The febrile adult
Examination of the febrile adult
Symptoms and definitions
Fever (pyrexia) is a body temperature >99th percentile of the healthy adult maximum (p. 61). Fever is present if the oral temperature is >37.7°C, or tympanic temperature >37.5°C. In immunodeficient or neutropenic patients, fever is a single temperature >38.3°C, or a temperature >38°C sustained for >1 hour.
Body temperature is tightly controlled to maintain normal metabolic processes. The set point is controlled by the hypothalamus and modified by infection, inflammation and, rarely, other conditions, e.g. hypothyroidism, lymphoma. Infection is the most common cause but in very young or elderly patients and those with impaired immune function (due to primary disease, e.g. human immunodeficiency virus (HIV), or following treatment, e.g. oral steroids, immunosuppressants) it may not produce fever.
Body temperature depends upon the balance between heat generation and loss, and the ambient environment. Heat-related illness occurs with exercise in high temperatures and humidity. It is more common at the extremes of age and may be precipitated or aggravated by drugs which affect thermoregulation, e.g. phenothiazines, alcohol, or which are associated with excessive exercise, e.g. ‘rave’ drugs, including ecstasy, amphetamines (Boxes 17.1 and 17.2).
Fictitious fever is produced artificially by the patient or an attendant. It may form part of a Munchausen or Munchausen-by-proxy syndrome (Box 17.3).
Extreme fever (>41°C) is life-threatening and is usually associated with:
• central problems with temperature regulation, e.g. following intracranial haemorrhage or head injury
• drug reactions, e.g. to anaesthetic agents, or drugs associated with the neuroleptic malignant syndrome
• severe environmental conditions often with strenuous unaccustomed exertion (heatstroke)
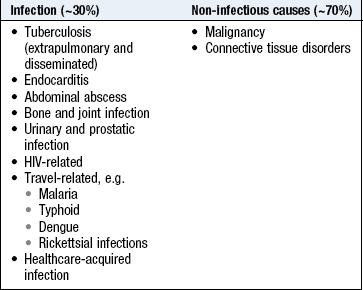
Fever (pyrexia) of unknown origin (FUO or PUO) is documented fever which remains unexplained after 2–3 weeks’ investigation. Healthcare-acquired PUO is fever in patients hospitalised for >48 hours with no infection evident at admission, and in whom the diagnosis remains uncertain after ≥3 days of appropriate evaluation (Box 17.4).
Rigors (chills) are bouts of uncontrollable muscular shaking, often with ‘chattering’ teeth, lasting for minutes. They are associated with rapid temperature rises and may be caused by cytokines and acute-phase proteins resetting the hypothalamic temperature set point. Subjectively the patient feels cold and unwell and the episode may be followed by sweating. A rigor may be associated with bacteraemia or malaria and is of poor diagnostic value.
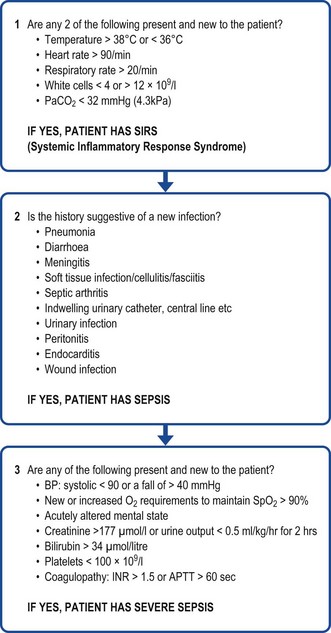
The terms systemic inflammatory response syndrome (SIRS), sepsis, severe sepsis and septic shock reflect progressively increasing morbidity and mortality in response to infection. Multiple organ failure and death ensue if recognition or treatment is delayed (Fig. 17.1). The term SIRS is not specific to infection.
The history
How has the fever been documented? What is its severity and time course? Have there been rigors or sweating?
Has there been a rash or skin changes? If yes, ask about its timing in relation to the fever, the distribution and direction of any progression and associated symptoms, e.g. pruritus, local lymphadenopathy.
Systematically ask about localising symptoms, e.g. cough, pleuritic chest pain, purulent sputum, vomiting, abdominal pain, jaundice, diarrhoea, dysuria, urinary frequency, headache, photophobia, neck stiffness, altered consciousness, joint pain, muscle aches, throat or ear discomfort and nasal discharge.
Are there constitutional symptoms, including easy fatigability, anorexia, weight loss, falls, change in daily activities or behaviour? Such symptoms may indicate infection in the elderly or immunocompromised.
Past medical history
Have there been previous or recurrent infections, illnesses, surgical operations or dental treatment?
Has there been contact or residence in a healthcare facility (including long-term care facility)?
Ask about a history of immunosuppression, e.g. HIV infection, chemotherapy, steroid therapy, transplantation, diabetes mellitus. Ask about indwelling catheters, e.g. urethral, intravenous (IV) or implants, e.g. pacemakers, joint replacements.
Drug history
Find out about all prescribed and non-prescribed medications, e.g. herbal remedies taken and ask specifically about immunosuppressants (including oral steroids), antibiotics, antipyretics. Have any ‘recreational’ drugs been taken; if so, have they ever been injected?
Note any history of adverse reactions, allergies or hypersensitivity to any drugs, particularly antibiotics.
Family and social history
Has the patient had contact with anyone with a similar illness? Find out about exposure to animals, birds or pets and if so, is the animal unwell? Note the patient’s occupation and hobbies. Are there clusters of similar symptoms or infections among family, friends or workmates?
Travel history
Has there been recent (in the past year) travel abroad? If so, take a detailed travel history including:
• travel destinations: dates, duration, mode of travel, stop-overs (Box 2.18)
• environment abroad: accommodation, altitude, climate, activities
• lifestyle: including diet, e.g. raw or unpasteurised products, sexual contact (who, when, how many partners), water sports, healthcare, piercings, tattoos
• medical history: including vaccination status, pre-existing conditions, antimalarial measures, particularly type, duration and compliance (Boxes 17.5 and 17.6).
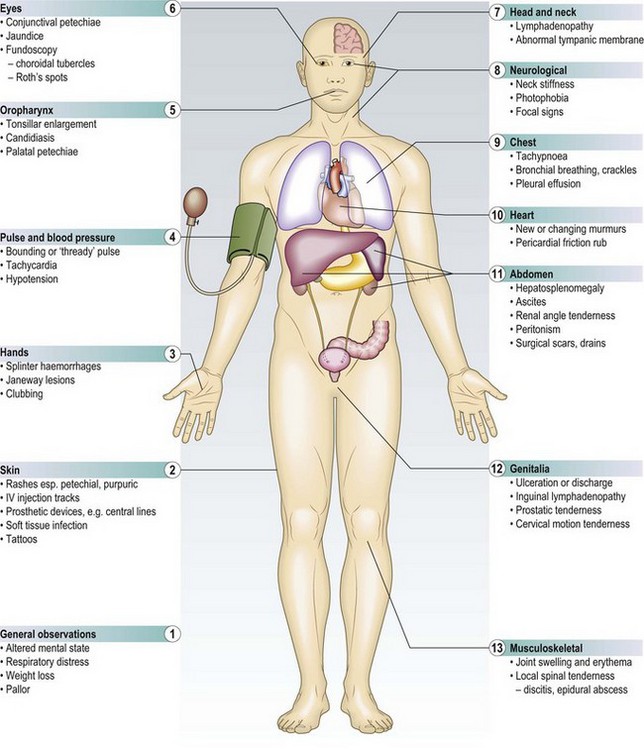
The physical examination
Specific situations
Injecting drug users: Injecting drug users are at particular risk of serious bacterial infection as well as viral diseases, e.g. HIV, hepatitis B and C. The commonest infections are of skin and soft tissue with bacteraemia leading to endocarditis (especially involving the tricuspid valve) and bone and joint infections. In an injecting drug user with fever, examine injection sites for discharge or signs of infection, listen to the chest for crackles or pleural rub (septic pulmonary emboli) and auscultate the heart for murmurs (right-sided valve endocarditis),
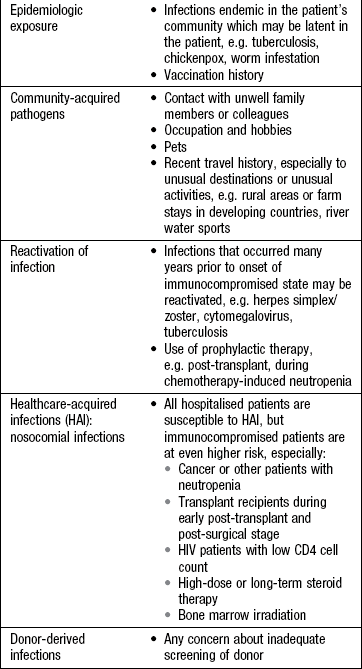
The immunocompromised patient: Although immunocompromised patients have less fever with infection, it is still the main presenting complaint. Because they are less able to mount an inflammatory response at the site of infection, the usual signs and symptoms may be absent, e.g. pneumonia without purulent sputum, tenderness without visible inflammation in a perirectal abscess.
In a febrile immunocompromised patient:
• symptoms are diminished or atypical
• obtain a detailed history for possible sources of infection
• expect atypical clinical and radiological findings
• expect the infection to be advanced at the time of presentation
• use computed tomography (CT) and magnetic resonance imaging (MR) scanning early for anatomic delineation of infection
• obtain tissue for histopathology and microbiology early for specific microbiologic diagnosis.
Use the examination sequence above, but additionally look for:
• cushingoid features (Fig. 5.18) suggestive of oral corticosteroid use
• malnourished or wasted appearance
• features of chronic alcohol consumption and liver cirrhosis (Fig. 8.11)
• changes related to renal failure and replacement therapy (Fig. 9.5)
• changes associated with diabetes mellitus (Ch. 5)
• subtle signs of infection around indwelling catheters and tubes
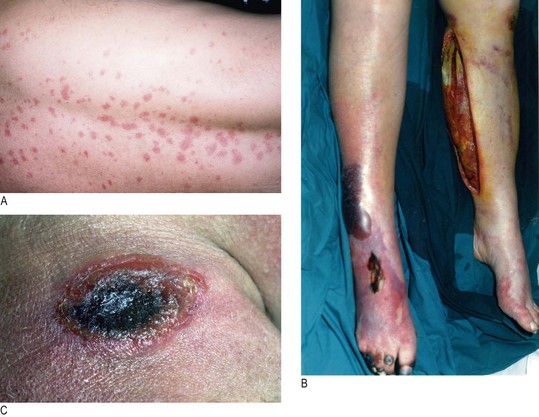
• constellations of lesions commonly seen in neutropenic patients, e.g. erythema, rash, erythema nodosum, soft-tissue infection, ulcers, furuncles, herpetic eruptions, paronychia, mucositis, dental or peritonsillar abscesses, perirectal infection
• constellations of lesions commonly seen in HIV infection – carefully examine the skin, mouth, genitalia and perianal area. In a severely immunocompromised patient avoid rectal examination as this may breach the rectal mucosa and cause iatrogenic infection (Boxes 17.10 and 17.11).
Healthcare-acquired infection (HAI): HAIs affect up to 10% of all hospital admissions. The close proximity of ill patients, coupled with the concentrated use of antimicrobial drugs and ease of transmission by healthcare workers, has led to multidrug-resistant organisms, e.g. meticillin-resistant Staphylococcus aureus (MRSA), Clostridium difficile. These infections are transmitted by many routes – contact, droplet spread, medication-related, transfusion, needlestick and air-borne. The commonest HAIs relate to indwelling urinary catheters and invasive devices, e.g. IV cannulae, and procedures. In a patient with fever and any invasive device find out how long the cannula, prosthesis or catheter has been present and look for redness or discharge at the entry site (Box 17.12).