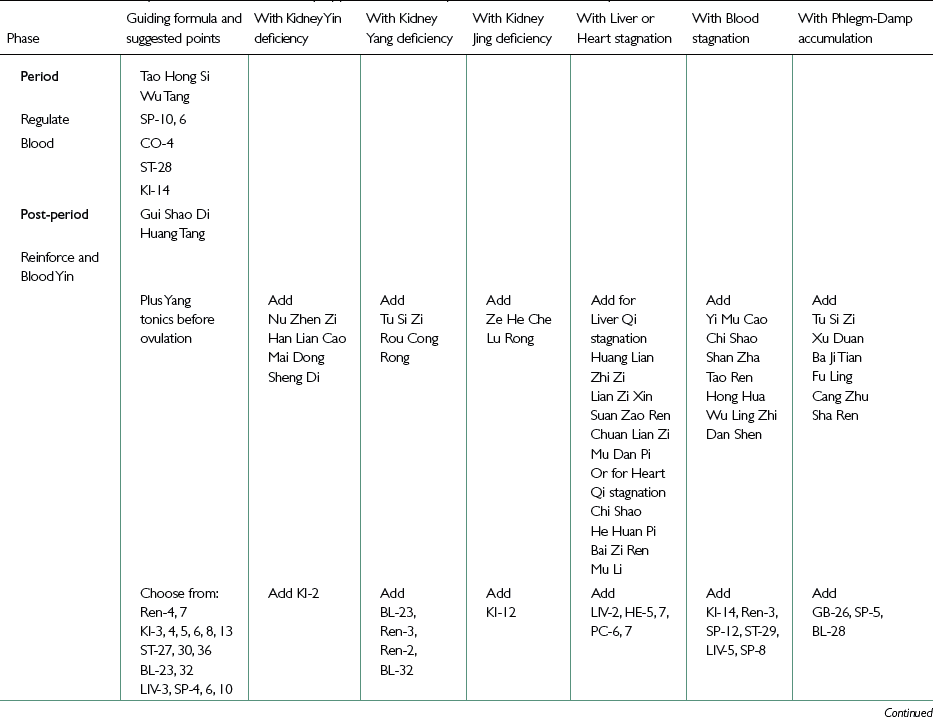
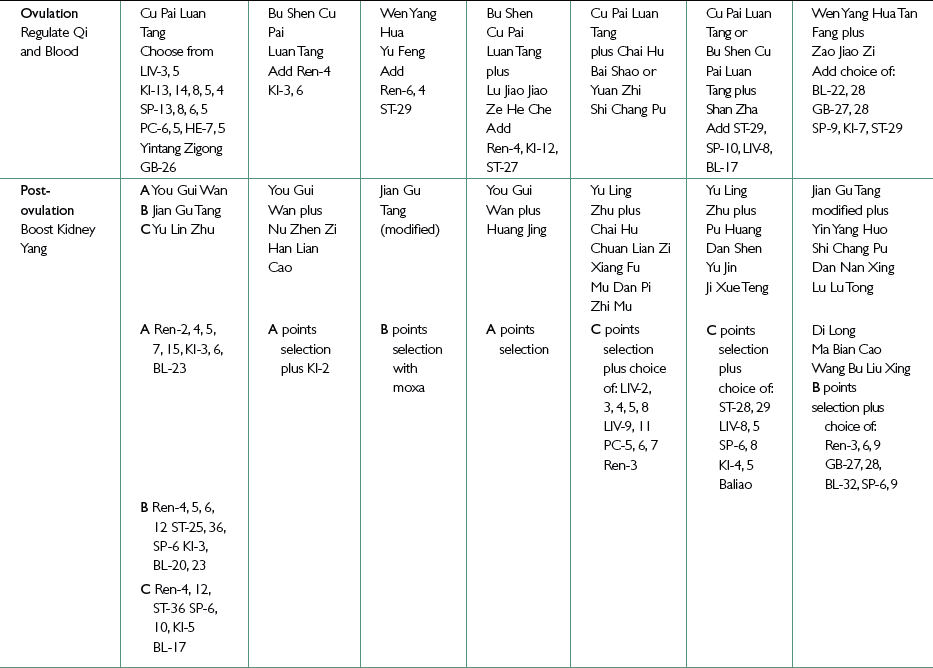
Modifications and Variations
Kidney Yin Deficiency
Herbal Formula: If the woman is not so young (>35 years) or there is Kidney Yin deficiency, some extra herbs need to be added to the basic ovulation formula, Cu Pai Luan Tang. This then becomes Bu Shen Cu Pai Luan Tang and is useful if the Yin levels have not been quite brought up to ideal levels before ovulation or if there is weak Qi and Blood movement.
Bu Shen Cu Pai Luan Tang (Reinforce Kidney Ovulation Formula)
| Dang Gui | 9 g | Radix Angelicae Sinensis |
| Chi Shao | 9 g | Radix Paeoniae Rubra |
| Bai Shao | 9 g | Radix Paeoniae Lactiflorae |
| Shan Yao | 9 g | Dioscorea Oppositae |
| Shu Di | 12 g | Radix Rehmanniae Glutinosae Conquitae |
| Nu Zhen Zi | 9 g | Fructus Ligustri Lucidi |
| Mu Dan Pi | 9 g | Cortex Moutan Radicis |
| Fu Ling | 12 g | Sclerotium Poriae Cocos |
| Bu Gu Zhi | 9 g | Fructus Psoraleae |
| Tu Si Zi | 9 g | Semen Cuscatae |
| Wu Ling Zhi | 9 g | Excrementum Trogopterori |
| Hong Hua | 6 g | Flos Carthami Tinctorii |
In comparison to Cu Pai Luan Tang, the first priority of this formula is supporting the Kidneys (Shu Di, Nu Zhen Zi, Bu Gu Zhi, Tu Si Zi), Spleen (Shan Yao) and Liver (Bai Shao). Moving the Blood (Wu Ling Zhi, Hong Hua, Dang Gui, Chi Shao, Mu Dan Pi) is secondary. Kidney Yin tonics support ovary function, Kidney Yang tonics promote maturation of the egg and reinforce its energy making capacity and Blood moving herbs promote development of the endometrium and ensure no obstruction to ovulation.
This formula is used for 3–5 days and, if successful, ovulation will occur and the basal body temperature pushed to its high level quickly and efficiently.
Kidney Yang Deficiency
Herbal Formula: In cases where there are generalized Kidney Yang deficient or Cold signs and symptoms we use warming and moving herbs to encourage effective ovulation. A formula like Wen Yang Hua Yu Fang can be used as the guiding formula here.
Wen Yang Hua Yu Fang (Warm Yang and transform stasis formula)
| Gui Zhi | 9 g | Ramulus Cinnamomi Cassiae |
| Hong Hua | 6 g | Flos Carthami Tinctorii |
| Dang Gui | 9 g | Radix Angelicae Sinensis |
| Chuan Xiong | 6 g | Radix Ligustici Wallichii |
| (Huai) Niu Xi | 9 g | Radix Achyranthis Bidentatae |
| Ji Xue Teng | 15 g | Radix et Caulis Jixueteng |
| Yin Yang Huo | 9 g | Herba Epimedii |
| Shu Di | 9 g | Radix Rehmanniae Glutinosae Conquitae |
| Zhi Fu Zi∗ | 6 g | Radix Aconiti Charmichaeli Praeparata |
This formula introduces quite a lot of Heat with herbs such as Zhi Fu Zi and Gui Zhi, and movement of Blood with herbs such as Hong Hua, Chuan Xiong, Ji Xue Teng and Dang Gui. Huai Niu Xi, Shu Di and Yin Yang Huo support the Kidney Yin and Yang.
These herbs are taken for around 3 days at midcycle or from the day of supposed ovulation. If they are used too early they will dry the fertile mucus and the protective mucus lining of the tubes. Because they are very heating it is important to ensure there is no Liver- or Heart-Fire or Yin-deficient Heat present.
Where there is ovulation pain, which is relieved by warmth, add:
| Xiao Hui Xiang | 6 g | Fructus Foeniculi Vulgaris |
Acupuncture Points: Add to points chosen from Table 4.5:
| Ren-6 | Qihai |
| Ren-4 | Guanyuan |
| ST-29 | Guilai |
| BL-32 | Ciliao |
Kidney Jing Deficiency
Herbal Formula: A lack of Kidney Jing really needs to be addressed from the beginning of the cycle and there is little more that can be done now we are at midcycle if the Jing Qi is not sufficient, i.e., there will be no eggs ripe and ready for ovulation. However, if the Jing tonic herbs applied early in the cycle seem to be having results, i.e., more fertile mucus is appearing (or blood tests show that estrogen levels are rising adequately), then the guiding formula Bu Shen Cu Pai Luan Tang can be given around midcycle, with the addition of:
| Lu Jiao Pian | 9 g | Cornu Cervi Parvum |
| Zi He Che∗∗ | 3 g | Placenta Hominis |
Acupuncture Points: Add to the choice of points in Table 4.5:
| Ren-4 | Guanyuan |
| KI-12 | Dahe |
| ST-27 | Daju |
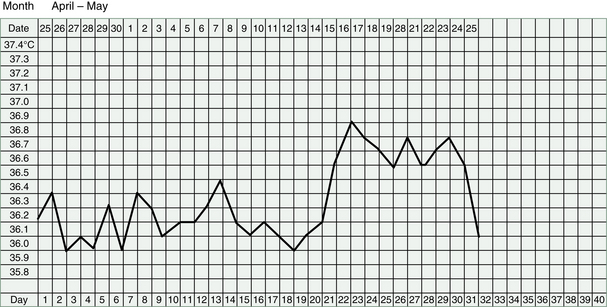
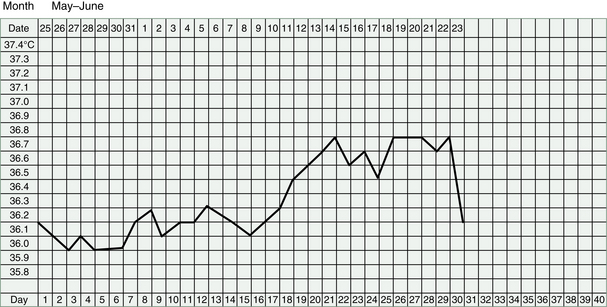
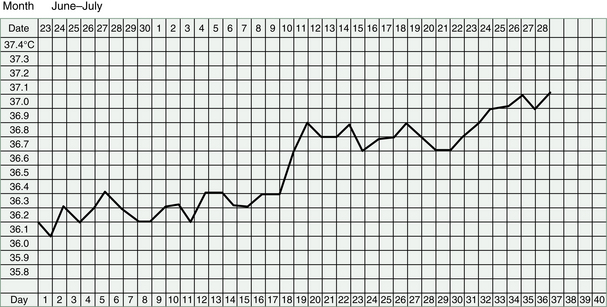
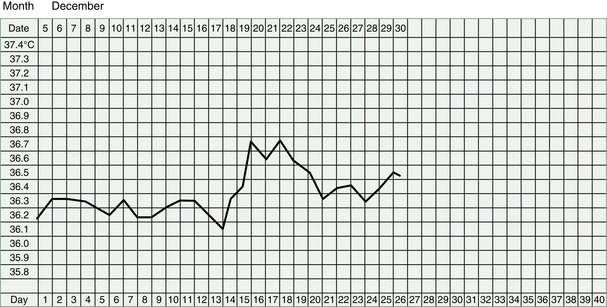
Any rise in the BBT after this treatment must be seen as very encouraging progress, because it indicates that an ovulation has occurred. However, the temperature may drop again quite soon or it may not reach a very high level and it may take many months of treatment before a good ovulation can be produced.
In fertility clinics in China, women are usually advised to establish reliable cycles and good ovulations (i.e., convincing BBT charts) before attempting pregnancy. However, in the case of women with Jing deficiency and a very erratic menstrual history, they will quite understandably want to take advantage of any ovulation at all since they are so few and far between. The risk, of course, is miscarriage, so I do try to persuade these women to wait a few months after commencing treatment before trying to conceive.
Heart and Liver Qi Stagnation
Herbal Formula: It is critical that Liver and Heart Qi remain unobstructed for ovulation to occur, so we must always pay great attention to these at this time of the cycle. Ovulation pain and breast or nipple tenderness alert us to stagnation of Liver Qi at this time. The liver (physiological organ) can be assisted by the following treatments to break down hormones without compromising estrogen production by the ovaries. This will usually be enough to stop symptoms of breast soreness.
In most cases, adding a few herbs to the base formula Cu Pai Luan Tang is enough to facilitate movement of Liver Qi and Heart Blood. For example:
| Chai Hu | 9 g | Radix Bupleuri |
| Bai Shao | 9 g | Radix Paeoniae Lactiflorae |
| Dan Shen | 9 g | Radix Salviae Miltiorrhizae |
| Suan Zao Ren | 15 g | Semen Ziziphi Spinosae |
However, if there is marked Heart or Liver Qi stagnation causing emotional disturbance, a stronger approach is necessary. A useful guiding formula is the following:
Yuan Zhi Chang Pu Yin (Polygala Acorus pill)
| Yuan Zhi | 6 g | Radix Polygalae Tenuifoliae |
| Shi Chang Pu | 9 g | Rhizoma Acori Graminei |
| Dang Gui | 9 g | Radix Angelicae Sinensis |
| Chi Shao | 9 g | Radix Paeoniae Rubra |
| Bai Shao | 9 g | Radix Paeoniae Lactiflorae |
| Shan Zha | 9 g | Fructus Crataegi |
| Fu Ling | 9 g | Sclerotium Poriae Cocos |
| Chai Hu | 6 g | Radix Bupleuri |
| Yu Jin | 9 g | Tuber Curcumae |
| Dan Shen | 9 g | Radix Salviae Miltiorrhizae |
| He Huan Pi | 12 g | Cortex Albizziae Julibrissin |
Yuan Zhi and Shi Chang Pu are combined here to quieten the mind during the ovulation phase. Yu Jin, Dan Shen, Chai Hu and He Huan Pi will support this action by removing Heart or Liver Qi stagnation. Liver and Heart Blood are reinforced with Dang Gui and Bai Shao. Chi Shao ensures that Liver-Heat is cleared and Fu Ling supports the Spleen function in the face of Liver Qi stagnation.
If such emotional instability is occurring in a woman with Kidney weakness (or she is over 35 years old) we should continue Kidney tonic herbs as well. The herbs listed above already include four of the herbs from our Kidney Yin deficiency ovulation formula (Bu Shen Cu Pai Luan Tang) and we could add several more. For example:
| Shu Di | 9 g | Radix Rehmanniae Glutinosae Conquitae |
| Shan Yao | 9 g | Dioscorea Oppositae |
| Xu Duan | 9 g | Radix Dipsaci |
| Tu Si Zi | 9 g | Semen Cuscatae |
If the high levels of hormones, which can occur at ovulation (especially where there is Liver Qi stagnation) cause a sensation of fullness or aching in the vulva, then adding herbs to strengthen Spleen Qi is appropriate. Add to the appropriate base formula (Yuan Zhi Chang Pu Yin modified or Cu Pai Luan Tang modified):
| Huang Qi | 12 g | Radix Astragali |
Acupuncture Points: Acupuncture is undoubtedly useful at ovulation time and it is worth the patient making an effort to book visits to the acupuncturist’s clinic to coincide with this particular time.
Choose points from Table 4.5 which emphasize the movement of Qi in the fallopian tubes and ensure there is no tension or constriction in these fine muscles, i.e., choose local abdomen points and Liver channel points. Additionally, choose points which calm the mind and clear the Bao vessel, i.e., Heart and Pericardium channel points and Yintang and KI-4.
Blood Stagnation
Herbal Formula: The sorts of formulas we use at midcycle already contain Blood-moving herbs. In some cases we might want to add stronger herbs or increase the doses of ones already chosen.
Blood stagnation of the type that will seriously disrupt ovulation might include cysts or endometriomas on the ovary – these are likely to cause pain and therefore demand attention at midcycle. Some forms of tube blockage are caused by Blood stagnation – these are covered in Chapter 6. In the case of substantial obstructions, we usually use Blood-breaking herbs like E Zhu or San Leng although in cycles where conception is attempted these herbs may be too harsh. However in robust young women with significant masses that are obstructing the ovaries or the tubes these herbs may be added for just a couple of days and in small doses.
In the case of cysts or masses in a strong and young woman, Cu Pai Luan Tang can be modified by adding:
| Shan Zha (Sheng) | 9 g | Fructus Crataegi |
| E. Zhu | 6 g | Rhizoma Curcumae Zedoariae |
and increasing the dose of Wu Ling Zhi to 12 g, and Hong Hua to 9 g.
In the case of endometriomas (and if there is a component of Kidney deficiency) you can modify Bu Shen Cu Pai Luan Tang in exactly the same way.
Acupuncture Points: Consider including among the points chosen from Table 4.5:
| ST-28 | Shuidao |
| KI-14 | Siman |
| KI-5 | Shuiquan |
| SP-8 | Diji |
| ST-29 | Guilai |
| SP-10 | Xuehai |
| LIV-8 | Ququan |
| BL-17 | Geshu |
Use with reducing method.
Phlegm-Damp Accumulation
Herbal Formula: In most women and in most cycles, herbs which strongly move Qi and Blood to facilitate ovulation are applied only when we get to the point where the Yin is well established and the egg is ready to be launched, i.e., around Day 13 or 14 in a 28-day cycle. However, when Phlegm-Damp is seriously gluing up the works, we need to apply such treatment well before ovulation, otherwise the egg may never be released or, if it is, it will not get very far before being obstructed by excess or pathological mucus secretions in the fallopian tubes.
In women diagnosed with Phlegm-Damp we added to our base formula Yang tonics and Damp-clearing herbs in the early part of the cycle. Once we have some evidence that we have established a good enough basis of Yin (there is fertile mucus or blood tests show rising estrogen levels) we use a more strongly activating formula, even if it is only I week past the period. For example, the formula Wen Yang Hua Tan Fang will transform Damp and Phlegm, warm Yang and activate Qi and Blood.
Wen Yang Hua Tan Fang (Warm Yang and Transform Phlegm Formula)
| Zhi Fu Zi∗ | 6 g | Radix Aconiti Charmichaeli Praeparata |
| Xu Duan | 9 g | Radix Dipsaci |
| Yin Yang Huo | 9 g | Herba Epimedii |
| Cang Zhu | 9 g | Rhizoma Atractylodes |
| Chen Pi | 5 g | Pericarpium Citri Reticulate |
| Fu Ling | 9 g | Sclerotium Poriae Cocos |
| Zhi Ke | 9 g | Fructus Citri seu Ponciri |
| Shan Zha | 9 g | Fructus Crataegi |
| Hong Hua | 6 g | Flos Carthami Tinctorii |
| Dan Nan Xing | 9 g | Rhizoma Arisaematis |
This formula combines a strong heating element (Zhi Fu Zi) with Yang tonics (Xu Duan and Yin Yang Huo) and herbs which encourage elimination of Damp (Cang Zhu, Fu Ling, Chen Pi, Zhi Ke and Dan Nan Xing). Because it is an ovulation formula, Blood-regulating agents (Shan Zha and Hong Hua) are added. Dan Nan Xing is added here for its ability to dissipate lumps (in this case, obstructions in the tubes).
If the release of the egg from the ovary appears to be obstructed by Phlegm-Damp add:
| Zao Jiao Zi | 6 g | Fructus Gleditsiae Sinensis |
Acupuncture Points: From the points chosen from Table 4.5, emphasize the Spleen channel and Dai vessel points and add:
| BL-22 | Sanjiaoshu |
| BL-28 | Pangguanshu |
| GB-27 | Wushu |
| GB-28 | Weidao |
| SP-9 | Yinlingquan |
| KI-7 | Fuliu |
| ST-29 | Guilai (with moxa) |
Use with even or reducing method.
Midcycle Bleeding
The dramatic peaks and falls of hormone levels (especially estrogen) at midcycle can sometimes provoke some bleeding from the endometrium. This is more likely to occur if the growth and structure of the endometrium has not been established soundly earlier in the follicular phase. In TCM terms, we say the Chong vessel is not consolidated. This can occur in cases of Yin and Blood deficiency or if there is Heat.
Herbal Formula: Rather than simply adding styptic herbs to our midcycle formula, chronic midcycle bleeding must be addressed by treating the imbalance at the early stages of the cycle so the uterine lining can be built after the period. For Yin deficiency with midcycle bleeding add:
| Han Lian Cao | 15 g | Herba Ecliptae Prostratae |
and increase Shan Yao and Nu Zhen Zi to 15 g each in post-menstrual and midcycle formulas.
| Jing Jie Tan | 6 g | Herba seu Flos Shizonepetae tenuifoliae (charred) |
| Zhi Zi | 9 g | Fructus Gardeniae Jasminoidis |