone or combined with rifampicin.
Bronchopneumonia is most frequently associated with pneumococci or haemophilus, so that amoxicillin, tetracycline or trimethoprim should be effective. More rarely, bronchopneumonia is caused by Staph. aureus, and flucloxacillin, fusidic acid or clindamycin is urgently required for treatment.
Acute exacerbations of chronic bronchitis are almost invariably associated with either Str. pneumoniae or H. influenzae. Amoxicillin, tetracycline or trimethoprim is usually effective.
In bronchiectasis, lung abscess or cystic fibrosis, antimicrobial treatment should be prescribed according to laboratory culture and sensitivity test results. Combinations of antibiotics may be effective in some of these patients. In pulmonary tuberculosis, combination treatment, usually with rifampicin, isoniazid and pyrazinamide, is mandatory.
Meningitis
A Gram film and cell count of cerebrospinal fluid (CSF) will usually differentiate viral from bacterial meningitis. If bacteria cannot be seen, initial treatment is with cefotaxime or ceftriaxone. This choice ensures adequate treatment of infections with Gram-negative bacilli (most common in neonates) and of infections with Neisseria meningitidis, H. influenzae and Str. pneumoniae, which are the most common causes of meningitis in young children. Care must be taken to differentiate Listeria monocytogenes infection, as this organism is less sensitive to penicillin and cefotaxime; a combination of amoxicillin and gentamicin is usually used.
When the causative organism is isolated, therapy may be altered to penicillin for meningococcal or pneumococcal infections. Pseudomonas aeruginosa meningitis may occasionally occur as a nosocomial infection and should be treated with full doses of gentamicin plus a β-lactam agent such as azlocillin. It is rarely necessary to give intrathecal antibiotics.
Where there is increased CSF pressure, as in spina bifida, shunts are inserted to facilitate the circulation of fluid. These often become contaminated, usually with staphylococci, probably derived from the skin. Antistaphylococcal antibiotics are used to control the growth of the infecting organism in anticipation of replacement of the prosthesis.
Intestinal infections
Mild bacillary dysentery, salmonella food poisoning and other forms of bacterial diarrhoea do not ordinarily require chemotherapy. Indeed, such therapy may make intestinal carriage more likely and increase the risk of the selection of antibiotic-resistant strains. The most important treatment is correction of fluid balance.
Patients with invasive infection (e.g. typhoid and paratyphoid fever) and those with severe bacillary dysentery or cholera may warrant treatment (see appropriate chapters). Even potentially fatal intestinal infections with E. coli O157 fare worse with antimicrobials than fluids alone. This may be due to excess toxin release.
Many intestinal infections are due to viruses, for which there is presently no specific chemotherapy. Cryptosporidiosis is now being diagnosed more frequently, but is usually self-limiting except in the immunocompromised. Infection with other protozoa, such as Giardia lamblia or Entamoeba histolytica, requires treatment with metronidazole.
Spread of infection from the bowel may give rise to serious infections and associated toxaemia. If subphrenic, retrocolic or pelvic abscesses form, drainage is the most important aspect of treatment, but antibiotics can assist recovery of the patient. Cephalosporins or an aminoglyoside plus ampicillin are useful in empirical treatment, and metronidazole should be added if bacteroides is likely to be present. Acute peritonitis after non-specific inflammation of the bowel, such as appendicitis, is usually effectively treated with amoxicillin (with or without clavulanate) or cefotaxime combined with metronidazole.
Liver infections
Bacterial infections of the liver and portal pyaemia are best treated with large doses of cefuroxime, cefotaxime, or an antibiotic chosen on the basis of laboratory findings (e.g. ampicillin against enterococci). Liver abscesses occur most frequently by spread via the portal tract of intestinal Gram-negative bacilli, or by retrograde spread in the biliary passages of streptococci (especially Str. milleri) and anaerobes from the gallbladder. Ampicillin is selectively concentrated in the bile, and is often useful in treatment of cholecystitis. Amoebic abscess requires prompt and specific treatment with metronidazole, and its possibility should always be kept in mind, particularly in a patient who has been abroad.
Infection caused by the hepatitis viruses B and C has been treated by α-interferon with ribavirin and lamivudine with variable success.
Bone and joint infections
Most infections of bones and joints are due to Staph. aureus. Large doses of flucloxacillin should be given in combination with either fusidic acid or clindamycin unless antibiotic resistant strains are involved which may limit the choice to a glycopeptide or linezolid.
Penicillin in prolonged high dosage is the drug of choice for streptococcal arthritis. Where other organisms, such as H. influenzae, neisseriae or Gram-negative rods are involved, specifically directed therapy is required.
Genital tract infections
Venereal infections such as syphilis and gonorrhoea were traditionally treated with penicillin, but a high proportion of isolates of gonococci are now resistant to this agent, in which case ceftriaxone, co-amoxiclav or ciprofloxacin should be used depending on local patterns.
Non-specific infections of the genital tract are common in women; aerobic and anaerobic bacteria, Candida species or Trichomonas vaginalis, may be involved. Frequently, an abnormal flora is isolated in the absence of an inflammatory exudate, and it may be difficult to decide on the necessity for chemotherapy. Bacterial vaginosis is such a clinical syndrome associated with Mobiluncus spp., which responds to metronidazole or amoxicillin. Vaginal candidiasis is usually treated topically with nystatin or an antifungal imidazole. In trichomoniasis, metronidazole is indicated.
More serious pelvic infection in women is often associated with chlamydiae, and tetracycline or erythromycin is the drug of choice. Azithromycin is a useful single dose agent for uncomplicated genital infection due to chlamydiae. Infection of the fallopian tubes usually involves anaerobic bacteria and metronidazole or co-amoxiclav may be prescribed.
Surgical wound infections
Most surgical infections are caused by the patient’s own organisms, but some arise exogenously, often by cross-infection. In orthopaedic units, most exogenous infections are due to staphylococci, but in gastrointestinal units, Gram-negative bacilli and anaerobes are more common. The situation may change from time to time as a result of ecological movements in the microbial flora within the unit, associated with selective pressures of antibiotic use.
Specimens from infected lesions should always be sent to the laboratory, since the identity of the isolate may have epidemiological significance as well as being of importance in the management of the patient. The microbiologist should always be informed of any therapy as this may affect the interpretation of bacteriological tests.
Superficial infections
Skin and soft tissue infections are common in general practice. Most are of bacterial origin, although some have a fungal or viral aetiology.
Common lesions such as boils, carbuncles, impetigo and infected wounds are associated with Staph. aureus and Str. pyogenes. Systemic treatment with appropriate antibiotics may be indicated in some patients, but topical treatment is often effective. The use of antibiotics commonly prescribed for systemic infections should be avoided in favour of antiseptics or topical antibiotics such as mupirocin.
Finch RG, Davey PG, Wilcox MH, Irving W. Antimicrobial Chemotherapy, ed 6. Oxford: Oxford University Press; 2011.
Finch RG, Greenwood D, Whitley RJ, Norrby SR. Antibiotic and Chemotherapy, ed 9. Churchill Livingstone, Edinburgh: Elsevier; 2011.
Grayson ML, ed. Kucer’s The Use of Antibiotics, ed 6, Butterworth-Heinemann, Oxford: Elsevier, 2010.
Mandell GL, Douglas RG, Bennett JE. Principles and Practice of Infectious Disease, ed 7, Churchill Livingstone, Philadelphia: Elsevier, 2010.
WHO Essential Drug Monitor. http://www.who.int/medicines/publications/monitor/en/.
British Society for Antimicrobial Chemotherapy. http://www.bsac.org.uk/.