The rheumatological examination
Examination anatomy
Inflammatory arthritis affects first the joint synovium. Thickening of this may be palpable and is called pannus. Later, destruction of surrounding structures including tendons, articular cartilages and the bone itself occurs.
Joint pain may be well localised if there is inflammation close to the skin, but deeper joint abnormalities may cause pain to be referred. The areas where joint pain is felt correspond to the innervation of the muscle attached to that joint—the myotome. For example, the glenohumeral joint of the shoulder and the posterior scapular muscles are supplied from C5 and C6, so pain over the shoulder or scapula may arise from any structure supplied from these nerve roots—including the shoulder muscles and joints but also the C5 and C6 segments of the spine. Figure 24.1 shows typical synovial joints affected in rheumatoid arthritis.
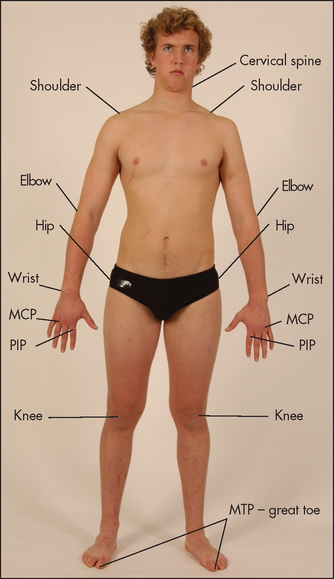
Figure 24.1 Typical synovial joints affected in rheumatoid arthritis (symmetrical, arms and legs, large and small joints) (Courtesy of Glenn McCulloch)
The extra-articular structures that surround a joint—the ligaments, tendons and nerves—may also be the source of joint pain. Disease of the joint itself tends to limit movement of the joint in all directions, both active movement (moved by the patient) and passive movement (moved by the examiner). Extra-articular disease causes variable limitation of movement in different directions and tends to cause more limitation of active movement than of passive movement.
Degenerative arthritis or osteoarthritis (OA) is the most common form of arthritis. It becomes increasingly common with old age. The condition affects synovial joints (see Figure 24.2) and is characterised by a loss of articular cartilage, new bone formation and changes to the shape of the joint. There are certain risk factors for osteoarthritis (see List 24.1).
Although any synovial joint can be affected the condition is more common in certain joints.
GENERAL INSPECTION
There are certain established ways of examining the joints and related structures1 and it is important to be aware of the numerous systemic complications of rheumatological diseases. The actual system of examination depends on the patient’s history and sometimes on the examiner’s noticing an abnormality on general inspection. Formal examination of all the joints is rarely part of the routine physical examination, but students should learn how to handle each joint properly and a formal examination is an important part of the evaluation of patients who present with joint symptoms or who have an established diagnosis and active symptoms. Diseases of the extra-articular soft tissues are particularly common.
General inspection is important for two reasons: first, it gives an indication of the patient’s functional disability, which is essential in all rheumatological assessments; and second, certain conditions can be diagnosed by careful inspection. Look at the patient as he or she walks into the room. Does walking appear to be painful and difficult? What posture is taken? Does the patient require assistance such as a stick or walking frame? Is there obvious deformity, and what joints does it involve? Note the pattern of joint involvement, which gives a clue about the likely underlying disease (see Lists 23.2 and 23.4).
For a more detailed examination the patient should be undressed as far as practical, usually to the underclothes. Depending on the patient’s condition and the parts of the body to be examined, the examination may best be begun with the patient in bed, or sitting over the side of the bed or in a chair, or standing. The opportunity of watching the patient remove the clothes should not be lost because arthritis can interfere with this essential daily task.
Consider the characteristic changes of osteoarthritis (see List 24.2).
Principles of joint examination
Certain general rules apply to the examination of all the joints and they can be summarised as: look, feel, move, measure and compare with the opposite side.
LOOK
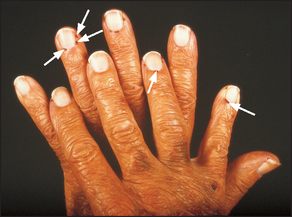
The first principle is always to compare right with left. Remember that joints are three-dimensional structures and need to be inspected from the front, the back and the sides. Inspect the skin for erythema indicating underlying inflammation and suggesting active, intense arthritis or infection, atrophy suggesting chronic underlying disease, scars indicating previous operations such as tendon repairs or joint replacements, and rashes. For example, psoriasis is associated with a rash and polyarthritis (inflammation of more than one joint). The psoriatic rash consists of scaling erythematous plaques on extensor surfaces. The nails are often also affected (see Figure 24.6). Also look for a vasculitic skin rash (inflammation of the blood vessels of the skin), which can range in appearance from palpable purpura or livedo reticularis (bluish-purple streaks in a net-like pattern) to skin necrosis.
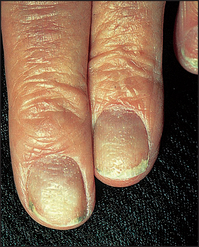
Figure 24.6 Psoriatic nails, showing onycholysis and discolouration, with typical pitting and ridging
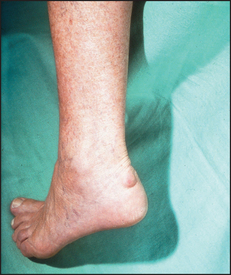
A small, firm, painless swelling over the back (dorsal surface) of the wrist is usually a synovial cyst—a ganglion.a A larger, localised, soft area of swelling of the dorsum of the wrist generally indicates tenosynovitis.
Note any swelling over the joint. There are a number of possible causes: these include effusion into the joint space, hypertrophy and inflammation of the synovium (e.g. rheumatoid arthritis), or bony overgrowths at the joint margins (e.g. osteoarthritis). It may also occur when tissues around the joints become involved, as with the tendinitis or bursitis of rheumatoid arthritis. Swelling of the lower legs may be due to fluid retention, which is painless and can occur in association with inflammation anywhere in the leg. Painful swelling may result from inflammation of the ankle joints or tendons, or of the fascia, or from inflammatory oedema of the skin and subcutaneous tissue.
Deformity is the sign of a chronic, usually destructive, arthritis and ranges from mild ulnar deviation of the metacarpophalangeal joints in early rheumatoid arthritis to the gross destruction and disorganisation of a denervated (Charcot’sb) joint (see Figure 29.13 on page 380). Deviation of the part of the body away from the midline is called valgus deformity, and towards the midline it is called varus deformity. For example, genu valgum means knock-kneed and genu varum means bow-legged.
Look for abnormal bone alignment. Subluxation is said to be present when displaced parts of the joint surfaces remain partly in contact. Dislocation is used to describe displacement where there is loss of contact between the joint surfaces.
Muscle wasting results from a combination of disuse of the joint, inflammation of the surrounding tissues and sometimes nerve entrapment. It tends to affect muscle groups adjacent to the diseased joint (e.g. quadriceps wasting with active arthritis of the knee) and is a sign of chronicity.
FEEL
Palpate for skin warmth. This is done traditionally with the backs of the fingers where temperature appreciation is said to be better. A cool joint is unlikely to be involved in an acute inflammatory process. A swollen and slightly warm joint may be affected by active synovitis (see below), infection (very warm; e.g. Staphylococcus) or crystal arthritis (e.g. gout).
Tenderness is a guide to the acuteness of the inflammation, but may be present over the muscles of patients with fibromyalgia. Tenderness elicited over the margins of a joint indicates inflammation. Where the joint cannot be examined directly (e.g. hips, mid tarsal joints), passive movement that causes pain is a surrogate for this. Tell the patient to state if the examination is becoming uncomfortable. Tenderness can be graded as follows:
Grade I Patient complains of pain
Grade II Patient complains of pain and winces
Grade III Patient complains of pain, winces and withdraws the joint
This may result from joint inflammation or from lesions outside the joints (periarticular tissues), including inflamed tendons, bursae or attachments (entheses). Infected joints are extremely tender and patients will often not let the examiner move the joint at all. Palpation of a joint or area for tenderness must be performed gently, and the patient’s face rather than the joint itself should be watched for signs that the examination is uncomfortable.
Palpate the joint deliberately now, if possible, for evidence of synovitis, which is a soft and spongy (boggy) swelling. This must be distinguished from an effusion, which tends to affect large joints but can occur in any joint. Here the swelling is fluctuant and can be made to shift within the joint. Bony swelling feels hard and immobile, and suggests osteophyte formation or subchondral bone thickening.
MOVE
Much information about certain joints is gained by testing the range of passive movement. (Passive movement is obviously contraindicated in cases of recent injury to the limb or joint, such as a suspected fracture.) Ask the patient to relax and let you move the joint. This must be attempted gently and will be limited if the joint is painful (secondary to muscle spasm), if a tense effusion is present, if there is capsular contraction or if there is a fixed deformity. The joints may have limited extension (called fixed flexion deformity) or limited flexion (fixed extension deformity). Passive movement of the spine is not a practical manoeuvre (unless the examiner is very strong), and active movement is tested here. Active movement is more helpful in assessing integrated joint function. Hand function and gait are usually applied as tests of function. Pain on motion indicates a joint or periarticular problem.
Stability of the joint is important and depends largely on the surrounding ligaments. This is tested by attempting to move the joint gently in abnormal directions to its usual limits, set by ligaments and muscular tone.
Joint crepitus, which is a grating sensation or noise from the joint, indicates irregularity of the articular surfaces. Its presence suggests chronicity.
MEASURE
Accurate measurement of the range of movement of a joint is possible with a goniometer, which is a hinged rod with a protractor in the centre. Open the jaws and line them up with the joint. Measurement of joint movements is performed from the zero starting position. For most joints this is the anatomical position in extension—e.g. the straightened knee. Movement is then recorded as the number of degrees of flexion from this position. A knee with a fixed flexion deformity may be recorded as ‘30° to 60°’, which indicates that there is 30° of fixed flexion deformity and that flexion is limited to 60°. At some joints both flexion and extension from the anatomical position can be measured, as at the wrists. The goniometer is not routinely used by non-rheumatologists and there is a wide range of normal values for joint movement. Most clinicians estimate the approximate joint angles.
A tape measure is useful for measuring and following serially the quadriceps muscle bulk and in examination of spinal movements.
Assessment of individual joints
HANDS AND WRISTS (See Figures 24.3 to 24.8)
Examination anatomy
The articulations between the phalanges are synovial hinge joints. The eight bones of the wrist (carpal bones) form gliding joints that allow wrist movements—flexion/extension and abduction/adduction as they slide over each other.
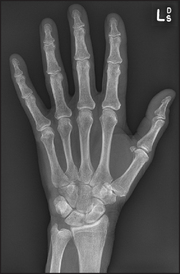
Figure 24.3 X-ray of normal hand (Courtesy M Thomson, National Capital Diagnostic Imaging, Canberra.)
History
Pain may be present in some or all of the joints. It is more likely to be vague or diffuse if it has radiated from the shoulder or neck or is due to carpal tunnel syndrome, and to be localised if it is due to arthritis. Stiffness is typically worse in the mornings in rheumatoid arthritis. Swelling of the wrist may indicate arthritis or tendon sheath inflammation. Swelling of individual joints suggests arthritis. Deformity of the fingers and hand due to rheumatoid arthritis or of the fingers as a result of arthritis or gouty tophi may be the presenting complaint. The sudden onset of deformity suggests tendon rupture. Locking or snapping of a finger (trigger finger) is typical of inflammation of a flexor tendon sheath (tenovaginitis). Loss of function is a serious problem when it involves the numerous functions of the hand and wrist. Ask what problems this has caused. Neurological symptoms as a result of nerve compression may cause paraesthesias, numbness or sometimes hyperaesthesia or limitation of strength or of complicated hand functions.
Examination
First sit the patient over the side of the bed and place the patient’s hands on the pillow with palms down. Often examination of the hands alone will give enough information for the examiner to make a diagnosis. As a result this is quite a popular test in the OSCE.
Look
Start the examination at the wrists and forearms. Inspect the skin for erythema, scleroderma, atrophy, scars and rashes. Look for swelling and its distribution. Next, look at the wrist for swelling, deformity, ulnar and styloid prominence. Then look for muscle wasting of the intrinsic muscles of the hand. This results in the appearance of hollow ridges between the metacarpal bones. It is especially obvious on the dorsum of the hand.
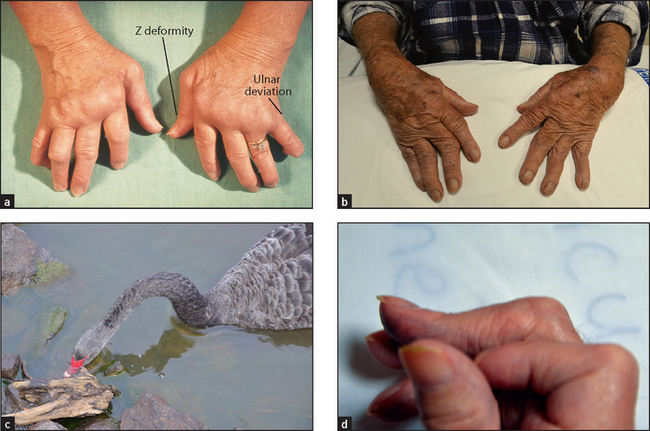
Go on to the metacarpophalangeal joints. Again note any skin abnormalities, swelling or deformity. Look especially for ulnar deviation and volar (palmar) subluxation of the fingers. Ulnar deviation is deviation of the phalanges at the metacarpophalangeal joints towards the medial (ulnar) side of the hand. It is usually associated with anterior (Volar) subluxation of the fingers (see Figure 24.4). These deformities are characteristic but not pathognomonic of rheumatoid arthritis (see List 24.3).
Next inspect the proximal interphalangeal and distal interphalangeal joints. Again note any skin changes and joint swelling. Look for the characteristic deformities of rheumatoid arthritis (see Figure 24.4). These include swan neck and boutonnière deformity of the fingers and Z deformity of the thumb (see Figure 24.4). They are due to joint destruction and tendon dysfunction. The swan neck deformity is hyperextension at the proximal interphalangeal joint and fixed flexion deformity at the distal interphalangeal joint. It is due to subluxation at the proximal interphalangeal joint and tendon shortening at the distal interphalangeal joint. The boutonnière (buttonhole) deformity consists of fixed flexion of the proximal interphalangeal joint and extension of the distal interphalangeal joints. This is due to protrusion of the proximal interphalangeal joint through its ruptured extensor tendon. The Z deformity of the thumb consists of hyperextension of the interphalangeal joint and fixed flexion and subluxation of the metacarpophalangeal joint.
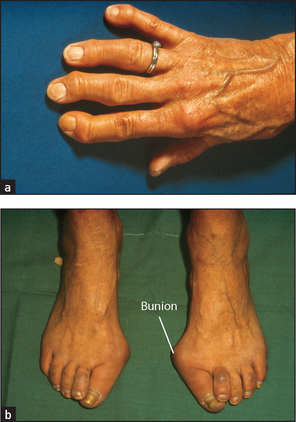
Now look for the characteristic changes of osteoarthritis (see Figure 24.5). Here the distal interphalangeal and first carpometacarpal joints are usually involved. Heberden’s nodesc are a common deformity caused by marginal osteophytes that lie at the base of the distal phalanx. Less commonly, the proximal interphalangeal joints may be involved and osteophytes here are called Bouchard’sd nodes.
Look also to see if the phalanges appear sausage-shaped (dactylitis). This is characteristic of psoriatic arthropathy, but can also occur in patients with reactive arthritis. It is due to interphalangeal arthritis and flexor tendon sheath oedema. Finger shortening due to severe destructive arthritis also occurs in psoriatic disease and is called arthritis mutilans. The hand may take up a main en lorgnette (‘hand holding long-handled opera glasses’) appearance due to a combination of shortening and telescoping of the digits. This is very rare now as a result of improved treatment of rheumatoid arthritis.
Look at the finger pulps for atrophy and digital ulcers, which suggest systemic sclerosis.
Now examine the nails. Characteristic psoriatic nail changes may be visible: these include onycholysis, pitting (small depressions in the nail), onycholysis (see Figure 24.6) and, less commonly, hyperkeratosis (thickening of the nail), ridging (a nonspecific sign) and discolouration. The presence of vasculitic changes around the nail folds implies active disease. These consist of black to brown 1–2 millimetre lesions due to skin infarction and occur typically in rheumatoid arthritis (see Figure 24.7). Splinter haemorrhages may be present in patients with systemic lupus erythematosus (and infective endocarditis) and are due to vasculitis. Unlike nail-fold infarcts they are located under the nails in the nail beds. Periungual telangiectasias occur in systemic lupus erythematosus, scleroderma or dermatomyositis.
Now turn the patient’s hands over and reveal the palmar surfaces. Look at the palms for scars (from tendon repairs or transfers), palmar erythema and muscle wasting of the thenar or hypothenar eminences (due to disuse, vasculitis or peripheral nerve entrapment). A Dupuytren’s contracture may be visible (page 188). Telangiectasia here would support the diagnosis of scleroderma.
Feel and move
Turn the hands back again to the palm-down position. Palpate the wrists with both thumbs placed on the dorsal surface by the wrists, supported underneath by the index fingers (see Figure 24.8). Feel gently for synovitis (boggy swelling) and effusions. The wrist should be gently dorsiflexed (normally possible to 75°) and palmar flexed (also possible to 75°) with your thumbs. Then radial and ulnar deviation (20°) is tested (see Figure 24.9). Note any tenderness or limitation of movement or joint crepitus. Palpate the ulnar styloid for tenderness, which can occur in rheumatoid arthritis.
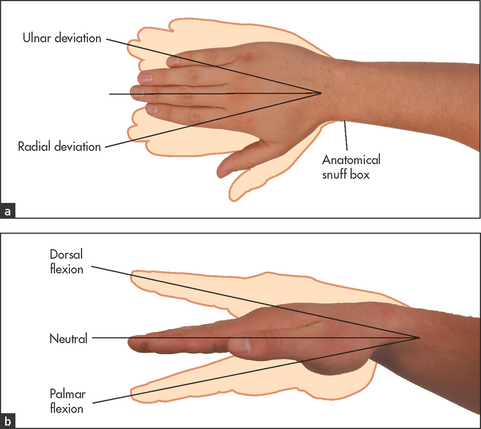
Figure 24.9 Movements of the wrist joint (a) Ulnar and radial deviation; (b) dorsal and palmar flexion. (Courtesy of Glenn McCulloch)
Now turn the patient’s hands over and reveal the palmar surfaces. Look at the palms for scars (from tendon repairs or transfers), palmar erythema and muscle wasting of the thenar or hypothenar eminences (due to disuse, vasculitis or peripheral nerve entrapment). A Dupuytren’s contracture may be visible (page 188). Telangiectasia here would support the diagnosis of scleroderma.e tenosynovitis. Boggy swelling distal to the styloid suggests synovitis.
Feel for tenderness in the anatomical snuff box which can be the result of first carpometacarpal joint arthritis or to scaphoid injury (see Figure 24.9). Test for tenderness distal to the head of the ulna for extensor carpi ulnaris tendinitis.
Go on now to the metacarpophalangeal joints, which are palpated in a similar way with the two thumbs. Again passive movement is tested. The joint are best examined in 90° flexion, which opens the joint margins. Volar subluxation can be demonstrated by flexing the metacarpophalangeal joint with the proximal phalanx held between the thumb and forefinger. The metacarpophalangeal joint is then rocked backwards and forwards (see Figure 24.10). Very little movement occurs with this manoeuvre at a normal joint. Considerable movement may be present when ligamentous laxity or subluxation is present.
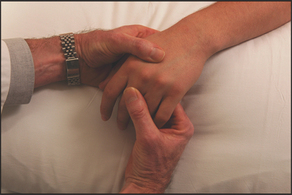
Figure 24.10 Examination for volar subluxation at the metacarpophalangeal joints (Courtesy of Glenn McCulloch)
Palpate the proximal and distal interphalangeal joints for tenderness, swelling and osteophytes. Use the thumb and forefinger of each hand and examine in two planes.
Next test for palmar tendon crepitus. Place the palmar aspects of your fingers against the palm of the patient’s hand while he or she flexes and extends the metacarpophalangeal joints. Inflamed palmar tendons can be felt creaking in their thickened sheaths and nodules can be palpated. This indicates tenosynovitis.
A trigger finger may also be detected by this manoeuvre. Here, the thickening of a section of digital flexor tendon is such that it tends to jam when passing through a narrowed part of its tendon sheath. Rheumatoid arthritis is an important cause. Typically, flexion of the finger occurs freely up to a certain point where it sticks and cannot be extended (as flexors are more powerful than extensors). The application of greater force overcomes the resistance with a snap.
If the carpal tunnel syndrome is suspected, ask the patient to flex both wrists for 30 seconds—paraesthesias will often be precipitated in the affected hand if the syndrome is present (Phalen’sf wrist flexion test). The paraesthesias (pins and needles) are in the distribution of the median nerve (page 446), when thickening of the flexor retinaculum has entrapped the nerve in the carpal tunnel (see List 24.4). This test is more reliable than Tinel’sg sign, in which tapping over the flexor retinaculum (which lies at the proximal part of the palm) may cause similar paraesthesias.2
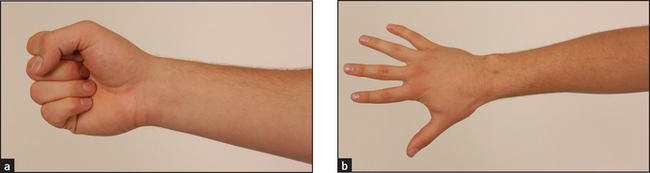
Now test active movements. First assess wrist flexion and extension as shown in Figure 24.11. Compare the two sides. Now go on to thumb movements (see Figure 24.12). The patient holds the hand flat, palm upwards, and your hand holds the patient’s fingers. Test extension by asking the patient to stretch the thumb outwards, abduction by asking for the thumb to be pointed straight upwards, adduction by asking the patient to squeeze your finger and opposition by getting the patient to touch the little finger with the thumb. Look for limitation of these movements and discomfort caused by them. Next test metacarpophalangeal and interphalangeal movements. As a screening test, ask the patient to make a fist then to straighten out the fingers (see Figure 24.13). Then test the fingers individually. If active flexion of one or more fingers is reduced, test the superficial and profundus flexor tendons (see Figure 24.14). Hold the proximal finger joint extended and instruct the patient to bend it; the distal fingertip will flex if the flexor profundus is intact. Then hold the other fingers extended (to inactivate the profundus) with the finger to be tested resting above your fingers and instruct the patient to bend the finger (inability indicates the superficialis is unable to work). The most common tendon ruptures are of the extensors of the fourth and fifth fingers.
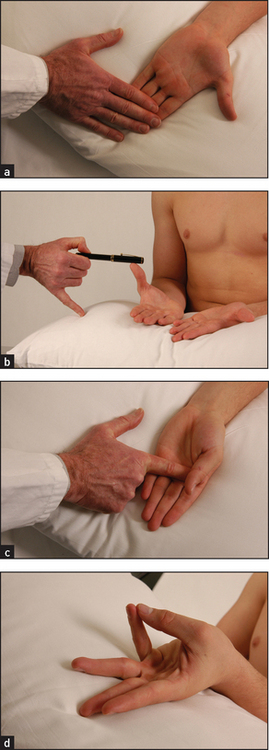
Figure 24.12 Thumb movements (a) Extension; (b) abduction; (c) adduction; (d) opposition. (Courtesy of Glenn McCulloch)
Function
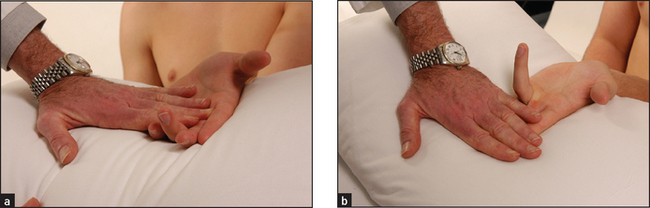
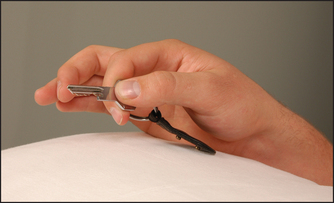
It is important to test the function of the hand. Grip strength is tested by getting the patient to squeeze two of your fingers. Even an angry patient will rarely cause pain if given only two fingers. Serial measurements of grip strength can be made by asking the patient to squeeze a partly inflated sphygmomanometer cuff and noting the pressure reached. Key grip (see Figure 24.15) is the grip with which a key is held between the pulps of the thumb and forefinger. Ask the patient to hold this grip tightly and try to open up his or her fingers. Opposition strength (see Figure 24.16) is where the patient opposes the thumb and individual fingers. The difficulty with which these can be forced apart is assessed. Finally, a practical test, such as asking the patient to undo a button or write with a pen, should be performed.
Tests of hand function should be completed by formally assessing for neurological changes (Chapter 34).
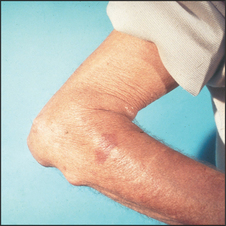
Examination of the hands is not complete without feeling for the subcutaneous nodules of rheumatoid arthritis near the elbows (see Figure 24.17). These are 0.5–3 centimetre firm, shotty,h non-tender lumps that occur typically over the olecranon. They may be attached to bone. They are found in rheumatoid factor-positive rheumatoid arthritis. Rheumatoid nodules are areas of fibrinoid necrosis with a characteristic histological appearance and are probably initiated by a small vessel vasculitis. They are localised by trauma but can occur elsewhere, especially attached to tendons, over pressure areas in the hands or feet, in the lung, pleura, myocardium or vocal cords. They are most commonly found firmly attached over the proximal ulna, just distal to the elbow. Occasionally they are within the olecranon bursa and can be moved freely within it. The combination of arthritis and nodules suggests the diagnostic possibilities outlined in List 24.5.
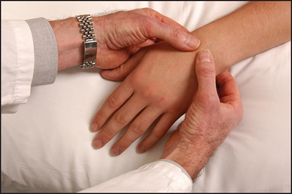
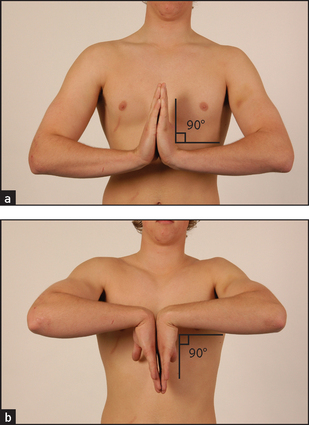
If the patient has diabetes mellitus, look for the features of diabetic cheiroarthropathy and then test function. The skin appears thick and tight and the patient may be unable to extend all digits fully. This is different to Dupuytren’s contractures, which usually affect only the fourth and fifth digits. Two simple tests can be helpful:
• To recognise contractures in the metacarpophalangeal, proximal interphalangeal and distal interphalangeal joints, ask the patient to bring the flat of the hands together as if praying (prayer sign).
• To recognise contractures in the metacarpophalangeal joints, ask the patient to flatten the palm against the surface of a table (table top test).
ELBOWS
Examination anatomy
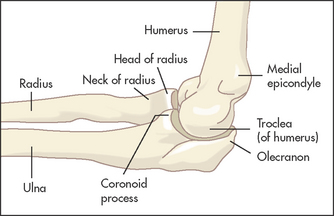
The humerus, radius and ulna meet at the elbow, which is a hinge and a pivot joint (see Figure 24.18). Pivoting occurs between the radius and ulna, and the articulation between all three bones forms a hinge joint.
History
Pain from the elbow is usually diffuse and may radiate down the forearm. It may occur over the lateral or medial epicondyle if the patient has tendinitis (tennis or golfer’s elbow). The patient may have noticed some swelling as a result of inflammation. Swelling over the back suggests olecranon bursitis. Stiffness may interfere with elbow movements and the patient may complain of difficulty combing the hair. When supination and pronation are affected the patient may complain of difficulty with carrying and holding. If the patient is aware of the elbow moving abnormally this suggests instability of the joint and may be a result of rheumatoid arthritis or trauma. Ulnar nerve trauma at the elbow may lead to a complaint of numbness or paraesthesias in the distribution of that nerve.
Examination
Watch as the patient undresses, for difficulty disentangling the arms from clothing. The upper arms should be exposed completely. Note any deformity or difference in the normal 5–10° valgus position (carrying anglei) as the patient stands with the palms facing forwards.
Look for a joint effusion, which appears as a swelling on either side of the olecranon. Discrete swellings over the olecranon or over the proximal subcutaneous border of the ulna may be due to rheumatoid nodules, gouty tophi, an enlarged olecranon bursa or, rarely, to other types of nodules (see List 24.5).
Feel for tenderness, particularly over the lateral and medial epicondyles, which may indicate tennis or golfer’s elbow, respectively. Palpate any discrete swellings. Rheumatoid nodules are quite hard, may be tender and are attached to underlying structures. Gouty tophi have a firm feeling and often appear yellow under the skin, but are sometimes difficult to distinguish from rheumatoid nodules. A fluid collection in the olecranon bursa is softly fluctuant and may be tender if inflammation is present. These collections are associated with rheumatoid arthritis and gout, but often occur independently of these diseases.
Small amounts of fluid or synovitis of the elbow joint may be detected by the examiner, facing the patient, placing the thumb of the opposite hand along the edge of the ulnar shaft just distal to the olecranon where the synovium is closest to the surface. Full extension of the elbow joint will cause a palpable bulge in this area if fluid is present.
Move the elbow joints passively. The elbow is a hinge joint. The zero position is when the arm is fully extended (0°). Normal flexion is possible to 150°. Limitation of extension is an early sign of synovitis.
If lateral epicondylitis is suspected, ask the patient to extend the wrist actively against resistance. Test the range of active movements by standing in front of the patient and demonstrating. If there is any deformity or complaint of numbness, a neurological examination of the hand and arm is indicated for ulnar nerve entrapment.
SHOULDERS
Examination anatomy
The shoulder is the most mobile joint in the body. It involves three bones: the clavicle, the scapula and the humerus (see Figure 24.19). The acromioclavicular joint is formed by the acromion of the scapula and the clavicle. Movements of the shoulder are a result of a combination of ball-and-socket articulation at the glenohumeral joint (between the glenoid cavity [fossa] of the scapula and the ball-shaped end of the humerus) and motion between the scapula and the thorax. Seventeen muscles are involved. Stability of the joint itself depends on four muscles: supraspinatus, infraspinatus, teres minor and subscapularis—the rotator cuff muscles. The shallow glenoid fossa is extended by a cartilage rim (the glenoid labrum). This cushions the humeral head and increases the depth and surface area of articulation. Instability of the joint can result from abnormality of, or injury to, any of these structures.
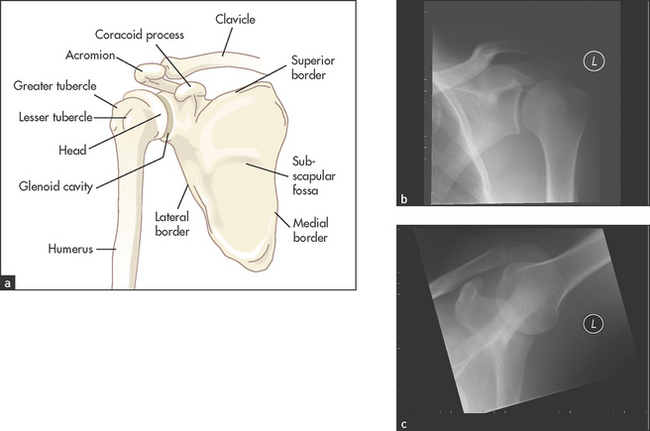
Figure 24.19 Examination of the shoulders (a) Anatomy of the shoulder. (b) X-ray of left shoulder in the neutral position; the relative positions of the humeral head, clavicle and scapulae can be seen. (c) X-ray of left shoulder in abduction. Abduction of the arm rotates the head of the humerus and the clavicle moves upwards. (X-rays courtesy M Thomson, National Capital Diagnostic Imaging, Canberra.)
The joint is encased in a capsule and is lined with synovium.
This complicated joint is frequently affected by a number of non-arthritic conditions involving its bursa, capsule and surrounding tendons; for example, ‘frozen (stiff) shoulder’ (adhesive capsulitis), tendinitis and bursitis. All of these disorders affect movement of the shoulder.
Instability of the joint can result in dislocation (all contact between the articular surfaces is lost) or subluxation (partial contact remains). Anterior dislocation or subluxation tends to occur after a fall onto an outstretched arm. More chronic instability is associated with gradual stretching of the supporting structures by sporting or work activities that involve use of the arm above the head. Patients with ligamentous laxity may have multidirectional instability and some are able to dislocate their shoulders voluntarily (e.g. at parties).
History
Pain is the most common symptom of a patient with shoulder problems.3 Typically it is felt over the front and lateral part of the joint. It may radiate to the insertion of the deltoid or even further. Pain felt over the top of the shoulder is more likely to come from the acromioclavicular joint or from the neck. Deformity has to be severe before it becomes obvious. Pain and stiffness may severely limit shoulder movement. Instability may cause the alarming feeling that the shoulder is jumping out of its socket. This is most likely to occur during abduction and external rotation (e.g. while attempting to serve a tennis ball). Loss of function may result in difficulty using the arms at above shoulder height or reaching around to the back.
Examination
Watch the patient undressing and note forward, backward and upward movements of the shoulders and whether these seem limited or cause the patient pain. Stand back and compare the two sides. The arms should be held at the same level and the outlines of the acromioclavicular joints should be the same. There may be wasting of one of the deltoid muscles that will not be obvious unless the two are compared. Deltoid wasting is characteristic of shoulder problems, whereas trapezius muscle wasting suggests cervical spine problems.
Look at the joint. A swelling may be visible anteriorly, but unless effusions are large and the patient is thin these are difficult to detect. Look for asymmetry and for scars as a result of injury or previous surgery.
Feel for tenderness and swelling. Stand beside the patient, rest one hand on the patient’s shoulder and move the arm into different positions (see below). As the shoulder moves, feel the acromioclavicular joint and then move your hand along the clavicle to the sternoclavicular joint.
Move the joint (see Figures 24.20 and 24.21). The zero position is with the arm hanging by the side of the body so that the palm faces forwards. Abduction tests glenohumeral abduction, which is normally possible to 90°. For the right shoulder, stand behind the patient resting your left hand on the patient’s shoulder, while your right hand abducts the elbow from the shoulder. Elevation is usually possible to 180° when it is performed actively, as movement of the scapula is then included. Adduction is possible to 50°. The arm is carried forwards across the front of the chest. External rotation is possible to 65°. With the elbow bent to 90° the arm is turned laterally as far as possible. Internal rotation is usually possible to 90°. It is tested actively by asking the patient to place his or her hand behind the back and then to try to scratch the back as high up as possible with the thumb. Patients with rotator cuff problems complain of pain when they perform this manoeuvre. Flexion is possible to 180°, of which the glenohumeral joint contributes about 90°. Extension is possible to 65°. The arm is swung backwards as in marching. During all these manoeuvres, limitation with or without pain and joint crepitus are assessed.
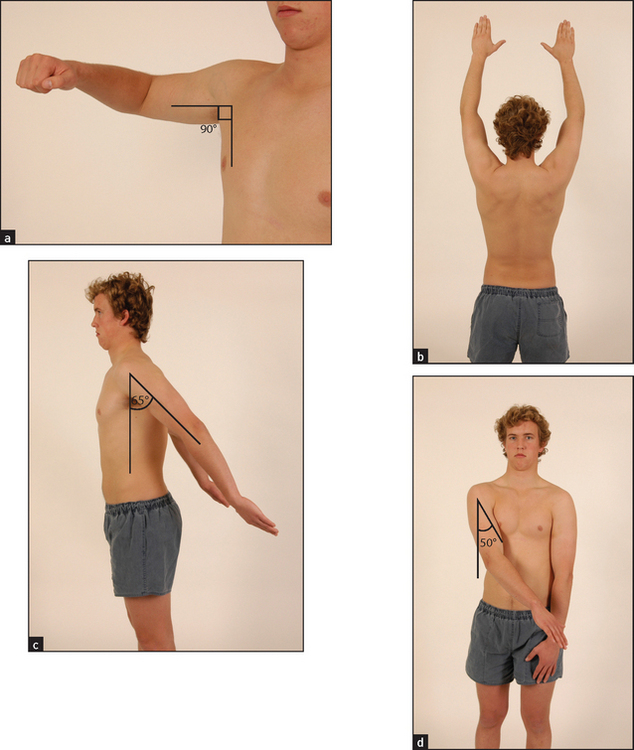
Figure 24.20 Movements of the shoulder joint (a) Abduction using the glenohumeral joint; (b) abduction using the glenohumeral joint and the scapula; (c) extension; (d) adduction. (Courtesy of Glenn McCulloch)
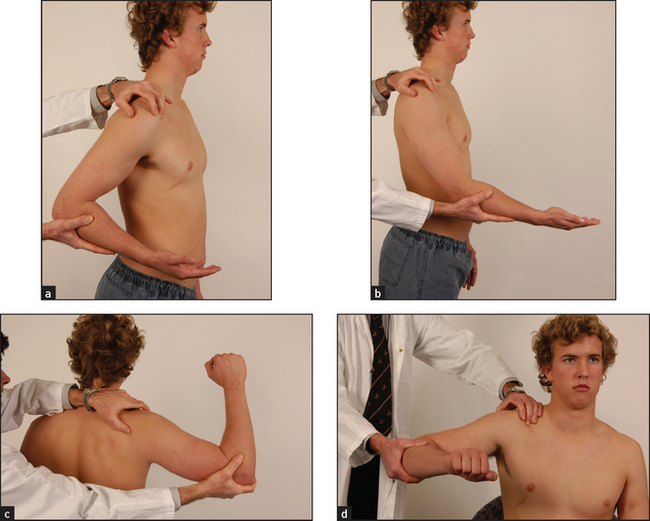
Figure 24.21 Examining the shoulder joint (a) Extension; (b) flexion; (c) apprehension test; (d) internal rotation and abduction. (Courtesy of Glenn McCulloch)
Rapid assessment of shoulder movement is possible using the three-step Apleyj scratch test (see Figure 24.22). Stand behind and ask the patient to scratch an imaginary itch over the opposite scapula, first by reaching over the opposite shoulder, next by reaching behind the neck and finally by reaching behind the back. If this test is normal there is usually no need to test passive shoulder movements.
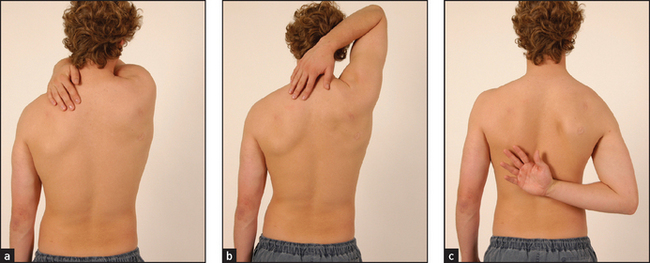
Figure 24.22 (a) to (c) Apley scratch test to assess shoulder movement (Courtesy of Glenn McCulloch)
The anterior stability of the shoulder joint is traditionally assessed by the apprehension test. Stand behind the patient, abduct, extend and externally rotate the shoulder (see Figure 24.21) while pushing the head of the humerus forwards with the thumb. The patient will strongly resist this manoeuvre if there is impending dislocation (LR+ 1.8, LR– 0.234). There will be a similar response if the arm is adducted and internally rotated and posterior dislocation is about to occur. The clunk test is probably kinder to the patient and more accurate. The patient lies supine with the arm fully abducted. It is then put into full external rotation and the head of the humerus is pushed a little anteriorly. Rather than looking for signs of distress, the examiner listens and feels for a grinding sensation from the shoulder (LR+ 16, LR– 0.67).
This is also the time to test biceps function. The patient flexes the elbow against resistance. A ruptured biceps tendon causes the biceps muscle to roll up into a ball.
As a general rule, intra-articular disease produces painful limitation of movement in all directions, while tendinitis produces painful limitation of movement in one plane only and tendon rupture or neurological lesions produce painless weakness. For example, if the abnormal sign is limited shoulder abduction in the middle range (45–135°), this suggests rotator cuff problems (i.e. the supraspinatus, infraspinatus, subscapularis and teres minor muscles) rather than arthritis.
Bicipital tendinitis causes localised tenderness over the groove. The supraspinatus tendon is a little higher, just under the anterior surface of the acromion. Supraspinatus tendinitis is common. Testing for it involves placing a finger over the head of the tendon while the shoulder is in extension. As this pushes the tendon forwards against your finger, the movement is painful. When the shoulder is then flexed the tendon moves away and the pain disappears.
Do not forget that arthritis affecting the acromioclavicular joint can be confused with glenohumeral disorders. Also remember to examine the neck and axillae in patients with shoulder pain.
TEMPOROMANDIBULAR JOINTS
History
The usual symptoms of temporomandibular joint dysfunction include clicking and pain on opening the mouth. The jaw may sometimes lock in the open position.
Examination
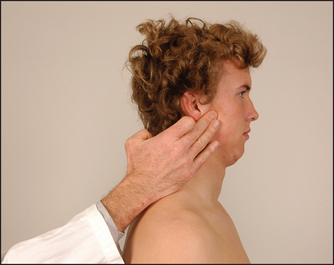
Look in front of the ear for swelling. Feel by placing a finger just in front of the ear while the patient opens and shuts the mouth (see Figure 24.23). The head of the mandible is palpable as it slides forwards when the jaw is opened. Clicking and grating may be felt. This is sometimes associated with tenderness if the joint is involved in an inflammatory arthritis. Rheumatoid arthritis may affect the temporomandibular joint.
NECK
Examination anatomy—the spine
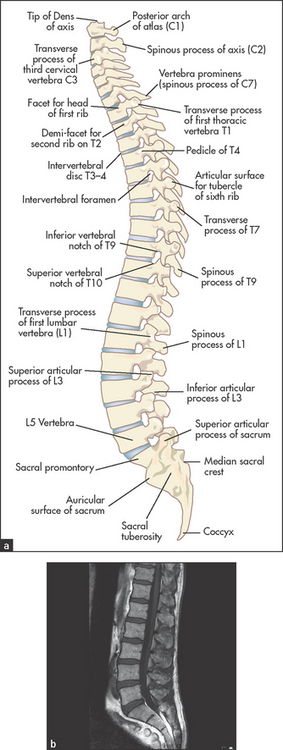
The spinal column (see Figure 24.24) is like a tower of bones that protects the spinal cord and houses its blood supply and efferent and afferent nerves. It provides mechanical support for the body and is flexible enough to allow bending and twisting movements. There are diarthrodial joints between the articular processes of the vertebral bodies, and the vertebral bodies are separated by the vertebral discs. These pads of cartilage are flexible enough to allow movement between the vertebrae. In the cervical spine from C3 to C7, the uncovertebral joints of Luschkak are present. These are formed between a lateral bony extension (uncinate process) from the margin of the more inferior vertebral body with the one above. Osteoarthritic hypertrophy of these joints may result in pain or nerve root irritation.
History
Pain is the most common neck symptom. Musculoskeletal neck pain usually arises in the structures at the back of the neck: the cervical spine, the splenius, semispinalis and trapezius muscles, or in the cervical nerves or nerve roots. Pain in the front of the neck may come from the oesophagus, trachea, thyroid gland or anterior neck muscles (e.g. sternomastoid and platysma). Pain may be referred to the front of the neck from the heart.
There may be a history of trauma from direct injury or a sudden deceleration causing hyperextension of the neck: ‘whiplash’ injury. Injury can also be caused by attempted therapeutic neck manipulations. The possibility of spinal cord injury must be considered in these patients. Ask about weakness or altered sensation in the arms and legs and any problem with bowel or bladder function.
The pain may have begun suddenly, suggesting a disc prolapse, or more gradually due to disc degeneration.
Postural tendon and muscle strains are common causes of temporary neck pain. These are often related to overuse. Ask about the patient’s occupation and whether work or recreational activities involve repeated and prolonged extension of the neck (e.g. painters and cyclists). These patients often describe neck stiffness, and pain and muscle spasm are often present. The repeated holding of a telephone between the shoulder and the ear can cause nerve root problems. Neck movement may cause radicular symptoms such as paraesthesias in the distribution of a cervical nerve after a hyperextension injury or cervical spine arthritis. Ask about paraesthesias and weakness in the arms and hands.
Deformity may occur as a result of muscle spasm or sometimes following disc prolapse. Torticollis is a chronic and uncontrollable twisting of the neck to one side as a result of a muscle dystonia or cervical nerve root problem.
Examination
The patient should be undressed so as to expose the neck, shoulders and arms (see Figure 24.25).
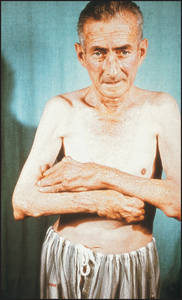
Figure 24.25 Rheumatoid arthritis Note the head tilt due to right atlanto-axial subluxation, the rheumatoid hands and the subcutaneous rheumatoid nodules.
Look at the cervical spine while the patient is sitting up, and note particularly his or her posture. Movement should be tested actively. Flexion is tested by asking the patient to try to touch his or her chest with the chin (normal flexion is possible to 45°). Extension (see Figure 24.26(a)) is tested by asking the patient to look up and back (normally possible to 45°). Lateral bending (see Figure 24.26(b)) is tested by getting the patient to touch his or her shoulder with the ear; lateral bending is normally possible to 45°. Rotation is tested by getting the patient to look over the shoulder to the right and then to the left. This is normally possible to 70°.
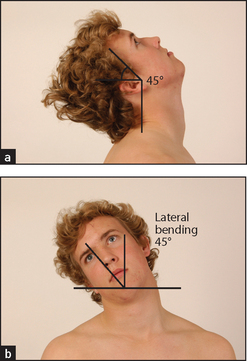
Figure 24.26 Movements of the neck (a) Extension—‘Look up and back’; (b) lateral bending—‘Now touch your right ear onto your shoulder’ (45°); rotation—‘Now look over your shoulder to the right and then to the left’ (70°). (Courtesy of Glenn McCulloch)
Feel the posterior spinous processes. This is often easiest to do when the patient lies prone with the chest supported by a pillow and the neck slightly flexed. Feel for tenderness and uneven spacing of the spinous processes. Tenderness of the facet joints will be elicited by feeling a finger’s breadth lateral to the middle line on each side (see Figure 24.27).
Neurological examination of the upper limbs, including testing of shoulder abduction (C5, C6) and the serratus anterior muscle (C5, C6, C7), is part of the assessment of the neck.
THORACOLUMBAR SPINE AND SACROILIAC JOINTS
History
Lower back pain is a very common symptom (see List 24.6). The discomfort is usually worst in the lumbosacral area. Ask whether the onset was sudden and associated with lifting or straining or whether it was gradual.5,6 Stiffness and pain in the lower back that is worse in the morning is characteristic of an inflammatory spondyloarthritis. Pain that shoots from the buttock and thigh along the sciatic nerve distribution is called sciatica. In sciatic nerve compression at a lumbosacral nerve root, the pain is often aggravated by coughing or straining or when the patient leans forwards slightly, for example to brush the teeth. The back pain that patients may call ‘lumbago’ is often due to referred pain (e.g. from the vertebral joints). There may be other neurological symptoms in the legs due to nerve compression or irritation. The distribution of the paraesthesias or weakness may indicate the level of spinal cord or nerve root abnormality. Ask about urinary incontinence and retention as well as numbness in the ‘saddle region’, erectile dysfunction and bowel incontinence, which can be a result of cauda equina involvement.
Examination
To start the examination, have the patient standing and clothed only in underpants. Look for deformity, inspecting from both the back and the side. Note especially loss of the normal thoracic kyphosis and lumbar lordosis, which is typical of ankylosing spondylitis. Also note any evidence of scoliosis, a lateral curvature of the spine that may be simple (‘C’ shaped) or compound (‘S’ shaped) and that can result from trauma, developmental abnormalities, vertebral body disease (e.g. rickets, tuberculosis) or muscle abnormality (e.g. polio).
Feel each vertebral body for tenderness and palpate for muscle spasm.5
Movement is assessed actively. Bending movements largely take place at the lumbar spine, while rotational movements occur at the thoracic spine. Range of movement is tested by observation (see Figure 24.28) and the use of Schober’s test (see below and Figure 24.29).
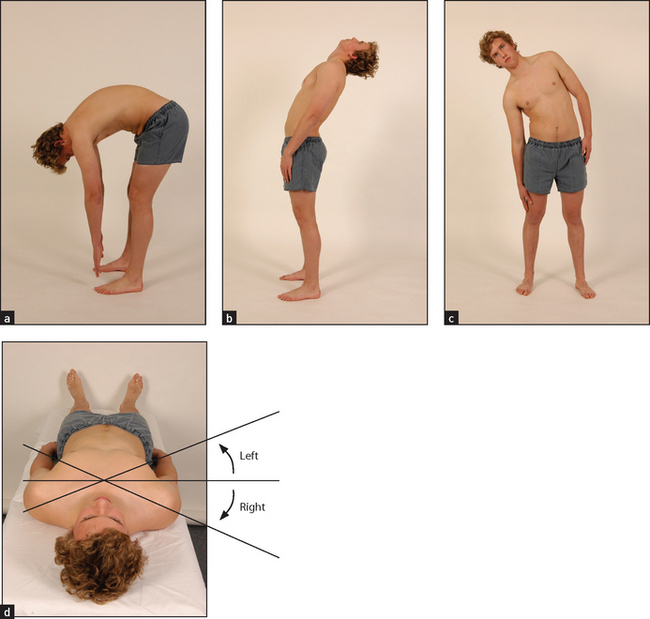
Figure 24.28 Movements of the thoracolumbar spine (a) Flexion; (b) extension; (c) lateral bending; (d) rotation. (Courtesy of Glenn McCulloch)
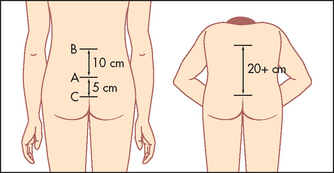
Figure 24.29 Schober’s test (From Douglas G, Nicol F and Robertson C. Macleod’s clinical examination, 12th edn. Edinburgh: Churchill Livingstone, 2009, with permission.) Churchill Livingstone
Flexion is tested by asking the patient to touch the toes with the knees straight. The normal range of flexion is very wide. Many people can reach only halfway down the shins when the knees are kept straight. As the patient bends, look at the spine: there is normally a gentle curve along the back from the shoulders to the pelvis. Patients with advanced ankylosing spondylitis have a flat ankylosed spine and all the bending occurs at the hips. Test extension by asking the patient to lean backwards. Patients with back pain usually find this less uncomfortable than bending forwards. Lateral bending is assessed by getting the patient to slide the right hand down the right leg as far as possible without bending forwards, and then the same for the left side. This movement tends to be restricted early in ankylosing spondylitis. Rotation is tested with the patient sitting on a stool (to fix the pelvis) and asking him or her to rotate the head and shoulders as far as possible to each side. This is best viewed from above.
Measure the lumbar flexion with Schober’s test (see Figure 24.29). Make a mark at the level of the posterior iliac spine on the vertebral column (approximately at L5). Place one finger 5 centimetres below and another 10 centimetres above this mark. Ask the patient to touch the toes. An increase of less than 5 centimetres in the distance between the two fingers indicates limitation of lumbar flexion. The finger-to-floor distance at full flexion can be measured serially to give an objective indication of disease progression.
Assess straight leg raising (Lasègue’sl test includes passive ankle dorsiflexion). With the patient lying down, lift the straightened leg if sciatica is suspected (normally to 80–90°). This will be limited by pain in lumbar disc prolapse (less than 60°).
Press directly on the anterior superior iliac spine on each side and apply lateral pressure so as to attempt to separate them. This may elicit pain in the sacroiliac joints when patients have sacroiliitis.
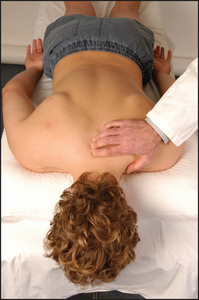
Now get the patient to lie in bed on the stomach. Look for gluteal wasting. The sacroiliac joints lie deep to the dimples of Venus.m By tradition, firm palpation with both palms overlying each other is used to elicit tenderness in patients with sacroiliitis. Test each side separately.
Now ask the patient to lie on one side. Apply firm pressure to the upper pelvic rim. This will also elicit pain in the sacroiliac joints.
The complete examination of the back also requires neurological assessment of the lower limbs.7
HIPS
Examination anatomy
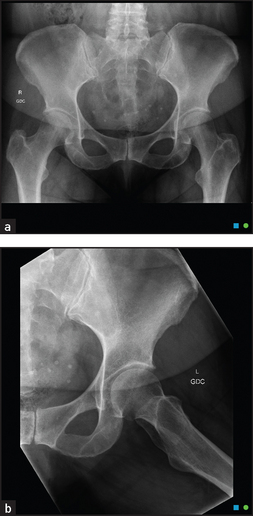
The hip is a ball-and-socket synovial joint (see Figure 24.30). The socket is formed by three bones: the ilium, the ischium and the pubis. The ball is the head of the femur. Surrounding tendons and nerves may cause symptoms that need to be distinguished from hip abnormalities.
History
The word ‘hip’ is used variably by patients to indicate a number of sites including the buttocks, low back or trochanteric region. Ask the patient to point to the site of pain (see List 24.7). The patient with true hip joint problems will often have pain that is felt anteriorly in the groin or may radiate to the knee. Athletes with ‘groin strain’ often have adductor tendinitis or osteitis pubis caused by trauma or overuse. Pain over the greater trochanter is more often a result of trochanteric bursitis, gluteus medius tendinitis or tear. It is exacerbated by crossing the legs. Find out what sport the patient plays. The condition is common in sports involving running. Typically the pain is present at the start of exercise and improves as the athlete ‘warms up’, only to recur later at rest. Take a detailed work history. Overuse syndromes related to work may be worst on Fridays and improve over the weekend. Jumping down off trucks or platforms may cause repeated trauma to the joint.
A limp may be noticed by the patient. When associated with pain it is a compensating mechanism, but when painless it may be due to differing limb length or instability of the joint. Patients are sometimes aware of clicking or snapping coming from the region of the hip. This may be due to a psoas bursitis or to slipping of the tendon of the gluteus maximus over the edge of the greater trochanter. Functional impairment usually results in difficulty walking and climbing stairs. Sitting down and standing up can become progressively more uncomfortable because of stiffness and pain.
A history of a fall and inability to walk or bear weight on the leg suggests a fracture of the neck of the femur. A history of rheumatoid arthritis and pain that is present at rest suggests rheumatoid arthritis of the hip. Osteoarthritis is more likely to evolve gradually in older people and is associated with obesity and with recurrent trauma.
Ask about systemic symptoms such as fever and weight loss, which might be a sign of septic arthritis.
Pain that is associated with paraesthesias and radiates in the distribution of the lateral cutaneous nerve of the thigh suggests an entrapment syndrome (meralgia paraesthetica).
Examination
Watch the patient walking into the room and note the use of a walking stick, a slow and obviously uncomfortable gait or a limp.
Get the patient to lie down, first on the back.
Looking at the hip joint itself is not possible because so much muscle overlies it. However, you must inspect for scars and deformity. The patient may adopt a position with one leg rotated because of pain.
Feel just distal to the midpoint of the inguinal ligament for joint tenderness. This point lies over the only part of the femoral head that is not intraacetabular. Now feel for the positions of the greater trochanters. Place your thumbs on the anterior superior iliac spine on each side while moving your fore and middle fingers posteriorly to find the tips of the greater trochanters. These should be at the same level. If one side is higher than the other, the higher side is likely to be the abnormal one.
Move the hip joint passively (see Figure 24.31). Flexion is tested by flexing the patient’s knee and moving the thigh towards the chest. Keep the pelvis on the bed by holding the other leg down. A fixed flexion deformity (inability to extend a joint normally) may be masked by the patient’s arching the back and tilting the pelvis forwards and increasing lumbar lordosis unless Thomas’n test is applied. The legs are fully flexed to straighten the pelvis. One leg is then extended. A fixed flexion deformity (e.g. as result of osteoarthritis) will prevent straightening. Rotation is tested with the knee and hip flexed. One hand holds the knee, the other the foot. The foot is then moved medially (external rotation of the hip, normally possible to 45°), then laterally (internal rotation of the hip, normal to 45°). Abduction is tested by standing on the same side of the bed as the leg to be tested. The right hand grasps the heel of the right leg while the left hand is placed over the anterior superior iliac spine to steady the pelvis. The leg is then moved outwards as far as possible. This is normally possible to 50°. Adduction is the opposite. The leg is carried immediately in front of the other limb and this is normally possible to 45°.
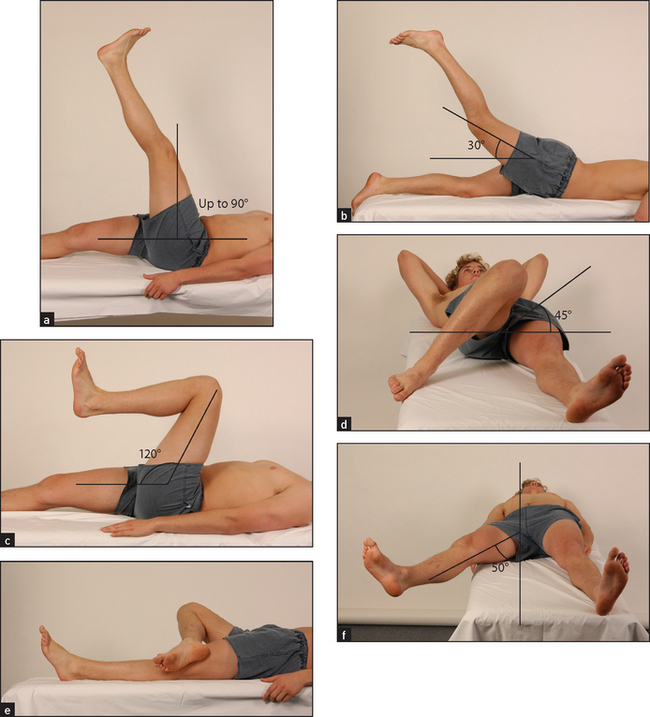
Figure 24.31 Movements of the hip (a) Flexion; (b) extension; (c) flexion, knee bent; (d) internal rotation; (e) external rotation; (f) abduction. (Courtesy of Glenn McCulloch)
Ask the patient to roll over onto the stomach. Extension is then tested by placing one hand over the sacroiliac joint while the other elevates each leg. This is normally possible to about 30°. Ask the patient to stand now and perform the Trendelenburgo test. The patient stands first on one leg and then on the other. Normally the non-weight-bearing hip rises, but with proximal myopathy or hip joint disease the non-weight-bearing side sags.
Finally, the true leg length (from the anterior superior iliac spine to the medial malleolus) and apparent leg length (from the umbilicus to the same lower point) for each leg should be measured. A difference in true leg length indicates hip disease on the shorter side, while apparent leg length differences are due to tilting of the pelvis.
In patients with osteoarthritis of the joint, internal rotation, abduction and extension are usually restricted.8 Osteoarthritic joints show loss of joint space, sclerosis (thickening and increased radiodensity) at the joint margins and osteophyte (bony outgrowth) formation on plain X-ray films.
KNEES
Examination anatomy
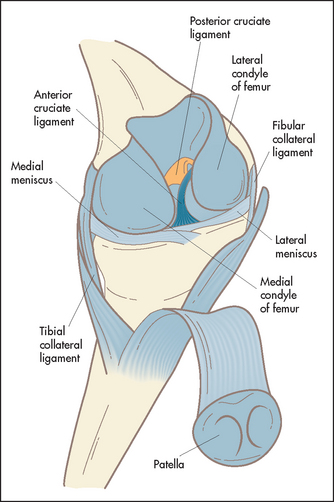
The knee is a complex hinge joint formed by the distal femur, the patella and the proximal end of the tibia (see Figure 24.32). The bones are enclosed in a joint capsule with an extensive synovial membrane. Lateral stability is provided by the lateral collateral ligaments, and antero-posterior movement is restricted by the cruciate ligaments. There is extensive articular cartilage that acts as a shock absorber and allows smooth gliding movements between the ends of the bones.
History
Pain is a common knee problem (see Table 24.1). If there has been an injury or if the pain is due to a mechanical abnormality, it is often localised. Inflammatory diseases more often cause diffuse pain. Ask the patient to point to the place where the pain is most severe. Stiffness is usually of gradual onset and is typical of osteoarthritis. It tends to be worse after inactivity. Locking of the knee usually means there is a sudden inability to reach full extension. The knee is often stuck at about 45° of flexion. Unlocking may occur just as suddenly, sometimes following some form of manipulation by the patient. The cause is mechanical: a loose body or torn meniscus has become wedged between the articular surfaces of the joint. Swelling that occurs suddenly after an injury is often due to a haemarthrosis from a fracture or ligamentous tear; if swelling occurs after a few hours, a torn meniscus is more likely to be the cause. Arthritis and synovitis cause a chronic swelling. Patients sometimes notice deformity, which in later life is usually due to arthritis. Sometimes the patient may complain that the knee is unstable or gives way. Patellar instability and ruptured ligaments may present this way. Always ask about loss of function. There is often a reduced ability to walk distances, climb stairs and get into and out of chairs.
TABLE 24.1
Differential diagnosis of knee pain
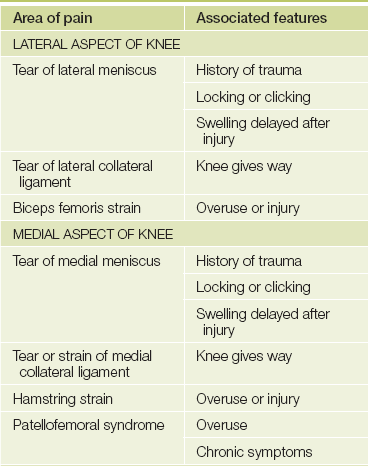
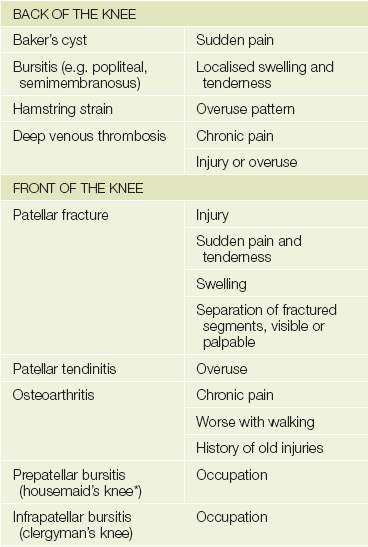
*Described by Henry Hamilton Bailey (1894-1961) as ’the most elementary diagnosis in surgery’.
Osteoarthritis of the knee is very common. Older age, previous injury and stiffness lasting less than half an hour are in favour of this diagnosis as the cause of knee pain. Physically active adolescents may present with pain and swelling below the knee at the point of attachment of the patellar tendon to the tibial tuberosity—tibial apophysitis or Osgood Schlatter’sp disease. This is the most common traction apophysitis.
Ask if there has been previous knee surgery or arthroscopy.
Take an occupational and sporting history. Injury and overuse syndromes are often related to exercise (particularly competitive sport) and occupations associated with repetitive minor injuries to the knees.
Examination
This is performed with the patient in a number of positions and, of course, walking.9,10 Even more than with the other joints, it is important to examine the more normal or uninjured knee first. This will help with the interpretation of changes in the other knee and give the patient more confidence that the examination will not be painful.
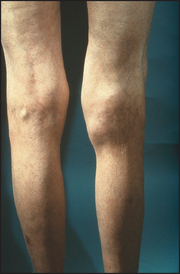
Look first with the patient lying down on the back with both knees and thighs fully exposed. The affected knee will often be flexed, the most comfortable position. Note any quadriceps wasting. This begins quite soon after knee abnormalities lead to disuse of the muscle. Examine the knees themselves for skin changes, scars (including those from previous surgery or arthroscopy), swelling and deformity. Compare each side with the other. Localised swellings may move about as the knee flexes and extends. They are often cartilaginous loose bodies. Fixed lumps in the line of the joint may be meniscal cysts.
Swelling of the synovium or a knee effusion is usually seen medial to the patella and in the joint’s suprapatellar extension. Loss of the peripatellar grooves may be an early sign of an effusion. Assess fixed flexion deformity by squatting down and looking at each knee from the side. A space under the knee will be visible if there is permanent flexion deformity arthritis.
Varus and valgus deformity may be obvious here but are more easily seen when the patient stands. Varus deformity is often related to osteoarthritis and valgus deformity to rheumatoid arthritis.
Now watch as the patient flexes and straightens each knee in turn. As the knee extends the patella glides upwards and remains centred over the femoral condyles. If there is patellar subluxation it will slip laterally during knee flexion and return to the midline during knee extension.
Feel the quadriceps for wasting. Palpate over the knees for warmth and synovial swelling.
Test carefully for a joint effusion. The patellar tap is used to confirm the presence of large effusions (see Figure 24.33). Rest one hand over the lower part of the quadriceps muscle and compress the suprapatellar extension of the joint space. With your other hand push the patella downwards. The sign is positive if the patella is felt to sink and then comes to rest with a tap as it touches the underlying femur. The bulge sign is used to detect small effusions. Use your left hand to compress the suprapatellar pouch while you run the fingers of your right hand along the groove beside the patella on one side and then the other. A bulging along the groove due to a fluid wave, on the side not being compressed, is a sign of a small effusion.
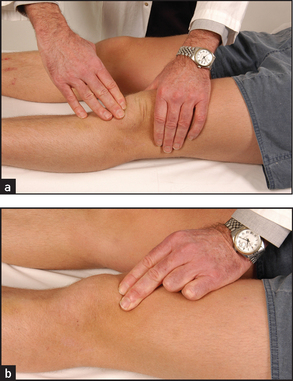
Figure 24.33 Testing for patellar effusion (a) The patellar tap; (b) the bulge sign: compressing the suprapatellar pouch. (Courtesy of Glenn McCulloch)
Examine for patellofemoral lesions by sliding the patella sideways across the underlying femoral condyles.
Move the joint passively. Test flexion (normally possible to 135°) and extension (normal to 5°) by resting one hand on the knee cap while the other moves the leg up and down (see Figure 24.34(a)). Note the range of movements and the presence of crepitus. While holding the knee flexed, feel for and attempt to localise tenderness. Feel gently for tenderness along the joint line at the patellar ligament and at the sites of attachment of the collateral ligaments.
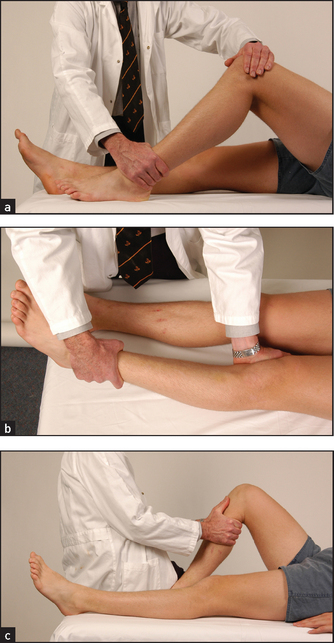
Figure 24.34 Knee examination (a) Testing knee flexion; (b) testing the collateral ligaments; (c) testing the cruciate ligaments. (Courtesy of Glenn McCulloch)
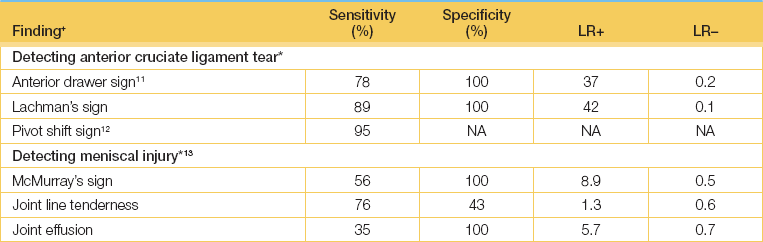
Test the ligaments next (see Good signs guide 24.1). The lateral and medial collateral ligaments are assessed by having the knee slightly flexed while holding the leg, with your forearm resting along the length of the tibia; lateral and medial movements of the leg on the knee joint are tested (see Figure 24.34(b)). Meanwhile steady the thigh with your other hand. Movements of more than 5–10° are abnormal. The cruciate ligaments (Figure 24.34(c)) are tested next. Steady the patient’s foot with your elbow or by sitting on it. Flex the patient’s knee to 90°. Grasp the tibia and attempt anterior and posterior movements of the leg on the knee joint. Movement may be detected by your thumbs positioned at the joint margins. Again, movement of more than 5–10° is abnormal. Increased anterior movement suggests anterior cruciate ligamentous laxity, and increased posterior movement suggests posterior cruciate ligamentous laxity. The Lachman test may be more accurate (LR+ 42.0, LR– 0.1).9 Here the knee is flexed 20–30° while the patient is lying supine. Grasp the femur (place your hand above the knee) to steady it, then grab the lower leg below the knee and give it a quick forward tug. It is abnormal when there is exaggerated anterior tibial movement or the knee fails to stop with a thud.
When recurrent dislocation or subluxation of the patella is suspected, the patellar apprehension test should be performed. Push the patella firmly in a lateral direction while slowly flexing the knee. The patient’s face should be studied for the anxious look that suggests impending dislocation (it is then time to suspend the test).
Ask the patient to roll into the prone position. Look and feel in the popliteal fossa for a Baker’sa cyst. This is a pressure diverticulum of the synovial membrane that occurs through a hiatus in the knee capsule (see Figure 24.35). It is best seen with the knee extended and if not obvious when the patient is lying down look again when he or she is standing and with the knee hyperextended. Rupture of this into the calf muscle produces signs that may mimic a deep venous thrombosis. Rupture is often associated with the ‘crescent sign’—ecchymoses below the malleoli of the ankle. A Baker’s cyst must be distinguished from an aneurysm of the popliteal artery, which will be pulsatile, and a bony tumour (very hard).
This is also the position in which Apley’s grinding test may be performed (see Figure 24.36). This is a test of meniscal damage. Flex the patient’s leg to 90°, stabilise the thigh by kneeling lightly on it and while pressing on the foot rotate the leg backwards and forwards. Pain or clicking makes the test positive. The distraction test is the opposite. Here the patient’s leg is pulled upwards so as to take the strain off the menisci and stretch the ligaments. If the patient finds the test painful, a ligamentous abnormality may be the cause.
McMurray’sa test (see Figure 24.37) is another way of detecting a meniscal tear. With the patient lying on the back, stand on the side to be tested and hold the patient’s ankle. Place your other hand on the medial side of the knee and push to apply valgus force. Extend the patient’s leg from the flexed position while internally and then externally rotating it. The test is positive if there is a popping sensation, which may be followed by inability to extend the knee.
Stand the patient up. Look particularly for varus (bow-leg) and valgus (knock-knee) deformity.
Finish with a test of function. Get the patient to walk to and fro. Study the gait and the movement of the knees, particularly for a sideways wobble.
Ankles and feet
Examination anatomy
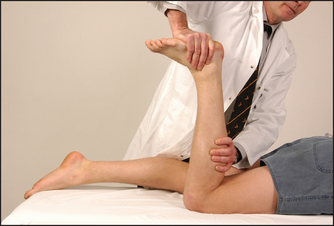
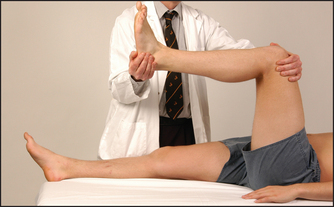
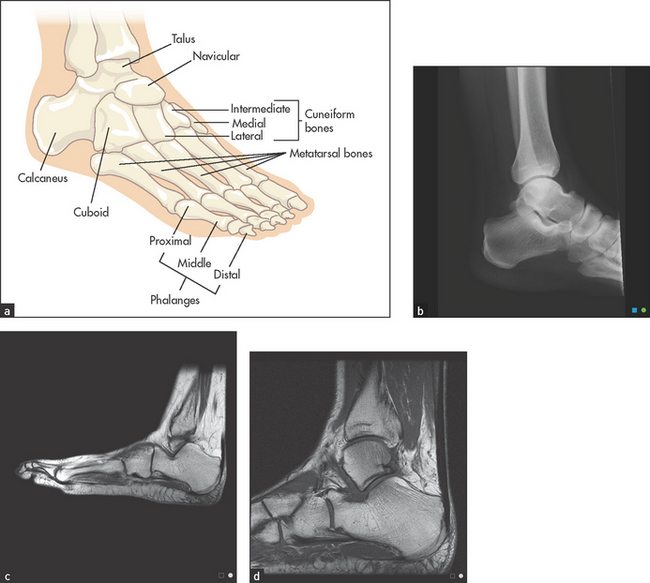
The ankle is a synovial hinge joint formed between the distal ends of the tibia and the fibula, and the talus bone (see Figure 24.38). Protrusions from the ends of the tibia and the fibula, which are called malleoli, form a socket that in combination with lateral ligaments stabilises the joint. The proximal part of the foot is called the tarsus and contains the seven tarsal bones (talus, calcaneus [heel], navicular, cuboid and the three cuneiform bones) with their supporting ligaments and joint capsules. The joints and ligaments around these bones allow the movements of the foot: inversion and eversion, dorsi- (upward) and plantar (downward) flexion.
History
The usual symptom is pain. If this is present only when the patient wears shoes, the shoes rather than the feet may be the problem. There may be a specific area that is painful and the patient should be asked to point to this. There may be a history of injury or of intensive or unusual exercise. Ankle injuries are common in certain sports that involve twisting of the foot on the leg (e.g. netball, football; see List 24.8). Rupture of the Achilles tendon occurs in squash and tennis players over 50 years of age and following forced dorsiflexion of the foot. Heel pain (both plantar and retrocalcaneal) is often due to plantar fasciitis, Achilles tendinitis or retrocalcaneal bursitis.
Patients with foot pain (see List 24.9) or ankle pain may have a history of rheumatoid arthritis. This can cause pain and deformity and affect the ankle subtalar, midtarsal and metatarsophalangeal joints.
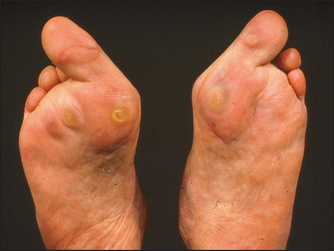
Very severe pain involving the first metatarsophalangeal joint is usually due to gout. Pain right over one of the metatarsals that comes on after unusually vigorous exercise may be due to a stress fracture.
There may be deformity involving the ankle or toes. Patients find this especially troublesome if it makes it difficult to put on shoes. The patient may have noticed swelling; ask if this is painful or not and whether it involves one or both feet. Bilateral swelling is more likely due to inflammation. Swelling over the medial aspect of the first metatarsal head (a bunion) occurs commonly as people get older, but may be associated with rheumatoid arthritis.
Paraesthesias in the feet may have been noticed. Try to find out the distribution of the abnormal sensation, which may be a result of peripheral nerve injury or peripheral neuropathy. Coldness of the feet is very common but cyanosis and ulceration are more worrying problems. Chronic foot ulcers mean diabetes must be excluded.
Examination
This examination includes the ankles, feet and toes.
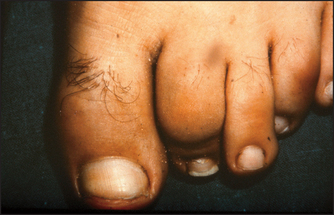
Look at the skin. Note any swelling, scars, deformity or muscle wasting. Deformities affecting the forefoot include hallux valgus (fixed lateral deviation of the main axis of the big toe), clawing (fixed flexion deformity) and crowding of the toes, as occurs in rheumatoid arthritis. Sausage deformities of the toes occur with psoriatic arthropathy or Reiter’ss disease (see Figure 24.39).
Look for the nail changes that suggest psoriasis. Inspect the transverse arch of the foot, which runs underneath the metatarsophalangeal joints, and the longitudinal arch, which runs from the first metatarsophalangeal joint to the heel. These arches, which bear the weight of the body, may be flattened in arthritic conditions of the foot like rheumatoid arthritis. Calluses over the metatarsal heads on the plantar surface of the foot occur with subluxation of these joints (see Figure 24.40).
Feel, starting with the ankle, for swelling around the lateral and medial malleoli. This should not be confused with pitting oedema. If an ankle fracture is suspected because of a history of injury, tenderness over the posterior medial malleolus is a reliable sign.14
Move the talar (ankle) joint, grasping the midfoot with one hand. Dorsiflexion is tested by raising the foot towards the knee—normally possible to 20°—and plantar flexion by performing the opposite manoeuvre, which is normally possible to 50°.
With the subtalar joint, only inversion and eversion of the foot on the ankle are tested. Pain on movement is more important than range at this joint. The midtarsal (midfoot) joint allows rotation of the forefoot when the hindfoot is fixed. This is done by steadying the ankle with one hand and rotating (twisting) the forefoot. Again, pain on motion rather than loss of range of movement is noted.
Squeeze the metatarsophalangeal joints by compressing the first and fifth metatarsals between your thumb and forefinger. Tenderness suggests inflammation, common in early rheumatoid arthritis. Press upwards from the sole of the foot just proximal to the metatarsophalangeal joints of the third and fourth toes. Pain here suggests Morton’st neuroma. This is due to entrapment and swelling of the digital nerve between the toes. It is associated with pain and numbness of the sides of these toes.
Each individual interphalangeal joint is then assessed by feeling and moving. These are typically affected in the seronegative spondyloarthropathies. Extremely tender involvement of the first metatarsophalangeal joint is characteristic of acute gout. In this case the joint also looks red and swollen.
Palpate the Achilles tendon for rheumatoid nodules (see Figure 24.41) and tenderness due to Achilles tendinitis. An old Achilles tendon rupture may be detected by squeezing the calf: normally, the foot plantar flexes unless the tendon has previously ruptured (Simmonds’a test). Also palpate the inferior aspect of the heel for tenderness; this may indicate plantar fasciitis, which occurs in the seronegative spondyloarthritis and sometimes for no apparent reason.
References
1. Fuchs, HA. Joint counts and physical measures. Rheum Dis Clin Nth Am. 1995; 21:429–444. [Describes useful quantitative methods to evaluate tenderness, pain on motion, swelling, deformity and limitation of movement.].
2. Katz, JN, Larson, ME, Sabra, A, et al. The carpal syndrome: diagnostic utility of the history and physical examination findings. Ann Intern Med. 1990; 112:321–327. [This study compares the neurophysiological assessment of the carpal tunnel syndrome with the information obtained by examination and history. No single symptom or sign is sufficiently predictive.].
3. Glockner, SM. Shoulder pain: a diagnostic dilemma. Am Fam Phys. 1995; 51:1677–1687. [1690–1692. Reviews the utility of symptoms and signs in differential diagnosis.].
4. T’Jonk, L, Staes, F, et al. The relationship between clinical shoulder tests and the findings in arthroscopic examination. Geneeskunde Sport. 2001; 34:15–24.
5. Van den Hoogen, HMM, Koes, BW, Van Eijk, JTM, Bouter, LM. On the accuracy of history, physical, and the erythrocyte sedimentation rate in diagnosing low back pain in general practice: a criteria based review of the literature. Spine. 1995; 20:318–327. [Unfortunately, distinguishing mechanical from non-mechanical causes of low back pain such as ankylosing spondylitis is clinically difficult. However, tenderness to pressure over the anterior superior iliac spines and over the lower sacrum may, based on other studies, be somewhat helpful for the positive diagnosis of ankylosing spondylitis.].
6. Deyo, RA, Rainville, J, Kent, DL. What can the history and physical examination tell us about low back pain. JAMA. 1992; 268:760–765.
7. Katz, JN, Dalgas, M, Stucki, G, et al. Degenerative lumbar spinal stenosis. Diagnostic value of the history and physical examination. Arth Rheum. 1995; 38:1236–1241. [Describes symptoms (severe lower limb pain which is absent when the patient is seated) and signs (including a wide-based gait, positive Romberg’s sign, thigh pain with lumbar extension) that help predict this rare condition in older patients.].
8. Murtagh, J. Diagnosis of early osteoarthritis of the hip joint: the four-step stress test. Aust Fam Phys. 1990; 19:389. [Discusses the diagnosis of osteoarthritis of the hip in a systematic way, suggesting a four-step approach.].
9. Solomon, DH, Simel, DL, Bates, DW, et al. Does this patient have a torn meniscus or ligament of the knee. JAMA. 2001; 286:1610–1620.
10. Scholten, RJ, Opstetten, W, vander Plas, CG, et al. Accuracy of physical diagnostic tests for assessing ruptures of the anterior cruciate ligament: a meta-analysis. J Fam Pract. 2003; 52:689–694.
11. Lee, JK, Yao, et al. Anterior cruciate ligament tears: MR imaging compared with arthroscopy and clinical tests. Radiology. 1988; 166(3):861–864.
12. Liu, SH, Osti, L, et al. The diagnosis of acute complete tears of the anterior cruciate ligament. J Bone and Joint Surg Br. 1995; 77(4):586–588.
13. Barry, OCD, Smith, H, et al. Clinical assessment of suspected meniscal tears. Ir J Med Sci. 1983; 152(4):149–151.
14. McGee, S. Evidence-based clinical diagnosis, 3rd edn. Philadelphia: Saunders, 2012.
aThe traditional treatment, striking the lesion very hard with the family Bible, is not effective.
bJean Martin Charcot (1825–1893), Parisian physician and neurologist. He became professor of nervous diseases, holding the first Chair of Neurology in the world. His pupils included Babinski, Marie and Freud.
cWilliam Heberden (1710–1801), London physician, and doctor to George III and Samuel Johnson, described these in 1802. He was the first person to describe angina.
dCharles Jacques Bouchard (1837–1915), Parisian physician.
eFritz de Quervain (1868–1940), professor of surgery in Berne, Switzerland.
fGeorge Phalen, orthopaedic surgeon, the Cleveland Clinic.
gJules Tinel (1879–1952), physician and neurologist in Paris. In 1915 he described tingling in the distribution of a nerve that had been severed and was regrowing when it was percussed.
hThey feel like the pellets emitted by a shot-gun.
iThis is wider in women so that their larger hips are accommodated.
jAlan Apley, orthopaedic surgeon, St Thomas’s Hospital, London.
kHubert von Luschka (1820–75), professor of anatomy in Tübingen.
lCharles E Lasègue (1816–83), professor of medicine in Paris and pupil of Trousseau.
mRoman goddess of love—her ancient Greek equivalent was Aphrodite.
nHugh Thomas (1834–91), ‘the father of orthopaedic surgery’, worked in Liverpool as a bone-setter but did not have a hospital appointment.
oFriedrich Trendelenburg (1844–1924), professor of surgery at Rostock, Bonn and Leipzig.
pRobert Osgood (1873–1956) worked in France during World War I and then at the Massachusetts General Hospital where he founded the X-ray department and subsequently developed several radiation-induced skin tumours. Carl Schlatter (1864–1934), professor of surgery in Zurich, pioneered a total gastrectomy operation in 1897.
aWilliam Baker (1839–96), surgeon at St Bartholomew’s Hospital, London, described this in 1877.
aThomas McMurray (1888–1949), the first professor of orthopaedic surgery in Liverpool.
sHans Reiter (1881–1969), professor of hygiene in Berlin, described the syndrome in 1916. This was well before he became an enthusiastic Nazi.
tThomas Morton (1835–1903), general and eye surgeon, Philadelphia Hospital, performed one of the first appendicectomies.
aFranklin Simmonds (1911–1983), orthopaedic surgeon, Rowley Bristow Hospital, Surrey, UK.

 denotes symptoms for the possible diagnosis of an urgent or dangerous problem.
denotes symptoms for the possible diagnosis of an urgent or dangerous problem.