Using Nursing Care Plans to Individualize and Improve Care
Introduction
According to the American Nurses Association (ANA), nursing is the diagnosis and treatment of human responses to actual and potential problems. A broad foundation of scientific knowledge, including the biological and behavioral sciences, combined with the ability to assist patients, families, and other caregivers in managing their own health needs, defines the scope of nursing practice. Nursing care in this context transcends settings, crosses the age continuum, and supports a wellness philosophy focused on self-care. In many ways, the roles of nurses are enhanced by opportunities to provide nursing care in the more natural, less institutional paradigms that are demanded by restructured health care financing. Studies continue to document that society places its highest trust in nurses. To deserve this trust, nurses will need to continuously strive to improve health care quality. The current challenges in seizing these opportunities include the following: (1) recognition of the growing chasm between what currently “exists” in health care and what “should be” to achieve the safe, quality care that every patient deserves; (2) the importance of working effectively in interdisciplinary teams to deliver patient-centered care; (3) the need for more effective professional communication; (4) the need to help patients better navigate through difficult acute and chronic care issues; (5) the ability of the nursing educational system to increasingly prepare nurses for settings outside the hospital environment, as well as within the complex hospital setting; (6) the ability of nurses themselves to be comfortable with the responsibility of their roles; (7) the need to increase the recruitment and retention of nurses from diverse backgrounds to meet the needs of an increasingly diverse population; and (8) the availability of tools to assist nurses in assessing, planning, and providing care. Nursing Care Plans: Diagnoses, Interventions, and Outcomes is such a tool.
Components of These Nursing Care Plans
Each care plan in this book begins with an expanded definition of the title problem or diagnosis (Figure 1-1). These definitions include enough information to guide the user in understanding what the problem or diagnosis is, information regarding the incidence or prevalence of the problem or diagnosis, a brief overview of the typical management and/or the focus of nursing care, and a description of the setting in which care for the particular problem or diagnosis can be expected to occur.
Each problem or diagnosis is accompanied by one or more cross-references, some of which may be synonyms (see Figure 1-1). These cross-references assist the user in locating other information that may be helpful in deciding whether this particular care plan is indeed the one the user needs.
For each care plan, appropriate nursing diagnoses are developed, which include the following components:
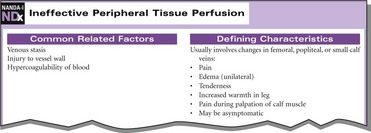
• Common related factors (those etiologies associated with a diagnosis for an actual problem) (Figure 1-2)
• Defining characteristics (assessment data that support the nursing diagnosis) (see Figure 1-2)
• Common risk factors (those situations or conditions that contribute to the patient’s potential to develop a problem or diagnosis) (Figure 1-3)
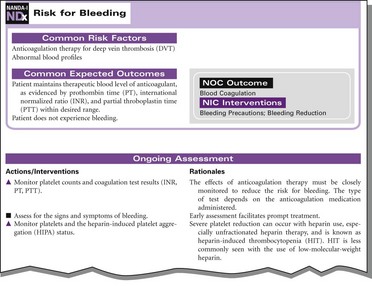
Figure 1-3 Common risk factors, common expected outcome, and ongoing assessment of the nursing diagnosis.
• Common expected outcomes (see Figure 1-3)
• Ongoing assessment (see Figure 1-3)
• Therapeutic interventions (both independent and collaborative) (Figure 1-4)
Each nursing diagnosis developed is based on the NANDA International (NANDA-I) label unless otherwise stated. Wherever possible, expanded rationales assist the user in understanding the information presented; this allows for use of Nursing Care Plans: Diagnoses, Interventions, and Outcomes as a singular reference tool. The interventions and supporting rationales for each care plan represent current research-based knowledge and evidence-based clinical practice guidelines for nursing and other health care professionals. Many care plans also refer the user to additional diagnoses that may be pertinent and would assist the user in further developing a care plan. Each diagnosis developed in these care plans also identifies the Nursing Interventions Classification (NIC) interventions and the Nursing Outcomes Classifications (NOC) outcomes.
Nursing Diagnoses Taxonomy, and Interventions and Outcomes Classifications
As Nursing Care Plans: Diagnoses, Interventions, and Outcomes continues to mature and reflect the changing times and needs of its readers, as well as the needs of those for whom care is provided, nursing diagnoses continue to evolve. The body of research to support diagnoses, their definitions, related and risk factors, and defining characteristics is ever increasing and gaining momentum. Nurses continue to study both independent and collaborative interventions for effectiveness and desirable outcomes.
The taxonomy of nursing diagnoses as a whole continues to be refined; its use as an international tool for practice, education, and research is testament to its importance as an organizing framework for the body of knowledge that is uniquely nursing. As a taxonomy, nursing diagnosis and all its components are standardized. This standardized language for nursing diagnoses, outcomes, and interventions is being incorporated into many computer programs for nursing documentation in an electronic medical record. Nurses must remember that care plans developed for each diagnosis or cluster of diagnoses for particular patients must be individualized. The tailoring of the care plan is the hallmark of nursing practice.
NIC presents an additional opportunity for clarifying and organizing what nurses do. With NIC, nursing interventions have been systematically organized to help nurses identify and select interventions. In this eighth edition, NIC information continues to be presented along with each nursing diagnosis within each care plan, giving the user added ability to use NIC taxonomy in planning for individualized patient care. According to the developers of NIC, nursing interventions are “any treatment, based upon clinical judgment and knowledge, that a nurse performs to enhance patient/client outcomes” (Bulechek et al., 2013). These interventions may include direct or indirect care and may be initiated by a nurse, a physician, or another care provider. Student nurses, practicing nurses, advanced practice nurses, and nurse executives can use nursing diagnoses and NIC as tools for learning, organizing, and delivering care; managing care within the framework of redesigned health care and within financial constraints through the development of critical paths; identifying research questions; and monitoring the outcomes of nursing care both at an individual level and at the level of service provision to large populations of patients.
Nurse investigators at the University of Iowa developed NOC, a taxonomy of patient outcomes that are sensitive to nursing interventions. The authors of this outcomes taxonomy state, “For the nursing profession to become a full participant in clinical evaluation research, policy development, and interdisciplinary work, it is essential that patient outcomes influenced by nursing care be identified and measured” (Moorhead et al., 2013). In this context, an outcome is defined as the status of the patient or family that follows and is directly influenced by nursing interventions.
The following portion of this chapter guides the user of this text through the steps of individualized care plan development. It also contains recommendations about how this book can be used to ensure safe and quality care, as a tool for quality improvement work and creating seamless nursing care delivery regardless of where in the continuum of health care the patient happens to be, for the development of patient education materials, and as the basis of critical path development.
Using Nursing Care Plans: Diagnoses, Interventions, and Outcomes
Developing an Individualized Care Plan
The nursing care plan is best thought of as a written reflection of the nursing process: What does the assessment reveal? What should be done? How, when, and where should these planned interventions be implemented? What is the desired outcome? That is, will the delivery of planned interventions result in the desired goal? The nurse’s ability to carry out this process in a systematic fashion, using all available information and resources, is the fundamental basis for nursing practice. This process includes correctly identifying existing needs, as well as recognizing potential needs and/or risks. Planning and delivering care in an individualized fashion to address these actual or potential needs, as well as evaluating the effectiveness of that care, is the basis for excellence in nursing practice. Forming a partnership with the patient and/or caregiver in this process and humanizing the experience of being a care recipient is the essence of nursing.
The Assessment
All the information that the nurse collects regarding a particular patient makes up the assessment. This assessment allows a nursing diagnosis, or clinical judgment, to be made. This, in turn, drives the identification of expected outcomes (i.e., what is desired by and for this particular patient in relation to this identified need) and the care plan. Without a comprehensive assessment, all else is a “shot in the dark.”
Nurses have always carried out the task of assessment. As science and technology progress, information is more abundant than at any other time in history; however, length of contact with each patient becomes shorter, so astute assessment skills are essential to a nurse’s ability to plan and deliver effective nursing care.
Assessment data are abundant in any clinical setting. What the nurse observes; what a history (written or verbal) reveals; what the patient and/or caregiver reports (or fails to report) about a situation, problem, or concern; and what laboratory and other diagnostic information is available are all valid and important data.
Methods useful in gathering these diverse data include interview, direct and indirect observation, physical assessment, medical records review, and analysis and synthesis of available laboratory and other diagnostic studies. The sum of all information obtained through any or all of these means allows the nurse to make a nursing diagnosis.
Gordon’s (1976) definition of a nursing diagnosis includes only those problems that nurses are capable of treating, whereas others have expanded the definition to include any health-related issue with which a nurse may interface. In Nursing Care Plans: Diagnoses, Interventions, and Outcomes the nursing diagnosis terminology conforms to the NANDA-I Nursing Diagnoses: Definitions & Classification, 2012-2014 unless otherwise stated.
Performing the Assessment
A nurse has knowledge in the physical and behavioral sciences, is a trusted member of the health care team, and is the interdisciplinary team member who has the most contact with a patient. Because of these qualities, a nurse is in a key position to collect data from the patient and/or caregiver at any point at which the patient enters the health care continuum, whether in the home, in a hospital, in an outpatient clinic, or in a long-term care facility.
Interviewing is an important method of gathering information about a patient. The interview has the added dimensions of providing the nurse with the patient’s subjective input on not only the problem but also what the patient may feel about the causes of the problem, how the problem has affected the patient as an individual, what outcomes the patient wants in relation to the particular problem, as well as insight into how the patient and/or caregiver may or may not be capable of participating in management of the problem.
Good interviewing skills are founded on rapport with the patient, the skill of active listening, and preparation in a systematic, thorough format, with comprehensive attention given to specific health-related problems. The nurse as the interviewer must be knowledgeable of the patient’s overall condition and the environment in which the interview will take place. A comprehensive interview that includes exploration of all the functional health patterns is ideal and will provide the best overall picture of the patient. When time is a limiting factor, the nurse may review existing medical records or other documents before the interview so that the interview can be focused. Care must be taken, however, not to “miss the forest for the trees” by conducting an interview in a fashion that precludes the discovery of important information the patient may have to share.
During an interview the patient may report the following types of information:
• Bothersome or unusual signs and symptoms (e.g., “I have been having cramps and bloody diarrhea for the past month.”)
• Changes noticed (e.g., “It’s a lot worse when I drink milk.”)
• The impact of these problems on his or her ability to carry out desired or necessary activities (e.g., “I know every washroom at the mall. It’s tough having lunch with friends.”)
• Issues associated with the primary problem (e.g., “It’s so embarrassing when my stomach starts to rumble loudly.”)
• The impact of these problems on significant others (e.g., “My daughter cannot understand why a trip to the zoo feels like a challenge.”)
• What specifically caused the patient to seek attention (e.g., “The amount of blood in the past couple of days really has me worried, and the pain is getting worse.”)
In addition, the patient may share the following:
• Previous experiences or history (e.g., “My brother has had Crohn’s disease for several years; this is how he started out.”)
• Health beliefs and feelings about the problem (e.g., “I have always figured it would catch up with me sooner or later, with all the problems like this in our family.”)
• Thoughts about what would help solve the problem (e.g., “Maybe I should watch my diet better.”)
• What has been successful in the past in solving similar problems (e.g., “They kept my brother out of surgery for years with just a diet and medicine.”)
From this scenario, it is clear that the interviewing nurse would want to explore issues of elimination, pain, nutrition, knowledge, and coping.
Information necessary to begin forming diagnoses has been provided, along with enough additional information to guide further exploration. In this example, the nurse may choose diarrhea as the diagnosis. Using NANDA-I–approved related factors for diarrhea, the nurse will want to explore stress and anxiety, dietary specifics, medications the patient is taking, and the patient’s personal and family history of bowel disease.
The defining characteristics for diarrhea (typical signs and symptoms) have been provided by the patient to be cramping; abdominal pain; increased frequency of bowel movements and sounds; loose, liquid stools; urgency; and changes in the appearance of the stool. These defining characteristics support the nursing diagnosis diarrhea.
To explore related concerns such as pain, nutrition, knowledge, and coping, the nurse should refer to defining characteristics for imbalanced nutrition: less than body requirements; deficient knowledge; acute pain; and ineffective coping. The nurse should then interview the patient further to determine the presence or absence of defining characteristics for these additional diagnoses.
To continue this example, the nurse might ask the patient the following questions: Have you lost weight? Of what does your typical breakfast/lunch/dinner consist? How is your appetite? Describe your abdominal cramping. How frequent is the discomfort? Does it awaken you at night? Does it interfere with your daily routine? On a scale of 1 to 10, with 10 being the worst pain you have ever had, how bad is the cramping? Can you tell me about your brother’s Crohn’s disease? Have you ever been told by a doctor that you have Crohn’s or a similar disease? How are you handling these problems? Have you been able to carry out your usual activities? What do you do to feel better? In asking these questions, the nurse can decide whether the four additional diagnoses (imbalanced nutrition: less than body requirements; deficient knowledge; acute pain; and ineffective coping) are supported as actual problems or are problems for which the patient may be at risk.
Family, caregivers, and significant others also can be interviewed. When the patient’s condition makes him or her incapable of being interviewed, these may be the nurse’s only sources of interview information.
Physical assessment provides the nurse with objective data regarding the patient and includes a general survey followed by a systematic assessment of the physical and mental conditions of the patient. Findings of the physical examination may support subjective data already given by the patient or may provide new information that requires additional interviewing. In reality, the interview continues as the physical assessment proceeds and as the patient focuses on particulars. The patient is then able to enhance earlier information, remember new information, become more comfortable with the nurse, and share additional information.
Patient comfort and cooperation are important considerations in performing the physical examination, as are privacy and an undisturbed environment. Explaining the need for assessment and what steps are involved is helpful in putting the patient at ease and gaining cooperation.
Methods used in physical assessment include inspection (performing systematic visual examination), auscultation (using a stethoscope to listen to the heart, lungs, major vessels, and abdomen), percussion (tapping body areas to elicit information about underlying tissues), and palpation (using light or heavy touch to feel for temperature, normal and abnormal structures, and any elicited subjective responses). The usual order of these assessment techniques is inspection, palpation, percussion, and auscultation, except during the abdominal portion of the physical examination. Percussion and palpation may alter a finding by moving gas and bowel fluid and changing bowel sounds. Therefore percussion and palpation should follow inspection and auscultation when the abdomen is being examined.
To continue the example, the nurse may note, through inspection, that the patient is a thin, pale, well-groomed young woman who is shifting her weight often and has a strained facial expression. When asked how she feels at the present, the patient gives additional support to the diagnoses ineffective coping and deficient knowledge (“I don’t understand what is wrong with me; I feel tired and stressed out all the time lately”). Physical examination reveals a 10-pound weight loss, hyperactive bowel sounds, and abdominal pain, which is expressed when the nurse palpates the right and left lower quadrants of the patient’s abdomen. These findings further support the nursing diagnoses diarrhea, imbalanced nutrition: less than body requirements; and acute pain.
Using General Versus Specific Care Plan Guides
At this point, the nurse has identified five nursing diagnoses: diarrhea, imbalanced nutrition: less than body requirements, acute pain, deficient knowledge, and ineffective coping. Nursing Care Plans: Diagnoses, Interventions, and Outcomes is organized to allow the nurse to build a care plan by using the primary nursing diagnoses care plans in Chapter 2. A nurse can also select, by medical diagnosis, a set of nursing diagnoses that have been clustered to address a specific medical diagnosis and then further individualize it for a particular patient.
Using the first method from Chapter 2, the nurse had every possible related factor and defining characteristic from which to choose to tailor the care plan to the individual patient. It is important to individualize these comprehensive care plans by highlighting those related factors, defining characteristics, assessment suggestions, and interventions that actually pertain to specific patients. Nurses should add any that may not be listed, customize frequencies for assessments and interventions, and specify realistic time frames for outcome achievement. (The blanket application of these standard care plans negates the basic premise of tailoring care to meet individual needs.) To complete the example used to demonstrate individualizing a care plan using this text, the nurse should select the nursing interventions based on the assessment findings, proceed with care delivery, and evaluate whether selected patient outcomes have been achieved.
Specific
Using the clustered diagnoses usually labeled by a medical diagnosis found in Chapters 5 to 15 (e.g., inflammatory bowel disease), the nurse has the added benefit of a brief definition of the medical diagnosis; an overview of typical management, including the setting (home, hospital, outpatient); synonyms that are useful in locating additional information through cross-referencing; and associated nursing diagnoses with related factors and defining characteristics. Again, it is important that aspects of these care plans be selected and applied (i.e., individualized) based on specific assessment data for a particular patient.
As a tool that guides nursing care delivery, the care plan must be updated and revised periodically to remain useful in care provision. Revisions are based on goal attainment, changes in the patient’s condition, and response to interventions. In today’s fast-paced, outpatient-oriented health care system, revision will be required often.
As the patient moves through the continuum of care, a well-developed care plan can enhance the continuity of care and contribute to seamless delivery of nursing care, regardless of the setting in which the care is provided. This will serve to replace replication with continuity and ultimately increase the patient’s satisfaction with care delivery.
A Focus on Optimizing Health
Chapter 3 provides an additional type of care plan with its focus on Health Promotion and Risk Factor Management. Typical nursing care plans throughout this book focus on sick care and helping patients manage their medical illnesses. This chapter is unique in that it showcases patients who are actively engaged in health-seeking behaviors. To reflect this positive approach, the nursing diagnoses reflect a more positive, active title—beginning with Readiness for. The nurse realizes that making changes to one’s lifestyle is very complex. Thus the nurse needs to use multifaceted evidence-based strategies known to reflect successful behavior changes. It is these strategies that serve as the assessment and therapeutic intervention foci for these health promotion care plans. These strategies include a combination of methods to enhance awareness of risk factors, increase motivation for change, set realistic goals, focus on tailoring the regimen, incorporate self-monitoring, enhance self-efficacy, provide skills in problem solving, include social support and rewards, and address relapse prevention. These care plans demonstrate the important partnership nurses have with patients in assisting them to develop the knowledge and skills needed for making healthy lifestyle decisions and enacting health behaviors.
Other Common Themes
Many patient conditions warrant attention to specialized yet commonly used interventions such as central venous access devices, blood component therapy, and total parenteral and enteral nutrition. These care plans now have a dedicated space in Chapter 4, where they can be easily accessed and incorporated into specialty care plans for a wide variety of medical problems. Another common theme that does not reflect on only one chapter is death and dying (end-of-life issues), common mood disorders, and substance abuse. The nurse who encounters these problems can simply refer to the care plans in this chapter to guide interventions.
Ensuring Quality and Safety
Ever since the 1999 Institute of Medicine published its landmark report, To Err Is Human: Building a Safer Health System, there has been a major focus on transforming the health care environment. With nurses as the largest provider of health care in this country, quality and safety must be “their job.”
Nurses are well positioned to positively influence patient outcomes. These efforts are in concert with those of physicians and hospital administrators in pursuit of high-quality, safe care. Accreditation and regulatory bodies, professional nursing and medical societies, and quality improvement organizations alike are partnering to provide a culture of safety for patients and families. For example, in 2002 The Joint Commission (TJC) established its National Patient Safety Goals (NPSGs) program to help accredited organizations address specific areas of concern in regard to patient safety. Some of the general performance measures identified as a means of reducing errors included “do not use” abbreviations, hand-off communication, standardized drug concentrations, infusion-pump free-flow protection, Centers for Disease Control and Prevention (CDC) hand hygiene guidelines, surgical site marking, “time-out” before surgery, and medication reconciliation. Although an extremely important part of medical and nursing practices, these procedures would not be described in a typical nursing care plan. Similarly, general guidelines for implementing evidence-based practices to prevent health care–associated infections caused by multiple-drug–resistant organisms, to prevent central line–associated bloodstream infections, and to prevent surgical site infections, although critical to patient safety, are also not routinely found in a typical care plan.
In contrast, the Patient Safety Indicators recommended by the Agency for Healthcare Research and Quality (AHRQ) provide information about potentially preventable complications and adverse events for a variety of diagnoses or procedures, and these are incorporated into relevant care plans in Nursing Care Plans: Diagnoses, Interventions, and Outcomes. Some examples include attention to fall assessment and prevention, pressure ulcer assessment and prevention, pain management, prevention of pulmonary embolism or deep vein thrombosis, prevention of postoperative sepsis, prevention of hospital-acquired pneumonia, and avoidance of selected infections as a result of medical care. Moreover, TJC provides National Quality Improvement Goals and Guidelines that when followed by health care providers have resulted in faster patient recoveries with fewer complications. Some of these include pneumonia care, acute myocardial infarction care, heart failure care, blood clot prevention, and surgical infection prevention care. These measures are highlighted in the respective care plans.
Finally, when evidence-based practice and clinical practice guidelines are used to guide health care decisions and deliver care, the best patient outcomes are achieved. Such guidelines, when available, are well integrated into the plans of care in Nursing Care Plans: Diagnoses, Interventions, and Outcomes. Nurses are reminded that a key element in evidence-based clinical decision making is the responsibility to personalize the evidence to apply to a specific patient’s values and circumstances. Even the best research evidence cannot be followed blindly.
Tools for Performance Improvement
This book can also be used to identify outcome criteria in quality improvement projects and in the development of monitoring tools. For example, a nursing department, home health agency, or interdisciplinary pain management team may be interested in monitoring and improving its pain management outcomes. Using the Chapter 2 care plan for acute pain, the process of pain management can be monitored simply by using each assessment and intervention as a measurable indicator. The outcome of pain management assessment and intervention can also be studied through direct observation, records review, and patient satisfaction measures. There has been increasing focus on the interrelatedness of services and systems. The care plans in this text include independent and collaborative assessment suggestions and interventions, which facilitate use of the care plans as tools for quality improvement activities. Nurses, other health care professionals, clinical managers, and risk management and quality improvement staff will find that the care plans in this text provide specific, measurable detail and language. This aids in the development of monitoring tools for a broad scope of clinical issues.
Finally, when benchmarks are surpassed and there is desire to improve an aspect of care, the plans of care in Nursing Care Plans: Diagnoses, Interventions and Outcomes contain state-of-the-art information that will be helpful in planning corrections or improvements. These outcomes can be measured after implementation. The similarities between the nursing process (assess, plan, intervene, and evaluate) and accepted methods for quality improvement (measure, plan improvements, implement, and remeasure) make these care plan guides natural tools for use in performance improvement activities.
Development of Patient Education Materials
Education of patients and their families and/or significant others has always been a priority role for nurses. Nursing Care Plans: Diagnoses, Interventions, and Outcomes is an excellent source book for key procedural and self-care information to share with patients for more than 200 medical problems. It also provides guidance for teaching both the population of ill patients and healthier clients seeking health promotion and disease prevention strategies. Educational content is provided using two formats. For the Chapter 2 general nursing diagnoses, a separate section on Education/Continuity of Care is found near the end of each plan of care. This chapter also provides a more general overview of key educational assessments and interventions pertaining to all learners, as found in the deficient knowledge care plans. The subsequent chapters using the clustered medical diagnoses have the patient education material integrated throughout the care plan, rather than in a separate section at the end. These interventions, along with associated rationales, follow the Ask Me 3 directive on health literacy, which recommends that patient education sessions provide answers to the following questions: What is my main problem? What do I need to do? Why is it important for me to do this? For some medical problems that require a larger focus on education and self-management, a separate nursing diagnosis of deficient knowledge may be found within the care plan.
A Basis for Clinical Paths
Clinical paths (also called critical paths, critical pathways, or care maps) are interdisciplinary care plans to which time frames have been added. The clinical path is designed to track the care of a patient based on average and expected lengths of stay in an acute care setting. Clinical paths can also be developed for the home care and long-term care settings. The path provides guidelines about the sequence of care provided by the various members of the health care team responsible for the care of the patient. Interventions in a specific clinical path may include patient education, diet therapy progression, medications, consultations and referrals to other members of the health care team, activity progression, and discharge planning. The nurse is usually responsible for implementing and monitoring the patient’s progress and noting deviations from the suggested time frame.
Clinical paths are useful in organizing care delivered to a specific population of patients for whom a measurable sequence of outcomes is readily identifiable. For example, most patients having total hip replacement sit on the edge of the bed by the end of the operative day and are up in a chair by noon on the first postoperative day. They also resume a regular diet intake and stand by the end of the first postoperative day. They progress to oral analgesics by the third postoperative day and are ready for discharge on the fifth postoperative day. Every patient with total hip replacement may not progress according to this path because of individual factors such as other medical diagnoses, development of complications, or simple individual variation. However, most will, and therefore a clinical path can be a powerful tool not only in guiding care but also in monitoring use of precious resources and making comparative judgments about outcomes of one physician group, hospital unit, or facility against external benchmarks. This may facilitate consumer decision making and enable those who finance health care to base judgments about referrals on outcome measures of specific physicians, hospitals, surgical centers, and other places.
The care plan forms the basis of a clinical path. Nursing Care Plans: Diagnoses, Interventions, and Outcomes can be used as the clinical basis from which to begin the development of the clinical path. Because nursing care plans in this text are organized by nursing diagnoses, adaptation of these care plans into clinical paths may require organizing the information differently.
References
Bulechek G, Butcher H, Dochterman J, Wagner C, eds. Nursing Interventions Classification (NIC), ed 6, St. Louis: Mosby, 2013.
Gordon, M. Nursing diagnosis and the diagnostic process. American Journal of Nursing. 1976;76:1298.
Moorhead S, Johnson M, Maas M, Swanson E, eds. Nursing Outcomes Classification (NOC), ed 5, St. Louis: Mosby, 2013.