Bacterial Diseases
Skin infection with bacteria may be a primary problem (e.g. impetigo) or a complication of another skin disease (e.g. atopic dermatitis). Nomenclature of these diseases often reflects the site and the depth of infection – that is, from the stratum corneum to the subcutaneous tissue (Fig. 61.1) – as well as the suspected causative organism.
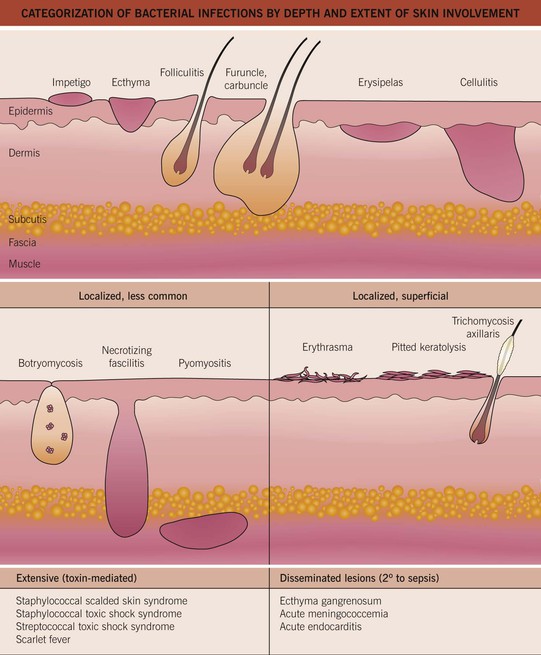
Fig. 61.1 Categorization of bacterial infections by depth and extent of skin involvement. More common, localized infections are depicted first; these infections are often secondary to Staphylococcus aureus or group A streptococci. Adapted from ‘Common bacterial infections of the skin,’ American Academy of Dermatology.
Gram-Positive Cocci
Staphylococcal and Streptococcal Skin Infections
Streptococcal infections may be complicated by acute post-streptococcal glomerulonephritis; this occurs in <1% of patients in high-income countries, but it remains a significant problem in low-income countries.
Impetigo
• Major organisms are Staphylococcus aureus and Streptococcus pyogenes (group A streptococci [GAS]).
• A very common, highly contagious bacterial infection, most commonly seen on the face or extremities of children; usually the skin is eroded with overlying ‘honey-colored’ crusts, but there is a bullous variant (Fig. 61.2).
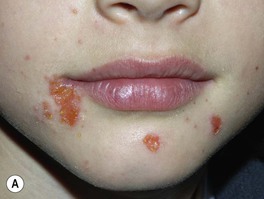
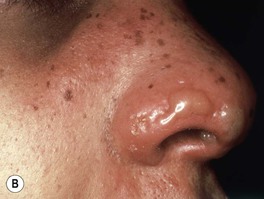
Fig. 61.2 Staphylococcal impetigo. A Honey-colored crusts on the chin and cheeks of a child with impetigo. B Superficial bullae and dry erosion on the nose due to bullous impetigo. A, Courtesy, Julie V. Schaffer, MD.
• Interestingly, bullae formation due to S. aureus can be explained by local release of an exfoliative toxin that binds to desmoglein 1 and leads to dissolution (i.e. acantholysis) of the upper epidermis (see Chapter 23).
• Risk factors for infection: nasal carriage of S. aureus and breaks in the epidermal barrier, e.g. atopic dermatitis, arthropod bites, trauma, scabies.
• DDx of eroded lesions: insect bites, prurigo simplex, dermatitis (e.g. atopic, nummular), herpes simplex viral infection.
• DDx of bullae: bullous insect bites, thermal burns, herpes simplex viral infection, and occasionally autoimmune bullous dermatoses.
• Rx: local wound care (including soap), removal of crusts by soaking; for mild cases, topical mupirocin or retapamulin; for moderate to severe infections, oral antibiotics, the choice of which is dependent on prevalence of methicillin-resistant S. aureus (MRSA) in the local community (Table 61.1).
Table 61.1
Empiric treatment of cutaneous staphylococcal and streptococcal infections in adults.
Treatment duration is usually 7–10 days, depending on the severity and clinical response. Initial choice of antibiotic is dependent on known resistance patterns in a given community. The contents of pustules or exudate (e.g. underlying a crust) should be sent for culture and sensitivities prior to beginning therapy. Quinolones and macrolides are not optimal for treatment of community-acquired methicillin-resistant Staphylococcus aureus (CA-MRSA) because resistance is common and may develop rapidly.
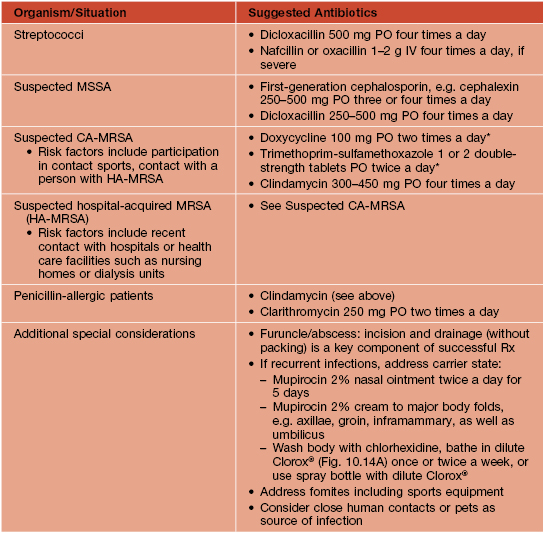
* Does not provide coverage of group A streptococci; if coverage of the latter is desired, a β-lactam is also prescribed.
MSSA, methicillin-sensitive Staphylococcus aureus.
Ecthyma
• Most commonly secondary to Streptococcus pyogenes.
• Ulceration with hemorrhagic crust that extends into the superficial dermis, i.e. is deeper than impetigo (Fig. 61.3); can heal with scarring.
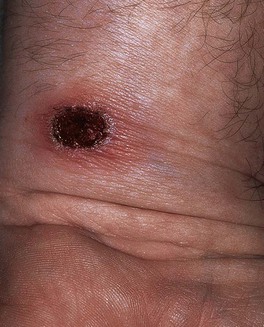
Fig. 61.3 Ecthyma. Ulceration with hemorrhagic crust on the wrist due to infection with group A streptococci. Courtesy, Kalman Watsky, MD.
• Often on the lower extremities, and risk factors include an edematous limb, arthropod bites, and a pre-existing ulceration.
• Rx: see Table 61.1.
Bacterial Folliculitis
• Staphylococcus aureus is the most common cause, followed by gram-negative bacteria; the latter can occur in patients with acne vulgaris on long-term antibiotic therapy; see Chapter 31 for Pseudomonas folliculitis.
• Usually superficial, but occasionally deep, infection centered on hair follicles (see Fig. 61.1).
– Superficial – 1- to 4-mm pustules on an erythematous base (see Fig. 31.2); centrally, a hair shaft may be noted.
– Deep – also referred to as sycosis – tender, erythematous papulonodules, often with a central pustule.
• Commonly in the beard area, on the upper trunk, or on the buttocks and thighs; shaving can be an exacerbating factor.
• DDx: culture-negative (normal flora) folliculitis, acne vulgaris, folliculitis due to fungi (e.g. Pityrosporum) or viruses (e.g. herpes simplex virus), rosacea, and pseudofolliculitis barbae (see Chapter 31).
• Rx: for superficial form – antibacterial washes (e.g. benzoyl peroxide, chlorhexidine) or topical gels (e.g. combination clindamycin/benzoyl peroxide); widespread staphylococcal folliculitis – oral antibiotics (see Table 61.1).
Abscesses, Furuncles, and Carbuncles
• By definition, a furuncle involves a hair follicle; involvement of multiple, adjacent follicles is termed a carbuncle (see Fig. 61.1).
• Most common organism is S. aureus, and this is the most frequent presentation for community-acquired MRSA (CA-MRSA).
• Clinically, furuncles appear as firm, tender, red nodules; carbuncles begin similarly but become larger in size and can develop multiple draining sinus tracts.
• Common locations are the face, neck, axillae, buttocks, perineum, and thighs.
• DDx: ruptured epidermoid inclusion cyst, hidradenitis suppurativa, and cystic acne.
• Rx: fluctuant lesions should be incised and drained; systemic antibiotics are generally reserved for: (1) furuncles around the nose, in the external auditory canal, or in other locations where drainage is difficult; (2) severe or extensive disease (e.g. multiple sites); (3) lesions with surrounding cellulitis/phlebitis or associated with signs or symptoms of systemic illness; (4) lesions not responding to local care; and (5) patients with concerning comorbidities or immunosuppression (see Table 61.1 for Rx options).
Erysipelas
• Most commonly due to Streptococcus pyogenes.
• Represents infection of the superficial dermis along with significant lymphatic involvement; often on the face and neck or the leg.
• Presents as a well-defined area of hot, indurated, bright erythema that is painful and tender (Fig. 61.4); occasionally, there may be superimposed pustules, vesicles, bullae, or areas of hemorrhagic necrosis.
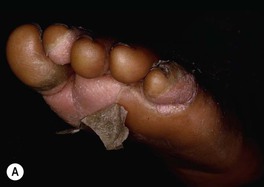
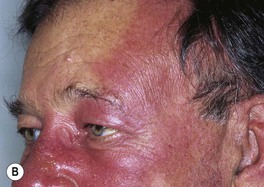
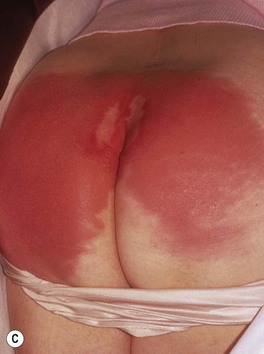
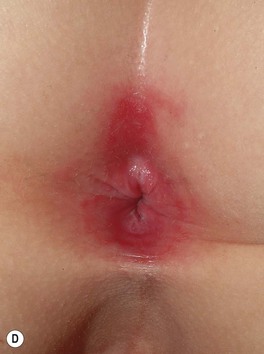
Fig. 61.4 Cutaneous manifestations of streptococcal infections. Prominent desquamation of the feet (A) following scarlet fever. Sharply demarcated erythema of the face, most obvious on the forehead (B), and of the buttocks (C) in two patients with erysipelas. Bright red erythema extending from the anal verge in a young boy with streptococcal perianal disease (D). A, Courtesy, Eugene Mirrer, MD; B, Courtesy, Kalman Watsky, MD; C, Courtesy, Mary Stone, MD; D, Courtesy, Julie V. Schaffer, MD.
• Favors the young, debilitated, elderly, and limbs with edema or lymphedema.
• DDx: cellulitis, erysipeloid breast cancer, irritant contact dermatitis, early necrotizing fasciitis or herpes zoster, erysipeloid, Sweet's syndrome, and if it involves the ear, chondritis.
• Rx: 10- to 14-day course of penicillin if due to Streptococcus pyogenes, with route depending on the severity and risk factors.
Streptococcal Intertrigo/Perianal Disease
• Presents as patches of erythema, especially in children (see Fig. 61.4 and Table 60.5).
• DDx: outlined in Fig. 13.4 and Table 60.5.
• Rx: 7- to 10-day course of a first-generation cephalosporin (see Table 61.1) or penicillin.
Cellulitis
• Most commonly due to Streptococcus pyogenes or S. aureus; in diabetics and immunocompromised hosts, other organisms (e.g. gram-negative bacilli) may be the cause.
• In children, Haemophilus influenzae can be a cause of cellulitis, but its incidence has decreased since introduction of the H. influenzae vaccine.
• Infection of the deep dermis and sometimes the subcutaneous fat (see Fig. 61.1).
• Skin rubor (redness), calor (warmth), dolor (pain), and tumor (swelling) are present; more ill-defined borders than erysipelas and may have skip areas; can become bullous or necrotic (Figs. 61.5 and 75.8).
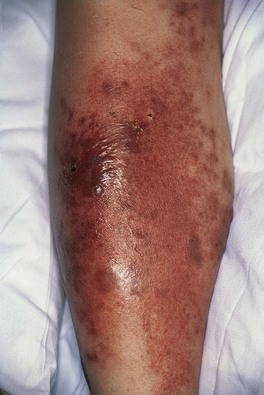
Fig. 61.5 Bullous cellulitis. Extensive soft tissue infection of the lower extremity due to group A streptococcal infection.
• Systemic symptoms include fever, chills, and malaise; CBC usually shows leukocytosis and bandemia.
• Risk factors for cellulitis of the lower extremity include previous DVT, previous cellulitis with lymphangiitis, chronic edema, and tinea pedis (especially in patients who have undergone saphenous venectomy).
• DDx: on the lower extremity, lipodermatosclerosis and stasis dermatitis (see Fig. 11.5); elsewhere, erysipelas and the early stage of necrotizing fasciitis, as well as causes of pseudocellulitis (Table 61.2).
• Rx: see Table 61.1.
Blistering Distal Dactylitis
• Most commonly secondary to GAS or S. aureus.
• Localized infection of the volar fat pad of a finger or, less often, a toe; occurs most commonly in children.
• Initially erythema and swelling of the skin, followed by development of one or more vesicles or bullae.
• Rx: drainage of blisters and systemic antibiotics (see Table 61.1).
Botryomycosis
• Most commonly caused by S. aureus, followed by Pseudomonas spp.
• Cutaneous and subcutaneous nodules that may have superimposed pustules, purulent discharge, or become ulcerative or verrucous; often in immunosuppressed hosts.
• Grains, representing macroscopic colonies of bacteria, are seen in biopsy specimens as well as the pustular discharge; grains are also seen in eumycotic and actinomycotic mycetoma (see Chapter 64) and actinomycosis (see below).
• Often develops at sites of trauma.
• DDx: ruptured epidermoid cyst, abscess, mycetoma, actinomycosis, and atypical mycobacterial or dimorphic fungal infection.
Necrotizing Fasciitis
• Usually represents polymicrobial infection with both anaerobes and aerobes; ~10% secondary to GAS.
• Rapidly progressive necrosis of subcutaneous fat and fascia that leads to undermining and ulceration; may have a foul discharge.
• Risk factors include older age, diabetes mellitus, alcoholism, peripheral vascular disease, and immunosuppression.
• Initially may resemble cellulitis, but associated pain is often out of proportion to the clinical findings; additional clues include tense edema and a violaceous or gray color reflecting impending necrosis (Figs. 61.6 and 75.9).
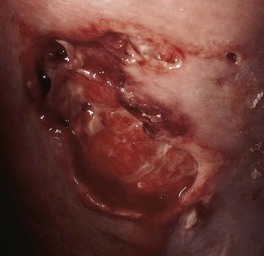
Fig. 61.6 Necrotizing fasciitis. Necrosis of the subcutaneous fat and fascia of the inner aspect of the upper arm in an elderly patient with diabetes mellitus. Note the watery discharge. Courtesy, Jean L. Bolognia, MD.
• Diagnosis requires a high index of suspicion; when anogenital, it is referred to as Fournier's gangrene.
• Patients may have fever, chills, malaise, and leukocytosis.
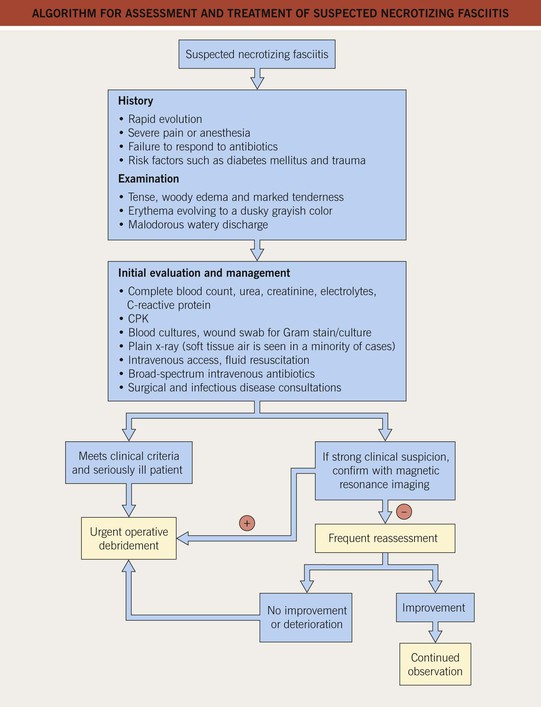
• Dx: outlined in Fig. 61.7.
• Rx: surgical debridement is the mainstay of therapy; broad-spectrum IV antibiotics.
Pyomyositis
• Primary bacterial infection of skeletal muscle, most commonly with S. aureus (see Fig. 61.1); associated with immunosuppression, including HIV infection.
Staphylococcal Scalded Skin Syndrome (SSSS)
• Secondary to S. aureus, phage group II strains, which produce exfoliative toxins that bind to desmoglein 1 and lead to dissolution (i.e. acantholysis) of the upper epidermis.
• More commonly seen in infants and children; occasionally, adults with chronic renal insufficiency can develop SSSS.
• Prodrome of malaise, fever, irritability, sore throat, and tender skin; purulent rhinorrhea or conjunctivitis may be present because the initial site of staphylococcal infection is usually extracutaneous.
• Tender erythema on the face and in intertriginous zones that generalizes to the remainder of the body over 1 or 2 days; due to the split in the upper epidermis, the skin becomes ‘wrinkled’ and then sloughs over 3–5 days, leading to denuded areas; on the face, radial fissures with scale-crust develop around the mouth and eyes (see Fig. 3.11).
• DDx: sunburn, drug reaction, Kawasaki disease (erythema often first appears in the groin), Stevens–Johnson syndrome/toxic epidermal necrolysis (SJS/TEN; usually affects older children and adults, has mucosal involvement, and nearly always drug-induced).
• Rx: hospitalization and IV anti-staphylococcal antibiotics (see Table 61.1).
Toxic Shock Syndrome (Other Than Streptococcal) (TSS)
• Secondary to Staphylococcus aureus, which produces an exotoxin, toxic shock syndrome toxin-1.
• Case definition of staphylococcal TSS is outlined in Table 61.3.
Table 61.3
Case definitions for the toxic shock syndromes.
For details on the current case definitions, see wwwn.cdc.gov/nndss and enter condition name as ‘toxic shock syndrome’ or ‘streptococcal toxic shock syndrome’.

* Defined as a definite case.
† Defined as a probable case, excluding any other possible etiology.
• Historically associated with menstruation and tampon use, but nowadays with surgical packing, meshes, and cutaneous infections (e.g. abscesses).
• Sudden onset of high fever, myalgias, vomiting, diarrhea, headache, and pharyngitis; hypotension is a key finding.
• Clinically, scarlatiniform changes initially appear on the trunk and then spread centrifugally; erythema and edema of the palms and soles can be followed by desquamation 1–3 weeks later.
• Mucous membrane findings: erythema, strawberry tongue, hyperemia of the conjunctivae (Fig. 61.8).
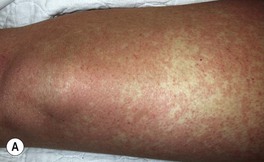
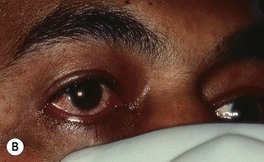
Fig. 61.8 Toxic shock syndrome due to Staphylococcus aureus infection. A Blotchy erythema is evident on the thigh. B Hyperemia of the conjunctiva is seen.
• DDx: streptococcal TSS, drug reaction plus hypotension from sepsis; in children, Kawasaki disease and scarlet fever.
• Rx: hospitalization and IV antibiotics (see Table 61.1).
streptococcal toxic shock syndrome (Streptococcal TSS)
• Secondary to GAS (especially M types 1 and 3), which produce exotoxins A and/or B.
• Case definition of streptococcal TSS is outlined in Table 61.3.
• Most common site of the associated streptococcal infection is the skin, e.g. cellulitis or necrotizing fasciitis.
• Rx: hospitalization and IV antibiotics (see Table 61.1).
Scarlet Fever
• Secondary to GAS, which produce erythrogenic toxins types A, B, and C.
• Seen in children (ages 1–10 years), usually following streptococcal tonsillitis or pharyngitis.
• Sore throat, headache, malaise, chills, anorexia, nausea, and high fevers precede erythema of the neck, chest, and axillae that becomes generalized over 4–6 hours.
• The erythema blanches with pressure and is studded with tiny papules (‘sunburn with goose pimples’); the cheeks are also flushed with circumoral pallor.
• Pastia lines (linear petechial streaks) are seen in major body folds, e.g. axillary, inguinal, antecubital.
• Desquamation of distal digits occurs after 7–10 days.
• Postinfectious sequelae include acute glomerulonephritis and rheumatic fever.
• DDx of palmoplantar desquamation: Kawasaki disease, TSS, and any preceding infection (including viral) with a high fever.
• DDx of exanthem: drug eruption, viral exanthem, early SSSS; a scarlatiniform eruption is also seen in TSS and Kawasaki disease.
Bacteremia/Septicemia
• Septic emboli can present as petechiae and purpura that may develop central pustules or hemorrhagic bullae; subcutaneous abscesses can also be seen.
• Endocarditis can be acute or subacute and caused by organisms including S. aureus and Streptococcus spp., respectively; cutaneous signs of endocarditis include splinter hemorrhages (see Chapter 58), Osler nodes, and Janeway lesions (see Table 18.2).
Gram-Positive Bacilli
Clostridial Skin Infections
• Clostridia spp. are gram-positive bacilli that live on dead organic matter and can cause anaerobic cellulitis or myonecrosis (gas gangrene).
– Risk factors: trauma, diabetes mellitus, peripheral vascular disease, and injection drug use.
– Generally due to Clostridium perfringens > other anaerobic bacteria (e.g. Bacteroides); incubation period >3 days with a rapid course.
– Minimal visible skin changes; signs include crepitus and a thin, dark gray-brown, foul-smelling (‘dirty dishwater’) exudate; pain often absent or mild without symptoms of toxemia (e.g. tachycardia).
• Myonecrosis, in contrast to anaerobic cellulitis, has a shorter incubation period with a very rapid course; overlying skin has a dark yellow to bronze discoloration, sometimes with bullae or necrosis, and severe swelling; toxemia (e.g. hypotension) is generally present.
• Rx: early surgical debridement and empirical antibiotics (e.g. clindamycin plus a third-generation cephalosporin) until culture and sensitivities obtained.
Corynebacterium (And Kytococcus) Skin Infections
Erythrasma
• Superficial, localized infection due to Corynebacterium minutissimum.
• Three major clinical variants.
– Interdigital – the most common variant, characterized by chronic maceration with fissuring or scaling; needs to be distinguished from interdigital tinea pedis.
– Intertriginous – thin red-brown plaques in the axillae and groin/upper inner thigh that may be misdiagnosed as tinea cruris (see Table 60.5; Fig. 61.9).
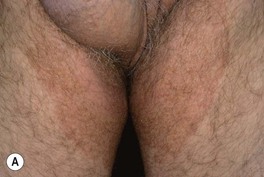
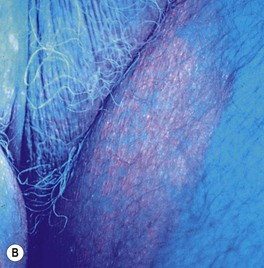
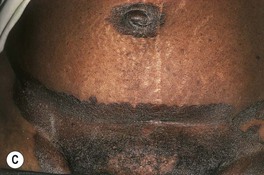

Fig. 61.9 Erythrasma. A Pink to brown scaly patches on the upper inner thighs. B Coral-red fluorescence upon illumination with a Wood's lamp. C Hyperpigmented plaques in the inguinal and periumbilical areas (intertriginous zones). D Well-demarcated, scaly, hyperpigmented plaque of disciform erythrasma. A, B, Courtesy, Louis A. Fragola, MD.
– ‘Disciform’ – often on the trunk and diabetes mellitus is a risk factor (Fig. 61.7D).
• Bright, coral-red fluorescence with Wood's lamp examination (see Figs. 61.9B and 13.2).
• Rx: topical clindamycin or erythromycin; prevent moisture accumulation with topical aluminum chloride 6–20% (axillae).
Pit ted Keratolysis
• Secondary to Kytococcus sedentarius (Micrococcus sedentarius) and Corynebacterium spp.
• Hyperhidrosis, prolonged occlusion, and increased surface pH are contributing factors; the latter plus bacterial infection lead to 1- to 3-mm crater-like depressions in the stratum corneum that may coalesce, with involvement of soles >> palms (Fig. 61.10).
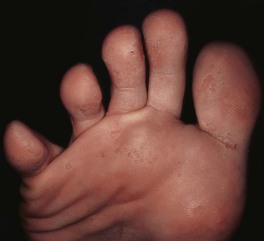
Fig. 61.10 Pitted keratolysis of the plantar surface of the foot. Multiple small craters with decreased stratum corneum that favor pressure points on the plantar surface. Courtesy, Kalman Watsky, MD.
• Often accompanied by a distinctive malodor.
• Rx: topical clindamycin or erythromycin; decrease eccrine sweat production with topical aluminum chloride 20%.
Trichomycosis Axillaris
• Common disorder that may be clinically subtle; often accompanied by malodor.
• Hair shafts are ensheathed with adherent yellow > red or black concretions composed of organisms (Fig. 61.11); most common in the axillae and a cause of chromhidrosis (see Chapter 32).
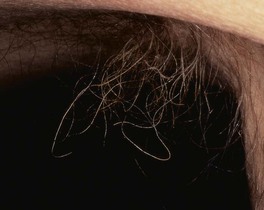
Fig. 61.11 Trichomycosis axillaris. Cylindrical sheaths and beading of the axillary hairs. A yellow color is seen most commonly.
• DDx: other causes of nodules on hair shafts (see Fig. 64.3).
• Rx: shaving of hair; topical antimicrobials (e.g. benzoyl peroxide, erythromycin) can help prevent recurrence.
Other Gram-Positive Skin Infections
Anthrax
• Bacillus anthracis causes inhalational, gastrointestinal, and cutaneous disease.
• Occurs most commonly in farmers and ranchers exposed to animals such as sheep, cows, horses, and goats; also secondary to exposure to hides from these animals (e.g. skins used for drums).
• Emerged as an agent of biological terrorism.
• Clinical characteristics of cutaneous disease are outlined in Table 61.4.
Table 61.4
Cutaneous anthrax – clinical characteristics.

Adapted from Carucci JA, McGovern TW, Norton SA, et al. Cutaneous anthrax management algorithm. J. Am. Acad. Dermatol. 2002;47:766–769.
• Rx for cutaneous disease: fluoroquinolone (e.g. ciprofloxacin 500 mg PO twice daily) for 60 days.
Erysipeloid
• Due to Erysipelothrix rhusiopathiae.
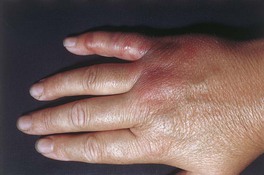
– Localized cellulitis – infection due to traumatic inoculation; seen in individuals who prepare fish and meat; the hand is a frequent site of involvement and the color is characteristically red-violet (Fig. 61.12).
– Generalized – uncommon form; multiple pink plaques, usually in the setting of immunosuppression, with associated fever and arthralgias; blood cultures are generally negative.
• DDx of localized form: cellulitis due to more common infectious agents (see above), atypical mycobacterial infection, early Vibrio infection.
• Rx for localized form: penicillin 500 mg PO four times a day for 7–10 days.
Gram-Negative Cocci
Acute Meningococcemia
• Systemic infection due to Neisseria meningitides.
• Primarily seen in young children (6 months to 1 year of age) and young adults in close quarters (e.g. dormitories, barracks).
• In most individuals, infection results in an asymptomatic carrier state.
• In acute meningococcemia, one-third to one-half of patients have skin lesions due to septic emboli, initially subtle petechiae that evolve into irregularly shaped purpura with a central gunmetal gray color that reflects necrosis (Fig. 61.13); gram-negative cocci may be seen on Gram staining of lesional tissue.
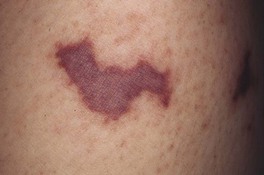
Fig. 61.13 Acute meningococcemia. Purpura with irregular outline and central gunmetal gray color. Courtesy, Kalman Watsky, MD.
• The septic lesions are to be distinguished from those due to disseminated intravascular coagulation (see Table 18.1).
• Additional systemic manifestations include fever, chills, hypotension, meningoencephalitis, pneumonia, pericarditis, and myocarditis.
• Rx: IV penicillin or ceftriaxone; vaccination is important for prevention.
Chronic Meningococcemia
• An indolent infection due to Neisseria meningitides.
• Recurrent episodes of fever, chills, night sweats, and arthralgias; skin lesions are polymorphous, e.g. pink macules and papules, nodules, petechiae/purpura; the skin lesions represent small vessel vasculitis without visible organisms by light microscopy, but PCR may be used to detect organisms.
Gonorrhea & Disseminated Gonococcal Infection
See Chapter 69.
Gram-Negative Bacilli
Pseudomonal Infections
Green nail syndrome is discussed in Chapter 58.
Gram-Negative Toe-Web Infection
• Although Pseudomonas aeruginosa is the most common cause, other gram-negative bacilli can be implicated (e.g. Escherichia coli, Proteus mirabilis).
• Risk factors are pre-existing tinea pedis and occlusion (e.g. tight-fitting shoes).
• Symptoms of burning and pain; signs include a malodorous exudate with a blue-green tinge, a grape-juice odor, and a moth-eaten appearance of skin due to maceration and erosions (Fig. 61.14).
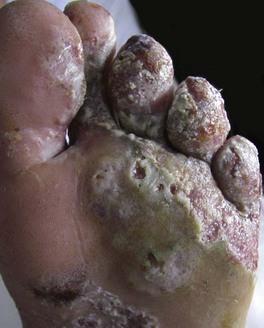
Fig. 61.14 Severe superficial infection of the skin with Pseudomonas. Note the macerated border, the erosions, and the moth-eaten appearance of the skin. Courtesy, Kalman Watsky, MD.
Otitis Externa (‘Swimmer’s Ear’)
• Swollen auditory ear canal with greenish purulent discharge.
• Extreme pain with manipulation of the pinna.
• Rx: antimicrobial drops (e.g. ofloxacin) with or without an ear wick, oral analgesics (e.g. NSAIDs).
Pseudomonal Folliculitis (Hot Tub Folliculitis)
See Table 31.2.
Pseudomonas Hot-Foot Syndrome
• Develops acutely on the soles of children and adolescents who are otherwise healthy after swimming in water with high concentrations of Pseudomonas aeruginosa.
• Painful and tender, red-purple, 1- or 2-cm nodules appear on the weight-bearing aspects of the feet (Fig. 61.15).
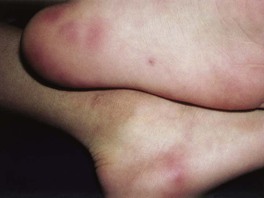
Fig. 61.15 Pseudomonas hot-foot syndrome. Tender erythematous nodules on the heel. Courtesy, Justin J. Green, MD.
• Self-limiting and DDx is primarily idiopathic palmoplantar hidradenitis (Chapter 32).
Cellulitis
• Clinical features are similar to those of cellulitis due to S. aureus (see above); can occur on the lower extremity in the setting of gram-negative toe-web infection or on the external ear postoperatively.
• Sometimes, it can be difficult to distinguish soft tissue infection from colonization with Pseudomonas, particularly in chronic ulcers.
Ecthyma Gangrenosum
• A sign of bacteremia or septicemia.
• Most commonly due to gram-negative bacilli, including Pseudomonas, but can also be due to opportunistic fungi; primarily seen in immunocompromised hosts, especially those with prolonged neutropenia.
• A red-purple macule or patch that develops central necrosis; sometimes the necrosis is preceded by a hemorrhagic bulla; the number can vary from one to a dozen or more (Fig. 61.16).
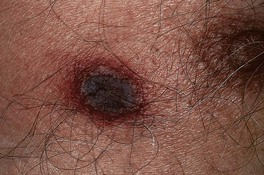
Fig. 61.16 Ecthyma gangrenosum. Embolic lesion of Pseudomonas aeruginosa on the chest. Note the necrotic center and inflammatory border.
• The most common location for ecthyma gangrenosum due to Pseudomonas is the groin.
• To establish the diagnosis, culture of tissue, obtained via sterile biopsy technique (see Fig. 2.10), is performed in combination with histopathology.
Treatment of Pseudomonal Infections
• For superficial infection (e.g. gram-negative toe-web infection): 5% acetic acid soaks followed by application of a topical antibiotic (e.g. gentamicin, silver sulfadiazine); if minimal improvement or severe, oral fluoroquinolone.
• For severe or systemic infections: piperacillin/tazobactam or doripenem if penicillin-allergic; may be combined with an aminoglycoside antibiotic.
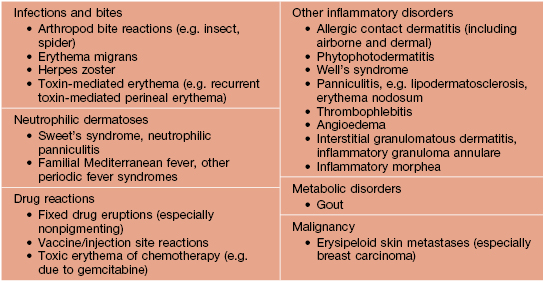
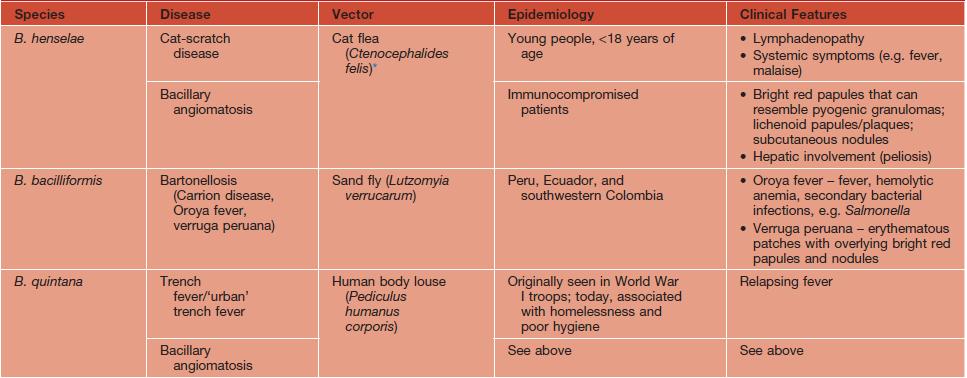
Diseases Caused by Bartonella Species
See Table 61.5.
Other Gram-Negative Skin Infections with Fever and Skin Findings
See Table 61.6.
Spirochetes
Lyme Disease
See Chapter 15.
Syphilis
See Chapter 69.
Other Treponemal Diseases
• Like syphilis, other treponemal diseases may have primary, secondary, and tertiary stages.
– Due to Treponema pallidum endemicum.
– Seen most commonly in Africa, the Arabian peninsula, and Southeast Asia.
– Children younger than the age of 15 years are most often affected.
– Primary lesion often missed.
– Secondary stage: macerated patches on lips, tongue, and pharynx; angular stomatitis; condyloma lata; generalized lymphadenopathy.
– Tertiary stage: gummas that can lead to destruction of the palate and nasal septum.
– Seen primarily in Central and South America.
– Primary stage: minute macules or papules with erythematous haloes, most commonly on the lower extremities, that develop into infiltrated plaques over several months.
– Secondary stage: smaller, variably pigmented (red, blue, black, or hypopigmented), scaly macules and papules that may coalesce; clustered near the initial primary lesion or generalized.
– Tertiary stage: symmetric, depigmented, vitiligo-like lesions that are atrophic or keratotic.
– Due to T. pallidum pertenue.
– Seen in warm, humid, tropical climates.
– Children younger than the age of 15 years are most often affected.
– Primary: erythematous, infiltrated, painful papule, usually on the extremities; enlarges to become up to 5 cm in diameter and ulcerates; heals spontaneously over 3–6 months.
– Secondary: smaller lesions adjacent to orifices or adjacent to site of initial primary lesion (Fig. 61.17).
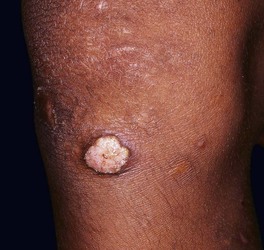
Fig. 61.17 Cutaneous yaws on the knee of an adolescent from Indonesia. Courtesy, Peter Ehrnstrom, MD.
– Tertiary: destructive skin lesions, palmoplantar thickening that can lead to difficulty with ambulation, chronic osteitis (sabre tibia).
Filamentous Bacteria
Actinomycosis
• Most commonly due to Actinomyces israelii.
• Three major sites of involvement – cervical, pulmonary, and gastrointestinal.
• Skin involvement is most common with the cervical variant and is sometimes referred to as ‘lumpy jaw’ due to irregular subcutaneous nodules; the latter can drain and the exudate contains grains (Fig. 61.18).
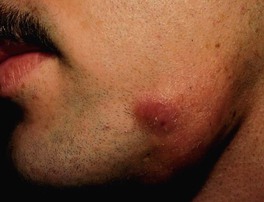
Fig. 61.18 Cervicofacial actinomycosis or ‘lumpy jaw’ with soft tissue swelling and draining ulcerated nodules. The discharge contained sulfur granules, a term used when the grains are yellow in color. Courtesy, M. Joyce Rico, MD.
Actinomycotic Mycetoma
• Most commonly due to Nocardia as well as Actinomadura madurae, Actinomadura pelletieri, and Streptomyces somaliensis; organisms are found in soil and on plant material (Table 61.7).
Table 61.7
Four major clinical forms of cutaneous nocardiosis.
Rx: Sulfonamides are the drugs of choice for primary cutaneous nocardiosis, with minocycline being an alternative for sulfonamide-allergic patients. Duration of treatment is at least 6-12 weeks for localized disease in immunocompetent hosts. Surgical excision may be required for deep abscesses.
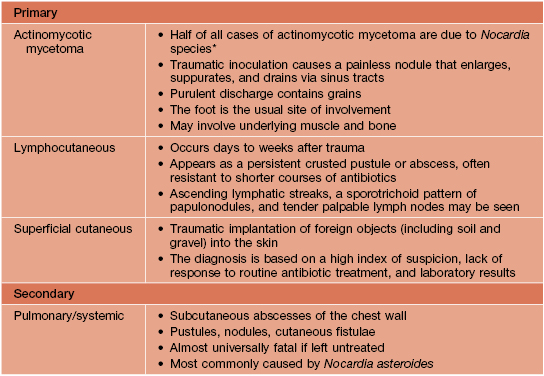
* In Mexico and Central and South America, N. brasiliensis is the etiologic agent of 90% of actinomycotic mycetomas, whereas in the United States, most mycetomas are caused by true fungi.
• DDx: distinguishing this entity from eumycotic mycetoma requires culture of grains or tissue; prior to the return of tissue or grain culture results, a presumptive diagnosis can be made based on the diameter of the filaments or hyphae composing the grains in biopsy specimens.