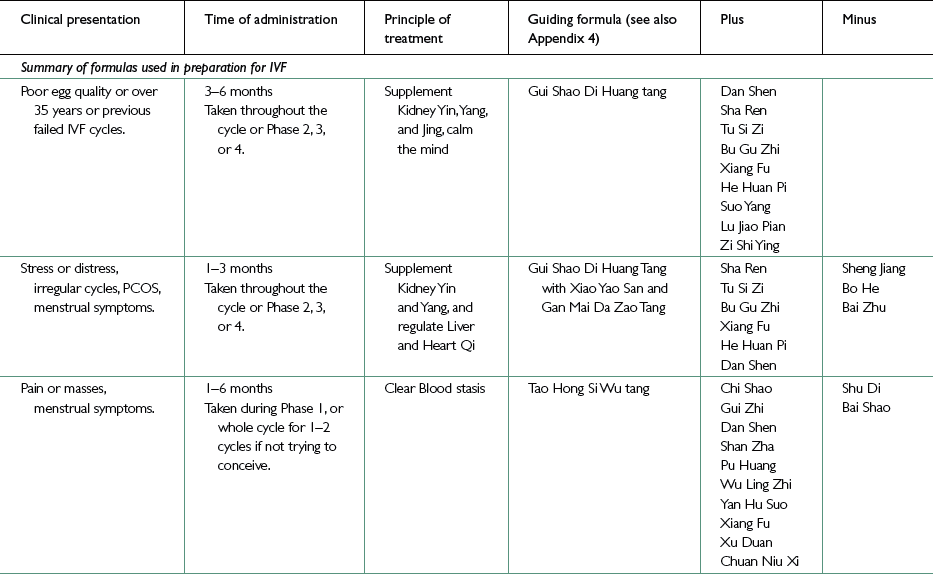
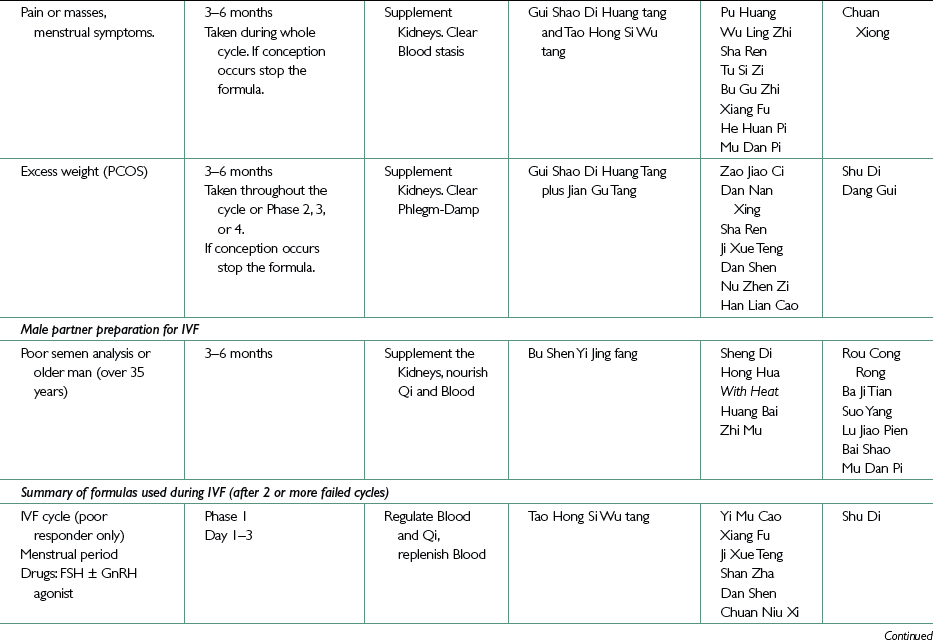
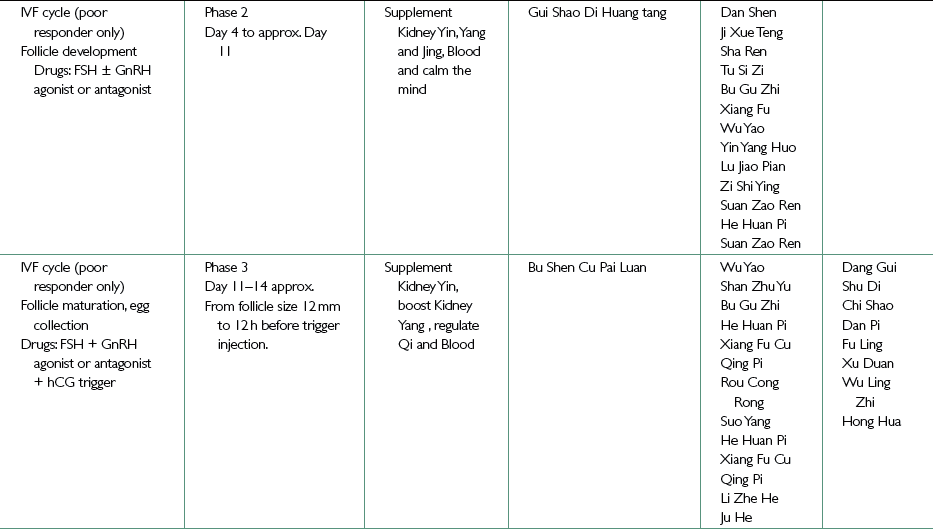
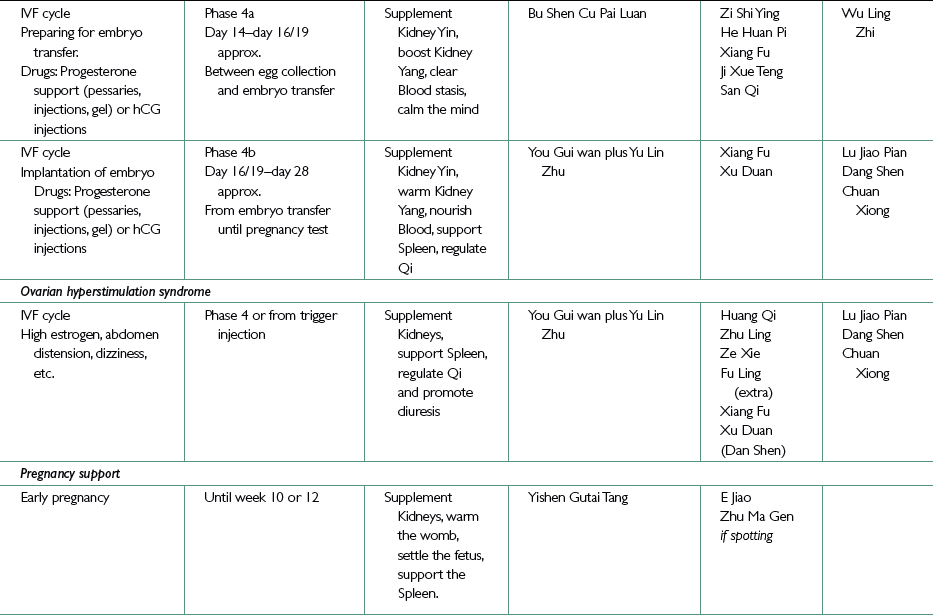
Traditional Chinese medicine treatment of the IVF patient
Using TCM in Preparation for an IVF Cycle
Treatment During the IVF Cycle
Ovarian Hyper-Stimulation Syndrome
Using TCM in Preparation for an IVF Cycle
Once a full TCM diagnosis of the cause of infertility or other conditions is made, we follow the protocols outlined in detail in Chapter 4.
In an ideal situation, 6–9 months of ovary ‘make over’ is advisable. This allows time to remove factors that might be toxic to ovary and uterine health, like internal Heat or Damp, stagnant Blood (such as is found in endometriosis, PCOS, pelvic inflammatory disease, etc.), and includes identifying and avoiding workplace and domestic pollutants and lifestyle changes such as optimizing good diet and minimizing certain dietary ‘indiscretions’. It is also an appropriate period of time over which Kidney Jing can be replenished with herbs and the function of Kidney Yin and Yang can be improved with tonics for the Yin, Yang, Qi and blood. This will not increase the number of eggs in the ovaries but well nourished eggs in a balanced hormonal environment can be more responsive to stimulation by FSH from the pituitary or the pharmacist’s EpiPen. However, it is rare that a patient who has reached the point of considering IVF, or doing further IVF, will be in a position to spend 9 months doing this sort of preparation. Often, anything is better than nothing, and I try to persuade patients to consider at least 3 months of preparation before starting IVF (again).
Some women who are not infertile but are doing IVF due to male factor infertility will choose to use TCM treatment to prepare their body for optimal outcomes. A diagnosis is done in the usual way, considering the constitution and any symptoms. But additionally, we are mindful of increasing ovarian resilience and response by boosting Kidney function, and will also be mindful of clearing any signs of stagnation in the uterus. It is usually the case that a shorter preparation time is necessary for these women, unless there are significant general health issues.
Our approach to treatment of women with infertility will be according to the four categories of infertility we have previously described (Kidney deficiency, Liver/Heart Qi stagnation, Blood stagnation, Phlegm-Damp obstruction). We shall discuss each of these categories and describe a simplified approach to treatment with herbs that can be undertaken in the weeks or months leading up to IVF.
Kidney deficiency (and egg quality)
A large number of the women seeking help for infertility from the Chinese medicine clinic and the IVF clinic fall into a Kidney deficient category. These are often women in their late 30s and early 40s, or those who are depleted by overwork. If they have already attempted some IVF cycles they will often have heard from their specialist that their egg quality is not so good.
Egg quality is something mentioned in hallowed terms in IVF clinics because it is somewhat unfathomable and seemingly beyond the influence of the IVF specialists or scientists. Some ovaries age more quickly than others and unfortunately, neither acupuncture nor Chinese herbs (nor much else) can increase the number of eggs left in the ovary or change the integrity of the chromosomes. Nobody, not even the most skilled doctor, can improve the genetic quality of an ‘old’ egg because its genetic material was created decades earlier, when the woman was an embryo herself, and it has been subject to the relentless cellular wear and tear of decades. However, there is more to an egg than just its DNA and it is in consideration of its other components that we hope to apply some influence.
The environment that eggs occupy during their lengthy maturation process inside the follicles of the ovary has an impact on what shape they are in before meeting a sperm (with or without an IVF embryologist in attendance). They need a good blood supply, sufficient oxygen, adequate amounts of the right nutrients, the right hormone signals and the capacity to supply enough energy to the embryo.
This has important implications, particularly for eggs that are coming from slightly older ovaries (or where AMH levels are low or FSH levels are elevated) and possibly for eggs coming from women with PCOS or endometriosis.
The question is, can Chinese medicine be used to rejuvenate some oocyte characteristics by improving delivery of oxygen and nutrition to the developing egg and enhancing capacity to make energy (ATP), thus increasing the chances of making viable embryos? There is evidence to say that it can.
Research has shown that eggs that come from follicles with optimal blood supply and oxygen content have higher fertilization rates and developmental potential leading to improved IVF outcomes.1
The blood supply to the follicles in older ovaries is reduced at the later stages of their development, meaning that these eggs do not receive optimal oxygen or nutrition,2 which may be a contributing factor to the poor quality of older eggs. Unlike chromosomal integrity, this is something we can influence.
Acupuncture has been shown to promote the growth of new blood vessels (angiogenesis)3 and to specifically increase blood flow to the ovaries.4
In summary, we could say that the use of certain acupuncture point combinations, stimulated with a gentle electrical pulse can promote blood supply, and delivery of nutrition and oxygen to the follicles and therefore hope to improve their potential to fertilize and create embryos. Another way we may be able to improve egg quality is by improving the egg’s capacity to make energy so that it can impart this enhanced capacity onto an embryo after fertilization. The organelles in the cytoplasm of the oocyte, called the mitochondria, have been identified as possible markers for egg and embryo quality. These powerhouses of the cell, which are donated from the egg to the embryo, are responsible for providing energy for cell division and metabolism in a process called aerobic respiration.
Those oocytes that consume more oxygen before fertilization (i.e., have more active aerobic respiration), are the ones which form better quality embryos.5
The early pre-implantation embryo occupies a low oxygen environment (the fallopian tube or the Petri dish in the IVF lab) and relies on anaerobic as well as aerobic respiration. By the time the embryo reaches the uterus (Day 5 or 6), it needs not only good numbers of mitochondria but optimal mitochondrial function and ATP production via aerobic respiration to succeed in implanting.6
It is at this level that Chinese medicine hopes to exert some beneficial influence by ensuring the number and activity of the mitochondria in the ripening eggs is optimal. We know that eggs with more energy (ATP) have a better chance of making viable embryos and that the rate of division and successful implantation of embryos has more to do with how much energy they have than with maternal age. However, the mitochondria of older eggs are not so good at producing ATP7 and the eggs of poor responders to IVF drugs have three times less mitochondria than those of good responders.8
Similarly, it is known that older follicles have fewer antioxidant defenses against cellular damage caused by aerobic respiration and oxidative stress,9 and that this too is related to poorer IVF outcomes.10
The ART embryologists have been experimenting with adding younger mitochondria to the eggs from older women to see if this helps to make better embryos. The Chinese herbalist uses Kidney Yang herbs to do the something similar. These are the herbs that we saw added to fertility formulas in the late stages of the follicular phase (Phase 3) (see Ch. 4).
Interestingly, researchers have shown that it is precisely these particular herbs (used in fertility clinics in China for many centuries!) that markedly enhance mitochondrial activity and ATP production in laboratory studies on mice, while other herb categories such as Qi or Yin tonics have little effect on mitochondrial ATP production. These same herbs were shown to enhance antioxidant defenses at the cellular level.11
What the ancients knew from trial and error scientists are now proving in labs. We must bear in mind however, that for the doctor of TCM, the clinical experience of thousands of years of Chinese herbalists treating infertility carries more weight than the lab findings examining mouse tissues. That is not to say it isn’t satisfying when a new science can verify an old one.
Thus, we might surmise that the Kidney Yang herbs that are taken in the days leading up to ovulation, when the egg is maturing, can boost mitochondrial function, which then gives a newly formed embryo an advantage by dint of increased energy making capacity to aid development and successful implantation.
The herbs in Box 11.1 were found to increase ATP output in mice tissues. They are listed in descending order of effectiveness.
Thus, when we are choosing which Yang herbs to add to our formulas in the days before ovulation, we might consider not only the characteristics we examined in Chapter 4 when constructing our formulas but also the potency they have shown in laboratory tests.
Back to the clinic and to our patient who is concerned with egg quality, we must recognize that we have a condition, Kidney deficiency, that is not one that responds quickly to treatment – it takes time, rest, regular routines, reduced stress, adequate sleep, good nutrition and the sorts of treatments a doctor of Chinese medicine can provide.
However, time is usually the one thing these women often don’t have. They are anxious to get to the IVF clinic, or back to the IVF clinic, hounded by the ticking of the biological clock and the sound of their IVF specialists voice saying, ‘You shouldn’t have left it so long!’ But the sad irony is that for these women, IVF or repeated IVF, only drains the Kidney further.
What to do? …
In the case of a woman who is older or who has responded poorly in previous IVF cycles and now wishes to add a TCM approach, we focus especially on ovarian function and egg quality. This is done in exactly the way we described previously, by focusing on strongly reinforcing Kidney Jing, Yin and Blood. Ideally, this is done over a period of 6 months or more but even if only 3 months of strong Kidney Jing and Yin nourishment can be maintained alongside important lifestyle changes, then some changes will be achieved and hopefully responsiveness and resilience of the ovary will be sufficiently improved.
If your patient is actively trying to conceive, then use the treatment principles outlined in Chapter 4 for Kidney Jing and/or Yin deficiency. However, your patient may now be planning or waiting to do IVF and may no longer be trying so actively to conceive naturally. You and she may prefer an approach that is a little simpler than the complex 4-Phase one. In this case, you can combine the ideas inherent in both Phases 2 and 4 to create a formula which can be taken all month.
A comprehensive formula which combines both Gui Shao Di Huang Tang with Kidney Jing and Yang tonics is appropriate for across the board use in Phases 2, 3, and 4.
Herbal formula: Such a formula can be modified to take into account Yin-deficient Heat with the addition of Zhi Mu and Huang Bai. If the Spleen is weak you may need to increase the amount of Sha Ren and reduce the amount of Shu Di.
Gui Shao Di Huang Tang (Angelica Peonia Rehmannia decoction) modified
| Shu Di | 12 g | Radix Rehmanniae Glutinosae Conquitae |
| Shan Yao | 9 g | Radix Dioscorea Oppositae |
| Shan Zhu Yu | 9 g | Fructus Corni Officinalis |
| Fu Ling | 9 g | Sclerotium Poriae Cocos |
| Mu Dan Pi | 9 g | Cortex Moutan Radicis |
| Ze Xie | 6 g | Rhizoma Alismatis |
| Dang Gui | 9 g | Radix Angelicae Sinensis |
| Bai Shao | 9 g | Radix Paeoniae Lactiflorae |
| Dan Shen | 9 g | Radix Salviae Miltiorrhizae |
| Sha Ren | 6 g | Fructus seu Semen Amomi |
| Tu Si Zi | 9 g | Semen Cuscatae |
| Bu Gu Zhi | 9 g | Fructus Psoraleae |
| Xiang Fu | 6 g | Rhizoma Cyperi Rotundi |
| He Huan Pi | 9 g | Cortex Albizziae Julibrissin |
| Suo Yang | 6 g | Herba Cynomorii Songarici |
| Lu Jiao Pian | 6 g | Cornu Cervi Parvum |
| Zi Shi Ying | 6 g | Fluoritum |
This expanded version of Gui Shao Di Huang Tang prepares a woman for IVF by reinforcing the Kidney Yin, Yang, and Jing, and calming the mind.
This formula can be taken for 3 or more months, with a break during the period if required. As we saw in Chapter 4, the main action of Gui Shao Di Huang tang is to reinforce Kidney Yin and the Blood. Here, we add herbs that support Kidney Yang as well, and herbs to calm the mind and keep the Qi and blood moving smoothly, so that it is applicable at all times of the cycle. Should your patient conceive during this preparation time, then switch formulas to one focusing on miscarriage prevention (see below).
During the menstrual period, a formula based on Tao Hong Si Wu Tang (see Ch. 4) could be taken.
Acupuncture treatment used to prepare for IVF will take into account patient circumstances, constitutional factors and the time of the cycle. (Follow the principles outlined in Ch. 4, and refer to Tables 4.1–4.7.)
Heart and Liver Qi stagnation (and sleep and stress)
As mentioned above, it is women with Heart and Liver Qi stagnation who benefit greatly from treatment during the IVF cycle, however preparatory treatment to regulate the cycle and calm the nervous system will also pay dividends. Sometimes in a big way, these patients are quite likely to respond quickly to acupuncture and may conceive before the (next) IVF cycle.
Treatment protocols following the 4 Phases are those found in Chapter 4. If, however, a simpler approach is required, then combining an expanded version of Gui Shao Di Huang Tang with elements of Xiao Yao San or Gan Mai Da Zao Tang could be taken all month to prepare your patient and her ovaries for IVF.
Herbal formula: The formula of choice is:
Gui Shao Di Huang Tang (Angelica Peonia Rehmannia decoction) with Xiao Yao San (Bupleurum and Tangkuei powder) and Gan Mai Da Zao Tang (Licorice, Wheat, and Jujube Decoction) modified
| Shu Di | 9 g | Radix Rehmanniae Glutinosae Conquitae |
| Shan Yao | 9 g | Radix Dioscorea Oppositae |
| Shan Zhu Yu | 9 g | Fructus Corni Officinalis |
| Dang Gui | 9 g | Radix Angelicae Sinensis |
| Bai Shao | 9 g | Radix Paeoniae Lactiflorae |
| Dan Shen | 9 g | Radix Salviae Miltiorrhizae |
| Fu Ling | 9 g | Sclerotium Poriae Cocos |
| Mu Dan Pi | 9 g | Cortex Moutan Radicis |
| Ze Xie | 9 g | Rhizoma Alismatis |
| Sha Ren | 3 g | Fructus seu Semen Amomi |
| Tu Si Zi | 9 g | Semen Cuscatae |
| Bu Gu Zhi | 6 g | Fructus Psoraleae |
| Xiang Fu | 6 g | Rhizoma Cyperi Rotundi |
| He Huan Pi | 9 g | Cortex Albizziae Julibrissin |
| Chai Hu | 9 g | Radix Bupleuri |
| Fu Xiao Mai | 6 g | Semen Tritici Aestivi Levis |
| Da Zao | 6 pieces | Fructus Zizyphi Jujuba |
| Gan Cao | 6 g | Radix Glycyrrhizae Uralensis |
Using this sort of formula to prepare for IVF will provide support for the Kidney Yin and Yang and Blood at the same time adding a little more focus on regulation of the Heart and Liver Qi. The actions of Gui Shao Di Huang Tang and Xiao Yao San we have discussed before. The sweetness of Da Zao, Gan Cao and Fu Xiao Mai (Gan Mai Da Zao Tang) soothe the mind and relieve melancholy and sadness, commonly experienced by patients who have given up the possibility of conceiving naturally.
Should your patient conceive during this preparation time, then switch the formula to one focusing on early pregnancy support (see below).
During the menstrual period, a formula based on Tao Hong Si Wu Tang (see Ch. 4) could be taken. For acupuncture protocols, please refer to Tables 4.1–4.7 for general prescriptions, alongside modifications for Liver and Heart stagnation, Table 4.8.
Reducing stress
Apart from regulating the menstrual cycle and helping your patient’s mood, there is good reason to regulate the Liver Qi and reduce stress hormone levels before IVF. We know that stress can have a negative impact on IUI12 and IVF outcomes,13 and that women who have taken active measures to reduce their stress have had better results with IVF than those who don’t, especially if they are doing their second or more cycles.14–16 Women who do not feel depressed before starting IVF treatment conceive twice as often as women who are depressed before treatment,17,18 so ensuring healthy and unobstructed Liver Qi can have significant implications for a future IVF cycle.
Some researchers suspect that stress may impact specific factors in the endometrium as well as its general effects on hormones. It is not so easy to directly examine endometrial implantation sites in women trying to conceive, but studies on animal models have revealed a negative impact of stress on uterine receptivity and number of implantation sites.19 Stress, and its affect on fertility in general is discussed in Chapter 12.
The formula above addresses many of the aspects of infertility related to stress, but in more severe cases, the dose of He Huan Pi can be increased.
Improving sleep
Sleep quality and quantity (see also Ch. 12) should be a focus of our attention in the patient with an unstable Shen planning to do IVF, particularly if she suffers from insomnia. People with chronic insomnia tend to have higher levels of some cytokines, notably interleukin-6 and tumor necrosis factor.20 These immune factors can impact implantation of the embryo and placental development. Some researchers have proposed that a suboptimal cytokine environment can contribute to miscarriage.21 Certain cytokines can lead to clotting of the placental vessels in cases of early or late pregnancy loss, or interference of angiogenesis in cases of occult pregnancy loss.
The formula above can be further modified with Shen calming agents such as Mu Li and Suan Zao Ren, in the case of insomnia.
Blood stagnation
Treatment in the 3 cycles before IVF can be very useful in going some way to resolving blood stagnation, which might affect oocyte or endometrium quality. Most Blood stagnation pathologies affect the endometrium, whether they be ones that require surgery such as large submucosal fibroids or polyps, or ones not always so amenable to surgery such as adenomyosis, endometritis or diffuse endometriosis. Some forms of Blood stagnation appear to affect the egg quality as well as the endometrium quality, and this is also amenable to treatment. For example there is some evidence to show that Chinese herbs improve egg quality in patients with endometriosis by reducing inflammatory markers in the follicular fluid.22
Treatment protocols are those described in Chapter 4 with a large emphasis on clearing stagnation during Phase 1, during the menstrual flow. In this way, we hope to alter the endometrium and the way it forms in the hope that this will reduce risk of implantation failure. This sort of treatment aims to minimize the effect of immune and clotting factors which can jeopardize implantation and placenta formation.
Improving the hormonal and immune milieu of the ovaries of these patients with endometriosis with acupuncture or Chinese herbs in the months before doing IVF could have benefits similar to treatment of older ovaries, i.e., an improvement in the egg quality.
The progress of your treatment may be effectively monitored by menstrual symptoms such as pain or the nature of the menstrual flow.
A simplified approach using herbs in preparation for IVF would be the use of a Phase 1 type of formula such as that below, during the period, and at other times of the cycle if natural conception is not being attempted. Where your patient is still attempting to conceive, use the formula below (Tao Hong Si Wu tang modified) during the period followed by the next formula (Gui Shao Di Huang tang plus Tao Hong Si Wu tang modified) for the rest of the cycle to prepare the ovaries for the IVF drugs.
Herbal formula: The formula of choice is:
Tao Hong Si Wu tang (Persica Carthamus Four Substances decoction) modified
| Dang Gui | 9 g | Radix Angelicae Sinensis |
| Chi Shao | 9 g | Radix Paeoniae Rubra |
| Chuan Xiong | 6 g | Radix Ligustici Wallichii |
| Tao Ren | 9 g | Semen Persicae |
| Hong Hua | 9 g | Flos Carthami Tinctorii |
| Gui Zhi | 3 g | Ramulus Cinnamomi Cassiae |
| Dan Shen | 9 g | Radix Salviae Miltiorrhizae |
| Shan Zha | 6 g | Fructus Crataegi |
| Pu Huang | 9 g | Pollen Typhae |
| Wu Ling Zhi | 9 g | Excrementum Trogopterori |
| Yan Hu Suo | 12 g | Rhizoma Corydalis Yanhusuo |
| Xiang Fu | 9 g | Rhizoma Cyperi Rotundi |
| Xu Duan | 9 g | Radix Dipsaci |
| Chuan Niu Xi | 6 g | Radix Cyathulae |
This formula which expands the reach of Tao Hong Si Wu tang (described in Ch. 4) is single pointed in its application to clearing Blood stasis and can be taken in the weeks leading up to an IVF cycle in patients who show clear signs of stasis, such as menstrual clots or abdomen pain. If the stasis is material and substantial in the form of endometriosis or fibroids then the relevant sections in Chapter 5 or Chapter 8 should be consulted.
Gui Shao Di Huang tang (Angelica Peonia Rehmannia decoction) and Tao Hong Si Wu tang (Persica Carthamus Four Substances decoction) modified
| Shu Di | 9 g | Rehmanniae Glutinosae Conquitae |
| Shan Yao | 9 g | Dioscorea Oppositae |
| Shan Zhu Yu | 9 g | Fructus Corni Officinalis |
| Dang Gui | 9 g | Radix Angelicae Sinensis |
| Bai Shao | 9 g | Radix Paeoniae Lactiflorae |
| Dan Shen | 9 g | Radix Salviae Miltiorrhizae |
| Mu Dan Pi | 9 g | Cortex Moutan Radicis |
| Fu Ling | 9 g | Sclerotium Poriae Cocos |
| Ze Xie | 9 g | Rhizoma Alismatis |
| Sha Ren | 3 g | Fructus seu Semen Amomi |
| Tu Si Zi | 9 g | Semen Cuscatae |
| Bu Gu Zhi | 6 g | Fructus Psoraleae |
| Xiang Fu | 6 g | Rhizoma Cyperi Rotundi |
| He Huan Pi | 9 g | Cortex Albizziae Julibrissin |
| Tao Ren | 9 g | Semen Persicae |
| Hong Hua | 9 g | Flos Carthami Tinctorii |
| Pu Huang | 9 g | Pollen Typhae |
| Wu Ling Zhi | 9 g | Excrementum Trogopterori |
This formula is an expanded version of Gui Shao Di Huang Tang combined with Tao Hong Si Wu tang (both described in Ch. 4) and other herbs to clear stagnation. The patient preparing for IVF can take this throughout the cycle to reinforce the Kidneys and clear stasis but should she conceive it should be discontinued and a formula to support early pregnancy given (see below).
In the case of endometriosis, formulas described in Chapter 5 should be taken in preparation for IVF (and natural conception avoided). Fibroids should also be addressed before doing IVF if they are large or multiple and affecting the endometrium; these treatments are covered in the Blood stagnation sections of Chapters 4 and 8.
For acupuncture protocols please refer to Tables 4.1–4.7 for general prescriptions, alongside modifications for Blood stasis, Table 4.9.
Phlegm-Damp (and weight loss)
Blockages caused by Phlegm-Damp should be addressed before IVF. Although mucus secretions in the fallopian tubes will be circumnavigated by the IVF process, the presence of Phlegm-Damp in the Uterus does not create a desirable environment for the transferred embryo.
Herbal formula: The formula of choice is:
Gui Shao Di Huang Tang (Angelica Peonia Rehmannia decoction) plus Jian Gu Tang (Strengthen and Consolidate decoction) modified
| Nu Zhen Zi | 9 g | Fructus Ligustri Lucidi |
| Han Lian Cao | 9 g | Herba Ecliptae Prostratae |
| Shan Yao | 9 g | Dioscorea Oppositae |
| Shan Zhu Yu | 9 g | Fructus Corni Officinalis |
| Ji Xue Teng | 9 g | Radix et Caulis Jixueteng |
| Bai Shao | 9 g | Radix Paeoniae Lactiflorae |
| Dan Shen | 9 g | Radix Salviae Miltiorrhizae |
| Mu Dan Pi | 9 g | Cortex Moutan Radicis |
| Fu Ling | 15 g | Sclerotium Poriae Cocos |
| Ze Xie | 9 g | Rhizoma Alismatis |
| Sha Ren | 6 g | Fructus seu Semen Amomi |
| Yi Yi Ren | 15 g | Semen Coicis Lachryma-jobi |
| Dang Shen | 9 g | Radix Codonopsis Pilulosae |
| Bai Zhu | 9 g | Rhizoma Atractylodis Macrocephalae |
| Tu Si Zi | 9 g | Semen Cuscatae |
| Ba Ji Tian | 9 g | Radix Morindae Officinalis |
| Yin Yang Huo | 9 g | Herba Epimedii |
| Zao Jiao Ci | 6 g | Spina Gleditsiae Sinensis |
| Dan Nan Xing | 6 g | Rhizoma Arisaematis |
This simplified approach, which can be used at any time of the menstrual cycle in the weeks before the IVF cycle begins, uses a modified Gui Shao Di Huang tang and combines it with a formula such as Jian Gu Tang (both described in Ch. 4), to strengthen the Kidneys and the Spleen and remove Phlegm-Damp.
Should your patient conceive during this preparation time, then switch formulas to one focusing on early pregnancy support (see below).
During the menstrual period, a formula based on Tao Hong Si Wu tang could be taken (see Ch. 4).
For acupuncture protocols, see Tables 4.1–4.7 for general prescriptions, alongside modifications for Phlegm-Damp accumulation, Table 4.10.
Losing weight
In the case of overweight patients, including patients with PCOS, acupuncture and herbs that aim to clear Damp can be extremely useful. We know that loss of weight and reduction in insulin resistance will improve ovarian function and egg quality. IVF success rates are higher in women with normal range BMIs. Acupuncture and herbs can be used to promote lipolysis, reduce appetite and increase metabolism generally. Weekly acupuncture sessions serve not only to boost Spleen and Stomach function to improve metabolism, but provide a regular checking in point where diet and exercise schedules are monitored and weight is measured. Patients with Phlegm-Damp accumulation can be difficult to motivate so persistence and encouragement is needed. But it is good to remind them that it is the initial mobilizing of Damp that is the crucial step in improving ovarian function. Once the first 10% of body weight is lost, or even 5 kg, ovary function will start to improve and the patient will be more motivated to continue with the treatment and the relevant lifestyle changes. (For more discussion on this topic, see Chs 5 and 12).
Note that it is not only women who need to pay attention to weight. It appears that obesity affects sperm negatively and this is discussed further in Chapters 7 and 12.
At the same time as helping weight loss, Chinese medicine can contribute to an improved environment in which eggs are maturing. Acupuncture using Spleen and Stomach points, which promote clearing of Damp, has been shown to reduce the elevated levels of testosterone and luteinizing hormone in women with PCOS both of which are thought to have a negative impact on egg quality.23 Some IVF specialists use Metformin or Glucophage ‘off-label’ to achieve something similar.
Like improving Kidney function, clearing Phlegm-Damp is not a quick process. However, patients in this category are often younger and have more time to prepare for IVF; 3–6 months is ideal. (See Chs 4 and 5 for more discussion of treatments for Phlegm-Damp Infertility.)
Preparation for IVF for men
It is worthwhile treating male factor infertility even if the couple plan to do IVF with ICSI. If the sperm vitality improves, ICSI may not be necessary. If it improves enough, IVF may not be necessary! (For the treatment of male factor infertility, see Ch. 7.)
Herbal formula: The formula below for reinforcing Kidney Yin, Yang and Jing and nourishing and invigorating Blood and Qi is applicable to any Kidney deficiency male factor infertility and should be taken for some weeks or months before the IVF cycle. It can be taken in small doses by partners of women doing IVF who have no male factor but who would like to maximize sperm quality.
Bu Shen Yi Jing fang (Supplement the Kidneys Benefit the Jing formula) modified
| Tu Si Zi | 9 g | Semen Cuscatae |
| Fu Pen Zi | 12 g | Fructus Rubi Chingii |
| Nu Zhen Zi | 9 g | Fructus Ligustri Lucidi |
| Gou Qi Zi | 9 g | Fructus Lycii Chinensis |
| He Shou Wu | 12 g | Radix Polygoni Multiflori |
| Sheng Di | 9 g | Radix Rehmanniae Glutinosae |
| Shan Zhu Yu | 9 g | Fructus Corni Officinalis |
| Dang Shen | 9 g | Radix Codonopsis Pilulosae |
| Dan Shen | 9 g | Radix Salviae Miltiorrhizae |
| Hong Hua | 6 g | Flos Carthami Tinctorii |
| Huang Qi | 12 g | Radix Astragali |
| Yin Yang Huo | 9 g | Herba Epimedii |
Bu Shen Yi Jing fang was discussed in Chapter 7.
If there are signs of Heat then replace Huang Qi and Yin Yang Huo with Huang Bai (Phellodendri Cortex) 9 g and Zhi Mu (Anemarrhenae Rhizoma) 9 g.
Acupuncture is applicable to male factor infertility and is recommended in the weeks before doing IVF for the same reasons that herbs are recommended, i.e., to maximize the chances of success and the possibility of not requiring ICSI. If the partner of a woman who will be doing IVF has a normal semen analysis but wishes to maximize chances of a good outcome, it is quite reasonable to offer acupuncture treatment based on his constitution and symptoms (if any), combined with points that have been shown in research to improve microcirculation in the testes.24 This is particularly useful if the patient is over 35 and/or has any signs or symptoms of Blood stagnation or Kidney deficiency.
Treatment will be continued for a course of 10 or 12 treatments, or weekly until the sperm donation on the day of OPU. (For further discussion of appropriate treatment where there is male factor infertility, see Ch 7.)
Acupuncture points: Choose from the following (and see Table 11.1):
Table 11.1
Acupuncture points suggested for use with male patients in preparation for IVF
| Treatment goal | Acupuncture points |
| To reinforce Kidney Jing, Yin and Yanga | Ren-4, K-6, K-3, BL-23, BL-52, DU-4 |
| To resolve Blood or Qi stagnationb | ST-30, LIV-5, 8, SP-10, PC-6, BL-32, 33 |
| To clear Damp Heatb | CO-4, CO-11, GB-41, GB-27, LIV-8. |
| To regulate Liver Qi, relieve stressb | LIV-3 CO-4 |
| To reinforce Spleen/Stomach Qia | Ren-6, SP-6, ST-36 |
| To calm shen, relieve insomniaa | HT-7, PC-6, DU-20 |
| To increase blood flow in the testiclesc | ST-29, SP-6 |
cUse electroacupuncture (10 Hz) joining SP-6 to ST-29 on the same side for 5–20 min.
| SP-6 | Sanyinjiao |
| Ren-4 | Guanyuan |
| K-6 | Zhaohai |
| ST-36 | Zusanli |
| ST-29 | Guilai |
| K-3 | Taixi |
| BL-23 | Shenshu |
| BL-52 | Zhishi |
| DU-4 | Mingmen |
| ST-30 | Qichong |
| LIV-5 | Ligou |
| LIV-8 | Ququan |
| SP-10 | Xuehai |
| PC-6 | Neiguan |
| BL-32 | Ciliao |
| BL-33 | Zhongliao |
| CO-4 | Hegu |
| CO-11 | Quchi |
| LIV-3 | Taichong |
| GB-41 | Zu linqi |
| GB-27 | Wushu |
In summary, there are many ways we can use TCM to help couples prepare for IVF, both in terms of useful lifestyle and physiologic changes such as diet and weight loss, and improvements to sleep and stress levels and so on but also, specifically in terms of maximizing egg and sperm quality. Box 11.2 summarizes some of the useful ways (based on early research findings) we can possibly help couples in the months before they embark on IVF.
Treatment During the IVF Cycle
When treating the IVF patient in the TCM clinic, we do exactly what we always do as Chinese medicine doctors, and analyze precisely what we see in front of us from a TCM perspective and administer treatment according to our diagnosis and according to what we have learnt about the treatment of infertility from experts over the centuries of TCM history. Some of what we learned (see Ch. 4) about specifically timed treatments for female functional infertility will still apply in the context of an IVF cycle, however we will need to make some adjustments for altered physiologic conditions and symptoms arising as a result of IVF drugs. This is a new frontier for Chinese medicine doctors, both in the West and also for those in China. We do not yet have the wealth of experience of generations of experts working with IVF patients to guide or inform our approach to treatment. What I present here is a brief summary of programs we have been developing in specialist support clinics set up in Australia for IVF patients. These clinics have seen several thousand patients at the time of writing, with the result that a lot of data has been collected. This sort of information, along with the clinical experience and trials being run by our and other centers will, over time, inform and refine treatment that is appropriate and most advantageous for the patient preparing for, and undertaking IVF. But in terms of TCM, clinical experience is still in its early days, and until such time as more experience and data is available, all the treatment suggestions made below must be seen as just that – considered suggestions.
Chinese medical treatment of internal disorders including infertility, relies on herbal medicine; while this approach may well be comfortable from the Chinese medicine doctor’s point of view, it can be worrying from the IVF specialist’s point of view. There is a concern that there may be unexpected or unfavorable interactions with the IVF drugs. This is a valid concern, since no studies have been done that I am aware of which examine the interaction of Chinese herbs with IVF drugs. Uncontrolled interference with medications can cloud the clinical picture.
If fruit juices like apple, orange, or grapefruit can interact with drug metabolizing enzymes and drug uptake transporters25 then we must assume that herbs may do something similar (although IVF patients are not told to avoid fruit juice, yet!).
Anecdotally, there are Chinese medicine practitioners and IVF specialists in this country who are quite happy to combine the two medicines and apparently with no untoward effect, in fact possibly the opposite. However, these practitioners are in the minority, and at the support clinics we do not prescribe herbs during the drug phase of the IVF cycle (up until egg collection). Until drug interaction studies have been done, most Chinese herbalists should take the cautious approach of advising their patients to stop taking Chinese herbs for a 5–7 day washout period before they begin taking their IVF drugs (the half-life of most aqueous herbal compounds is measured in hours rather than days or weeks, so this timeframe is more than adequate). This applies especially in the case of the agonist and antagonist downregulating drugs. These drugs prevent the pituitary gland producing hormones to stimulate the ovaries, and prescribing herbs that promote reproductive function (Kidney tonics) at the same time is counterintuitive, at least theoretically. Our clinical observations (and those of thousands of gynecologists in China before us) indicate that Kidney Yin herbs have the capacity to promote ovarian activity and increase their estrogen output, e.g., many patients report more regular menstrual cycles, stronger menstrual flow and specifically, increased secretions of cervical mucus when they take these herbs. However, we don’t know the mechanism by which these herbs are achieving this. We can say however, that the use of Kidney tonic herbs to promote ovarian function at the same time as the administration of FSH is at least theoretically, a clinically congruent action.
Additionally, we need to be aware of overall drug load on the liver’s detoxification systems. Women who are getting side-effects like nausea, headaches, rashes or fatigue may be showing signs of an overloaded liver. Adding more substances to the mix may risk exacerbation of these symptoms or worse.
Having made this point loud and clear, I now wish to add that there are circumstances where the addition of Chinese herbs to an IVF cycle appears to be useful and also acceptable. If an IVF patient has completed two or more stimulated cycles, with poor response to the IVF drugs and no or very few embryos produced, then patients and their specialists may well be looking for something else to try. This is often where the Chinese herbalist can step in, with the encouragement of the patient and the blessing of the IVF specialist (or at least a ‘we have nothing to lose’ viewpoint). We hope that treating Kidney deficiency may increase the responsiveness of the ovaries to the drugs (given enough time), and that treating Blood or Qi stagnation may increase implantation rates.
Since downregulating and FSH drugs are given by injection (or by nasal spray), interference of uptake and absorption by herbs taken orally may not be a critical issue, however separate timing of administration of IVF drugs and herbs by 4 h is recommended to reduce possible interactions. Response to the herbs and the drugs should be monitored regularly and doses of herbs reduced if the patient is getting side-effects such as nausea, dizziness, or headaches.
For cycles involving the transfer of frozen embryos, there is no contraindication to the taking of Chinese herbs. Similarly, in artificial insemination cycles where downregulating drugs are not being used, there is no contraindication to the use of Chinese herbs. The use of Chinese herbs with ovulation inducing drugs such as clomifene has been well documented and researched in China and is strongly recommended.
We mustn’t forget however, that preparation with Chinese medicine treatment for ovary health and gamete vitality is best done well before IVF is started (3–9 months). While that opportunity does not always exist, it is important that patients and IVF specialists realize that it is the contribution that can be made before the IVF cycle that is the real place of Chinese medicine.
Of course it goes without saying that concerns about drug interactions do not apply to acupuncture, which can and should continue to be applied according to standard TCM diagnostic and treatment procedures (combined with research-based protocols where appropriate) during the IVF cycle. The use of Kidney channel points with their possible stimulatory action on the pituitary or the ovary during a downregulated phase, is unlikely to adversely impact a pituitary gland that has been switched off pharmaceutically.
The practitioner must have a good understanding of the IVF process and will take into account all clinical symptoms or side-effects arising as a result of the IVF drugs into his/her diagnosis.
4-Phase TCM treatment during the IVF cycle
Treatments according to the 4 Phases we described in Chapter 4 can be modified for use during the IVF cycle. In Chapter 4, when we applied the 4-Phase treatments we maintained a close awareness of the natural physiology of the menstrual cycle and applied treatments that followed these. However, in the case of the IVF patient, we must now be aware of the physiology of the drug manipulated ovary. Rather than enhancing the natural processes of the menstrual cycle as we did in Chapter 4, we must now track and support what are essentially pathologic states as some of the pituitary and hypothalamus activity is shut down and the ovaries are artificially hyper-stimulated.
Suggestions made here for herbal prescriptions to be taken during the IVF cycle (for those patients who have a history of poor response to IVF drugs, as discussed above) follow the requirements of each of the 4 Phases of the menstrual cycle, manipulated as it is. However, in comparison with the complex and many layered approach to treatment of infertility the doctor of TCM takes as primary practitioner, here we take a simpler role as a support practitioner to the IVF specialist.
We need to be clear about what it is exactly that we are supporting in this physiologically artificial and manipulated situation. Essentially, we are assisting the patient emotionally and her ovaries physiologically. Our aims are to:
• support the ovaries (the Kidneys) to promote optimal response to the FSH drugs
• reduce stress and anxiety and bolster the patient’s resilience
Assisting the ovaries as they are induced by non-physiologic doses of FSH to ripen multiple eggs means in TCM terms supporting the Kidneys; this is usually achieved with the use of herbal medicine. This sort of treatment will most often be requested by the ‘poor responder’, as we discussed above. The ovaries of women with depleted Kidney Qi, or those who have done a lot of IVF cycles, tend to respond poorly to stimulation by IVF drugs.
IVF patients who do not need this support (the ‘good responders’ who produce adequate numbers of eggs and younger women) may request Chinese medicine treatment during their IVF cycle to deal with stress, anxiety and side-effects. This is best achieved with acupuncture and administration of herbal medicine is not indicated in these cases.
The guiding prescriptions offered as support for IVF patients who are not good responders and have a history of failed IVF cycles address the immediate situation (namely, ripening of ovarian follicles) as much as the patient with her original infertility diagnosis. Hence, compared with the guiding formulas described in Chapter 4, there are fewer modifications required relating to the original cause of fertility.
Here, we will describe the 4 Phases of the menstrual cycle modified to take into account the effects of the drugs used in an IVF cycle. For women on a long downregulated IVF cycle, drugs will be administered before we actually get to Phase 1 (the menstrual phase) and these GnRH agonist drugs tend to delay the period. At this point, what is required is regulation of Qi and Blood to encourage menstrual flow and to prevent stagnation. Acupuncture to regulate the movement of Qi and Blood is particularly helpful at this time. Additionally, we want to support the Kidneys and their Jing, as they prepare for the demands on them once the stimulating drugs commence. Except in the circumstances described above, herbs are not usually prescribed during this downregulating phase and if your patient has been taking herbs in the preparation phase for IVF, then she will usually be advised to discontinue them before she starts the GnRH agonist.
Once the period arrives, we shall arrange our treatment according to the 4 Phases as described below.
Phase 1 (menstrual period) Day 1–3
Drugs: FSH ± GnRH agonist
You will recall that the main aim of Phase 1 treatment is to encourage an efficient removal and remodeling of the endometrial layers such that the uterine environment is conducive for implantation of an embryo that might arrive later in the cycle.
Acupuncture points: Acupuncture is usefully applied in this phase to promote movement of Qi and Blood – choose from the points below and see Table 11.2:
Table 11.2
Acupuncture pointsa suggested for use during an IVF cycle: menstrual phase
| Treatment goal | Acupuncture points |
| To open the uterus and encourage downward movement and a smooth and thorough discharge of the menstrual flow | CO-4 with SP-6 |
| To moderate this action and hold the Qi | Ren-6 |
| To treat all aspects of the Blood, both its movement and its supplementation and control heavy bleeding if there is Heat | SP-10 |
| To remove obstructions to Blood flow | SP-8 |
| To move Blood in the Chong channel | KI-14 |
| To regulate the Qi in the uterus and moderate the descending action of SP-6 | Tituo |
| To regulate Qi in the lower Jiao | BL-25 and BL-30 |
| To regulate Qi specifically in the Uterus | BL-32, Shiqizhui |
| To regulate Qi, particularly if there is pain in the sacrum | Baliao (BL-31–34) |
| To make Blood flow smoothly, relieve pain, calm the mind | PC-5 |
aUse reducing method on leg and trunk points and even method needling on wrist points.
| CO-4 | Hegu |
| SP-6 | Sanyinjiao |
| SP-10 | Xuehai |
| SP-8 | Diji |
| Ren-6 | Qihai |
| Tituo xue | |
| KI-14 | Siman |
| BL-25 | Dachangshu |
| BL-30 | Baihuangshu |
| BL-32 | Ciliao |
| Shiqizhui | |
| BL-31–34 | Baliao |
| PC-5 | Jianshi |
Herbal formula: In the case of Blood stagnation (clotty or painful periods, or history of endometriosis, etc.), the use of Blood moving herbs should be considered.
Tao Hong Si Wu tang (Persica Carthamus Four Substances decoction) modified (for use during IVF cycle in restricted circumstances – Phase 1)
| Dang Gui | 12 g | Radix Angelicae Sinensis |
| Bai Shao | 9 g | Radix Paeoniae Lactiflorae |
| Chuan Xiong | 6 g | Radix Ligustici Wallichii |
| Tao Ren | 6 g | Semen Persicae |
| Hong Hua | 9 g | Flos Carthami Tinctorii |
| Yi Mu Cao | 9 g | Herba Leonuri Heterophylli |
| Xiang Fu | 12 g | Rhizoma Cyperi Rotundi |
| Ji Xue Teng | 12 g | Radix et Caulis Jixueteng |
| Shan Zha | 6 g | Fructus Crataegi |
| Dan Shen | 12 g | Radix Salviae Miltiorrhizae |
| Chuan Niu Xi | 6 g | Radix Cyathulae |
Tao Hong Si Wu Tang is the ideal basis for a formula applied during the period at the start of an IVF cycle because it has a gentle but firm action on the movement of blood and at the same time builds up Blood, i.e., it helps replace blood at same time it is being lost through menstruation. It is augmented with herbs such as Yi Mu Cao and Chuan Niu Xi to encourage a thorough shedding of the lining and Dan Shen and Shan Zha to facilitate this movement. The addition of Qi regulators such as Xiang Fu, promotes the action of Qi leading the Blood and ameliorates cramping of the uterus.
In the case of Blood stagnation (clotty or painful periods, or history of endometriosis, etc.), the use of stronger blood moving herbs (Yan Hu Suo, Wu Ling Zhi, Pu Huang) should be considered. FSH drugs are commenced during this phase, usually on Day 2. Support of follicle stimulation, with herbs or acupuncture, will begin in the next phase however.
Phase 2 (follicle development) Day 4 to approx. Day 11
Drugs: FSH ± GnRH agonist or antagonist
FSH drugs stimulate the ovaries to ripen a number of eggs from the available cohort of recruits. Because the agonist drug (or the antagonist drug introduced on about Day 6 of stimulation) will stop the pituitary from responding to the rising levels of estrogen and triggering ovulation, many follicles continue to develop unhindered.
The process of folliculogenesis, as you will remember from Chapter 2, relies on Kidney Yin and Blood and draws on Kidney Jing stores. During an IVF cycle, the growth of more follicles than usual means there will be a larger draw on these resources than in a natural cycle and hence, greater Kidney support may be required. The rise in Yin and Blood and the effect of the FSH drugs (and the herbs if they are used) will be measured in the rise of estrogen and in the growth of the follicles seen on ultrasound. This will happen more rapidly for some patients than for others. In an ideal case this phase of follicle stimulation will last approximately 7 or 8 days, during which time several follicles ripen steadily at about the same rate to reach 13 or 14 mm, and at the same time, the uterine lining gradually thickens. It is common to feel the Kidney pulse fill out during this and the next phase as the follicles grow. If there are side-effects from the drugs and the process of hyperstimulating the ovaries, it may also be felt on the Liver pulse (which may become tight and wiry) and Spleen pulse (which may become weak).
In some cases, the ultrasounds may show that after several days of FSH injections, the follicles are not growing as expected or that there are few of them. The IVF specialist will usually increase the dose of FSH in this case, and the projected date for egg collection might be delayed. On the other hand, sometimes follicles develop more rapidly than expected and are ready for collection after only a few days of stimulation. Neither the slow nor the rapid growing follicles represent an ideal situation and it is preferable that follicles ripen in a time frame similar to a natural cycle (i.e., over about 2 weeks).
Acupuncture: Acupuncture at this point supports the Kidneys and the Blood and regulates the function of the Ren and Chong vessels (such as it is). Maintaining Chong vessel function as much as possible and promoting unfettered movement of Liver Qi in the abdomen, may help the regular and ordered growth of the recruited follicles so that they grow at a similar rate. This increases the possibility of collecting more eggs at the correct stage of maturity on the day of egg collection.
Moving the Liver and Heart Qi helps relieve stress and calm the emotions and since we know that women who feel more stressed during IVF procedures (measured by raised heart beat and high systolic blood pressure) have significantly lower implantation rates it is important to continue treatment at this time.26 Some side-effects such as headaches may be apparent, however the physiological pressure and abdomen discomfort caused by enlarged ovaries does not usually come into play until late in this phase or in the next.
It is useful to incorporate some of the research based protocols (described below) which increase blood flow to the ovaries and uterus. This will aid in getting maximal delivery of nutrients, oxygen and drugs to the follicles as they are developing, and in promoting the development of lining of the uterus as the Blood in the Chong channel increases.
In the case that estrogen levels are slow to rise and follicles are slow to grow then increasing blood flow to the ovaries with acupuncture may facilitate drug delivery to stimulate follicle growth. Likewise, in the case that the endometrium is thin, using acupuncture points which improve blood flow to the uterus may be helpful.
Acupuncture points: Choose from the list below (and see Table 11.3):
Table 11.3
Acupuncture pointsa suggested for use during an IVF cycle: stimulation phase
| Treatment goal | Acupuncture points |
| To regulate Ren and Chong vessels | Ren-7, KI-5, KI-8, KI-13 |
| To encourage Blood production (build endometrium) | ST-36, LIV-3, BL-17, BL-20, SP-10 |
| To support Kidney Yin and Jing | KI-3, KI-5, KI-6, SP-6, BL-23, Ren-4, ST-27 |
| To increase Blood flow to the uterusb | BL-28, BL-23, SP-6, BL-57, SP-4, PC-6, ST-30 |
| To increase Blood flow to the ovariesb | ST-28, ST-29, SP-6, SP-9 |
| To regulate Qi around the ovaries | ST-28, ST-29, Zigong, LIV-5, LIV-8 |
| To stabilize Shen | Yin Tang, HT-7, HT-4, Ren-14 |
| To treat headaches, depression, irritability | CO-4, LIV-3, YT, GB-20, DU-20 |
aUse even method needling. Acupuncture applied twice a week (or more) is recommended during this phase.
bUse electroacupuncture (10 Hz) linking abdomen or lower back points to Spleen points on the lower leg.
| Ren-7 | Yinjiao |
| KI-5 | Shuiquan |
| KI-8 | Jiaoxin |
| KI-13 | Qixue |
| KI-3 | Taixi |
| KI-6 | Zhaohai |
| SP-6 | Sanyinjiao |
| ST-36 | Zusanli |
| Ren-4 | Guanyuan |
| BL-23 | Shenshu |
| ST-27 | Daju |
| BL-28 | Pangguanshu |
| BL-57 | Chengshan |
| SP-4 | Gongsun |
| PC-6 | Neiguan |
| ST-30 | Qichong |
| ST-28 | Shuidao |
| ST-29 | Guilai |
| SP-9 | Yinlingquan |
| SP-6 | Sanyinjiao |
| SP-10 | Xuehai |
| Zigong | |
| LIV-3 | Taichong |
| LIV-5 | Ligou |
| LIV-8 | Ququan |
| Yin Tang | |
| HT-7 | Shenmen |
| HT-4 | Lingdao |
| Ren-14 | Juque |
| CO-4 | Hegu |
| GB-20 | Fengchi |
| DU-20 | Baihui |
Herbal formula: If a considered decision has been made to prescribe herbs during an IVF cycle for a patient with previous poor response, then those that reinforce Kidney Jing, Yin and Blood will be required.
Gui Shao Di Huang tang (Angelica Peonia Rehmannia decoction) modified
| Shu Di | 12 g | Radix Rehmanniae Glutinosae Conquitae |
| Shan Zhu Yu | 9 g | Fructus Corni Officinalis |
| Shan Yao | 9 g | Radix Dioscorea Oppositae |
| Dang Gui | 9 g | Radix Angelicae Sinensis |
| Bai Shao | 9 g | Radix Paeoniae Lactiflorae |
| Dan Shen | 9 g | Radix Salviae Miltiorrhizae |
| Ji Xue Teng | 9 g | Radix et Caulis Jixueteng |
| Mu Dan Pi | 9 g | Cortex Moutan Radicis |
| Fu Ling | 9 g | Sclerotium Poriae Cocos |
| Ze Xie | 6 g | Rhizoma Alismatis |
| Sha Ren | 6 g | Fructus seu Semen Amomi |
| Tu Si Zi | 9 g | Semen Cuscatae |
| Bu Gu Zhi | 6 g | Fructus Psoraleae |
| Xiang Fu | 9 g | Rhizoma Cyperi Rotundi |
| Wu Yao | 3 g | Radix Linderae Strychnifoliae |
| Yin Yang Huo | 6 g | Herba Epimedii |
| Lu Jiao Pian | 6 g | Cornu Cervi Parvum |
| Zi Shi Ying | 6 g | Fluoritum |
| He Huan Pi | 12 g | Cortex Albizziae Julibrissin |
| Suan Zao Ren | 9 g | Semen Ziziphi Spinosae |
We use this expanded version of Gui Shao Di Huang tang (described in Ch. 4) to support Kidney Jing, Yin, and Yang to promote follicle growth. As well as encouraging follicle development we want to protect the Kidneys from being drained by the artificial stimulation by external FSH.
The Blood tonic herbs nourish and promote circulation of blood to promote endometrial growth, and Qi regulating herbs prevent Qi stagnation occurring as the ovaries swell.
Herbs that calm the mind are added in recognition of the emotional stress associated with infertility in general and doing IVF in particular. Previously, we used mind calming herbs in Phase 2 formulas (see Ch. 4) for another reason. In a natural conception cycle, a stable Shen is important to ensure Bao vessel function and follicle growth. In the case of the IVF patient, this is no longer so relevant since the FSH stimulation of the follicles comes from an injection rather than from the pituitary gland, hence this aspect of Bao vessel function is supplanted. Some Kidney Yang herbs are added in recognition of the fact that a ‘poor responder’ likely has deficiencies of Kidney Yin and Yang, and that the eggs will be (hopefully) steadily maturing under the influence of the FSH drugs (reaching the more Yang phase of their development).
Phase 3 (approx. Day 11–14, follicle maturation, trigger injection + egg collection)
Drugs: FSH + GnRH agonist or antagonist + hCG trigger
By Phase 3, the phase in which ovulation occurs in a natural menstrual cycle, physiological events take an even larger departure from normal. The ovaries are by now in quite an unnatural state. The FSH drugs continue to stimulate the ovaries and the follicles will reach their maximal size in this phase, however they are inhibited from releasing eggs by the action of the agonist or antagonist drugs. Once the eggs reach the appropriate size (around 20 mm), the trigger injection will be given. This finalizes the last stages of maturation and loosens the eggs from their follicle housing so they can be flushed out. In a natural cycle Phase 3 spans the days leading up to ovulation and the events immediately afterwards. In the IVF cycle Phase 3 continues only up until the day of egg collection.
This is a more intense time of the IVF cycle as the moment for egg collection approaches. Ultrasounds and blood tests are often done more frequently at this juncture so as to determine the best time for collection. Stress and anxiety relating to the results of these tests and the number and size of the follicles often builds at this time. The crucial nature of the timing of the hCG trigger injection (administered exactly 36 h before the egg collection) adds to the anxiety for some.
Acupuncture: Acupuncture is very useful at this point to address side-effects that may be worrying the patient. Most commonly, these are related to Liver Qi stagnation. There are several reasons that the Liver may be strained or overworked. First, there is the profound disruption to a natural physiologic cycle that is overseen by the Liver. By this stage of the IVF cycle, the ovaries may be swelling in the abdomen and obstructing Liver Qi and there will be unusually large amounts of estrogen taxing the liver’s enzymes in addition to metabolism of the IVF drugs. Headaches, abdomen distension and pain, irritability and nausea are indications that the Liver Qi needs treatment.
Insomnia and anxiety are signs that the Heart Qi and the Shen need attention.
Dizziness is a less common symptom but may indicate Liver wind. Research-based acupuncture protocols which increase blood flow to reproductive organs can be continued in this phase.
It is in Phase 3 that warning signs of excessive hyperstimulation may appear (high blood estrogen levels or large numbers of follicles on ultrasound or severe abdomen distension), and the practitioner should be aware of these and take timely action. Treatment will be largely symptomatic at this stage, based primarily on regulating Liver Qi in the abdomen. (We discuss treatment of ovarian hyperstimulation syndrome below). The points chosen in the days before egg collection will be similar to those Phase 3 points described in Chapter 4. However, while the integrity and activity of the fallopian tubes were of prime concern there, in this case they are irrelevant.
Acupuncture points: Choose from the points below (and see Table 11.4):
Table 11.4
Acupuncture pointsa suggested for use during an IVF cycle: trigger injection and egg collection phase
| Treatment goal | Acupuncture points |
| To support Kidneys and promote growth of the follicles/eggs (days before trigger injection) | Ren-4, KI-6, KI-13, K-14 |
| To boost Kidney Yang and promote final maturation of follicles/eggs (day of trigger injection) | KI-5, KI-8, Zigong, SP-6 |
| To enhance Kidney function and stabilize emotions | KI-4 |
| To regulate Qi, relieve abdomen distension (lower), promote circulation to ovaries | Ren-6, ST-28, ST-29, SP-6, LIV-5, SP-13, Ah Shi points |
| To regulate Qi, relieve abdomen distension (upper) | GB-34, Ren-12, LIV-5, LIV-8, REN-9 |
| To regulate Liver Qi, relieve irritability, depression or headaches | LIV-3, CO-4 |
| To calm Liver wind, relieve dizziness | LIV-8, CO-11 |
| To clear Heat, relieve rashes | SP-10, CO-11 |
| To regulate the Heart Qi, calm the mind, relieve insomnia | PC-4, 5 or 6, HE-5, 7, Yintang |
aUse local and leg points with reducing method and even method with wrist points. The choice of abdomen or back points can be guided by sensations or pain.
| Ren-4 | Guanyuan |
| KI-6 | Zhaohai |
| KI-13 | Qixue |
| K-14 | Siman |
| SP-13 | Fushe |
| KI-5 | Shuiquan |
| KI-8 | Jiaoxin |
| Zigong | |
| SP-6 | Sanyinjiao |
| KI-4 | Dazhong |
| Ren-6 | Qihai |
| ST-28 | Shuidao |
| ST-29 | Guilai |
| SP-6 | Sanyinjiao |
| LIV-5 | Ligou |
| LIV-8 | Ququan |
| GB-34 | Yanglingquan |
| Ren-12 | Zhongwan |
| Ren-9 | Shuifen |
| PC-4 | Ximen |
| PC-6 | Neiguan |
| HE-5 | Tongli |
| HE-7 | Shenmen |
| Yintang |
Herbal formula: Just as the information from the blood tests and ultrasounds lets the IVF specialist know when to administer the trigger injection, this information will also let you know when you need to change the formula (in the case that you and the IVF doctor have made a decision to include herbs). It is when the follicles are measuring around 12–14 mm (i.e., they are approx 3–4 days from maturity) that you should prescribe a formula that continues to support Kidney Yin but will now contain more Kidney Yang tonic herbs in higher doses than before. This is to provide a final boost to the energy making capacity of the eggs before they are harvested.
In some women, as the ovaries swell with multiple follicles, abdominal discomfort increases as does distension. Thus the Phase 3 formulas will contain more herbs that regulate Qi to alleviate distension. Promoting Liver Qi movement also enables your patient to deal with stress.
Blood moving herbs with blood thinning qualities, such as those found in Phase 3 formulas in Chapter 4, are not included in this formula because of the impending surgical procedure. For the same reason, the patient will be advised to stop the formula altogether before the trigger injection, i.e., approx. 48 h before the egg collection procedure. Thus, this formula is for short use only, 2–3 days. Because we are not relying on correct functioning of the Bao Vessel for ovulation, we do not need to emphasize herbs to stabilize the Shen in the same way we did when we prescribed treatment in Phase 3 of a natural cycle. Similarly, we do not need to be concerned with the free movement of the fallopian tubes or the production of cervical mucus.
Bu Shen Cu Pai Luan is a Phase 3 formula used to support Kidney Yin and boost Kidney Yang while regulating the Qi to prepare for ovulation.
Bu Shen Cu Pai Luan Tang (Reinforce Kidney and Ovulation formula) modified
| Bai Shao | 9 g | Radix Paeoniae Lactiflorae |
| Nu Zhen Zi | 9 g | Fructus Ligustri Lucidi |
| Shan Yao | 9 g | Dioscorea Oppositae |
| Shan Zhu Yu | 9 g | Fructus Corni Officinalis |
| Tu Si Zi | 12 g | Semen Cuscatae |
| Bu Gu Zhi | 6 g | Fructus Psoraleae |
| Rou Cong Rong | 9 g | Herba Cistanches |
| Suo Yang | 6 g | Herba Cynomorii Songarici |
| He Huan Pi | 9 g | Cortex Albizziae Julibrissin |
| Xiang Fu Cu | 12 g | Rhizoma Cyperi Rotundi |
| Qing Pi | 3 g | Pericarpium Citri Reticulatae Viride |
| Ju He | 3 g | Semen Citri Reticulatae |
| Li Zhe He | 3 g | Semen Litchi |
| Wu Yao | 3 g | Radix Linderae Strychnifoliae |
This variation of Bu Shen Cu Pai Luan (described in Ch. 4) incorporates the Kidney Yang tonics that boost ATP production which we discussed above, and we hope will confer an enhanced energy making capacity to the eggs and hence to the embryo. These are combined with a strong Qi regulating element (the last five herbs listed, above), to emphasize circulation of Qi around the ovaries as they enlarge with a number of swollen follicles.
Phase 3 ends with egg collection. The patient is usually advised to rest for the rest of the day, because of the invasiveness of the procedure (with or without general anesthetic) and the possible physical trauma, but to consider returning for acupuncture in the days following.
The male partner’s role
The spotlight has been on the ovaries and follicles, but it is at this moment that the sperm need to play their part.
As far as the male partner is concerned, we know that improving sperm motility and morphology can takes several weeks but, even in the short term, sperm vitality can be influenced. Electroacupuncture (and in some cases moxa) applied to the lower abdomen just before sperm donation, may help not only ‘performance’ and ‘stage fright’ but also galvanize the sperm for their task in the Petri dish.
Acupuncture points: Choose from the points below (and see Table 11.5):
Table 11.5
Acupuncture pointsa suggested for use during an IVF cycle: male partner on day of sperm donation
| Treatment goal | Acupuncture points |
| Reinforce K Qi | Ren-4b K-3, K-6, LU-7 |
| Fortify Yang | Ren-4 and 6 with moxa (if there is Cold), DU-20 |
| Reinforce and regulate Qi and Blood supply | ST-29c, SP-6, SP-10, LIV-5, 8, PC-6 |
| Reduce anxiety | YT, LIV-3, CO-4 (20 min only) |
| Clear Damp in Lower Jiao, if necessary | GB-41, TH-5 |
aUse local and leg points with mild reducing method and even method with wrist points.
bUse deep but gentle needling with deqi traveling downwards.
c5 or 10 min of electroacupuncture (10 Hz) joining ST-29 to SP-6 on the same side.
| K-3 | Taixi |
| K-6 | Zhaohai |
| LU-7 | Lieque |
| Ren-4 | Guanyuan |
| Ren-6 | Qihai |
| DU-20 | Baihui |
| ST-29 | Guilai |
| SP-6 | Sanyinjiao |
| SP-10 | Xuehai |
| LIV-5 | Ligou |
| LIV-8 | Ququan |
| PC-6 | Neiguan |
| Yin Tang | |
| LIV-3 | Taichong |
| CO-4 | Hegu |
| GB-41 | Zu linqi |
| TH-5 | Weiguan |
Phase 4a (Day 14–Day 16/19, from egg collection to embryo transfer)
Drugs: progesterone support (pessaries, injections, gel) or HCG injections
Phase 4 in a natural cycle begins a few days after ovulation. For treatment of the IVF patient, we have divided Phase 4 into two parts, the first part spanning the days immediately after egg collection up until the embryo transfer (this may be anywhere between 2 and 5 days, during which time the embryo is in the incubator); and the second part from the day after the transfer of the embryo and up to the pregnancy test or the period.
Acupuncture – after egg collection
Acupuncture administered in the 2–3 days after egg collection aims at restoring normal Qi and blood flow in the channels through the reproductive organs, settling any tissue trauma, reducing effects of internal bleeding, reducing swelling of the ovaries and promoting circulation in the lining of the uterus. We do this by clearing Blood stasis, re-establishing Chong and Ren function, regulating Liver Qi and supporting Kidney function, especially Kidney Yang. By so doing, we aim to create favorable implantation conditions.
Additionally, help with managing stress is usually required. This is a nerve-racking time as your patient waits to hear whether her eggs have fertilized, and then whether the embryo(s) are developing. IVF clinics will usually report the total number of embryos on the day after fertilization and then will leave them undisturbed until the 3rd day, in incubator conditions that mimic as closely as possible the environment of the fallopian tube. If a reasonable number of embryos have survived at this point, the embryologist will suggest leaving them for another 2 days until they reach blastocyst stage.
Herbal formula: Now that the eggs are collected and the downregulating drugs are no longer required, drug–herb interactions are of less concern, and IVF patients can feel comfortable with taking herbs if they so wish, whether or not they have taken them at other times of their IVF cycle. There is no known or theoretical contraindication to using Chinese herbs at the same time as the exogenous progesterone (or hCG) that is administered at this phase.
Table 11.6
Acupuncture pointsa suggested for use during an IVF cycle: Phase 4a, after egg collection
| Treatment goal | Acupuncture points |
| To regulate Qi and Blood in the Ren and Chong channels | Ren-7, Ren-3, K-14, PC-6, SP-4 |
| To regulate Liver Qi, reduce swelling, alleviate pain | LIV-5, LIV-4, GB-34, GB-27 or Ah Shi points on the abdomen |
| To regulate Blood, clear Blood stasis, promote circulation to the endometrium | SP-10, SP-8, ST-29, ST-30, BL-57, BL-32 |
| To boost Kidney Yang | Ren-4, Ren-6, K-13, K-6, K-3, BL-23 |
| To calm the Shen | HT-7, YT, DU-20 |
aUse local and leg points with mild reducing method and even method with wrist and head points.
Herbs to prepare the uterus for implantation are now prescribed. We combine some of the principles of treatment from Phase 3 with Phase 4 treatment principles.
This formula can be commenced after egg collection on the same day and will be continued for 6 or 7 days until the time the embryo implants – in other words, until a day or two after the transfer of a blastocyst, or 3–4 days after the transfer of a Day 3 embryo. Our treatment is focused on removing any stasis resulting from internal bleeding after the surgical removal of the eggs, and preparing the endometrium which may have been adversely affected by the drugs and hormone levels of the stimulation phase. Stability of the Shen and the Bao vessel is important in Phase 4a and 4b to keep the uterus closed.
We modify the same formula Bu Shen Cu Pai Luan, with herbs to regulate the Blood as well as the Qi.
Bu Shen Cu Pai Luan (Reinforce Kidney Ovulation formula) modified
| Dang Gui | 9 g | Radix Angelicae Sinensis |
| Chi Shao | 6 g | Radix Paeoniae Rubra |
| Bai Shao | 6 g | Radix Paeoniae Lactiflorae |
| Hong Hua | 3 g | Flos Carthami Tinctorii |
| Ji Xue Teng | 9 g | Radix et Caulis Jixueteng |
| San Qi | 3 g | Radix Pseudoginseng |
| Shan Yao | 6 g | Dioscorea Oppositae |
| Shu Di | 6 g | Rehmanniae Glutinosae Conquitae |
| Nu Zhen Zi | 6 g | Fructus Ligustri Lucidi |
| Mu Dan Pi | 6 g | Cortex Moutan Radicis |
| Fu Ling | 6 g | Sclerotium Poriae Cocos |
| Tu Si Zi | 12 g | Semen Cuscatae |
| Xu Duan | 12 g | Radix Dipsaci |
| Zi Shi Ying | 6 g | Fluoritum |
| He Huan Pi | 9 g | Cortex Albizziae Julibrissin |
| Xiang Fu | 9 g | Rhizoma Cyperi Rotundi |
Bu Shen Cu Pai Luan (described in Ch. 4) is modified here with herbs which clear Blood stasis and maintain Shen stability. Support Kidney Yin and Yang, clear blood stasis, calm the mind.
To the original Bu Shen Cu Pai Luan, we add Ji Xue Teng to gently encourage Blood circulation in the endometrium, which alongside the Kidney Yin and Yang support we hope will create an optimal environment conducive to implantation. San Qi is added to address any internal bleeding from the egg collection procedure.
Acupuncture – the day of embryo transfer
Acupuncture is often performed on the day of embryo transfer. If the embryo transferred is a blastocyst, it is anticipated that implantation will happen within the following day or 2. If the embryo was transferred at 3 days, then implantation will occur in the following few days. Implantation is a complex event. Subtle changes in immune factors, up or downregulation of implantation factors, blood supply, hormone levels and so on, can all influence the delicate interaction of uterus and embryo. Equally, subtle external influences may exert an effect on implantation – like laughing, or being hypnotized, or having acupuncture. Such influences increase the endorphin level, or decrease the cortisol level or change certain cytokines levels or any number of other subtle biochemical or physiological changes about which we still know very little. Acupuncture points are chosen for their ability to support Kidneys and regulate local Qi and Blood flow with the aim of creating favorable implantation conditions. It may well be the fact that some of these points will reduce factors that hinder implantation, such as uterine contractions or autoimmune or clotting factors but at this stage, the mechanism of acupuncture’s action at the time of implantation has not been elucidated. We will discuss the clinical trials that look at the effect of acupuncture or other interventions on the day of embryo transfer below. Most of these clinical trials have applied acupuncture both before and after the transfer on the same day. The trials that applied acupuncture stimulation only after the transfer, or on the day before the transfer, claim to achieve similar results. Thus, the acupuncture schedule you choose may be dictated by factors such as time and convenience, as much as clinical trial results. Most of the trials used the same acupuncture prescription with little or no variation (see below).
Acupuncture points: Choose from the points below (and see Table 11.7):
Table 11.7
Acupuncture pointsa suggested for use during an IVF cycle: Phase 4a, at embryo transfer
| Treatment goal | Acupuncture points |
| To regulate Liver Qi, reduce uterine cramping | LIV-3, GB-34, CO-4 |
| To regulate Blood, clear stasis, promote circulation to the endometrium | SP-10, SP-8, ST-29 |
| To promote production of Blood and Qi | ST-36, SP-6 |
| To boost Kidney Yang | Ren-4, Ren-6, K-6, K-3 |
| To regulate the activity of the Chong and Ren vessels | Ren-7 |
| To calm the Shen | HT-7, PC-6, YT, DU-20 |
aUse local and leg points with mild reducing method and even method with wrist points. Abdomen points are used only in the treatments before the embryo transfer.
| LIV-3 | Taichong |
| GB-34 | Yanglingquan |
| CO-4 | Hegu |
| SP-10 | Xuehai |
| SP-8 | Diji |
| ST-29 | Guilai |
| ST-36 | Zusanli |
| SP-6 | Sanyinjiao |
| Ren-4 | Guanyuan |
| Ren-6 | Qihai |
| K-6 | Zhaohai |
| K-3 | Taixi |
| Ren-7 | Yinjiao |
| HT-7 | Shenmen |
| PC-6 | Neiguan |
| Yin Tang | |
| DU-20 | Baihui |
Phase 4b (from day after embryo transfer until pregnancy test or period, implantation)
Drugs: progesterone pessaries, injections or gel or hCG injections
Implantation and development of the early placenta occurs in this phase. We support this process with treatment that reinforces Kidney, Spleen, and the Blood. Some IVF patients describe this waiting period as the most difficult time of the whole cycle. Now that there is no longer attention from the nurses, doctors, and radiographers, the support of the acupuncturist plays an important role.
Acupuncture points: Choose from the points below (and see Table 11.8):
Table 11.8
Acupuncture pointsa suggested for use during an IVF cycle: Phase 4b, between embryo transfer and pregnancy test
| Treatment goal | Acupuncture points |
| To boost Kidney Yang | K-6, K-5 |
| To regulate Liver Qi, reduce uterine cramping | GB-34, LIV-3, LIV-4, LIV-5, LIV-9, LIV-11 |
| To regulate Blood in the Liver, Kidney and Ren channels and address Liver Blood deficiency | LIV-8, LIV-3, KI-5 |
| To invigorate the Spleen and Stomach and promote production of Blood and Qi | ST-36, BL-17, BL-20, BL-21 |
| To calm the Shen, safeguard the Bao Luo vessel | YT, DU-20, Ren-15, HE-5, HE-7, K-9 |
| To relieve stress and regulate Liver Qi in the upper body | LIV-5, PC-6, PC-7, PC-5 |
aUse local and leg points with mild reducing method and even method with wrist points. Avoid abdomen and lower back points.
| Yin tang | |
| DU-20 | Baihui |
| Ren-15 | Jiuwei |
| HE-5 | Tongli |
| HE-7 | Shenmen |
| GB-34 | Yanglingquan |
| LIV-3 | Taichong |
| LIV-4 | Zhongfeng |
| LIV-5 | Ligou |
| LIV-9 | Yinbiao |
| LIV-11 | Yinlian |
| LIV-8 | Ququan |
| KI-5 | Shuiquan |
| ST-36 | Zusanlin |
| BL-17 | Geshu |
| BL-20 | Pishu |
| K-9 | Zhubin |
| K-6 | Zhaohai |
| KI-5 | Shuiquan |
| PC-6 | Neiguan |
| PC-7 | Daling |
| PC-5 | Jianshi |
Herbal formula: From this point, we focus on nourishing Kidney Yin and Yang, with the aim of supporting the secretory function of the endometrium and the implantation of the embryo. Kidney Yang herbs have been observed to increase progesterone levels and may be useful in supporting the action of hCG injections, which are given to promote corpus luteum function at this stage or supplementing any exogenous progesterone. Adequate progesterone levels are important to maintain endometrium function and support early pregnancy. There is no danger in having too much progesterone. Nourishing Blood supports nutrition to the endometrium, as does the use of Spleen Qi tonics. Herbs which regulate Qi in the abdomen ameliorate the cramping symptoms that the supplemental progesterone can cause.
You Gui Wan (Restore the Right Kidney pill) plus Yu Lin Zhu (Fertility Pearls) modified
| Bai Zhu | 12 g | Rhizoma Atractylodis Macrocephalae |
| Fu Ling | 9 g | Sclerotium Poriae Cocos |
| Dang Gui | 9 g | Radix Angelicae Sinensis |
| Bai Shao | 9 g | Radix Paeoniae Lactiflorae |
| Shu Di | 9 g | Radix Rehmanniae Glutinosae Conquitae |
| Shan Zhu Yu | 9 g | Fructus Corni Officinalis |
| Shan Yao | 9 g | Dioscorea Oppositae |
| Tu Si Zi | 12 g | Semen Cuscatae |
| Xu Duan | 12 g | Radix Dipsaci |
| Du Zhong | 6 g | Cortex Eucommiae Ulmoidis |
| Ba Ji Tian | 9 g | Radix Morindae Officinalis |
| Xiang Fu | 9 g | Rhizoma Cyperi Rotundi |
| Gan Cao | 3 g | Radix Glycyrrhizae Uralensis |
Yu Lin Zhu and You Gui Wan are formulas we discussed in Chapter 4. This combination reinforces Kidney Yin and warms Kidney Yang, nourishes Blood, supports Spleen and regulates Qi.
If there are immune factors which may be implicated in impaired implantation, then consider adding Huang Qi in a large dose (20 g). For clotting factors, we might consider Dan Shen in a small dose, however most patients diagnosed with clotting factors will be taking low molecular weight heparin, and the addition of extra blood thinning agents will not be necessary.
Ovarian Hyper-Stimulation Syndrome
The main symptoms of ovarian hyper-stimulation syndrome (OHSS) usually manifest in Phase 4, although warning signs can occur as early as Phase 2 during stimulation of the follicles. Such a disturbance of water metabolism is more likely to occur in patients with Kidney deficiency, and secondarily in those with Spleen (and Lung) deficiency and stagnation of Qi and Blood.
Kidneys, Spleen, and Lungs are responsible for fluid movement in the upper, middle and lower Jiao, respectively.
Moderate or severe OHSS itself is an acute and excess condition and our first priority is to mobilize fluids then to support Kidney, Spleen (and Lungs). Qi and Blood stagnation may also need to be addressed. Herbal treatment focuses on regulating water metabolism in the body by using diuretic herbs and promoting Kidney Yang and Spleen Qi.
Herbal formula: The Phase 4b formula (You Gui wan plus Yu Lin Zhu modified) can be further modified to correct water metabolism with the addition of:
| Huang Qi | 20–30 g | Radix Astragali |
| Zhu Ling | 15 g | Polyporus |
| Ze Xie | 15 g | Rhizoma Alismatis |
and increasing Fu Ling (Poria) to 15 g.
If there is marked stasis, and embryo transfer has been postponed for another time,
Dan Shen (Radix Salviae Miltiorrhizae) 15–20 g, can be added.
Acupuncture points: Choose from the points below (and see Table 11.9):
| Ren-9 | Shuifen |
| Ren-5 | Shimen |
| ST-28 | Shuidao |
| K-5 | Shuiquan |
| SP-9 | Yinlingquan |
| BL-22 | Sanjiaoshu |
| BL-28 | Pangguanshu |
| SJ-10 | Tianjing |
| LIV-4 | Zhongfeng |
| CO-6 | Pianli |
| K-14 | Siman |
| BL-32 | Ciliao |
| GB-26 | Daimai |
| GB-27 | Wushu |
| GB-28 | Weidao |
| Ren-17 | Shanzhong |
| LU-7 | Lieque |
| LU-1 | Zhongfu |
Table 11.9
Acupuncture pointsa suggested for use during an IVF cycle: Phase 4, OHSS
| Treatment goal | Acupuncture points |
| To regulate water passages and alleviate pain and distension of abdomen | Ren-9, Ren-5, ST-28, K-5, SP-9 |
| To promote removal of fluids via the bladder | BL-22, BL-28 |
| To descend rebellion, alleviate shortness of breath, ascites | SJ-10, LIV-4, CO-6, Ren-17 |
| To resolve accumulations and swelling via the Dai Channel | GB-26, GB-27, GB-28 |
| To regulate Qi and Blood, clear stasis | K-14, BL-32 |
| To regulate water passages and descend Lung Qi | LU-7, LU-1 |
| To regulate water passages and benefit Kidney | K-7 |
Treatment should be applied twice a week or in more severe cases every 2nd day or daily.
aUse points with reducing method. Needle abdomen points very shallowly.
The Positive Pregnancy Test
A pregnancy achieved after a period of (female) subfertility needs careful nurturing in the first few weeks. This patient’s risk of miscarriage is raised compared to women with no history of fertility difficulties.
Acupuncture once a week is recommended. The idea behind our treatments at this stage is to support the Kidney Qi and to stabilize the Bao vessel and Bao channel so that the uterus remains closed.
Some research has indicated that just the act of monitoring early pregnancy seems to help reduce miscarriage rates in women with a history of pregnancy loss,27 and many IVF clinics offer similar services now, with weekly blood tests and/or ultrasounds. The rising hCG in the blood tests or the growing fetus on the ultrasound provides confirmation that helps to settle the Shen and stabilize the Bao Mai.
In the acupuncture clinic, we can offer something similar in the way of reassurance of a healthy pulse picture (a strong gliding quality on the Kidney position is ideal, although it is not every viable pregnancy that shows this in the early days). But we can do something more. Using herbs and acupuncture points to support Kidney and Spleen Qi will support endometrial function and nourishment of the developing fetus. By using herbs and points which calm the Shen, we shall be ensuring the Bao Mai is stable and the uterus remains closed.
Acupuncture points: Choose from the points below (and see Table 11.10):
| Yin Tang | |
| DU-20 | Baihui |
| PC-6 | Neiguan |
| K-9 | Zhubin |
| K-6 | Zhaohai |
| ST-36 | Zusanli |
| HT-7 | Shenmen |
| LIV-3 | Taichong |
| GB-34 | Yanglingquan |
| K-4 | Dazhong |
Herbal formula: There is some evidence from clinical trials to show that using Chinese herbs to support the Kidneys and the Spleen in the early part of pregnancy, reduces miscarriage rates after IVF cycles.28
Table 11.10
Acupuncture pointsa suggested for use in the early stage of pregnancy after an IVF cycle
| Treatment goal | Acupuncture points |
| To stabilize Shen | YT, DU-20, PC-6, HT-7, K-4, K-9 |
| To support Kidney Qi | K-6 |
| To support Spleen Qi | ST-36 |
| To alleviate residual abdominal discomfort or ovarian swelling | LIV-5, GB-34 |
aUse points with even method. Avoid abdomen and lower back points.
The formula used in this research ‘Gu tai tang’ or Protect Fetus decoction has many different versions, but fundamentally they all aim to support Kidney and Spleen Qi while nourishing the blood and quieting the fetus.
Herbal formula for use after a positive pregnancy test in an IVF cycle; Yishen Gutai Tang (Nourish Kidney and Protect Fetus) modified. Reinforce Kidney and Spleen Qi, nourish Blood and quiet the fetus.
Yishen Gutai Tang (Nourish Kidney and Protect Fetus decoction) modified
| Tu Si Zi | 20 g | Semen Cuscatae |
| Du Zhong | 15 g | Cortex Eucommiae Ulmoidis |
| Xu Duan | 15 g | Radix Dipsaci |
| Sang Ji Sheng | 15 g | Ramulus Sangjisheng |
| Bai Zhu | 15 g | Rhizoma Atractylodis Macrocephalae |
| Huang Qin | 9 g | Radix Scutellariae Baicalensis |
| Gou Qi Zi | 12 g | Fructus Lycii Chinensis |
| Dang Shen | 12 g | Radix Codonopsis Pilulosae |
| Bai Zhu | 12 g | Rhizoma Atractylodis Macrocephalae |
| Da Zao | 3 pieces | Fructus Zizyphi Jujuba |
| Sha Ren | 3 g | Fructus seu Semen Amomi |
| He Shou Wu | 12 g | Radix Polygoni Multiflori |
If there is any bleeding, add:
| E Jiao | 15 g | Gelatinum Asini |
| Zhu Ma Gen | 9 g | Radix Boehmeriae |
For Morning sickness, see Chapter 4.
The Negative Pregnancy Test
If the IVF cycle has not succeeded, then the treatment priorities are to re-establish Chong and Ren channel function, clear stagnation of Qi and Blood, reinforce Spleen and Kidney function and to treat Lungs and Heart for grief and sadness. The menstrual cycle immediately after an IVF cycle will sometimes be longer than usual, as the ovaries may take some time to recover.
Weekly acupuncture treatment is useful at this time and should be continued until at least one good menstrual cycle has been achieved. Then the patient may start preparing for another IVF cycle using the suggestions for herb and acupuncture prescriptions made earlier.
If she is not planning on repeating IVF so soon, or she plans to try and conceive naturally, then a 3-month program can be constructed using the protocols outlined in Chapter 4, or above.
Acupuncture points: Choose from the points below (and see Table 11.11):
Table 11.11
Acupuncture pointsa suggested for use following a negative pregnancy test after an IVF cycle
| Treatment goal | Acupuncture points |
| To re-establish Chong channel function | SP-4, PC-6 |
| To regulate Chong and Ren channels | Ren-3, Ren-7 |
| To alleviate grief and sadness, benefit sleep | LU-3, HT-7, HT-4, YT |
| If bleeding after IVF cycle persists for longer than usual | SP-10, K-3 |
| To relieve abdominal bloating or discomfort | Ren-6, ST-28, LIV-5, SP-6 |
| To strengthen the Kidney Qi | Ren-4, K-6 |
| SP-6 | Sanyinjiao |
| SP-4 | Gongsun |
| PC-6 | Neiguan |
| LU-3 | Tian Fu |
| LIV-5 | Ligou |
| K-6 | Zhaohai |
| SP-10 | Xuehai |
| K-3 | Taixi |
| Ren-3 | Zhongji |
| Ren-7 | Lingdao |
| HT-7 | Shenmen |
| HT-4 | Lingdao |
| Yin Tang | |
| Ren-6 | Qihai |
| ST-28 | Shuidao |
This concludes our discussion on the use of Chinese medicine for the patient doing IVF, before, during and after her cycle (Table 11.12). As I stated at the outset, it will be some decades of careful observation in the clinic and informed and considered clinical experimentation before we can become expert in this sort of treatment. However I am, as are my colleagues, thrilled to be part of this exciting era of exploring the frontiers of reproductive medicine and the place that Chinese medicine can play in it. Some intrepid clinicians and researchers have already made wonderful contributions to this area and it is only just the beginning! This is what we shall discuss next.
Research on Acupuncture and IVF
Many IVF patients heard about the possible benefits of combining acupuncture with their IVF cycle after results of a small trial were published in 2002. This was followed by a spate of repeat trials from 2006 onwards. More than 20 trials, of varying quality, which look at the effect of acupuncture on the day of embryo transfer have been published in peer reviewed journals. While many of these have shown a positive effect on pregnancy rates when acupuncture is used, a number of other trials have shown no effect.
The abstracts of the many studies to-date that investigate the effect of acupuncture done at the time of embryo transfer, can be found online.29,30
Despite the fact that the jury is still out on whether acupuncture performed in this way is actually increasing pregnancy rates, many IVF patients are seeking out acupuncture as an adjunctive treatment. And, despite lack of consistent evidence of increased pregnancy rates, there is no doubt that IVF patients generally appreciate the increased well-being they experience as a result of the acupuncture. This has been shown in clinical studies to have the effect of reducing the stress and distress experienced during the cycle and increasing resilience and ability to cope with repeated IVF cycles if they are necessary.31–34
Additionally, it has been shown that acupuncture increases blood flow to the uterine lining and (in rats) to the ovaries. This theoretically could mean increased drug delivery and nutrition to these areas. Many clinics that offer acupuncture treatment to IVF patients combine the points that increase blood flow to ovaries and the uterus during the stimulation phase of the cycle when the woman is using the FSH drugs, and then points used in the above mentioned trials at the time of embryo transfer.
Effects on implantation and pregnancy rate
It is thought that the acupuncture points applied on the day of embryo transfer may confer some advantage to the process of implantation.
The original investigators said that they chose acupuncture points that ‘relax the uterus according to the principles of TCM’ and that ‘because acupuncture influences the autonomic nervous system, such treatment should optimize endometrial receptivity.’ They state that the points they chose ‘stimulate Taiying meridians (Spleen) and Yangming meridians (Stomach, Colon) to result in better blood perfusion and more energy in the uterus’ and that stimulation of other points, aimed to ‘sedate the patient and stabilize the endocrine system.’
A number of subsequent reviews have postulated that the effect of acupuncture given at the time of transfer might be to reduce contractions in the uterus, change the immune milieu, increase blood flow or to relax the patient and reduce cortisol. It has been noted that pregnancy and implantation rates are negatively impacted by uterine contractions at the time of transfer.35 One study on rats found that acupuncture reduced uterine contractions.36
One group thought that acupuncture might reduce endometrial motility and uterine contractions and therefore facilitate implantation of the embryo but when they tested this theory with ultrasound, they found little difference in the movement of the uterus at transfer between acupuncture and non-acupuncture groups.37
Another clinic33 has shown that acupuncture (whether by pricking the points or penetrating the points) reduces levels of the stress hormone cortisol, and also reduces the vascularity of the endometrium. They wondered if just having the patients lie down and relax before their embryo transfer might have the same result but found that it didn’t and that the acupuncture was the active intervention.
We don’t yet know exactly what effect cortisol level has on implantation, although stress has definitely been shown to be associated with lower fertility38 and lower implantation rates.26
Another study looked at the effect of repeated electroacupuncture treatments (using points which have been shown to increase blood flow to the uterus) before and during the drug phase of an IVF phase, on the serum cortisol and prolactin levels. They found that cortisol and prolactin levels were higher (cortisol still in normal physiologic range, but prolactin higher than normal physiologic range) in the acupuncture group than the control group for the week prior to embryo transfer, although the difference was not sustained after EPU.39
Endorphin levels, or other stress markers like adrenalin, sympathetic nervous system activity or heart rate have not to-date been measured in trials looking at the effect of acupuncture on implantation.
Acupuncture points used on the day of embryo transfer (ET)
Nearly all researchers using acupuncture (or electrical stimulation on acupuncture points) at the time of ET have used (for the treatment group) the original points used in the trial in 2002.40 Results have varied (in terms of pregnancy rates), despite use of the same points. The acupuncture protocol was varied in some trials.41–43 Box 11.3 summarizes the points used in these trials.
Another small study looked at the effect of hypnosis and another at the effect of laughter on IVF patients having embryo transfer. In both cases, the ‘treatment’ groups showed a higher pregnancy rate than the control group, indicating that stress reduction might have a beneficial effect on implantation.44,45
Effects on endometrium
We do not yet fully understand the effects of increased or decreased blood flow to the uterus or its lining on implantation. Electroacupuncture performed on certain points appeared to increase blood flow to the uterus of women taking downregulating drugs of the type used in IVF cycles in a small clinical trial, although these women were not actively doing IVF46 and the endometrium itself was not examined in this study.
One group,33 found that acupuncture (using the Paulus pre-transfer points, manual stimulation only) performed just before embryo transfer during an IVF cycle, reduced vascularity or endometrium volume. Less vascularity of the endometrium may promote a more hypoxic environment and since the mammalian embryo develops in a low-oxygen environment (especially during its first 5 days when it is normally traveling down the fallopian tube to the uterus), this may confer an advantage. This local hypoxia promotes angiogenesis (growth of new blood vessels) in anticipation of the demands of the growing embryo for oxygen and nutrients.47,48
Interestingly, acupuncture has also been shown to promote angiogenesis (in rat brains, using EA on DU-26).49
It may be an interesting combination of acupuncture-induced reduction of endometrial vascularity and hypoxia, combined with an increased stimulus to angiogenesis from both the acupuncture and the hypoxia that benefits implantation. If some types of acupuncture treatment do indeed promote a hypoxic environment that is advantageous to implantation and early embryo development, TCM doctors would be advised to avoid applying those acupuncture treatments which have been shown to increase blood flow to the uterus (see Box 11.4, below) at the time of embryo transfer, or the days following. In fact, these points were included in those treatments applied during the drug stimulation phase of the IVF cycle when the uterine lining is thickening. Most acupuncturists would be reluctant to apply electroacupuncture to the lower back, abdomen or Spleen points at the time of implantation in any case.
Additionally, we should be wary at this time of using herbs that have been shown to increase blood flow to the uterus.50
Conclusion
A number of advances have occurred in ART in the last 2 decades, much of it driven by the innovative work of embryologists who are working on developing the best conditions in which embryos form and thrive in vitro. What happens in the ovary before they get their hands on the egg and once the embryo is returned to the womb is more of a mystery. Ovary function, the follicular milieu and the quality of the egg are mostly things viewed by ART specialists as being hard wired in a woman’s genetic script and therefore out of reach. Similarly, the receptive or not so receptive, uterine environment is described as the hidden frontier by these specialists; they cannot see what happens after they put the embryo back and they cannot experiment ethically with women who have new embryo/s on board.
But it is precisely these inaccessible areas that we hope to work with. The strength of Chinese medicine is its ability to foster subtle balance – and doctors of Chinese medicine are used to working with the hidden and the subtle.
As long as we continue to focus intently on the balance of the Kidney Yin and the Yang, the Qi and the Blood, clearing Heat, Cold, Stasis or Damp, as needed, then we can improve the follicular and the uterine environment.
It may well be the case that some of our Kidney Yang herbs increase DHEA production or enhance oocyte mitochondrial function, or that the Kidney Yin herbs reduce oxidative damage inside the follicle. Or indeed, that acupuncture reduces the levels of inflammatory markers, increases nutrition and oxygen to the follicle and helps to create the correct balance of immune factors required for the survival of the fledgling embryo and its early development. While this is interesting to us, it does not fundamentally change the TCM diagnosis we make, or the treatment we apply.
Many TCM practitioners who work in integrated settings are attempting to achieve a balance between a traditional approach based on history, empirical knowledge and comprehension of Chinese medicine theory with the findings from clinical trials conducted on IVF patients. Ideally, we root our diagnosis and treatment in TCM principles while using research findings to augment the effectiveness of what we do where appropriate.
It is a challenging and stimulating arena requiring careful, inquiring reflective practice and data collection, and well thought out clinical trials, so that in some decades to come, we will have a substantial body of knowledge and discovery that will inform future doctors of Chinese medicine who treat IVF patients.
References
1. Bhal, P.S., Pugh, N.D., Gregory, L., et al. Perifollicular vascularity as a potential variable affecting outcome in stimulated IUI treatment cycles. Hum Reprod. 2001;16:1682–1689.
2. Van Blerkom, J., Antczak, M., Schrader, R. The developmental potential of the human oocyte is related to the dissolved oxygen content of follicular fluid: association with vascular endothelial growth factor levels and perifollicular blood flow characteristics. Hum Reprod. 1997;12:1047–1055.
3. Du, Y., Shi, L., Li, J., et al. Angiogenesis and improved cerebral blood flow in the ischemic boundary area were detected after electroacupuncture treatment to rats with ischemic stroke. Neurol Res. 2011;33(1):101–107.
4. Stener-Victorin, E., Kobayashi, R., Kurosawa, M. Ovarian blood flow responses to electro-acupuncture stimulation at different frequencies and intensities in anaesthetized rats. Auton Neurosci. 2003;108:50–56.
5. Tejera, A., Herrero, J., de los Santos, M.J. Oxygen consumption is a quality marker for human oocyte competence conditioned by ovarian stimulation regimens. Fertil Steril. 2011;96(3):618–623.
6. Lonergan, T., Bavister, B., Brenner, C. Mitochondria in stem cells. Mitochondrion. 2007;7(5):289–296.
7. Dumollard, R., Duchen, M., Carroll, J. The role of mitochondrial function in the oocyte and embryo. Curr Top Dev Biol. 2007;77:21–49.
8. May-Panloup, P., Chrétien, M.F., Jacques, C., et al. Low oocyte mitochondrial DNA content in ovarian insufficiency. Hum Reprod. 2005;20:593–597.
9. Tarin, J.J., Gomez-Piquer, V., Pertusa, J.F., et al. Association of female aging with decreased parthenogenetic activation, raised MPF, and MAPKs activities and reduced levels of glutathione S-transferases activity and thiols in mouse oocytes. Mol Reprod Dev. 2004;69:402–410.
10. Wiener-Megnazi, Z., Vardi, L., Lissak, A., et al. Oxidative stress indices in follicular fluid as measured by the thermochemiluminescence assay correlate with outcome parameters in in vitro fertilization. Fertil Steril. 2004;82(Suppl 3):1171–1176.
11. Ko, K.M., Leon, T.Y., Mak, D.H.F., et al. A characteristic pharmacological action of ‘Yang-invigorating’ Chinese tonifying herbs: Enhancement of myocardial ATP-generation capacity. Phytomedicine. 2006;13:636–642.
12. Demyttenaere, K., Nijs, P., Steeno, O., et al. Anxiety and conception rates in donor insemination. J Psychosom Obstet Gynaecol. 1988;8:175–181.
13. Ebbesen, S., Zachariae, R., Mehlsen, M.Y., et al. Stressful life events are associated with a poor in-vitro fertilization (IVF) outcome: a prospective study. Hum Reprod. 2009;24(9):2173–2182.
14. De Liz, T.M., Strauss, B. Differential efficacy of group and individual/couple psychotherapy with infertile patients. Hum Reprod. 2005;20:1324–1332.
15. Klonoff-Cohen, H., Natarajan, L. The concerns during assisted reproductive technologies (CART) scale and pregnancy outcomes. Fertil Steril. 2004;81(4):982–988.
16. Domar, A., Rooney, K.L., Wiegand, B. Impact of a group mind/body intervention on pregnancy rates in IVF patients. Fertil Steril. 2011;95(7):2269–2273.
17. Thiering, P., Beaurepaire, J., Jones, M., et al. Mood state as a predictor of treatment outcome after in vitro fertilization/embryo transfer technology (IVF/ET). J Psychosom Res. 1993;37(5):481–491.
18. Demyttenaere, K., Bonte, L., Gheldof, M., et al. Coping style and depression level influence outcome in in vitro fertilization. Fertil Steril. 1998;69(6):1026–1033.
19. Kondoh, E., Okamoto, T., Higuchi, T., et al. Stress affects uterine receptivity through an ovarian-independent pathway. Hum Reprod. 2009;24:945–953.
20. Rogers, N.L., Szuba, M.P., Staab, J.P., et al. Neuroimmunologic aspects of sleep and sleep loss. Semin Clin Neuropsychiatry. 2001;6(4):295–307.
21. King, K., Smith, S., Chapman, M., et al. Detailed analysis of peripheral blood natural killer (NK) cells in women with recurrent miscarriage. Hum Reprod. 2010;25(1):52–58.
22. Lian, F., Li, X., Sun, Z. Effect of Quyu Jiedu Granule on Microenvironment of Ova in Patients with Endometriosis. Chin J Integr Med. 2009;15(1):42–46.
23. Stener-Victorin, E., Jedel, E., Janson, P.O., et al. Low-frequency electroacupuncture and physical exercise decrease high muscle sympathetic nerve activity in polycystic ovary syndrome. Am J Physiol Regul Integr Comp Physiol. 2009;297(2):R387–R395.
24. Cakmak, Y.O., Akpinar, I.N., Ekinci, G., et al. Point- and frequency-specific response of the testicular artery to abdominal electroacupuncture in humans. Fertil Steril. 2008;90:1732–1738.
25. Farkas, D., Greenblatt, D.J. Influence of fruit juices on drug disposition: discrepancies between in vitro and clinical studies. Expert Opin Drug Metab Toxicol. 2008;4(4):381–393.
26. Gallinelli, A., Roncaglia, R., Matteo, M.L., et al. Immunological changes and stress are associated with different implantation rates in patients undergoing in vitro fertilization-embryo transfer. Fertil Steril. 2001;76(1):85–91.
27. Liddell, H.S., Pattison, N.S., Zanderigo, A. Recurrent miscarriage – outcome after supportive care in early pregnancy. Aust N Z J Obstet Gynaecol. 1991;31(4):320–322.
28. Ying, Liu, Jing-zhi, Wu. Effect of gutai decoction on the abortion rate of in vitro fertilization and embryo transfer. Chin J Integr Med. 2006;12(3):189–193.
29. Acupuncture IVF . Support Clinic. Research and reviews http://www.acupunctureivf.com.au/pages/research_by_cat.php?research_type_id=1.
30. Acupuncture IVF . Support Clinic. Research and reviews http://www.acupunctureivf.com.au/pages/research_by_cat.php?research_type_id=8.
31. Domar, A.D., Meshay, I., Kelliher, J., et al. The impact of acupuncture on in vitro fertilization outcome. Fertil Steril. 2009;91(3):723–726.
32. De Lacey, S., Smith, C., Paterson, C. Building resilience: An exploration of women’s perceptions of the use of acupuncture as an adjunct to IVF. BMC Complement Altern Med. 2009;9:50.
33. So, E.W., Ng, E.H., Wong, Y.Y., et al. A randomized double blind comparison of real and placebo acupuncture in IVF treatment. Hum Reprod. 2009;24(2):341–348.
34. Balk, J., Catov, J., Horn, B., et al. The relationship between perceived stress, acupuncture, and pregnancy rates among IVF patients: a pilot study. Complement Ther Clin Pract. 2010;16(3):154–157.
35. Fanchin, R., Righini, C., de Ziegler, D., et al. Effects of vaginal progesterone administration on uterine contractility at the time of embryo transfer. Fertil Steril. 2001;75:1136–1140.
36. Kim, J., Shin, K.H., Na, C.S. Effect of acupuncture treatment on uterine motility and cyclooxygenase-2 expression in pregnant rats. Acupunct Electrother Res. 1991;16:1–5.
37. Paulus, W., Zhang, M., Strehler, E., et al. Motility of the endometrium after acupuncture treatment. Fertil Steril. 2003;80(Suppl 3):131.
38. Buck Louis, G.M., Lum, K.J., Sundaram, R., et al. Stress reduces conception probabilities across the fertile window: evidence in support of relaxation. Fertil Steril. 2011;95(7):2184–2189.
39. Magarelli, P.C., Cridennda, D.K., Cohen, M. Changes in serum cortisol and prolactin associated with acupuncture during controlled ovarian hyperstimulation in women undergoing in vitro fertilization-embryo transfer treatment. Fertil Steril. 2009;92(6):1870–1879.
40. Paulus, W.E., Zhang, M., Strehler, E., et al. Influence of acupuncture on the pregnancy rate in patients who undergo assisted reproduction therapy. Fertil Steril. 2002;77(4):721–724.
41. Dieterle, S., Ying, G., Hatzmann, W., et al. Effect of acupuncture on the outcome of in vitro fertilization and intracytoplasmic sperm injection: a randomized, prospective, controlled clinical study. Fertil Steril. 2006;85:1347–1351.
42. Moy, I., Milad, M.P., Barnes, R., et al. Randomized controlled trial: effects of acupuncture on pregnancy rates in women undergoing in vitro fertilization. Fertil Steril. 2011;95:583–587.
43. Zhang, R., Feng, X.J., Guan, Q., et al. Increase of success rate for women undergoing embryo transfer by transcutaneous electrical acupoint stimulation: a prospective randomized placebo-controlled study. Fertil Steril. 2011;96(4):912–916.
44. Levitas, E., Parmet, A., Lunenfeld, E., et al. Impact of hypnosis during embryo transfer on the outcome of in vitro fertilization–embryo transfer: a case-control study. Fertil Steril. 2006;85:1404.
45. Friedler, S., Glasser, S., Azani, L., et al. The effect of medical clowning on pregnancy rates after in vitro fertilization and embryo transfer. Fertil Steril. 2011;95(6):2127.
46. Stener-Victorin, E., Waldenstrom, U., Andersson, S.A., et al. Reduction of blood flow impedance in the uterine arteries of infertile women with electro-acupuncture. Hum Reprod. 1996;11:1314–1317.
47. Genbacev, O., Joslin, R., Damsky, C.H., et al. Hypoxia alters early gestation human cytotrophoblast differentiation/invasion in vitro and models the placental defects that occur in preeclampsia. J Clin Invest. 1996;97(2):540–550.
48. Breier, G. Angiogenesis in embryonic development – a review. Troph Res. 2000;14:11–15.
49. Du, Y., Shi, L., Li, J., et al. Angiogenesis and improved cerebral blood flow in the ischemic boundary area were detected after electroacupuncture treatment to rats with ischemic stroke. Neurol Res. 2011;33(1):101–107.
50. Wing, T., Sedlmeier, E. Measuring the effectiveness of Chinese Herbal Medicine in improving female fertility. J Chin Med. 2006;80:22.
51. Ho, M., Huang, L.C., Chang, Y.Y., et al. Electroacupuncture reduces uterine artery blood flow impedance in infertile women. Taiwan J Obstet Gynecol. 2009;48(2):148–151.