Diagnosis and Treatment of Female Infertility
The Two Key Elements: Ovulation and Menstruation
TCM Categories of Female Infertility
Part 2 – Traditional Chinese Medicine Treatments for Functional Infertility
Same Disease, Different Treatments
Problems in the Follicular Phase or at Ovulation
Menstrual Phase – Discharging the Lining of the Uterus
Midcycle Phase – Promoting Movement of Qi And Blood
Problems in the Luteal Phase or at Implantation
Part 1
Making a Diagnosis
Introduction
Before any TCM treatment is applied, the doctor must be sure of the diagnosis. By gathering together the relevant details of the case history, and looking at the tongue and taking the pulse, the pieces of the puzzle will usually form a picture which roughly approximates one or more of the patterns outlined in this chapter.
We seldom find a clear-cut textbook case in our clinics. Most women we see in infertility clinics in the West have already run the gauntlet of investigations and treatments – some of them quite invasive – and the diagnostic picture may have been considerably complicated by these. Nevertheless, with time and experience, the TCM doctor learns to sniff out what is relevant and ignore what is not, until a diagnosis and a plan of action can be made, as illustrated in the case histories throughout this book.
The Two Key Elements: Ovulation and Menstruation
Traditionally, the menstrual cycle, and any disturbances of it, were described in Chinese medicine texts only in terms of the period – the arrival (late, early or on time) or the non-arrival of the period – this being the most clearly observable external sign. Thus, observations of the timing and nature of the menstrual flow were the most important signs upon which a diagnosis could be made. Historically, treatments for infertility also gave great emphasis to the period, i.e., treatments were applied during or just before the menstrual flow.
We can now incorporate more modern ideas based on discoveries about female physiology made by Western doctors and scientists, and base our TCM diagnosis on more than just the menstrual flow. We can follow the menstrual cycle not just by the appearance of the period but also by other key events: most importantly the time that the egg is released from the ovary, i.e., ovulation. When we are concerned with fertility this is the key event of the menstrual cycle.
We have at our disposal in the wealthy Western countries extraordinary diagnostic tools which allow us not only to pinpoint the ovulatory event itself but also all the steps leading up to it. For example, a vaginal ultrasound can track the progress of a follicle from the very first signs of stimulation by the follicle-stimulating hormone (FSH) right up to its full size at maturity when the egg will be released. The ultrasound also reveals the readiness (i.e., thickness and structure) of the lining of the uterus to receive a fertilized egg. Blood tests can track ovulation by measuring:
• FSH, which stimulates follicle growth
• estrogen levels, which increase as the follicle grows
• luteinizing hormone (LH), which heralds the imminent release of the egg
• the progesterone produced by the corpus luteum after the egg has been released.
IVF clinics make full and productive use of all these diagnostic tools on a frequent and regular basis, which is one of the reasons these infertility programmes can be so expensive.
However, we do not need to rely on expensive and invasive tests to monitor the internal events of the menstrual cycle. Although not so quantitative in their measurements, careful observation of certain external signs can give us useful qualitative information (Box 4.1).
Taking a History
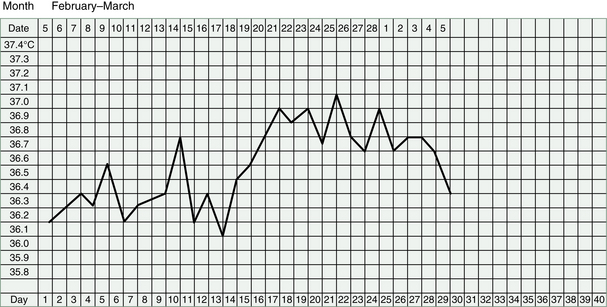
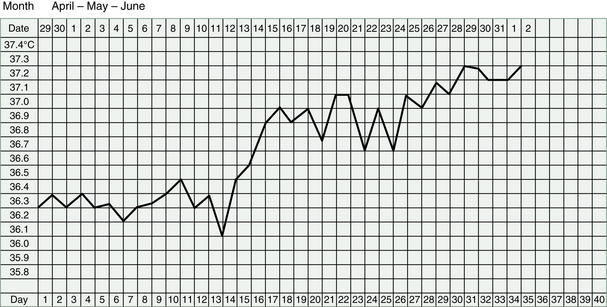
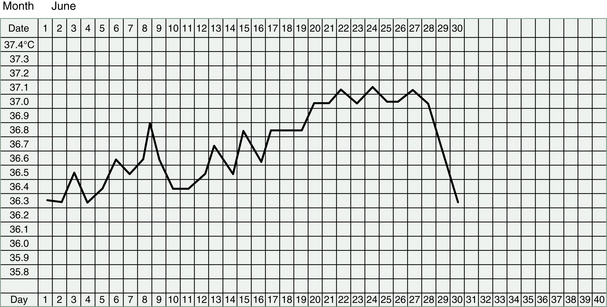
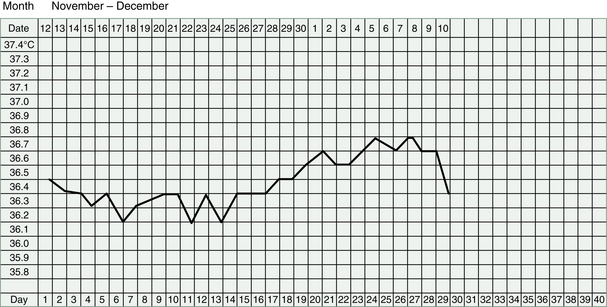
It makes good sense to start making our TCM diagnosis, and designing treatments, using these physiological signposts as well as subjective descriptions of symptoms. Questions about the period, the middle of the cycle and about sensations in the ovaries, breasts or genitals will offer valuable information. If our patient is recording her BBT, then we can discern even more information about her condition and the diagnosis of her infertility. The shape of the chart, as we saw in Chapter 3, will tell us about the Kidney Yin and Yang and the Qi of the Heart and Liver.
The Period
The period gives us unique insights into the workings of the reproductive system. The questions we ask are:
• When – regularity and length of cycle (early, late, on time)?
• How long – short or protracted period?
• How much – heavy, medium or scanty flow?
• Looks like – bright red, dark red, purplish, mucusy, clotty?
From such information we can already discern aspects of diagnosis related to Blood stagnation, or Qi deficiency or internal Heat or Cold and so on.
Midcycle
Symptoms and signs at midcycle are much more subtle and some women will notice very little until they are requested to watch closely for certain changes. What we want to know about primarily is the quality and quantity of the mucus produced by the glands in the cervix in response to the estrogen coming from the ripening follicles.
We ask the following questions about the fertile mucus and ovulation:
• When – Day 14, earlier, later?
• How long – fertile mucus evident for several days or just a few hours?
• How much – copious or scanty and difficult to detect?
All of this gives us information about the quality of the Yin and the movement of the Qi and when and how well it is developing in this phase of the cycle.
Pain in the Ovary
Some women feel pain or an ache on one or other side of the abdomen when the ovary on that side is enlarged with several ripening follicles. The pain is usually felt before the egg is released and from that point of view, is a useful indicator of the most fertile time for sexual intercourse. It is a cruel irony that for some women this pain is so strong that the idea of sex is anathema.
Breast Tenderness
Less commonly, the breasts and nipples react to the peak of estrogen produced by the ripening follicle and they can become swollen and sore. This tells us that there is probably a good amount of estrogen circulating. TCM theory, however, tells us that pain, even when associated with a normal physiological process, is an indicator of Qi being obstructed. In this case, the Liver Qi is not circulating well and the pain represents some stagnation of the Qi in the breasts.
TCM Categories of Female Infertility
At an infertility clinic in the West, we may describe female infertility using such labels as fallopian tube blockage, polycystic ovaries, inadequate luteal phase, oligomenorrhea or irregular, infrequent ovulation, resistant ovary syndrome, endometriosis and so on. Although these disease labels do not usually translate directly into specific TCM categories of infertility, the symptom pictures they manifest are easily analyzed and categorized to fit a TCM diagnostic pattern.
The section on female infertility in traditional TCM gynecology texts is usually found in the last chapter as one of ‘eight miscellaneous diseases.’ These texts usually describe four main categories of infertility (and sometimes numerous subcategories), which are given in Box 4.2.
What one sees when prescriptions are handed out to patients in the infertility clinic of the TCM teaching hospital which we visited in Chapter 1, or any other infertility clinic in China, is that nearly all the prescriptions treat the Kidneys. This is not because the last three of the four patterns described in Box 4.2 do not occur in practice but because they usually occur in combination with, or even as a result of, a Kidney weakness. If there is functional infertility, then by definition the Kidney Yin and Yang are depleted or not functioning correctly.
The categories of functional female infertility could be rewritten (Box 4.3):
1. Problems related to ovulation – Kidney Yin deficiency or Heart Qi stagnation (either of these two patterns can be complicated by Liver Qi stagnation, Phlegm-Damp or Blood stagnation)
2. Problems of embryo implantation – Kidney Yang deficiency (possibly complicated with Liver Qi stagnation, Phlegm-Damp or Blood stagnation).
We know there is no (or rare) ovulation if:
• there are very irregular periods
• the BBT chart shows no biphasic pattern
• blood tests show low estrogen/progesterone levels or high FSH levels.
We know there is ‘poor’ ovulation if:
• the BBT chart shows a small rise in temperature
• the temperature rise is very short-lived
• blood tests taken in the middle of the luteal phase show low levels of progesterone
We suspect problems with implantation if:
• there are fibroids or other physical barriers to implantation
• the uterine lining is inadequate on ultrasound and periods are scanty or dark or clotty
• we have eliminated everything else and pregnancy is still not occurring.
The following are general clinical pictures. It is important to remember when making a diagnosis that not all women who suffer from a particular deficiency or stagnation will show all (or even some) of the described symptoms and signs. Every case will manifest a different constellation, depending on where the deficiency or stagnation exerts its influence most.
Kidney Deficiency
The most common cause of functional infertility, Kidney deficiency, often underlies or coexists with other causes.
Women with weak Kidney energy will often present with some or all of the following:
• Poor stamina, low reserves of energy
• Some difficulty with urination, e.g., daytime frequency or frequent nocturia or slight incontinence
Kidney Jing Deficiency
Signs and Symptoms: Kidney Jing deficiency will be the diagnosis if there are, in addition to any of the above symptoms, the following:
• obvious developmental disorders in the reproductive organs, or
• little development of secondary sexual signs such as breast development, or
• under-functioning ovaries, even if the ovaries appear normal. Puberty may be late and ovulation may be erratic; sometimes the only sign is an inability of the ovaries to respond to fertility drugs.
BBT Chart and Fertile Mucus: BBT charts are usually not recorded because the cycle is erratic or absent. However, where charts are completed, there will usually be no pattern or an indistinct biphasic response. Fertile mucus is rarely seen.
Blood Tests: AMH (anti-Mullerian hormone) which is produced by the primary and preantral follicles in the ovary, will be low indicating a low reserve of follicles available for recruitment. In the case that ovaries are not functioning well, estrogen levels (in the follicular phase) and progesterone levels (in the luteal phase) will also be low. FSH may be elevated.
Kidney Yin Deficiency
Signs and Symptoms: This is an increasingly common diagnosis of infertility. Kidney Yin deficiency occurs especially in older women and usually arises out of depletion of resources – working (and playing) too hard without allowing the time and deep rest needed for replenishing body and soul.
A woman who is Yin deficient may complain of some or several of the following symptoms:
Often, but not always, she is thin or wiry and may tend to have dry skin or hair due to a lack of the cooling and moistening influence of Yin in the body – this leads to a relative excess of Yang, expressed as Heat or dryness. Yin deficiency often leads to Blood deficiency and the period flow may become scanty. On the other hand, Heat affecting the Blood may cause heavy bright-red periods.
BBT Chart and Fertile Mucus: The follicular phase of the Yin deficient woman’s chart is often unsteady and may be longer than the usual 13 or 14 days if ovulation is delayed. However, if Yin-deficient Heat provokes the release of an immature egg the follicular phase will be shortened.
The average temperature in the low phase may, in some cases, hover around 36.7°C (98°F) instead of the more usual 36.5°C (97.7°F) or lower. When Yin is deficient, it can also contribute to a poorly sustained temperature rise in the luteal phase.
There may be little discernible vaginal lubrication or fertile mucus. Any fertile mucus produced may have a tendency to be too acid in these women.
Kidney Yang Deficiency
Signs and Symptoms: Kidney Yang deficiency may reflect a constitutional tendency or occurs:
• after an injury to the body by Cold
• if the body is overstrained or
• out of long-term Yin deficiency or Qi deficiency or Heart or Liver Qi stagnation.
When the Kidney Yang is deficient, fluids are not metabolized efficiently and edema may result. Generally, body metabolism slows and it is easier to put on weight and harder to shift it.
Kidney Yang-deficient patients often show signs of:
• Low libido and general motivation
• Lower backache, sometimes accompanied by pain in the knees and legs, which feels worse in the cold weather.
Often, there is diarrhoea and lower back pain just before or at the beginning of the period. Dysmenorrhea can occur if the Yang is insufficient to ‘drive’ the blood flow. Clots in the menstrual flow, which are composed of tissue rather than blood, are thought by some Chinese doctors to indicate Kidney Yang deficiency also.
BBT Chart: BBT readings of Kidney Yang-deficient women can be quite low (36.0°C or 96.8°F or less); sometimes the temperature readings are off the bottom of the chart.
The temperature rise at ovulation is not often delayed in cases of Kidney Yang deficiency unless it is combined with Kidney Yin deficiency or Heart Yang deficiency or it is complicated with Damp-Phlegm or Blood Stagnation.
Kidney Yang deficiency often leads to inadequate luteal phase – the BBT readings in the second phase are not as high as they should be, or the temperature does not stay raised for long enough.
Readings on the urine LH detector kit may be inconclusive if the LH surge is inadequate.
Kidney Yin and Yang Deficiency
Signs and Symptoms: Often both Kidney Yin and Yang are deficient. In this case there will not be many obvious clinical symptoms of one or the other – in other words, the imbalances tend to cancel each other out so that there is no relative excess of either. Or sometimes there will be a confusing mix of Kidney Yin-deficient symptoms, e.g., hot soles of feet at night – along with Kidney Yang-deficient symptoms such as lethargy with a pale swollen tongue.
The diagnosis will most often be one of Kidney Yin and Yang deficiency when a woman presents with infertility if she:
BBT Chart and Fertile Mucus: A weakness of Kidney Yang that results from inadequate Kidney Yin typically produces a BBT chart with a reluctant start to the luteal phase, i.e., a very slow climb to the higher temperature level or a very small rise, i.e., only 0.2°C, or a rise which is short-lived. In these women, there is usually little fertile mucus.
Heart and Liver Qi Stagnation
Signs and Symptoms: The Heart is a very important organ when it comes to ovulating regularly and on time. TCM describes the importance of communication between Heart and Uterus via the Bao vessel. In Western physiological terms, this refers to the signals the ovary receives from the brain which determine the growth and release of eggs.
If a woman has a history of irregular ovulation, or has stopped ovulating altogether (anovulation), and there are reasons to think there may be an emotional cause then Heart Qi stagnation must be considered a likely diagnosis. Most cases of chronic anovulation (amenorrhoea) from emotional causes and stagnation are due to Heart Qi stagnation.
The TCM doctor will also suspect a Heart disorder if there are emotional factors which have precipitated the amenorrhoea. These factors may be recent, such as a sudden shock or upset, or more chronic, such as ongoing extreme anxiety or agitation. They may also hark back to years before, e.g., during puberty, when severe emotional distress can profoundly affect the incipient functioning of the Chong and the Ren vessels as they begin their reproductive roles.
As with diagnoses of the Kidney dysfunction leading to infertility, diagnoses of Heart Qi stagnation leading to infertility may have few of the typical symptoms, particularly if the Shen-disturbing events which obstructed the Bao vessel occurred a long time ago. However, a very skilled TCM diagnostician will in such cases be able to pick up a Shen disturbance in the eyes and the pulse.
With disturbances of the Heart and Shen, we may expect to see other symptoms such as:
When Heart Qi stagnation is prolonged or severe, then Heart-Fire develops. There will be more severe signs of Shen disturbance, including:
BBT Chart: Shen disturbance usually shows clearly on the BBT chart in the follicular phase as peaks and troughs or a generally very unsteady graph.
Heart-Fire can take the peaks to levels as high or higher than the luteal phase levels.
Pulse: The pulse may have a choppy or tight feeling at the left distal position or may be very thready at this position.
Blood Tests: These might show that the pituitary gland is under- or over-producing FSH or LH and estrogen levels may be low. In a woman in her mid- to late-40s (with Kidney Yin or Jing deficiency) this scenario indicates impending menopause, but in a younger woman it indicates a disorder somewhere along the hypothalamus-pituitary-ovary axis.
Liver Qi Stagnation
Signs and Symptoms: The Liver, like the Heart, is influenced by the emotions; therefore, Heart Qi and Liver Qi stagnation can occur together. However, Liver Qi stagnation manifests in slightly different ways and can cause symptoms at different times in the menstrual cycle.
Disorder of the Liver Qi is a very common cause of gynecologic conditions generally. Stress easily obstructs the smooth flow of Liver Qi and, since the Liver channel traverses the pelvis, and particularly the reproductive organs, this can throw a spanner in the menstrual cycle works.
The unimpeded flow of Liver Qi is necessary for several of the processes of the normal menstrual cycle. For example, those parts of the cycle which require movement – such as the expulsion of the egg, the trapping of it by the fallopian tubes and the passage of it down to the uterus – all require unobstructed Liver Qi in the pelvic area. When the Liver Qi is unobstructed, the changes in hormone levels are negotiated more smoothly and rapidly and symptoms do not develop. When the Chinese made these observations and developed these theories thousands of years ago they did not know of course that the liver, as we know it in Western physiological terms, is responsible for helping regulate hormone levels. It is in the liver that they are broken down effectively, if there are plentiful enzymes and cofactors.
Emotional stress at the time of ovulation can prevent the release of the egg. We also know that stress can affect the levels of hormones released by the pituitary, which are necessary for the growth and release of an egg. Usually this means an obvious disruption of the menstrual cycle, i.e., the period won’t come.
It is also possible for stress to reduce the hormone output to a level where there is just enough LH produced to luteinize the follicle so that it will start behaving as if ovulation has occurred (i.e., produce progesterone and a period will therefore follow) but in fact it hasn’t. This situation, known as luteinized unruptured follicle (LUF), may lead to a short (inadequate) luteal phase and is found more often in women with irregular cycles or endometriosis.
Stress at the time of ovulation can also cause the fine muscles of the fallopian tubes to tense and contract such that the egg/zygote is not able to find free passage to the uterus. Similarly, tension in the uterus, cervix and tubes does not help the journey of the sperm in their quest.
The effect of stress on the Liver Qi is more commonly noticed by women towards the end of the cycle, when it manifests as premenstrual syndrome.
The effects of obstructed Liver Qi are prominent before the period, because at this point change needs to be negotiated smoothly – if the Liver Qi is not moving freely, such changes bring with them annoying or distressing symptoms. In some women, it is the inability to adjust quickly enough to the rapid change in hormones that occurs after ovulation – these are the unfortunate women who notice premenstrual symptoms for nearly 2 weeks of every cycle. More often, Liver Qi gets stuck at the point when the body is registering whether a conception has occurred or not and is making the necessary adjustments in the hormones. Specifically, the progesterone starts to fall if there is no conception. The response of the body may be irritability, breast soreness, bloating or headaches in the week before the period.
Although emotional stress is the most common cause of Liver Qi stagnation, it can also be caused by prolonged drug use (prescription or recreational), including the oral contraceptive pill (see Ch. 5).
When Liver Qi stagnation is prolonged or severe, then Liver-Fire develops. This brings with it more intense irritability to the point of uncontrollable anger. There may also be headaches with bloodshot eyes. Liver-Fire often feeds Heart-Fire (according to the Five-Element cycle) bringing with it more severe emotional imbalances.
BBT Chart: Liver Qi stagnation on its own will not significantly affect the shape of the chart itself, except by lengthening it if ovulation is delayed. However, premenstrual Liver-Fire can lift the luteal phase basal temperatures. Caution is needed in such cases because it can obscure a Kidney Yang deficiency, which would normally be associated with low luteal phase temperatures. Liver-Fire in the earlier parts of the cycle can cause some instability or temperature peaks.
Pulse: Pulses tend to be wiry when there is Liver Qi stagnation, especially on the left side in the central position.
Blood Stagnation
Signs and Symptoms: Blood stagnation often develops as the long-term consequence of other disorders (e.g., Cold, Damp-Heat or Kidney deficiency) and is a complex syndrome in any discipline, no less gynecology. So the clinical picture can reflect aspects of several pathologies and may be complicated. Less often, Blood stagnation can be the direct consequence of trauma, e.g., surgery or an accident.
From a TCM point of view, the menstrual cycle will be adversely affected by Blood stagnation in that the Chong vessel (the Sea of Blood) will not be filled smoothly, and will not empty properly. The function of the Heart, which controls Blood circulation, will also be compromised.
Problems with the Chong vessel will be reflected in problems with the endometrium. For example, the way the lining forms and the way it breaks down may be faulty – there will be clots and tissue in the menstrual flow and its discharge may be incomplete, followed by spotting. Or there may be discharge from endometrial implants in the pelvic cavity if the woman has endometriosis. Problems of the Heart will be associated with the pituitary gland, which may send erratic or erroneous signals to the ovary or none at all.
Blood stagnation usually causes pain felt at a confined localized site. Menstrual flow is clotty and unsmooth. The stagnation will often be associated with substantial masses or growths. In clinical terms this category of infertility usually describes an obstruction somewhere in the reproductive tract or in the glands which control it. Endometriosis, uterine fibroids or polyps, fallopian tube blockages, ovarian cysts and tumors and pituitary tumors all fall into this category.
BBT Chart: BBT charts do not directly register the presence of Blood stagnation. However, if the Chong vessel does not empty completely during the period (as is often the case in endometriosis where blood from endometrial implants remains in the pelvic cavity), then the temperature may not fall to its low level immediately the new cycle starts. Instead it may take several days to gradually fall to the appropriate level of the follicular phase.
Phlegm-Damp Accumulation
Signs and Symptoms: Like Blood stagnation, Phlegm-Damp accumulation describes a complex phenomenon (unique to TCM) which includes congealing of fluids at certain sites or in certain systems such that their function is disrupted. When we are considering causes of infertility, such disruption may be found in the pituitary, the ovaries, the uterus or the fallopian tubes causing pituitary tumors, ovarian cysts, endometrial congestion or blocked or edematous tubes.
In normal situations the mucus in the tubes is just sufficient to firstly coat the walls and make them slippery, to stop the embryo sticking and burrowing into them and, at the isthmus where the mucus is thicker, to delay the passage of the fertilized egg for a couple of days during its first few cell divisions. However, in pathological scenarios, the Damp might completely obstruct the tube and not allow passage of the egg to the isthmus or the zygote (if there has been a conception) to the uterus. It may also coat and stick together the fimbriae at the end of the tubes, or even the ovary itself, preventing the egg from being released or being caught by the tube. There is some evidence that this occurs in cases of endometriosis (discussed further in Ch. 5). Polycystic ovary syndrome (PCOS) often falls into this category, as do some tube pathologies such as hydrosalpinx.
Phlegm-Damp most often develops secondarily to other pathologies, such as deficient Kidney Yang, Liver Qi stagnation or Blood stagnation. For this reason it will usually manifest clinically as a mixture of symptoms that reflect the various pathologies.
In some cases, however, Phlegm-Damp accumulation is simply the result of overeating rich, sweet food. Little by little the body’s digestive system is damaged by such a diet and will tend to break down food and fluids less and less well, until fatty or mucus deposits (called Phlegm-Damp) begin to disrupt organs and their function. Thus, Phlegm-Damp is often associated with obesity, or at least a tendency to put on weight.
The menstrual periods will often be scanty and thick or mucusy, and may come at irregularly spaced long intervals.
BBT Chart and Fertile Mucus: BBT charts reflect the effects (e.g., delayed ovulation) or origins (e.g., Kidney Yang deficiency) of Phlegm-Damp. They may appear to have little of the usual biphasic pattern or, if there is a temperature shift at ovulation it will be a small one.
Although Damp conditions often cause an increase in mucous membrane discharges, including vaginal discharges, there is usually very little of the stretchy fertile mucus seen around ovulation time because the cervical glands become obstructed by Phlegm-Damp.
Pulse: The pulse in a Phlegm-Damp condition is typically slippery and full; however, if the accumulation of Phlegm-Damp is isolated in a discrete location (e.g., one fallopian tube) then it may not register on the pulse. If Kidney Yang deficiency or Liver Qi stagnation are contributing causes of the Phlegm-Damp, their characteristics may be felt on the pulse instead.
Part 2
Traditional Chinese Medicine Treatments for Functional Infertility
Same Disease, Different Treatments
In Chinese medicine there is a saying:
For example, in the clinic we may see four women all with polycystic ovary disease. But these women’s clinical presentation may reflect four different types of TCM diagnosis and therefore four different treatment plans. Three women, on the other hand, who suffer variously from amenorrhoea, menstrual headaches or dysmenorrhea may all receive the same basic TCM diagnosis and be treated using small variations of the same guiding herbal prescription. The treatment of many and diverse women arriving at the fertility clinic likewise will proceed according to their TCM diagnosis and despite the common label ‘infertility’ they will all receive different individualized treatments. Modern innovations to TCM treatments come from the information we receive about particular events in the menstrual cycle using blood tests, ultrasounds, BBT measurements or cervical mucus examination.
Wide fluctuations in Qi and Blood and Yin and Yang occur during the menstrual cycle, resulting in different imbalances manifesting at different times. Two of the most obvious examples, often seen in the clinic, are Blood deficiency after the period and Liver Qi stagnation before the period. We now know that Kidney Yin deficiency affects, in particular, the processes of the first phase of the cycle, and Kidney Yang deficiency affects, in particular, the processes of the second phase of the cycle. So, naturally, our diagnosis and the emphasis of treatment changes at different times of the cycle – this is why the treatment of women is considered so much more complex than that of men.
In Chinese medicine texts, the Kidney is said to ‘dominate reproduction’ – the Kidney Yin and Yang must be adequate and balanced for the correct functioning of all aspects of the female (and male) reproductive organs. Consequently, the treatment of Kidney Yin and Yang underpins all Chinese medicine prescriptions for infertility. The exception to this rule is infertility caused by simple obstruction in the reproductive tract with no impairment of gland function. A young woman with blocked fallopian tubes (possibly a result of a non-symptomatic chlamydia infection years earlier) will often fall pregnant very easily once the obstruction is removed (surgically) or circumnavigated (by IVF procedures).
When it comes to treating infertility, or any other gynecologic disorder, no matter what our diagnosis, it is important to always keep the treatments congruent with the phase and stage of the menstrual cycle during which it is being administered. This means following closely the relative activities of the Chong and the Ren vessels and the relative balance of Kidney Yin and Yang.
Prescribing Treatment
In this chapter, I present a few guiding formulas and acupuncture treatments which can be applied at different times of the menstrual cycle and which can be modified to make them uniquely fitting for the individual patient. The herbal formulas presented here – all of them used by doctors working in infertility clinics in China today – are age-old century-tested medicines applied according to diagnoses arrived at using the traditional Bian Zheng (or pattern recognition) methods of TCM in combination with modern diagnostic methods.
Sometimes, Western drug therapy is appropriate alongside herbal or acupuncture treatment. This will be mentioned briefly here and in the following chapter, which looks at Western disease categories of infertility. The combination of IVF and other assisted reproduction technology (ART) with Chinese medicine is covered in Chapters 10 and 11. Lifestyle and dietary changes are often crucial too (see Ch. 12). Any practitioner can follow the simple approach outlined in this chapter. Simple prescribing, however, does not mean simplistic. Many very skillful and experienced doctors use simple classical formulas – the skill comes in the timing of their administration and the adjustments that are made to account for individual nuances in the presenting pattern. With experience, specialists in infertility refine their prescriptions elegantly and subtly.
The most useful way to approach prescribing, for practitioners new to this area, is to choose an appropriate guiding formula and then customize it to fit the patient. For example, because we are treating the reproductive system the classical formula Liu Wei Di Huang Wan, which supplements Kidney Yin, will turn up time and time again, but will be modified to suit different patients and the stage of the menstrual cycle.
The treatments presented here are only one set of possible guidelines – historically, there were many approaches taken by infertility doctors, who each developed their own favorite protocols. The following treatments are based on those developed by Professor Xia Gui Cheng from the Jiangsu Province Hospital in Nanjing.1 They represent one of the more rational and consistent approaches to the treatment of infertility in women, comprising sound, well-tested and proven strategies based on both Chinese medicine and Western medicine knowledge.
Chinese herbs are not always very convenient (or palatable) for Western women, and for those women who have difficulty taking them in decoction there are good alternatives. Responding to a demand by Western consumers for ‘convenient’ medicines, and increasingly by Chinese patients themselves, factories in China are now producing quality controlled ‘instant’ preparations of individual herbs which appear to retain a high degree of potency. These granulated herbs can be mixed up into prescriptions which are then dissolved in boiling water to make a ready-to-drink tea, reducing preparation time significantly. And for patients who really cannot tolerate the taste, the granules can be put in capsules.
Timing of Treatments
The application of the following treatment schedule is not as complicated as it might at first seem. In an ideal situation, we might try to arrange treatment of the patient to start at the beginning of the period or just after it. Of course, treatment can begin on whichever day the patient first comes to the clinic but we should be aiming at treatment through 3–6 full cycles (if the woman has monthly menstrual cycles and does not fall pregnant during this time), starting from the day the period begins.
Once treatment has been given to help discharge the menstrual flow, then the treatment to prepare for ovulation begins (3 or 4 days into the cycle). In many ways this is the most crucial time of the entire cycle. The basis for ovulation and even the implantation of an embryo is established from these early days. It is helpful to try and arrange clinic visits during this phase so that the practitioner can check the status of Yin and Blood by examining the pulse and the tongue, and the general demeanor and well-being of the patient, and prescribe the appropriate formula.
Changes in vaginal secretions as the cycle proceeds will indicate when the formula should be modified. If a woman has a regular cycle and easily discerned variations in vaginal secretions, appropriately labeled formulas can be given at the time of the post-period clinic visit to be taken in a sequence until ovulation or her next clinic visit.
The next important time for a clinic appointment is at the time of ovulation itself. Different herbs related to ovulation will be prescribed and dispensed at this time and acupuncture given to facilitate movement in the fallopian tubes and to calm the mind.
Post-ovulation prescriptions need to be taken a couple of days after the temperature has risen on the BBT chart and, unless symptoms change, this formula will be the one which is taken until the period comes or there is a positive pregnancy test. If more acupuncture is to be administered, it is most effective (and least risky) during the first week after ovulation.
For patients who do not have a regular cycle and who cannot easily determine the time of ovulation, the schedule of best-timed treatments is not quite so easy to predict or plan. Fertility treatment should start from the beginning of a period and weekly visits scheduled with the flexibility to move these forward if signs of ovulation (particularly cervical mucus) present themselves. Where there is no cycle at all, treatment for amenorrhoea will proceed as described in the next chapter.
Prescriptions
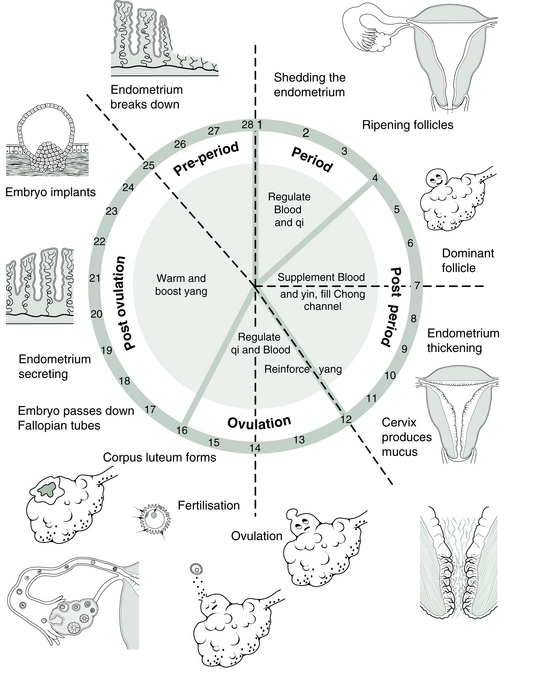
You will recall from Chapter 2 that the menstrual cycle is divided into four different phases (Fig. 4.1). Each of these phases has its own treatment characteristics.
Problems in the Follicular Phase or at Ovulation
Menstrual Phase – Discharging the Lining of the Uterus
Factors operating even at this early part of the cycle can already have a significant influence on events later in the cycle when an embryo might try to implant. So, our first concern in the clinic is to encourage the complete discharge of the menstrual blood so that a new endometrium can grow evenly on a smooth base. Although the Kidney Yin (Fig. 4.2) starts to grow as soon as a new cycle begins, we do not pay it attention immediately.
Clinicians working in ART centers have noticed that fertility is slightly increased in cycles after surgery in which the lining of the uterus is scraped out, a procedure known as dilatation and curettage (D&C). The state and environment of the newly formed endometrium appears to provide more favorable implantation sites for an embryo. In effect the acupuncture points used and the herbs prescribed during the period attempt a ‘herbal or acupuncture D&C’ – a good basis from which to start the next part of the treatment, which is the building of the Blood in the Chong vessel. Even if there is no evidence of stagnation (i.e., there is no pain or clotting), there may still be therapeutic benefit to be gained by encouraging a thorough ‘flushing’ of the uterine cavity before a new lining grows.
As we mentioned in Chapter 2, human females tend to have much heavier periods and have placentas that need much deeper invasion into the uterine lining than do other species. It is the priming and preconditioning of the uterine lining that happens during the menstrual phase to prepare for implantation and placental development that is what we wish to influence with out treatment during Phase 1.
Herbal Formula: The following well-known formula (Tao Hong Si Wu Tang) can be given in a patent pill form to encourage complete discharge of menses. However, if there are clinical signs of Blood stagnation, a decocted or granulated herbal preparation would be preferable to pills because they would have a more powerful action.
Tao Hong Si Wu Tang (Persica Carthamus Four Substances decoction)
| Dang Gui | 9 g | Radix Angelicae Sinensis |
| Shu Di | 12 g | Radix Rehmanniae Glutinosae Conquitae |
| Chuan Xiong | 6 g | Radix Ligustici Wallichii |
| Bai Shao | 12 g | Radix Paeoniae Lactiflorae |
| Tao Ren | 6 g | Semen Persicae |
| Hong Hua | 3 g | Flos Carthami Tinctorii |
The first four herbs in this prescription constitute Si Wu Tang, which nourishes and invigorates Blood. The addition of Tao Ren and Hong Hua aids in eliminating Blood stasis.
In the case of Qi deficiency, such that Qi does not lead the Blood add:
| Dang Shen | 9 g | Radix Codonopsis Pilulosae |
| Bai Zhu | 9 g | Rhizoma Atractylodis Macrocephalae |
Si Jun Zi Wan (Four Gentleman Combination).
In the case of Blood stagnation add:
| Wu Ling Zhi | 9 g | Excrementum Trogopterori |
| Pu Huang | 9 g | Pollen Typhae |
| Shan Zha | 12 g | Fructus Crataegi |
| Yan Hu Suo | 9 g | Rhizoma Corydalis Yanhusuo |
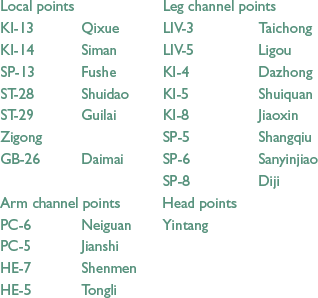
Acupuncture Points: Choose points from the following (and see Table 4.1):
Table 4.1
Acupuncture points used in treatment of infertility: menstrual phase
| Treatment goal | Acupuncture point |
| To open the uterus and encourage strong downward movement and a smooth and thorough discharge of the menstrual flow | CO-4 with SP-6 |
| To moderate this action and hold the Qi | Ren-6 |
| To treat all aspects of the Blood, both its movement and its supplementation and control the extent of the bleeding if there is Heat | SP-10 |
| To remove obstructions to Blood flow | SP-8 (Xi-cleft point of Spleen channel) |
| To move Blood | KI-14 (the most important point on the Chong channel for moving Blood) |
| To regulate the Qi in the uterus and moderate the descending action of SP-6 | Tituo |
| To regulate Qi in the lower Jiao | BL-25 and BL-30 |
| To regulate Qi specifically in the Uterus | BL-32 |
| To regulate Qi, particularly if there is pain in the back and sacrum | Baliao |
| To make Blood flow smoothly, relieve pain and calm the mind | PC-5 |
| SP-10 | Xuehai |
| SP-6 | Sanyinjiao |
| SP-8 | Diji |
| CO-4 | Hegu |
| ST-28 | Shuidao |
| KI-14 | Siman |
| Ren-6 | Qihai |
| Tituo | |
| BL-25 | Dachangshu |
| BL-30 | Baihuangshu |
| BL-32 | Ciliao or any of the other sacral points |
| PC-5 | Jianshi |
Post-Menstrual Phase – Building Kidney Yin and the Blood
In terms of building fertile potential, the post-menstrual, or follicular phase, is the most crucial phase of the cycle. Much careful thought must be given to making treatments as effective as possible at this time. Not only is this the time that the egg matures to its fullest potential for fertilization but it is also the time during which the lining of the uterus prepares from the ground up.
The way the endometrium constructs itself during this crucial post-menstrual phase has bearing on the success of implantation of an embryo and can also determine the nature of the next period flow (in terms of quantity and discomfort). Ideally, the endometrium should be around 10 mm thick by the time it has been completely reconstructed at midcycle. Both acupuncture and herbs can influence this orderly growth.
When do we Start to Reinforce the Yin?: We usually begin building Kidney Yin when the period finishes or is finishing. Typically, this is around Day 4 of the period (Day 1 being the 1st day of menstrual flow). If the bleeding is very scanty or short, it might be appropriate to start the Yin building treatment on Day 3. It is important to allow the endometrium time to completely discharge its unneeded fluids, blood and tissue before using tonics to start stimulating its growth again. On the other hand, if a woman has very long periods that continue well past Day 4 (e.g., for 10 days), starting Yin tonic treatment on Day 4 is recommended regardless. In such cases, giving herbs during the period to encourage it to discharge more efficiently over a shorter period of time is the appropriate course of action.
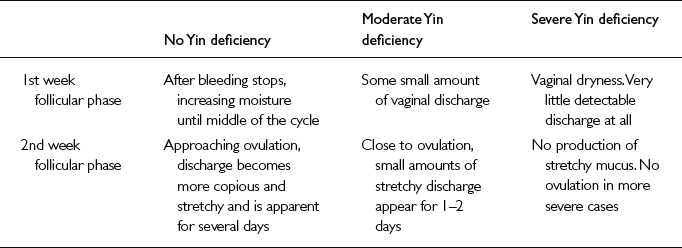
How do we know Yin Levels are Increasing?: When the bleeding stops, there is usually very little vaginal discharge, i.e., the Yin levels are still very low. Ideally, the vagina should be quite moist in the week after the period and the thicker stretchy fertile mucus should appear for several days prior to ovulation. Research done at the University of Umea in Sweden2 has shown us that there are three or four different types of fertile mucus produced by the cervix (see Ch. 3). The first is called the L type and is the type which gradually develops when Yin and Blood tonics are being taken during the first half of the cycle.
Assessing this vaginal discharge (i.e., asking the woman to observe very closely and record any changes) is one of the most useful ways of determining Kidney Yin levels (Table 4.2). The levels of discharge can, to some degree, decide the timing and the doses of the Yin tonic herbs the doctor prescribes.
Herbal Formula: In most fertility clinics, the base formula chosen is the famous Liu Wei Di Huang Tang, a treatment which was formulated hundreds of years ago and has been used ever since to build the Yin. Because we are going to use it just after the period and want to build the Blood as well as the Yin, it is usual to add the Blood tonics Dang Gui and Bai Shao. This makes the formula known as Gui Shao Di Huang Tang:
Gui Shao Di Huang Tang (Angelica Peonia Rehmannia decoction)
| Shu Di | 12 g | Radix Rehmanniae Glutinosae Conquitae |
| Shan Yao | 9 g | Radix Dioscorea Oppositae |
| Shan Zhu Yu | 9 g | Fructus Corni Officinalis |
| Fu Ling | 6 g | Sclerotium Poriae Cocos |
| Mu Dan Pi | 6 g | Cortex Moutan Radicis |
| Ze Xie | 6 g | Rhizoma Alismatis |
| Dang Gui | 9 g | Radix Angelicae Sinensis |
| Bai Shao | 9 g | Radix Paeoniae Lactiflorae |
Shu Di and Shan Zhu Yu enrich the Yin of the Kidney and Liver and Shan Yao enriches the Yin of the Spleen. To counteract the rich and cloying natures of the tonics (especially Shu Di), Ze Xie and Fu Ling are added. To clear Kidney-and Liver-Fire, Mu Dan Pi is added. The two extra Blood tonics added to this formula balance each other’s action: Dang Gui is warm and moist and moves the Blood gently; Bai Shao, on the other hand, while still nourishing the Blood, is cooling and sour and contracting.
If the period flow is still substantial on Day 4 the following herbs, which encourage the flow to finish by regulating the Blood, can be added to the guiding formula for a couple of days:
| Chi Shao | 9 g | Radix Paeoniae Rubra |
| Yi Mu Cao | 9 g | Herba Leonuri Heterophyll |
| Shan Zha (Sheng) | 9 g | Fructus Crataegi |
Some Yin and Blood tonics are hard to digest and, if that proves to be the case, then these formulas should be expanded to contain herbs to help Spleen function, e.g., Shu Di is often better digested if a few grams of Sha Ren are included. Alternatively, a patent medicine like Xiang Sha Lui Jun Zi Wan, which helps digestion by invigorating and regulating the Spleen and Stomach Qi, can be taken at the same time.
Preparing for Ovulation
Typically, the herbs are taken in decoction or granules once or twice a day until there starts to be evidence that the Yin is well established, i.e., until the vaginal discharge starts to become a little more marked. For some women it is difficult to make accurate or objective assessments of cervical mucus; however, with instruction and encouragement, it usually gets easier. And certainly, once the herbs have taken effect, fertile mucus becomes more copious and therefore easier to detect.
As Yin levels grow, Yang is consumed, i.e., the continuing growth of Yin depends on Yang. Therefore, as we approach the middle part of this phase of the cycle (around Day 8 or 9 say if ovulation is expected on Day 14) we need to start thinking about adding small amounts (5–6 g) of some mild Yang tonics to the guiding formula.
Herbal Formula: Choose two of the following:
| Tu Si Zi | 6 g | Semen Cuscatae |
| Rou Cong Rong | 6 g | Herba Cistanches |
| Xu Duan | 6 g | Radix Dipsaci |
This enhances the formation of stretchy cervical mucus, or S mucus, which, as we saw in Chapter 3, can provide very positive benefit to the sperm attempting to pass up the cervix.
Now as we approach midcycle, Yin is reaching its maximum. The Yin tonics in the base formula can be increased in dose:
| Shu Di | 15 g | Radix Rehmanniae Glutinosae Conquitae |
| Shan Zhu Yu | 12 g | Fructus Corni Officinalis |
More and stronger Yang tonics can be added now to aid the final and fullest stage of Yin growth (and the birth of Yang), which leads to plentiful fertile mucus, both S and the final P form, the release of LH and ovulation.
On Day 11 or 12 therefore, we add one or two of:
| Suo Yang | 6 g | Herba Cynomorii Songarici |
| Zi Shi Ying | 9 g | Fluoritum |
| Yin Yang Huo | 9 g | Herba Epimedii |
| Ba Ji Tian | 9 g | Radix Morindae Officinalis |
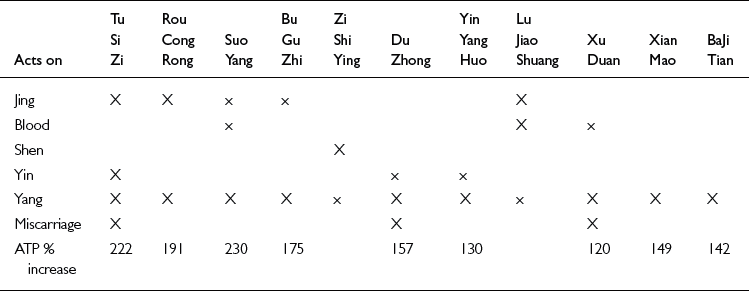
While the addition of Yang herbs to formulas prescribed when the egg inside the follicle is reaching maturity is based on an understanding of the cycle of Yin and Yang, researchers have found that these Yang herbs have a particular quality of enhancing energy (ATP) production in the mitochondria. This is precisely what is required in the developing egg cell as it is the mitochondria from the egg that will be responsible for providing the energy to drive the many cell divisions of the embryo in its first few days. Table 4.3 summarizes qualities of different yang herbs that might be used in fertility formulas and includes relative ATP production rates observed in laboratory studies on mice fed with different yang herbs.3
Acupuncture Points: There are many points that can be used in the first part of the menstrual cycle. There is documented evidence3 of increased blood supply to the uterus after acupuncture. Choose points from the following (and see Table 4.4):
Table 4.4
Acupuncture pointsa used in the treatment of infertility – post-menstrual phase
| Treatment goal | Acupuncture point |
| To balance both the Ren and Chong vessels at the outset of the cycle | Choose from: Ren-7, KI-5, KI-8, KI-13 |
| To influence Chong vessel activity | SP-4, ST-30 |
| To encourage Blood production | ST-36, LIV-3 and SP-10 |
| To emphasize development of Kidney Yin | Choose from: KI-3, KI-5, KI-6, SP-6, BL-23, Ren-4 |
| To influence Kidney Jing | ST-27 |
| To regulate Qi in the reproductive organs and supplement the Kidneys | Baliao |
| Ren-4 | Guanyuan |
| Ren-7 | Yinjiao |
| KI-3 | Taixi |
| KI-5 | Shuiquan |
| KI-8 | Jiaoxin |
| ST-30 | Qichong |
| KI-13 | Qixue |
| ST-27 | Daju |
| BL-23 | Shenshu |
| KI-4 | Dazhong |
| KI-6 | Zhaohai |
| SP-4 | Gongsun |
| SP-6 | Sanyinjiao |
| SP-10 | Xuehai |
| ST-36 | Zusanli |
| LIV-3 | Taichong |
| BL-32 | Ciliao or any of the other Baliao |
Throughout the post-menstrual phase, continue to use a selection of these points, especially those which reinforce both Kidney Yin and Yang and those which regulate the Chong and Ren vessels.
Modifications and Variations
If there are any other imbalances present: Heart or Liver stagnation, Blood stagnation or obstruction by Phlegm-Damp, we need to consider additions or subtractions to the basic formula. We also need to consider the relative balance of the Kidney Yin and Yang for each individual.
Kidney Yin Deficiency
The follicular phase, which is concerned with follicle and endometrium development, is the time when prescribed treatment includes building Yin whether there is a gross Yin deficiency or not. Here we discuss modifications to be made if the Yin deficiency is marked. It has long been recognized that Kidney Yin disorders are more difficult to treat successfully than Kidney Yang disorders, especially in women over 35.
Herbal Formula: If there is a functional ovulatory disorder we can assume a pathological deficiency of Kidney Yin. In some cases this will be accompanied by the systemic Yin-deficient signs and symptoms already discussed. In these cases we may need to add more Yin tonics to our base formula.
Add to the base formula (Gui Shao Di Huang Tang):
| Nu Zhen Zi | 12 g | Fructus Ligustri Lucidi |
| Han Lian Cao | 9 g | Herba Ecliptae Prostratae |
| Mai Dong | 9 g | Tuber Ophiopogonis |
Or increase the dose of the emperor herbs of our base formula from the beginning, e.g.:
| Shu Di | 15 g | Radix Rehmanniae Glutinosae Conquit |
| Shan Zhu Yu | 12 g | Fructus Corni Officinalis |
and add to these:
| Sheng Di | 15 g | Radix Rehmanniae Glutinosae |
To aid digestion of these herbs add:
| Sha Ren | 6 g | Fructus seu Semen Amomi |
Acupuncture Points: To directly nourish the Yin, herbs are more effective than acupuncture, but acupuncture is a useful adjunct, particularly where there is Yin deficiency Heat or the Chong and Ren vessel function is not well controlled due to the Kidney weakness. For some very restless or busy Yin-deficient women the half-hour rest on the acupuncture table may be the only time they stop in the day.
Choose points from those in Table 4.4 which emphasize treating the Kidney Yin. For example:
| KI-6 | Zhaohai |
| KI-3 | Taixi |
with reinforcing technique. And where there is Yin deficiency Heat add:
| KI-2 | Rangu |
with mild regulating technique.
Women with ovulatory disturbances (i.e., long irregular cycles) are often given a fertility drug called clomifene (Clomid or Serophene). In a Yin-deficient woman this is unfortunate – while clomifene is very effective in stimulating ovulation, it can be at the cost of the Yin. For example, the lack of fertile mucus and the thinness of the endometrium often seen in Yin-deficient women, can be exacerbated by this drug due to its anti-estrogen action (see Ch. 5). In the more unfortunate of these cases menstrual cycles may cease altogether. Ovulations induced by clomifene in Yin-deficient women rarely produce eggs which are of sufficient quality to produce viable embryos. TCM practitioners are always very wary of recommending the use of this drug for women who are distinctly Yin deficient.
Yin is usually depleted over a long period of time and, likewise, it takes some time to recover it. Yin-deficient women trying to fall pregnant may be looking at 6–12 months of building their Kidney Yin again with tonic herbs and a sensibly paced life.
The TCM practitioner also needs to encourage the woman to get enough good-quality sleep, a regular routine which factors in time for meals and exercise and ideally some down time for the mind. This could include meditation or mind-quietening activities such as yoga, tai chi, walking alone, swimming, etc.
Kidney Yang Deficiency
Herbal Formula: At the beginning of the cycle most of our treatment emphasis is on building Kidney Yin. However, if a woman is seriously Yang deficient this must be addressed at the same time we are nourishing Kidney Yin. Many women develop weak Spleen Qi and Kidney Yang functions as they age – this is why we often see a mixture of Kidney Yin and Kidney Yang-deficiency symptoms simultaneously in women in their late 30s and onwards. Remember though that the emphasis on building Kidney Yang still belongs mainly to the second half of the cycle and that is when strongest Yang tonic treatment can be applied. If there is a general Yang-deficient constitution, mild Kidney Yang tonics can be added to the base formula (Gui Shao Di Huang Tang) from Day 3 or 4, for example:
| Tu Si Zi | 9 g | Semen Cuscatae |
| Rou Cong Rong | 6 g | Herba Cistanches |
Stronger Kidney Yang tonics will be added only when the Yin base is established, i.e., the vaginal discharge is getting thicker and more stretchy.
If Rou Cong Rong causes diarrhea in someone with Spleen weakness it should be replaced with an alternative Yang tonic.
The use of fertility drugs, such as clomifene, is generally not contraindicated in cases of Yang deficiency unless the Yin is also quite deficient. In fact, ovulations induced by clomifene are generally followed by rather good luteal phases, indicating that this drug may indeed be beneficial to Kidney Yang.
Acupuncture Points: Points chosen from the list in Table 4.3 will emphasize those which reinforce both Kidney Yin and Yang, for example:
| Ren-4 | Guanyuan |
| KI-3 | Taixi |
And those which specifically boost Kidney Yang should be added:
| BL-23 | Shenshu |
| Ren-3 | Zhongji |
| BL-32 | Ciliao and the other Baliao |
Reinforcing technique and moxa are applicable for all points.
Kidney Jing Deficiency
Herbal Formula: The formula Gui Shao Di Huang Tang is very useful for supplementing Yin and Blood (i.e., stimulating the follicle and priming the endometrium) but the Jing (the eggs themselves) may also need attention. If ovulation is very uncertain or erratic, and particularly if that has been the case since puberty, the addition of herbs to nourish Jing is essential. Traditionally, this is done with the addition of animal products such as Gui Ban and Bie Jia. These substances are extracted from the soft part of the tortoise plastron. Since turtles and tortoises all over the world are now considered to be endangered species, the use of Gui Ban and Bie Jia should be restricted unless they come from a farmed source with a CITES certificate. Some practitioners and patients prefer to use the alternative Mu Li, which is made from ground oyster shell. Other substances, which can be added to our base formula when Jing is very low are:
| Zi He Che∗ | 1.5–3 g (in powder or pill form) | Placenta Hominis |
| Lu Jiao Jiao | 9 g | Cornu Cervi Parvum |
| He Shou Wu | 9 g | Radix Polygoni Multiflori |
Fertility drugs which act directly on the ovary (FSH preparations such as Puregon or Gonal-F) are often employed in these cases. These drugs are very potent stimulators of the ovary and, in most cases, if there are any follicles at all, an ovulation will be induced. However, the quality of the egg is not always good when the Jing is deficient.
Although Chinese herbs are much slower acting than fertility drugs, the ovulations they do eventually promote have a much better chance of being followed by a successful pregnancy.
Because Kidney Jing deficiency represents a deep level of deficiency, treatment will often need to continue for months or years. These cases can be difficult to treat successfully, especially if the reproductive organs are underdeveloped. Nevertheless, I have seen doctors in the fertility clinics in China commence treatment of seemingly very difficult cases of Kidney Jing deficiency to see if there was any response which would encourage further treatment – often there was.
Acupuncture Points: Some of the points listed for use in the follicular phase in Table 4.4 have an effect on the Jing, for example:
| BL-23 | Shenshu |
| Ren-4 | Guanyuan |
| ST-27 | Daju |
and other points such as:
| KI-12 | Dahe |
can be added but generally herbs have a greater impact on Jing deficiency than acupuncture.
Heart and Liver Qi Stagnation
Building and maintaining the Yin stores for the follicular phase requires a quiet mind. If the Heart Qi is disordered and the Shen is disturbed, it is very difficult to maintain such inner quiet and development of Yin is jeopardized. Women with such Shen disturbance would benefit greatly from a technique like meditation but often that is an impossible request – it is hard enough for them to sit still, let alone quiet the mind. Often it is best to encourage active pursuits which occupy the body and by their repetitive nature gradually quieten the mind, e.g., walking, jogging or swimming. Then, if appropriate, more internal exercises can be introduced like yoga or Tai Qi and then, eventually, may be meditation.
Herbal Formula: To stabilize the Shen and regulate Heart Qi add to the post-menstrual phase guiding formula (Gui Shao Di Huang Tang):
| He Huan Pi | 12 g | Cortex Albizziae Julibrissin |
| Bai Zi Ren | 9 g | Semen Biotae Orientalis |
| Mu Li | 15 g | Concha Ostreae |
or give at the same time the formula Gan Mai Da Zao Tang, which soothes the Heart with sweet flavors.
| Huang Lian | 3 g | Rhizoma Coptidis |
| Zhi Zi | 6 g | Fructus Gardeniae Jasminoidis |
| Lian Zi Xin | 1.5–3 g | Plumula Nelumbinis Nuciferae |
Liver Qi stagnation tends to cause more problems later in the cycle, but if there is general tension or high stress or pain with ovulation then herbs to regulate Liver Qi can usefully be added in the post-menstrual phase:
| He Huan Pi | 9 g | Cortex Albizziae Julibrissin |
| Suan Zao Ren | 12 g | Semen Ziziphi Spinosae |
| Chuan Lian Zi | 6 g | Fructus Meliae Toosendan |
| Qing Pi | 6 g | Pericarpium Citri Reticulatae Viridae |
| Mu Dan Pi | 9 g | Cortex Moutan Radicis |
| Chi Shao | 12 g | Radix Paeoniae Rubra |
Acupuncture Points: To the points chosen from Table 4.4, i.e., those which foster Yin and Blood and regulate the Chong and Ren vessels, add points to pacify Liver- and Heart-Fire such as:
| LIV-2 | Xingjian |
| HE-5 | Tongli |
| HE-7 | Shenmen |
| PC-6 | Neiguan |
| PC-7 | Daling |
These points can be needled with mild reducing technique if the patient is not too anxious.
Ovulation disturbances related to stress and emotional states tend not to be very long term and are generally not treated with fertility drugs by specialists (although occasionally an ardent GP will prescribe clomifene). Acupuncture treatment is generally very helpful in calming the mind to allow development of Yin in the post-menstrual phase.
Blood Stagnation
Symptoms of Blood stagnation manifest during the menstrual period and this is the best time to treat them. However, if we think the endometrium has not been smoothly discharged, herbs to regulate blood stagnation can also be added to the formulas we start using early in the follicular phase. Evidence of Blood stagnation could be continued spotting of dark blood after the period should have finished or a BBT chart on which the temperature does not drop with the arrival of the period.
Herbal Formula: In this case we should add to Gui Shao Di Huang Tang the herbs mentioned earlier that provoke more complete discharge of the endometrium:
| Yi Mu Cao | 15 g | Herba Leonuri Heterophylli |
| Chi Shao | 9 g | Radix Paeoniae Rubra |
| Shan Zha | 15 g | Fructus Crataegi |
If there is a known history of substantial Blood stagnation (e.g., endometrioma or ovarian cysts), then more herbs to regulate Blood can be added:
| Tao Ren | 9 g | Semen Persicae |
| Hong Hua | 6 g | Flos Carthami Tinctorii |
| Wu Ling Zhi | 9 g | Excrementum Trogopterori |
If a woman has been diagnosed with antisperm antibodies in the cervical mucus, sperm will be disabled before they can enter the uterus. Antisperm antibodies in the cervical mucus reflect a subtle level of Blood stagnation. Adding Blood-regulating herbs to those which reinforce the Kidney Yin will usually reduce the antibody load, allowing sperm to penetrate. Add to Gui Shao Di Huang Tang:
| Tao Ren | 6 g | Semen Persicae |
| Chuan Xiong | 6 g | Radix Ligustici Wallichii |
| Hong Hua | 3 g | Flos Carthami Tinctorii |
Even where there is no Blood stagnation it can be useful to encourage Blood circulation with herbs or acupuncture, as the endometrium is primed after the period and the new lining and blood vessels form. To aid this, add to the guiding formula just one herb:
| Dan Shen | 9 g | Radix Salviae Miltiorrhizae |
Acupuncture Points: Add to points chosen from Table 4.4, additional points to move Blood and Qi:
| KI-14 | Siman |
| Ren-3 | Zhongji |
| SP-12 | Chongmen |
| ST-29 | Guilai |
| LIV-5 | Ligou |
| SP-8 | Diji |
Reducing or regulating techniques are used on these points.
It is generally not a good idea for women to use fertility drugs in these cases and, especially where there is evidence of cysts or tumors on the ovaries or pituitary gland. Acupuncture with its excellent ability to move the Qi and Blood can be very useful in this category. Even where Blood stagnation is not evident, points that circulate the Blood will help the formation of the new endometrium.
Phlegm-Damp Accumulation
Phlegm-Damp accumulation presents us with a clinical challenge. We wish to build Yin to encourage follicle development which may have been retarded by the presence of Phlegm-Damp. However, herbs that enrich Yin create more moisture and are by nature sticky and therefore are not desirable when we want to clear out Damp and stickiness. Similarly, herbs that break up and dispel Phlegm-Damp are drying, which is not really the trend we want to encourage when we need the endometrium to grow and the cervix to start producing more fertile discharge.
Handling such a clinical conundrum requires expert judgment and some juggling. Initially, emphasis remains on building Kidney Yin; however, in this case it is necessary to add Kidney Yang tonics from the early stages as we did with Yang-deficient women. This is because strong Yang Qi prevents Damp accumulation. At the same time, herbs to help clear Phlegm-Damp can be added.
Herbal Formula: Thus, to our guiding formula (Gui Shao Di Huang Tang), we would add herbs such as:
| Tu Si Zi | 9 g | Semen Cuscatae |
| Xu Duan | 6 g | Radix Dipsaci |
| Ba Ji Tian | 6 g | Radix Morindae Officinalis |
| Yi Yi Ren | 15 g | Semen Coicis Lachryma-jobi |
| Sha Ren | 6 g | Fructus seu Semen Amomi |
And Fu Ling will be increased to 15 g.
In severe cases of Phlegm-Damp, or if there is difficulty digesting the herbs Shu Di and Dang Gui in the guiding formula should be replaced with:
| Nu Zhen Zi | 9 g | Fructus Ligustri Lucidi |
| Han Lian Cao | 9 g | Herba Ecliptae Prostratae |
| Ji Xue Teng | 12 g | Radix et Caulis Jixueteng |
Throughout the follicular phase, supplementation of Yin and Yang should be approximately equal. This minimizes some of the risks of using Yin tonics in a Damp environment. As Yin develops, herbs will be added quickly to promote ovulation (i.e., herbs which move Qi and Blood). In cases where there is Phlegm-Damp it is not advisable to wait until Yin is fully expressed (e.g., with copious fertile mucus) before starting to promote ovulation – it may never occur. Thus by Day 9 or 9 of a 28-day cycle, or when there are some initial signs of vaginal discharge or moisture, herbs which move the Qi and Blood (such as those discussed in the next section) will be employed.
Acupuncture Points: Add to the points chosen from Table 4.4:
| GB-26 | Daimai |
| SP-5 | Shangqui |
| BL-28 | Pangguangshu |
| Ren-6 | Qihai |
Use a regulating technique.
Sometimes fertility drugs such as clomifene, which promote ovulation and Kidney Yang, are used with good effect in Phlegm-Damp cases. However, caution must be used if there is evidence of cysts in the ovaries, a not uncommon expression of Phlegm-Damp (see Ch. 5).
Midcycle Phase – Promoting Movement of Qi and Blood
We have now reached the end of the post-menstrual phase, wherein the Yin and the Blood have been replenished and fortified. The ovary, at the time of fullest Yin, is now ready to release a mature egg. Plentiful stretchy mucus floods the cervical os ready to ferry thousands of sperm upwards and inwards. An egg is poised for liberation from its large ripe follicle when prompted by hormonal messages from the pituitary gland. This is a crucial moment that requires dramatic activity of the Qi and Blood and the switch from Yin to Yang.
The formulas described below for use in promoting ovulation will only be applied once the Yin base is laid, i.e., there must be some fertile mucus or indication of rapidly rising estrogen levels seen in blood tests. Then they can be used twice a day between 3 and 7 days.
Provided that Yin foundation is present we now apply strong herbal treatment to promote ovulation. One way to do this is to use herbs that move the Blood.
Herbal Formula: The formula Cu Pai Luan Tang is a well-known and often-used ovulation formula. In a young or relatively strong woman it will promote an effective ovulation from a sound Yin base. It can be used for around 3 days starting just before the assumed day of ovulation.
Cu Pai Luan Tang (Ovulation decoction)
| Dang Gui | 9 g | Radix Angelicae Sinensis |
| Chi Shao | 9 g | Radix Paeoniae Rubra |
| Chuan Xiong | 6 g | Radix Ligustici Wallichii |
| Hong Hua | 6 g | Flos Carthami Tinctorii |
| Dan Shen | 9 g | Radix Salviae Miltiorrhizae |
| Ze Lan | 9 g | Herba Lycopi Lucidi |
| Ji Xue Teng | 15 g | Radix et Caulis Jixueteng |
All seven herbs in this prescription regulate the Blood, ensuring there is no obstruction in the process of ovulation and passage of the egg in the fallopian tube. Circulation in the endometrium as it prepares for an embryo is enhanced also.
This formula should be boiled for a short time only (around 5 min) with the lid on so as not to lose the volatile components which are helpful in provoking Qi and Blood movement. Granulated herbs should be dissolved in hot rather than boiling water for the same reason.
Acupuncture Points: Choose points from (and see Table 4.5):
Table 4.5
Acupuncture pointsa used in the treatment of infertility – ovulation phase
| Treatment goal | Acupuncture point |
| To regulate the Qi in the area of the ovaries and the fallopian tubes | Choose from: KI-13, KI-14, SP-13, ST-28, ST-29, Zigong |
| To move the Qi in the Liver channel, which passes through the lateral abdomen region | LIV-3 and LIV-5 |
| To promote ovulation by regulating the Qi and Blood | KI-5 and KI-8 |
| To enhance Kidney function and stabilize emotions | KI-4 |
| To influence activity of the Chong and Ren vessels – especially useful at ovulation time through its influence on the Dai channel, ensuring the fallopian tubes are not obstructed by excess secretions | GB-26 |
| To calm the mind, an important consideration at ovulation; also useful if there is suspicion of tubal obstruction by excess secretions | SP-5 |
| To promote circulation of Blood at ovulation if there is some question of tube patency | SP-8 |
| To promote circulation of Blood and the action of the Spleen as an intermediary between the Heart and Kidneys (i.e., the Bao vessel and Bao channel) | SP-6 |
| To calm the spirit and influence the Bao vessel | HE-5 and PC-5 |
| To further calm the mind | HE-7 and PC-6, Yintang |
| To regulate the Heart Qi and clear Heat in the Blood which might show as midcycle spotting | PC-4 |
aUse local and leg points with mild reducing method and even method with wrist points. The choice of abdomen or back points can be guided by sensations or pain.