Pregnancy loss, miscarriage, immune infertility, and ectopic pregnancy
Miscarriage
Healthy fertility does not mean just the ability to conceive. Good fertility means establishing and then nurturing a pregnancy for 9 months to full term. Thus, doctors specializing in the treatment of infertility need to hold clearly in their mind the goal of the birth of a healthy baby and not focus only on the first hurdle, the positive pregnancy test: some of the modern technologies used in assisted reproduction place so much emphasis on achieving that first prize that the integrity of the rest of the pregnancy can be compromised. The quality of that small bundle of just a few cells, the pre-embryo, determines (to a significant extent) the development of the rest of the pregnancy. And the biological integrity of the embryo is directly related to the quality of the gametes that fuse to form it and, of course, the quality of the gametes depends on the health and circumstance of the men and women who make them. Equally, the integrity of the uterine lining and the uterine environment is crucial for successful implantation, development of the placenta and establishment of a viable pregnancy.
So, if we are to approach fertility in the broad view, all aspects of the health of both partners and their gametes must be considered, which means examining all aspects of lifestyle and life stresses before conceiving. It might mean avoiding exposure to certain environmental factors or changing eating patterns or addressing chronic diseases. Many different parts of our lives can have a big impact on fertility and can be reflected not only in ease of conception but also in miscarriage rates (see Ch. 12).
Miscarriage is a common event causing large numbers of women (e.g., a quarter of a million each year in the UK) to experience grief and distress The term miscarriage refers to pregnancy loss after a conception has produced viable quantities of the pregnancy hormone (human chorionic gonadotrophin (hCG) in the blood and urine, or the fetus has developed to the point where either a gestational sac (1 week after a missed menstrual period) or a heart beat is visible on ultrasound (2–3 weeks after a missed period). In its broadest definition, pregnancy loss refers to any fetal loss from conception until the time of fetal viability at 23 weeks’ gestation.
In the first part of this chapter, we shall examine pregnancy loss by miscarriage. We shall also look at all the steps that occur between fertilization and a well-established and viable pregnancy and how loss of embryos can happen at any of these stages, even before pregnancy is suspected. After examining all the options for treatment or prevention of miscarriage, the second part of this chapter examines pregnancy loss caused by implantation of the embryo in the wrong place – ectopic pregnancy.
When it comes to treatment, the focus is primarily on the female of the couple, as she is the stage on which the pregnancy is enacted. However, just because the sperm has left the male partner’s body and successfully made contact with an egg does not mean that we can ignore its role in the future survival of the fetus. There are many factors affecting both male and female gametes that can influence the future of the fetus and which will be examined in more detail below. Historically, however, in both Western medicine texts and in Chinese medicine texts, the miscarriage spotlight has fallen on the mother-to-be.
Pre- and post-implantation loss
Clinical rates of miscarriage are often reported to be between 10 and 25% – or higher depending on age. However, the loss of embryos after fertilization but before implantation is much higher than that.
Of the potential pregnancies which are lost, 75% are due to implantation failure and are not clinically recognized as miscarriages. If a small (unviable) amount of hCG is measured on an early pregnancy test, it is called a biochemical pregnancy; it has reached implantation stage but gotten no further. In these days of IVF, what used to be occult pregnancy losses are not so occult anymore.
Conceptions, therefore, occur much more frequently than we think but embryos can be lost before the woman even knows she is pregnant, maybe even before the trophoblast (which forms a week or so after fertilization) has started producing hCG to tell the corpus luteum to keep producing progesterone.
Defective embryos reflect faults in the egg (especially if it is older); faults in the sperm (especially if they have been exposed to radiation or toxic chemicals); faults in the fertilization process itself (polyspermia or fertilization by more than one sperm), or may be just a random strike of destiny in the way the embryo itself develops. The technical term for the reason for these failures of implantation or development is chromosomal embryopathy, i.e., a genetic fault exists in the embryo such as to make it unviable, and cell division and development cease. Because the genetic blueprint of each embryo is brand new, it has never been tested and so fatal mistakes are commonplace.
There are some chromosomal embryopathies which unfortunately do not make the embryo unviable enough and these are the chromosomal patterns which produce Down syndrome babies and other genetic syndromes. Ultrasound measurements of the fetus at week 11 or 12 will alert the mother to risk of abnormality. Where there is suspicion of increased risk of genetic abnormalities, tests may be ordered to determine the genetic make-up of the embryo. These tests are done by collecting cells from the newly forming placenta (CVS or chorionic villus sampling) or from the amniotic fluid (amniocentesis); from these cells the chromosomes of the embryo are analyzed.
Once a pregnancy is confirmed by an ultrasound which measures a healthy heartbeat, and there are no symptoms of back or abdomen pain or bleeding, then the risk of miscarriage falls to a low level (approx. 2%).1
Miscarriage and age
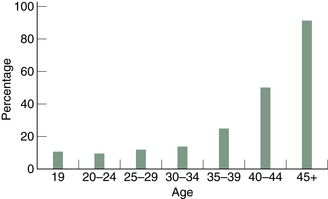
Advanced age is the primary risk factor for miscarriage. The risk rises sharply and exponentially from age 35 (see Fig. 8.1). While the effect of maternal age on miscarriage is marked, the male partner’s age also can impact miscarriage risk. Several studies have looked at the effect of the male partner’s age on miscarriage risk, noting that more advanced age (>35–40 years) is associated with more miscarriages.2–4 This increased risk is especially apparent where the female partner is under 35. The miscarriage rate in younger women with male partners aged ≥35 is double that of women with younger husbands.5
What does Chinese medicine say causes miscarriages?
Kidney Jing and Yin deficiency not only mean difficulty in producing gametes in the first place but also difficulty in producing healthy effective gametes (i.e., ones with intact chromosomes and undamaged DNA). Yin deficiency, which exerts its effects more noticeably with age, is a common factor affecting the viability of the gametes. In the case of ova, this viability is measured not only in the integrity of the chromosomes in the nucleus of the egg but also in the mitochondria (the organelles which produce the energy currency the cell needs to carry out all its activities), which have their own DNA. The DNA in a baby’s mitochondria is inherited only from the mother.
Although environment and lifestyle can affect the Kidney Jing and Yin (see Ch. 12), it is aging which is the main drain on Kidney reserves, evidenced by the fact that many women who become pregnant in their 40s miscarry (Fig. 8.1). As mentioned above, although the effect of age is not quite so marked in men, presumably because sperm are made afresh constantly, there are nevertheless more miscarriages when the male partner is older. Thus, the Jing-depleting effects of age affect men’s fertility too. The difficulty older women and men experience in trying to have children is a control provided by nature to discourage the production of offspring who do not have a strong Jing Qi inheritance. The offspring of parents who pass on poor-quality Jing may suffer the consequences. If the Jing that the new fetus inherits is too deficient, however, nature will ensure it will not survive and miscarriage will follow.
Interestingly, women who have taken the oral contraceptive pill for an extended period of time (≥8 years) have a reduced risk of miscarriage when they are older. In fact, the rate of miscarriage and infertility is half that of other women (≥35 years) who have not taken the pill.6 Because they have conserved rather than spent the thousands of eggs which years of menstrual cycles consume, they have a larger store of good-quality eggs and a larger store of Jing later in their reproductive years.
As practitioners of TCM, we can try to apply preventative treatment or measures for the gametes so that they do not develop abnormalities (see Prevention of future miscarriage, later). This might be easier to achieve with sperm than with eggs. Although stem cell science tells us there is a possibility that new oocytes can be produced by ovarian tissue, the fact is that the eggs in a woman’s ovaries available for ovulation have been present since before her birth; hence, their genetic integrity has much to do with their age and past history (of radiation, etc.). Certainly no influence can be exerted on the DNA in the chromosomes of these egg cells, but influence can be exerted on the nourishment and development of the follicle (see Ch. 11). Herbal and acupuncture treatment of men diagnosed with Yin deficiency and internal Heat (who often have a high percentage of abnormal sperm forms) can achieve a positive influence on the sperm quality.
Mechanism of embryo loss before implantation
As mentioned before, at least half of the embryos which fall by the wayside before they even implant in the uterus are those that show abnormal development, i.e., there is something wrong with the genetic programing.
For those embryos that do not have a genetic problem, other factors may arrest further development. This may be a lack of energy (ATP) required for cell division in the early embryo (discussed in Ch. 11). In some of these cases, the problem is not so much with the gametes or the embryo itself but with the reproductive tract of the mother; the fallopian tubes or the uterus.
Tubes – Qi stagnation/Damp: There may be a problem with the tubes such that the pre-embryo does not receive the necessary care and nourishment to take it through the first few cell divisions that occur after fertilization. A fault in the tubes may also mean that the embryo traverses them too rapidly or too slowly, thus it arrives in the uterus at a time when the stage of development of the endometrium does not match its own and implantation is not favored.
The TCM doctor gives treatment around ovulation time and immediately afterwards to regulate the Liver Qi and therefore the passage of the embryo in the tubes. If mucus secretions are suspected to be obstructing or slowing passage in the tubes, treatment to clear Damp will be added. (This has already been discussed in Chapters 4 and 6.)
Endometrium – Damp or Blood stagnation/Yin, Yang or Blood deficiency: Alternatively, or in addition, there may be a problem with the endometrium. Excess fluid or mucus on the surface can interfere with implantation. In TCM, such a situation represents excess Damp. The aim of treatment will be to clear Damp and Fluids with herbs and acupuncture.
In another situation, the endometrium does not provide a well formed surface with appropriate sites for attachment and implantation. In TCM terms, this may reflect Blood stagnation, deficient Yin or Blood, or a ‘Cold womb’. Blood stagnation is best treated during the period to ensure a thorough discharge of the endometrium and smooth remodeling of endometrial tissue to provide a more favorable surface for implantation later on. Blood and Yin deficiency, which lead to a thin or dry uterine lining, is best treated straight after the period with Blood and Yin tonic herbs and foods. A ‘Cold womb’ is how TCM doctors describe the uterus of a woman who is Yang deficient. Yang deficiency is often manifest in low progesterone levels, which means the lining of the uterus does not secrete sufficient nutrients in the luteal phase to nourish the embryo; thus, it fails to implant or develop.
TCM approach to the treatment of miscarriage
A miscarriage from the Chinese medicine point of view can be nearly as demanding on the body’s resources as childbirth, i.e., the physiologic changes experienced by a pregnant body which then suddenly becomes not pregnant are significant and require great adjustments. The hormone levels drop very rapidly after a miscarriage and if there has been significant blood loss, this will leave the body very weak. The recovery is not just physical; in the case of a miscarriage, there is usually emotional distress and this can be considerable if the miscarriage follows a period of infertility.
Chinese medicine texts describe several different clinical approaches to miscarriage, depending on the circumstances.
• Threatened miscarriage: trying to save a pregnancy at risk. If a woman who is pregnant starts bleeding, this is called a threatened miscarriage and treatment is employed to ‘pacify the fetus’ in an attempt to stabilize and save the pregnancy if possible. Since a large percentage of miscarriages are the result of genetic defects in the embryo, such treatment will in many cases, have very limited useful effects. Often, no matter what treatment is given, the miscarriage still occurs. Ideally, the TCM doctor needs to discover whether the fetus is doomed by chromosomal abnormality or whether it is quite healthy and it is the mother’s condition which needs to be improved. A master pulse-taker may be able to make such a diagnosis but for many less experienced practitioners, it may be signs of healthy development of the fetus (or not) on the ultrasound that can give us more precise information. In the end, many practitioners will choose to give treatment on a ‘lets give it a try, we’ve got nothing to lose’ basis.
• Inevitable miscarriage and sequelae. In the event the pregnancy is inevitably doomed, the doctor of Chinese medicine can contribute in quite a different way. Once the fetus has died and has been expelled, or still needs to be expelled, then Chinese medicine can be used to expedite the complete removal of all the contents of the uterus. Subsequently, recuperative treatment will address weakness in the mother due to blood loss and physiologic and psychological stress. When such weakness is made good, treatment to regulate the menstrual cycle again will be appropriate. In most cases, it is only after 2 or 3 healthy cycles that attempting pregnancy again is advised. This is an area in which skillfully applied TCM treatment brings great benefit and may, in the long term, be a sounder approach than the prevailing medical attitude which advises getting back on your feet and trying to conceive again as soon as possible.
• Recurrent miscarriage: preventing future miscarriages. If a woman has had two or three or more miscarriages, then it is more likely that a problem exists in one of the would-be parents. The aim of treatment will be to prevent future miscarriages and, in this case, the couple is asked to refrain from attempts to conceive for at least 3–6 months while the male or female partner is being treated.
Chinese medicine can realistically be expected to have a very useful impact on the treatment of recurrent miscarriage because it is the constitution of the would-be parent that is being treated, not the pregnancy or the fetus.
Threatened Miscarriage
The first signs of a miscarriage are some bleeding and cramping in the abdomen or lower back pain. If the pregnancy is in the very early stages (i.e., the period is late by only 1 week or less), then the woman may just experience what feels like a heavy period. Since the only evidence of pregnancy is the positive blood test for hCG, these are called subclinical miscarriages of biochemical pregnancies. As a rule, the flow of blood will carry all the products of conception out and a surgical procedure like a dilatation and curettage (D&C) to clear out the uterus is not necessary.
Later-stage miscarriages, called clinical miscarriages, occur after the pregnancy has already been well established, i.e., if there has been an ultrasound it reveals the gestational sac and maybe a heart beat. This sort of miscarriage can involve heavy clotty bleeding, pain and cramping, and shock. Where the pregnancy is more advanced, a D&C will often be recommended to resolve the miscarriage and ensure no pregnancy products remain.
If bleeding during pregnancy occurs without pain and examination by a doctor shows the cervix to be firmly closed, then a miscarriage is not inevitable. The bleed may just be reflecting some process in the endometrium as the new placenta starts to form and exchange blood vessel surfaces with those of the mother. A transvaginal ultrasound will usually reveal all; if the gestational sac and the embryo are the normal size for their age and the heart beat is obvious, then there is every likelihood that the pregnancy will develop normally despite some early bleeding. If, however, the gestational sac is too small or the heart beat is absent or too slow at a time when it should be well developed, then a miscarriage will likely follow the bleeding. Most fetuses which miscarry in the 1st trimester (first 3 months) show abnormal development. For the remaining miscarriages in which there is normal development and normal chromosomes, there is likely to be a hormonal, immunological, or emotional cause. Miscarriages occurring for one of these latter reasons are more common among couples who have recurrent miscarriage (described below).
Other causes of a threatened miscarriage (which is not part of a recurrent miscarriage pattern) include isolated events such as a high fever or drug or alcohol abuse, which can cause fetal death.
Causes of threatened miscarriage
Infections, fevers, and accidents
Fever at the time of ovulation can disturb cell division and lead to chromosomal abnormalities, which means, if that particular egg is fertilized the fetus will probably not be viable and miscarriage will follow. Fever during the 1st trimester of the pregnancy can also cause abnormalities in the baby, followed by miscarriage (or in rare cases, a baby with a malformation like a short or absent limb). High fever during pregnancy is usually managed effectively with paracetamol and lots of fluids and bed rest. Chinese herbs to reduce Heat and resolve the causative factor (usually a virus or in TCM terms a Wind-Heat or Wind-Cold attack) can also be useful if applied quickly.
Sometimes, infections are already present in the endometrium before conception and the inflammation they cause (endometritis) can irritate the fetal membranes and cause premature contractions of the uterus. If we are aware of a history of pelvic inflammation or diagnose it from the signs and symptoms the Chinese medicine doctor recognizes as Heat or Damp-Heat, then treatment can be applied to remove the Heat and inflammation and an attempt made to save the pregnancy. Of course it is always preferable to deal with endometritis before conception if possible (see Ch. 5). Sometimes, infections reach the fetus from the outside through the cervix, causing fetal death and a miscarriage. Rapid diagnosis and treatment may be helpful, but often the harm is done before the diagnosis is made.
Other infections which can damage a fetus directly – i.e., by crossing the placenta from the mother’s bloodstream – include German measles virus (rubella), the chickenpox virus (herpes zoster), the genital herpes virus (herpes simplex), cytomegalovirus, bacteria such as those causing syphilis and tuberculosis and parasites such as those causing toxoplasmosis and malaria. If the damage to the fetus is serious, then it will miscarry. Sadly, in some cases of rubella and syphilis infection, the baby will survive but be born with serious abnormalities. These infections are not the cause of recurrent miscarriages, because the woman usually develops an immunity to them after the first infection.
Infections in the genitourinary tract which are active at the time of pregnancy increase the risk of 2nd trimester miscarriage about three times over normal.7
A history of sexually transmitted disease often causes problems with becoming pregnant rather than with staying pregnant (see Ch. 6).
Accidents such as serious falls or shocks are sometimes blamed for miscarriages. From a TCM point of view, falls and injuries can cause Blood stagnation, which may manifest as a disorder of blood flow in the placenta or endometrium. In addition, the TCM doctor recognizes that shock can affect the Heart and obstruct the Bao vessel, an important channel for controlling Blood to the Uterus and therefore for nourishment of the fetus.
Strain of the lower back associated with lifting heavy loads can also cause a miscarriage. Studies with physiotherapists, kitchen workers, and cleaners show that work which involves lifting and bending can increase the risk of miscarriage more than three times above normal.8
Strain and overuse of the lower back damages the Kidney energy which, you may recall from Chapter 4, is a crucial factor from a TCM point of view for a healthy pregnancy.
Alcohol and drugs
Alcohol or drug abuse, if extreme, can create such toxic conditions for the fetus that it cannot survive. Or they damage the mother’s health sufficiently that her body is unable to sustain the pregnancy (see also Recurrent miscarriage, below).
In TCM, such agents are usually said to create internal Heat, which at a certain level damages the endometrium. Long-term alcohol or drug abuse is usually accompanied by malnutrition; in TCM terms, this implies insufficient Qi and Blood to nourish a fetus.
Prescription drugs taken in early pregnancy can in some cases present a risk, e.g., there is some evidence that even commonly used drugs such as non-steroidal anti-inflammatory drugs (NSAIDs) can contribute to miscarriage.9 One study found that the use of NSAIDs (ibuprofen, naproxen, or aspirin) during early pregnancy increased the risk of miscarriage by 80%. The risk was much higher when NSAIDs were taken around conception or were used for longer than a week. It is thought that prostaglandin inhibition by NSAIDs might interfere with implantation.10 Paracetamol use is not associated with any increased risk of miscarriage.
Other drugs such as Roaccutane (isotretinoin) used to treat resistant acne are well known for their ability to cause defects in the embryo; when these are lethal enough, miscarriage will follow.
There is much more research to be done in this area; meanwhile, drugs should be avoided in early pregnancy if possible.
Hot baths
The use of hot tubs is also a risk factor for miscarriage, especially in the first few weeks of pregnancy. Women who use hot tubs or Jacuzzis (which keep the water temperature high) in early pregnancy are twice as likely to miscarry as those women who do not use them. The use of regular bathtubs does not seem to be a risk factor, but sustained elevation of core body temperature is best avoided, not only because of the risk of miscarriage but also the increase in neural tube defects associated with hyperthermia.11
Exposure to chemical agents (e.g., during the preparation of synthetic drugs or use of industrial or domestic cleaners) as either discrete events or on an ongoing basis, can also contribute to miscarriage (such agents are discussed in the Causes of recurrent miscarriage, below).
There has been some debate about the effects of the oral contraceptive pill on pregnancies which closely follow its use. Not all specialists are in agreement about the persisting effects of the pill and, indeed, most claim there is no lingering effect.12 However, some manufacturers of the pill have advised that it be stopped for 3 or 4 months before attempting pregnancy, claiming an increased risk of miscarriage immediately after using contraceptive hormones.13 Other surveys have noted that taking the pill for more than 2 years is associated with an increased risk of miscarriage.14 This may be due to persistent disruption of endometrial function caused by the pill, which can result in implantation difficulties for the embryo, or it may be because oral contraceptive use depletes folic acid stores, which puts at risk the development of the fetus in its first few weeks.
There is much Chinese medicine can contribute to preparing the endometrium and the cervix for a healthy and stable pregnancy after stopping the pill. Following the treatment regimens described in Chapter 4, with a special emphasis on building the Yin (to promote cervical mucus production) and regulating and then building the Blood and boosting Kidney Yang (to promote a healthy endometrium) should facilitate rapid reversal of any undesired effects of the pill.
We will discuss more causes of miscarriage below when we discuss recurrent miscarriages.
TCM treatment of threatened miscarriage
In the event of a threatened miscarriage, TCM intervention can sometimes play a useful role. It is one of those times when Chinese medicine doctors like to be more proactive than their Western medicine counterparts, who view early miscarriages as relatively trivial events from a physiologic point of view (though not from a psychological point of view). If the pregnancy can be saved, the TCM doctor will have something up his sleeve rather than just adopting a fatalistic attitude of wait and see. Obviously in many cases, there is little that can be done and the miscarriage is necessary to expel a defective embryo. But in cases where the problem lies with the mother or the way in which the pregnancy is being established, then timely treatment may save a pregnancy. If there is no lower back pain or bleeding, the pulse is slippery, the tongue is not purple and the abdomen feels warm, then the threatening miscarriage has more chance of being rescued.
Chinese medicine texts describe a threatened miscarriage as ‘fetal restlessness’ or ‘fetal bleeding’. The symptoms are spotting or bleeding in early pregnancy sometimes accompanied by lower back pain and abdomen cramping. If the pregnancy is threatened for reasons other than chromosomal embryopathy, then it is ideal if treatment is administered before bleeding starts. However, this may be difficult to assess. Doctors working in infertility clinics in China will closely supervise the first few weeks of an at-risk pregnancy. ‘At risk’ in this context means the pregnancy follows a period of infertility, or there has been a history of previous miscarriage. In these clinics, women may be encouraged to continue taking basal body temperature (BBT) readings for the first few weeks after the pregnancy is confirmed; that way, the doctor can determine the vigor of the Kidney Yang by the temperature readings. If the temperature starts to drop at all, Kidney Yang tonics (and Qi tonics) will be administered, or increased if they are already being taken. Similarly, blood levels of hCG and progesterone can be monitored and vaginal ultrasounds can be taken. However, although these tests can give accurate assessments of the progress of the pregnancy, to do them on a frequent basis may be prohibitively costly.
Categories of threatened miscarriage are:
Kidney deficiency
When we constructed treatment protocols for encouraging conception, in Chapter 4, we emphasized Kidney Yin. Once conception has occurred, then treatment of Kidney Yang is emphasized, i.e., the Uterus must be kept ‘warm’. It is Kidney Yang deficiency which is the most common cause of early-stage (subclinical) miscarriage and also pre-implantation loss (where there is no chromosomal embryopathy). In the case where a diagnosed pregnancy is threatening to miscarry there will be spotting or bleeding, which may be accompanied by lower back pain, sore legs and frequent urination.
The pulse will be weak and soft. This will be especially notable in the Kidney position, which in a healthy pregnancy should quickly develop a firm, solid and slippery feel. The tongue will be pale or unremarkable.
Herbal formula: The guiding formula in this situation is:
Shou Tai Wan (Fetus Longevity pill)
| Tu Si Zi | 20 g | Semen Cuscatae |
| Du Zhong | 9 g | Cortex Eucommiae Ulmoidis |
| Sang Ji Sheng | 9 g | Ramulus Sangjisheng |
| E Jiao | 9 g | Gelatinum Asini |
Tu Si Zi is the most important herb to prevent miscarriage due to Kidney deficiency. It has a strong supplementing effect on the Kidney, combined with an astringent effect; consequently, the dose used is often much larger than usual. However, doses above the level given above are not advised.
Xu Duan can be used instead of Du Zhong in this formula, as they both have the effect of strengthening the Kidney and preventing miscarriage. Sang Ji Sheng supports the Kidneys and with E Jiao nourishes Blood and prevents miscarriage; E Jiao also has the action of stopping bleeding.
More herbs can be added to stop bleeding if necessary, e.g.
| Ai Ye tan | 9 g | Folium Artemisiae |
| Zhu Ma Gen | 15 g | Radix Boehmeria Nivea |
It is common for Kidney deficiency miscarriage to also show signs of Qi deficiency. In that case, some of the herbs mentioned in the next category (Qi deficiency) will be added to the above guiding formula, e.g.
| Huang Qi | 20 g | Radix Astragali |
| Bai Zhu | 9 g | Rhizoma Atractylodis Macrocephalae |
| Dang Shen | 9 g | Radix Codonopsis Pilulosae |
If there is a history of chronic miscarriage, these Qi tonic herbs will always be used before and after conception to encourage the Spleen Qi to hold the fetus in.
Acupuncture points: Choose from the following points (and see Table 8.1):
Table 8.1
Acupuncture pointsa used in treatment of threatened miscarriage due to Kidney deficiency
| Treatment goal | Acupuncture points |
| To strengthen Kidneys, especially Kidney Yang | KI-6, KI-3, BL-23 (cautious shallow needling or moxa), Ren-4 (light moxa only) |
| To reinforce and lift Spleen Qi | Ren-6 (shallow needling or moxa), Ren-12, DU-20 |
aReinforcing method is used; moxa can be applied on trunk and head points.
| Ren-4 | Guanyuan |
| BL-23 | Shenshu |
| Ren-6 | Qihai |
| KI-3 | Taixi |
| KI-6 | Zhaohai |
| Ren-12 | Zhongwan |
| DU-20 | Baihui |
Qi deficiency
Qi dropping is another cause of clinical or subclinical (usually the former) miscarriage. The woman will experience abdomen distension, with a bearing down sensation that may spread to the lower back. She will probably feel fatigue and may notice spotting of blood. If the cervix is examined, it may appear to be slightly open. The pulse will be thready and the tongue swollen or pale.
Herbal formula: The formula of choice is:
Bu Zhong Yi Qi Tang (Reinforce the Center and Benefit the Qi decoction)
| Huang Qi | 30 g | Radix Astragali |
| Dang Shen | 15 g | Radix Codonopsis Pilulosae |
| Bai Zhu | 12 g | Rhizoma Atractylodis Macrocephalae |
| Dang Gui | 9 g | Radix Angelicae Sinensis |
| Chen Pi | 6 g | Pericarpium Citri Reticulate |
| Sheng Ma | 6 g | Rhizoma Cimicifugae |
| Chai Hu | 6 g | Radix Bupleuri |
| Gan Cao | 6 g | Radix Glycyrrhizae Uralensis |
Large doses of Qi tonics (Huang Qi, Dang Shen and Bai Zhu) are used to lift the fetus and the Uterus, their tonic effects being moderated by Chen Pi, which regulates Qi. Sheng Ma and Chai Hu both help to lift the fetus. Nourishment of the fetus is very important, especially in Qi and Blood-deficient women. Dang Gui and Bai Zhu are often used together to both nourish the Blood and the Qi and prevent miscarriage. However, Dang Gui does have a slight Blood-moving action, so if there is any bleeding it needs to be replaced with E Jiao. Gan Cao (used here in a smaller dose than regular Bu Zhong Yi Qi Tang formulations) reinforces the Qi and moderates and harmonizes the actions of the other herbs.
If the cervix appears to be opening, add the following astringent herbs:
| Jin Ying Zi | 9 g | Fructus Rosae Laevigatae |
| Qian Shi | 9 g | Semen Euryales Ferox |
Both these herbs can astringe the Jing, and in these circumstances can help hold in the fetus.
Additionally, one of the following can be added to further the astringing effect:
| Sang Piao Xiao | 9 g | Ootheca Mantidis |
| Hai Piao Xiao | 9 g | Os Sepiae seu Sepiellae |
Sang Piao Xiao astringes and strengthens the Kidneys and Hai Piao Xiao stops bleeding.
If necessary, more herbs can be added to control bleeding:
| Ai Ye tan | 9 g | Folium Artemisiae |
| Zhu Ma Gen | 15 g | Radix Boehmeria Nivea |
and replace Dang Gui with:
| E Jiao | 9 g | Gelatinum Asini |
and replace Chen Pi with:
| Sha Ren | 6 g | Fructus seu Semen Amomi |
If there is lower back pain, add Kidney Yang tonics:
| Tu Si Zi | 9 g | Semen Cuscatae |
| Bu Gu Zhi | 6 g | Fructus Psoraleae |
Acupuncture points: Choose from the following points (and see Table 8.2):
| DU-20 | Baihui |
| Ren-12 | Zhongwan |
| BL-20 | Pishu |
| ST-36 | Zusanli |
| Ren-6 | Qihai |
| KI-3 | Taixi |
Blood deficiency
Blood deficiency is not a direct cause of threatened miscarriage, but it can compromise the health and development of the fetus. This may be more apparent in the later stages of pregnancy, after the first 2 or 3 months. If the mother is anemic, or the ultrasound shows that the fetus is small-for-dates, then the addition of Blood tonics is timely and useful. Diet and rest are also important considerations for the mother and she will need iron supplements if her diet is inadequate. Symptoms include fatigue, palpitations and pallor. The pulse will be weak and the tongue pale.
Table 8.2
Acupuncture pointsa used in the treatment of threatened miscarriage due to Qi deficiency
| Treatment goal | Acupuncture points |
| To support the Spleen Qi | Ren-12, BL-20 and ST-36 |
| To lift the Qi | DU-20 and Ren-6 |
| To support the Kidneys | KI-3 |
Herbal formula: The formula of choice is:
Dang Gui Shao Yao San (Angelica Peonia powder) modified
| Dang Gui | 9 g | Radix Angelicae Sinensis |
| Bai Shao | 15 g | Radix Paeoniae Lactiflorae |
| Fu Ling | 9 g | Sclerotium Poriae Cocos |
| Bai Zhu | 9 g | Rhizoma Atractylodis Macrocephalae |
| Ze Xie | 9 g | Rhizoma Alismatis |
| Dan Shen | 6 g | Radix Salviae Miltiorrhizae |
| (Zhi) Gan Cao | 3 g | Radix Glycyrrhizae Uralensis |
This modified formula, originally designed to treat abdomen pain in pregnancy, stimulates blood production with tonics such as Dang Gui and Bai Shao and encourages its supply to the fetus via the placenta. Dan Shen encourages circulation in the endometrium and placenta. Studies in China have shown that if fetal growth is retarded it can, in some circumstances, be accelerated with the use of Dan Shen, although of course this herb must be used very cautiously. Chuan Xiong has been removed from this version of Dang Gui Shao Yao San because in combination with Dang Gui, it has been shown to initiate uterine contractions. Bai Zhu, Fu Ling and Ze Xie work together to support Spleen function in production and circulation of Qi and fluids. (Zhi) Gan Cao harmonizes the various actions of these herbs. If there is any bleeding (in the absence of Blood stagnation), then Dang Gui and Dan Shen should be replaced with:
| E Jiao | 9 g | Gelatinum Asini |
| He Shou Wu | 9 g | Radix Polygoni Multiflori |
Blood tonics like Shu Di are too greasy for most women to digest in early pregnancy and may severely exacerbate any nausea they are experiencing. If Shu Di is prescribed then it is wise to add Sha Ren.
If the Spleen Yang and Kidney Yang of the mother are weak, this can also contribute to a small-for-dates fetus because nutrients from food will not be satisfactorily extracted and distributed and Blood production will be compromised. Also, the fundamental support (the Kidneys) for fetal development will be inadequate.
In such cases, add the Kidney and Spleen tonics:
| Du Zhong | 12 g | Cortex Eucommiae Ulmoidis |
| Tu Si Zi | 9 g | Semen Cuscatae |
| Dang Shen | 9 g | Radix Codonopsis Pilulosae |
Acupuncture points: Choose from the following points (and see Table 8.3):
Table 8.3
Acupuncture pointsa used in the treatment of threatened miscarriage due to Blood deficiency
| Treatment goal | Acupuncture points |
| To reinforce Spleen function to manufacture Blood | Ren-12 and ST-36 |
| To harmonize the Qi and Blood in the Chong and Ren channels | KI-5 and KI-3 |
| To encourage local blood supply and nourish the fetus; these points are used if there is no bleeding and the cervix is firm but ultrasound indicates that the baby is not growing | ST-29, KI-13 (light moxa) |
aUse reinforcing method and on the lower abdomen points use moxa.
| Ren-12 | Zhongwan |
| ST-36 | Zusanli |
| ST-29 | Guilai (moxa only) |
| KI-13 | Qixue |
| KI-5 | Shuiquan |
| KI-3 | Taixi |
Heat in the Blood
The Heat responsible for a threatened miscarriage usually arises from Yin deficiency and may threaten the pregnancy in its early stages, especially if it dries the endometrium and forces blood from the uterine blood vessels. Other factors which can contribute to creating a critical level of Heat in the Blood are anger (Liver-Fire) and a very pungent spicy diet. If the Heat affects the Heart, then there is a high risk of miscarriage because the Heart-Uterus connection via the Bao vessel can be disturbed. TCM theory posits that the Heart Qi has much to do with ‘opening’ of the Uterus and, when its Qi is disturbed (e.g., by Liver-Fire), the disruption in the Bao vessel may precipitate an untimely opening of the Uterus. For this reason, the cautious doctor is ever mindful of the Heart and Kidney relationship in early pregnancy. What this means is that the mental and emotional state of the newly pregnant woman can influence the pregnancy and a skillful doctor will take measures to safeguard the fetus by using acupuncture or herbs to calm the woman’s mind if she is excessively anxious or agitated.
A third factor which may contribute to Heat in the Blood is infection, most commonly in the endometrium itself. In the case of bacterial infection, antibiotics are usually given with Chinese herbs. And in the case of high fever, paracetamol is given to bring the temperature down until the herbs can effectively clear the Heat. Examination of the BBT readings taken after pregnancy is confirmed may show consistently and unusually high readings (e.g., 37.4°C or 98.8°F and up) and the woman may feel restless, thirsty, and hot. She may also be constipated with dry stools and the urine may appear dark. Uterine bleeding will be fresh red. The pulse will usually be rapid, while the tongue appears red. In this case, the Heat must be quickly cleared from the Blood (and Liver and Heart), while the Uterus must remain warm enough to nourish the fetus.
Herbal formula: The formula of choice is:
Bao Yin Jian (Protecting the Yin decoction)
| Sheng Di | 20 g | Radix Rehmanniae Glutinosae |
| Shan Yao | 12 g | Dioscorea Oppositae |
| Bai Shao | 9 g | Radix Paeoniae Lactiflorae |
| Huang Qin | 9 g | Radix Scutellariae Baicalensis |
| Huang Bai | 9 g | Cortex Phellodendri |
| Xu Duan | 9 g | Radix Dipsaci |
| Gan Cao | 3 g | Radix Glycyrrhizae Uralensis |
A large dose of Sheng Di cools the Blood to protect the Yin, while Huang Bai and Huang Qin remove Heat and Damp (infection) from the Blood and the lower body. Xu Duan ensures herbs do not cool the Uterus too much and protects the Kidney Yang. Bai Shao soothes the Liver Yin and Shan Yao, the Spleen Yin.
| Nu Zhen Zi | 9 g | Fructus Ligustri Lucidi |
| Han Lian Cao | 9 g | Herba Ecliptae Prostratae |
| Bai Mao Gen | 9 g | Rhizoma Imperatae Cylindricae |
| Di Yu (tan) | 9 g | Radix Sanguisorbae Officinalis |
| Qian Cao Gen | 10 g | Radix Rubiae Cordifoliae |
Acupuncture points: Choose from the following points (and see Table 8.4):
Table 8.4
Acupuncture pointsa used in the treatment of threatened miscarriage due to Heat in the Blood
| Treatment goal | Acupuncture points |
| To cool the Blood and stop bleeding | SP-1 and SP-10 |
| To clear Yin-deficient Heat | KI-2 |
| To clear Heat and stop bleeding | KI-8 |
| To clear Heart-Fire, Heat in the Blood and safeguard the Bao vessel | HE-5 |
| To clear Liver-Fire | LIV-2 |
| To clear Heat from the Blood | PC-3 |
| To calm the spirit | PC-6 |
aReducing or even method is used on these points, except SP-10 and KI-8, which should be needled cautiously with little manipulation.Moxa is used on SP-1.
| SP-1 | Yinbai |
| SP-10 | Xuehai |
| KI-2 | Rangu |
| LIV-2 | Xingjian |
| PC-3 | Quze |
| KI-8 | Jiaoxin |
| HE-5 | Tongli |
| PC-6 | Neiguan |
The patient must be advised to avoid heating foods such as curries and drink such as alcohol and coffee. Also, she should be kept as calm as possible.
Blood stagnation
This cause of threatened miscarriage may occur after a fall or accident has caused some trauma or bruising to the uterus. It may also occur after IVF procedures. There are also some situations where Blood stagnation has preceded the pregnancy (e.g., endometriosis, endometritis, polyps and fibroids), and is contributing to bleeding from the uterus during the pregnancy. Sharp or gnawing crampy abdominal pain will accompany the bleeding, which may be dark or clotty. The tongue may appear purplish and the pulse will have a choppy feel.
Treatment of such a condition is not without risk. Treatment must aim to clear the Blood stagnation but without dislodging the fetus. Some doctors prefer a conservative approach first, and will apply treatment to strengthen the Kidneys and to lift the Qi before initiating any other treatment. However, if this is not successful, then a careful approach can be taken using herbs.
Herbal formula: The formula of choice is:
Jiao Ai Si Wu Tang (Gelatinum Asini Artemesia Four Substances decoction) modified
| E Jiao | 9 g | Gelatinum Asini |
| Ai Ye | 9 g | Folium Artemisiae |
| Dang Gui | 9 g | Radix Angelicae Sinensis |
| Bai Shao | 9 g | Radix Paeoniae Lactiflorae |
| Dan Shen | 9 g | Radix Salviae Miltiorrhizae |
| Wu Ling Zhi | 9 g | Excrementum Trogopterori |
| Pu Huang | 9 g | Pollen Typhae |
| Gan Cao | 6 g | Radix Glycyrrhizae Uralensis |
| Xu Duan | 9 g | Radix Dipsaci |
Dang Gui, Dan Shen, Wu Ling Zhi, and Pu Huang regulate the Blood. The latter two herbs have been found to be particularly safe in clinics in China in terms of fetus stability. Most other Blood-regulating herbs are too risky to use in early pregnancy. As with the formula Dang Gui Shao Yao San mentioned earlier, Chuan Xiong has been removed because in combination with Dang Gui it can initiate uterine contractions. E Jiao and Ai Ye stop bleeding and Xu Duan, used in this particular context, not only protects the Kidney Yang but also helps invigorate the Blood. Wu Ling Zhi can be a difficult herb to take in decoction if there is much morning sickness because of its smell, so it is recommended this formula be dispensed in granules which are put into capsules.
Acupuncture points: Choose from the following points (and see Table 8.5):
Table 8.5
Acupuncture pointsa used in the treatment of threatened miscarriage due to Blood stagnation
| Treatment goal | Acupuncture points |
| To regulate Blood and remove stasis and relieve abdomen pain | PC-6, ST-29 and SP-10 |
| To hold the fetus secure while stagnation is being addressed | DU-20 and Ren-12 |
aReinforcing technique is used for DU-20 and Ren-12; even method needling for others. Particular care (i.e. no manipulation) must be taken with ST-29 and SP-10.
| DU-20 | Baihui |
| Ren-12 | Zhongwan |
| PC-6 | Neiguan |
| ST-29 | Guilai |
| SP-10 | Xuehai |
Western medical treatment for threatened miscarriage
In Western gynecology clinics, the hormone progesterone may be given in a short course (as progestogens) to try to prevent a threatened miscarriage, although it is generally recognized not to be very effective. From a TCM point of view, progestogen is seen to have warm and Qi raising activity. Viewed like this, the hormone may be of some use in the Kidney Yang deficiency or the Qi deficiency type of threatened miscarriage (used over the long term, however, this drug can harm Kidney Yang and Qi). For threatened miscarriage related to Blood deficiency, Heat or stagnation progestogens have no theoretical application. Progestogens also tend to exacerbate Damp accumulation and would be contraindicated in women of Damp constitution.
Inevitable Miscarriage
If the fetus has stopped growing or is abnormal and has died in the 1st trimester of pregnancy (a missed abortion), the TCM doctor will apply treatment on the basis of the following procedures.
Ensuring expulsion of all pregnancy products
This is achieved by using herbs and acupuncture which move stagnant Blood.
Herbal formula: The formula of choice is:
Sheng Hua Tang (Generating and Dissolving decoction)
| Dang Gui | 25 g | Radix Angelicae Sinensis |
| Chuan Xiong | 9 g | Radix Ligustici Wallichii |
| Tao Ren | 9 g | Semen Persicae |
| Pao Jiang | 3 g | Rhizoma Zingiberis Officinalis |
| (Zhi) Gan Cao | 3 g | Radix Glycyrrhizae Uralensis |
Large doses of Dang Gui and other herbs to move stagnant Blood are used for a limited time (usually 2–5 doses) to ensure the expulsion of the fetus, at the same time regenerating new Blood. Pao Jiang warms the channels and moderates the effect of the Blood-moving herbs so that there is no excessive blood loss.
Acupuncture points: Acupuncture treatments which encourage expulsion of all the uterine contents include abdomen points on the Chong, Spleen and Stomach channels such as the following (see also Table 8.6):
Table 8.6
Acupuncture pointsa used in the management of inevitable miscarriage to ensure expulsion of all pregnancy products
| Treatment goal | Acupuncture points |
| To move Blood and Qi in the Chong vessel | KI-14 and KI-18 |
| To regulate Blood in the Uterus | ST-28 and ST-29 |
| To regulate Qi and Blood in the abdomen and relieve pain | SP-12 and SP-13 |
| To effect a downward and clearing movement | SP-6 and CO-4 |
| KI-14 | Siman |
| KI-18 | Shiguan |
| ST-29 | Guilai |
| ST-28 | Shuidao |
| SP-12 | Chongmen |
| SP-13 | Fushe |
Two or three of these abdomen points should be chosen (perhaps according to sites of pain if relevant) and can be combined with:
| SP-6 | Sanyinjiao |
| CO-4 | Hegu |
to expel all the contents of the uterus.
Control the amount of blood lost
Herbal formula: The formula of choice is:
Tao Hong Si Wu Tang with Shi Xiao San (Persica Carthamus Four Substances decoction with Return the Smile powder) modified
| Dang Gui | 9 g | Radix Angelicae Sinensis |
| Chuan Xiong | 6 g | Radix Ligustici Wallichii |
| Shu Di | 12 g | Radix Rehmanniae Glutinosae Conquitae |
| Bai Shao | 9 g | Radix Paeoniae Lactiflorae |
| Tao Ren | 6 g | Semen Persicae |
| Hong Hua | 3 g | Flos Carthami Tinctorii |
| Pu Huang tan | 9 g | Pollen Typhae |
| Wu Ling Zhi | 6 g | Excrementum Trogopterori |
| Qian Cao Gen | 6 g | Radix Rubiae Cordifoliae |
| San Qi | 6 g | Radix Pseudoginseng |
When herbs are used to stop bleeding in cases like this, we must be careful not to prescribe those which can exacerbate Blood stagnation. Examples of safe styptic herbs, which stop bleeding but do not cause Blood stasis, are San Qi, Qian Cao Gen and Pu Huang. Dang Gui, Shu Di and Bao Shao nourish Blood in an attempt to replace what has been lost. Tao Ren, Chuan Xiong, Wu Ling Zhi and Hong Hua are used in small doses to clear Blood stasis.
Acupuncture points: Controlling blood loss can be achieved with acupuncture treatments similar to those used for heavy periods with Blood stagnation. Use the following points (and see Table 8.7):
Table 8.7
Acupuncture pointsa used in the management of inevitable miscarriage to control blood loss (in conjunction with points in Table 8.6)
| Treatment goal | Acupuncture points |
| To regulate Blood stagnation and stop bleeding | SP-10 |
| To stop bleeding | LIV-1 |
| To reinforce the Qi to control heavy bleeding | Ren-6 |
| SP-10 | Xuehai |
| Ren-6 | Qihai |
| LIV-1 | Dadun |
These points are added to some abdomen points chosen from the list given in Table 8.6. SP-6 and CO-4 will not be used if the bleeding is heavy.
Recover the Qi and Blood
Even early-stage miscarriages are draining on the woman’s energy, and this needs to be addressed as soon as the products of the miscarriage are expelled and bleeding is controlled.
Herbal formula: The formula of choice is:
Ba Zhen Tang (Eight Precious decoction)
| Shu Di | 15 g | Radix Rehmanniae Glutinosae Conquitae |
| Dang Gui | 9 g | Radix Angelicae Sinensis |
| Bai Shao | 9 g | Radix Paeoniae Lactiflorae |
| Chuan Xiong | 6 g | Radix Ligustici Wallichii |
| Dang Shen | 12 g | Radix Codonopsis Pilulosae |
| Bai Zhu | 9 g | Rhizoma Atractylodis Macrocephalae |
| Fu Ling | 9 g | Sclerotium Poriae Cocos |
| Gan Cao | 3 g | Radix Glycyrrhizae Uralensis |
This well-known formula combines four Blood tonics (Dang Gui, Bai Shao, Chuan Xiong, Shu Di) with four Qi tonics (Dang Shen, Bai Zhu, Fu Ling, Gan Cao). In pill form, it is known as Women’s Precious Pills and is used in many situations that require tonics.
Acupuncture points: Choose from the following points (and see Table 8.8):
Table 8.8
Acupuncture pointsa used in the recovery from miscarriage
| Treatment goal | Acupuncture points |
| To stimulate Spleen and Stomach function in producing Blood | ST-36, Ren-12, BL-20, SP-6 |
| To reinforce Qi | Ren-6 |
| To supplement Blood | BL-17, SP-10 |
| ST-36 | Zusanli |
| Ren-12 | Zhongwan |
| SP-6 | Sanyinjiao |
| Ren-6 | Qihai |
| BL-20 | Pishu |
| BL-17 | Geshu |
| SP-10 | Xuehai |
Late-stage miscarriage
In the case of the inevitable miscarriage which happens later in the pregnancy (after week 10 or 12), a dilatation and curettage (D&C) will usually be performed. Herbs and acupuncture can be used to reinforce the clearing out
of the uterus (although in most cases I think this is unnecessary). In the event that some products of pregnancy remain after a D&C, then the formula Sheng Hua Tang (see above) with additions of more Blood-moving herbs such as:
| Hong Hua | 6 g | Flos Carthami Tinctorii |
| Yi Mu Cao | 12 g | Herba Leonuri Heterophylli |
can be administered for several days.
Acupuncture treatments applied with strong reducing technique to points such as those described in Table 8.6 encourage expulsion of any retained tissue.
Because miscarriages are very weakening to the body, especially if there has been a significant amount of blood lost, treatments such as those described above need to be applied with caution and the patient’s response watched closely. Treatments which strongly move Blood and Qi can be damaging to the Zheng Qi (the upright Qi) of the body. It will be important in cases where such strong treatments are applied to quickly follow-up with recovery treatments as soon as all the pregnancy tissue is expelled from the uterus. Ba Zhen Tang (above) is a good guiding formula. If there has been significant blood loss, more Blood tonics can be added. Such tonics should be continued until the periods return.
The next stage of recovery from miscarriage involves the re-establishment of a healthy menstrual cycle. This is done using the methods we have described in Chapter 4 once the period returns. If a lot of blood has been lost, this may take some time. As the new cycle is established again, so is the mind gradually healed of its grief, and confidence in the ability to create a new pregnancy returns. Attempts to conceive again can resume in a couple of cycles if recovery is rapid and the circumstances are favorable.
Recurrent Miscarriage
Prevention of future miscarriage
Recurrent miscarriage is so defined after three consecutive miscarriages. However, investigations, and treatment if applicable, should be initiated after two miscarriages if the couple is worried or not so young. Or if the miscarriage occurs after a period of infertility, investigation may be initiated immediately because there is a chance that the miscarriage was caused by whatever is causing the infertility.
Chinese medicine has always recognized that it is often the same sorts of imbalances that can cause difficulty in becoming pregnant and difficulty in staying pregnant. You will see that the types of diagnoses a Chinese medicine doctor makes in the case of recurrent miscarriages are very similar to those that describe different categories of infertility.
Having a miscarriage is not such an uncommon event; it occurs in 10–25% (or more in older women) of all diagnosed pregnancies. However, only 1–3% of couples will suffer recurrent miscarriages. Women who already have a history of miscarriage are more likely to have miscarriages in the future (unless a treatable cause is addressed).15,16 Clearly, there are persisting risk factors in a number of recurrent miscarriers; discovering and treating these is what this section is about.
Western gynecologists can track down reasons for recurrent miscarriages in some cases and can administer appropriate treatment for a few of these, e.g., physical problems in the uterus and cervix. However, miscarriages can result from some unknown factor in a complex series of interactions between the mother’s womb and fetus and environment.
Researchers have noted that the lining of the womb is capable of recognizing and responding to developmentally abnormal embryos but only when adequately prepared (decidualized) for pregnancy.17 And that the ability of the endometrium to decidualize is grossly defective in women suffering from recurrent miscarriages.18
Some researchers have called this the ‘non fussy’ uterus, i.e., one which is not selective enough about the embryos it accepts. These women fall pregnant all too easily. It appears a filter that the properly prepared uterus offers is not operating.
It is often difficult to isolate just one cause of repeated miscarriage, and it can be even more difficult to provide effective treatments. Medical specialists have tried many remedies for miscarriage; some, like thalidomide and DES (diethylstilbestrol) had devastating effects and some have no proven effects (namely progesterone and hCG).
Similarly, through the ages, claims have been made for many herbal and other remedies to stop miscarriages – but controlled clinical trials are generally lacking. One trial looked at a number of women who conceived via IVF and then took Chinese herbs or progesterone. The miscarriage rate in the group who took the Chinese herbs was significantly less (13%) than that in the progesterone group (23%).19
Another group of researchers looking for adverse effects of chinese medicine treatments for threatened miscarriages found none and also found that such interventions were more effective than Western medicine ones.20 However, the main proof we have that TCM treatment for recurrent miscarriage offers some valid outcome is its performance in the living People’s Laboratory of China, where it has been employed for thousands of years and is still in use today, even in areas where modern pharmaceuticals are available. Eventually, Chinese medicine will be tested in the scientific laboratories of the West and, if valid and ethical experimental protocols can be put in place, interesting results should emerge. Until then, the practitioners of Chinese medicine have at their disposal the advice and wisdom distilled over many hundreds of years of doctors treating women who have suffered miscarriages. If the treatments these doctors have repeatedly applied over such a long period of time did not work, then they would not have stayed in the TCM repertoire.
Causes of recurrent miscarriage
Below are listed the known causes of recurrent miscarriage or pregnancy loss. Some of these are easily remedied, others not so easily. Genetic, endocrine or autoimmune causes are found in the majority of couples who suffer from repeated miscarriages. Other causes include structural and environmental factors.
Cervical incompetence and uterine malformations
If the cervix is unable to stay firm and closed because it has been weakened by previous obstetric or surgical trauma, then it can shorten and open sometime after the 14th week of pregnancy. The incompetent or insufficient cervix, as it is called, then releases the contents of the uterus with a gush of fluid and the pregnancy comes to an abrupt end. In women where an incompetent cervix is suspected, a suture can be added to hold the cervix closed, but where it is not suspected, the miscarriage happens suddenly and without warning other than some back pain and possibly some discharge. The use of a suture is the treatment of choice where cervical incompetence is suspected. The Chinese medicine practitioner can offer treatment to aid the lifting of the uterus and the fetus, i.e. take the pressure off the cervix, but this treatment is adjuvant to a surgical aid.
Other abnormalities such as large fibroids causing uterine distortion or congenital abnormality of the uterus may also contribute to the loss of a normally developing fetus. Ironically, women whose mothers took DES to prevent a miscarriage have double the rate of miscarriage themselves due to deformities of the uterus.21 In addition to increased risk of pregnancy loss, the incidence of fetal malposition and pre-term labor are higher in women with uterine abnormalities.
For serious uterine deformity, the advice of an experienced surgeon is essential. There are many different ways a uterus can be deformed, some of them congenital and some of them acquired from previous surgical procedures. Some of these deformities can be corrected surgically and some are better left alone, despite the higher miscarriage rates.22
Chinese medicine offers little in the way of treatment for serious malformations of the uterus.
Hormonal causes
Ovary
The ovary, or more precisely, the corpus luteum, is responsible for producing the progesterone which maintains the first few weeks of the pregnancy until the placenta can take over. While low progesterone levels are commonly associated with pregnancies which miscarry, giving women progesterone in early pregnancy does not improve pregnancy outcome.
This is because low progesterone levels reflect the fact that the pregnancy has not implanted successfully in the first place and this usually relates to the quality of the egg and the embryo.
If there are problems with ovarian function, e.g., in polycystic ovary syndrome (PCOS) or resistant ovaries disease or premature menopause, which contribute to infertility, there is a strong chance the same problem will increase the risk of miscarriage should a pregnancy occur.
The mechanisms for this are not clearly understood from a Western medicine point of view. However, the TCM doctor will be able to make a diagnosis for miscarriages which occur repeatedly during early pregnancy due to lack of hormonal support from the ovary. Often simply rectifying a Kidney Yang weakness (and supporting Kidney Yin) before conceiving, will reduce miscarriage risk in this category.
Placenta
The placenta makes hCG, which stimulates the ongoing function of the corpus luteum, particularly its production of progesterone. Failure of the placenta to make this hCG means failure of the corpus luteum to produce progesterone and the pregnancy will not survive. Administration of hCG does not help for the same reason that administration of exogenous progesterone does not help.
For miscarriages due to placental dysfunction, Chinese medicine will approach diagnosis and treatment in the same way as for ovary dysfunction, focusing on strengthening Kidney function before conception.
Genetic or inherited disorders
Chromosomal studies of couples who have suffered recurrent miscarriage sometimes reveal constitutional genetic abnormalities, i.e., abnormalities in the chromosomes which they have been born with and which exist in all their cells in all parts of their bodies but which have not affected them in any damaging way. For example, one of the partners might carry a balanced translocation, which means a part of one chromosome has become transferred to another. This causes no problem to the partner with the translocation but can cause problems during gametogenesis when their chromosomes are divided in half to make the eggs or the sperm. Such gametes have a high degree of chromosomal abnormality and lead to abnormal conceptions, many of which are unviable and will miscarry or, more tragically, lead to the birth of children with multiple abnormalities. There is no treatment offered by allopathic medicine or by traditional Chinese medicine, which can change the genetic make-up of the prospective mother or father; however, in cases of balanced translocations, the couple can be reassured that not all conceptions will be doomed and that hopefully one day, they will conceive a normal baby – an unenviably fraught wait-and-see approach. Genetic analysis of embryos, preimplantation genetic diagnosis (PGD), before they are transferred to the uterus in an IVF protocol, provides a solution for some couples.
Genetic counsellors play an important role for someone diagnosed with a chromosomal abnormality. All the risks and possible outcomes can be explained by the genetic counsellor and an appropriate plan constructed.
Thrombophilias
Recurrent miscarriages occur in some women who have inherited conditions which increase their blood clotting tendency. Factor V Leiden; prothrombin gene mutations (in the gene that codes for MTHFR, an enzyme involved in folate metabolism); antithrombin III and plasminogen activator inhibitor-1 (PAI-1) are genetically determined factors that may increase the risk of miscarriage. If blood clots occur in the blood vessels of the placenta, the risk of 2nd trimester miscarriage or a small-for-dates baby is increased.
Immunologic disorders
Some autoimmune diseases (this means making antibodies to your own cells) and some alloimmune diseases (making antibodies to foreign cells) are associated with increased incidence of miscarriage. The term immune infertility refers to an inability to conceive or maintain a pregnancy because some aspect of the immune system prevents it. It has been proposed that there may be a syndrome in which the presence of various immune factors (natural killer (NK) cells, antiphospholipid antibodies, thyroid antibodies, etc.) increase the likelihood of an immune reproductive disorder. Examples are autoimmune conditions such as Grave’s disease, Hashimoto’s disease, systemic lupus erythematosus, antiphospholipid syndrome, scleroderma, psoriasis and Sjögren syndrome.
The mechanisms behind immune disorder pregnancy loss are not fully understood, although we do know that the antiphospholipid antibodies in acquired thrombophilias (also the proteins made by genes in inherited thrombophilias), prevent the placental cells from properly attaching to the uterine lining. These antibodies prevent the formation of the syncytiotrophoblasts which have an important role in the establishment and function of the placenta. With each pregnancy loss, there is an increased chance that the mother will develop antibodies to phospholipid molecules. For the doctor of Chinese medicine, this is evidence that miscarriages themselves can increase the risk of Blood stagnation.
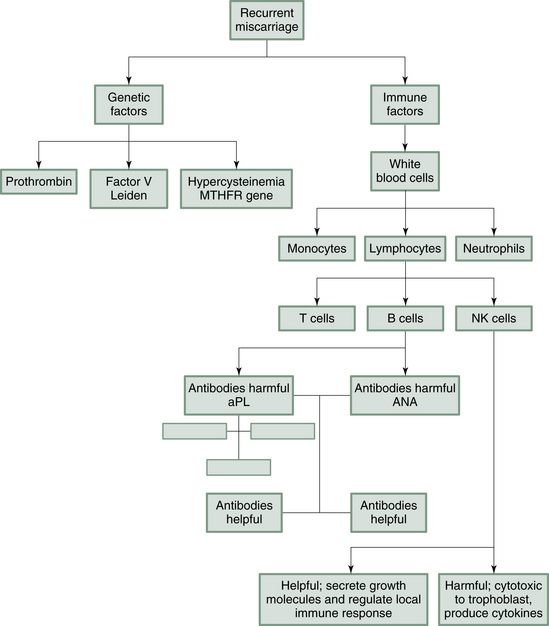
Elevated levels of NK cells have been shown to impede successful implantation or establishment of pregnancy, as have activated T lymphocytes.23 On the other hand, the actions of some T cells and NK cells are necessary to promote a favorable environment for implantation.24 It is largely through the secretion of signaling agents called cytokines released by these immune cells, that the intricate processes of implantation and creating a placenta can be either facilitated or stymied. Figure 8.2 summarizes the immune and clotting factors which can contribute to an increased risk of miscarriage.
In other cases, an overactive immune system may attack the gametes themselves, as is the case when excess macrophages phagocytize sperm in the female reproductive tract.
Miscarriages later in the pregnancy can be caused by clots in the blood vessels of the placenta blocking blood supply.
Medical treatment includes administration of low molecular weight Heparin to dissolve blood clots, steroids to dampen overactive NK cell activity and progesterone for its anti-inflammatory properties. These treatments are still the subject of controversy and research, e.g., studies of women with recurrent miscarriage have found little benefit for the use of aspirin or anticoagulants, even in women with known clotting tendencies.25 However, this medication is widely prescribed to women diagnosed with such factors.
Antibodies to the thyroid gland (thyroid autoimmunity is the most common autoimmune condition) double the chances of miscarriage even when the thyroid function appears to be normal.26,27 There is no current medical treatment to reduce thyroid antibodies but where this is associated with elevated TSH, small doses of thyroid hormone will be given.
There are some recent findings which indicate that endometriosis shows some characteristics of an autoimmune disease too. Again, there is no medical treatment which addresses this aspect of endometriosis directly, but Chinese medicine treatment of endometriosis will certainly take into account its inflammatory (Damp-Heat) and internal bleeding (Blood stasis) aspects.
Research examining the influence of acupuncture on the immune system is revealing interesting effects – the exact mechanisms are not yet clear and may turn out to be as intricate and as involved as the immune system itself. However it is the anti-inflammatory or immunosuppressive actions of acupuncture are of particular interest in the field of immune related pregnancy loss. Women with autoimmune disorders tend to have an imbalance between T helper 1 cell derived (pro-inflammatory) and T helper 2 cell derived (anti-inflammatory) cytokines. Correcting this Th1/Th2 balance has been a key strategy in the treatment of various immune disorders. One study has shown that this ratio may be reset by acupuncture which corrected an imbalance in Th1/Th2 derived cytokines TNF-α and IL4 (and also decreased pro-inflammatory cytokine interleukin IL1).28
Herbal formulas known to be helpful in reducing the risk of miscarriage related to Kidney and Spleen deficiency, have also been shown to correct a Th1/Th2 imbalance (in this case by increasing Interleukin 10 and decreasing Interleukin 2).29 Recent reviews on the effect of acupuncture on the immune system have concluded that appropriate and frequently applied acupuncture treatment can provoke sustained anti-inflammatory activity, without stimulation of pro-inflammatory cells.30,31 We know that stress affects the immune system, elevating levels of activated T cells which can reduce implantation rates of embryos. We also know that high resting levels of cortisol are linked with elevated markers of inflammatory processes in the body which may affect successful implantation of the embryo.32 Fortunately, acupuncture has been shown to exert a beneficial modulatory effect on such immune imbalances caused by anxiety and stress. In one study, the maximum effect on the immune system of women suffering heightened anxiety was measured 72 h after they received acupuncture and the effects of a course of acupuncture were still evident 1 month after it was completed.33 It is thought that the immunomodulatory effect of acupuncture may result from the increase in levels of endogenous opioids: endorphin, met-encephalin, leu-encephalin, and serotonin, all of which increase with acupuncture treatment. These neurotransmitters create a sense of relaxation and have immunomodulator effects on the immune system.34
In general, most research on treatment of autoimmune disorders with Chinese herbal remedies centers around the concepts of clearing Heat, reinforcing Yin, supporting Qi and resolving Blood stasis. One of the factors that is traditionally considered important at the time of early placental development is warm and flourishing Kidney Yang. Interestingly, deficiency of Kidney Yang and Wei Qi is thought by some Chinese Medicine scholars to contribute to disorders of the immune system.
Inflammatory markers are also affected by diet and weight loss,35 which is one reason that treatment for women diagnosed with immune system disorders will be advised to pay attention to their diet and take supplements such as omega-3 fatty acids, vitamin E and antioxidants which decrease inflammatory markers.
Alloimmune (distinct from autoimmune) origins of pregnancy loss occur when the mother rejects fetal tissue as foreign, which of course it is! Nature has devised schemes whereby the mother learns to tolerate the fetus, but if something goes wrong with this scheme, the mother produces antibodies to the fetus and miscarriage can follow. Some forms of immunotherapy have been devised by specialists, but clinical trials have produced conflicting results. Chinese medicine infertility specialists do not talk in terms of the immune system; however, several of the possible diagnoses for recurrent miscarriage will include immune system disorders, e.g. Kidney Yin deficiency with Heat or Blood stagnation.
Gynecological disorders
There is an increased chance of miscarriage with just about every cause of relative infertility or subfertility. In other words, most gynecological disorders which lower fertility will increase miscarriage risk.
Endometriosis
Pregnancies have been thought to be more at risk of miscarriage if there is active endometriosis at the time of conception. The exceptions are pregnancies achieved with IVF. Possibly, the high levels of hormones given during the IVF procedures help the stability of the pregnancy in the early days, so miscarriages are not unusually frequent.36
From a TCM perspective, most cases of endometriosis are associated with Kidney Yang deficiency and Blood stagnation (see Ch. 5), both of which can be associated with an increased risk of miscarriage. Treatment should be applied to correct these conditions well before pregnancy is attempted.
Polycystic ovary syndrome
PCOS is a complex condition which affects ovary function. Small cysts accumulate in the ovaries and the release of an egg may be sporadic rather than monthly. Those eggs which are released are not always mature or of good quality and, if fertilization is successful, the fetus may be compromised and the risk of miscarriage elevated. Similarly, because the hormonal environment is abnormal in PCOS, conditions in early pregnancy are not always optimum. Women with PCOS who conceive with IVF have been reported to have higher than normal miscarriage rates.37
There are many reasons, including Kidney deficiency and obstruction to the Chong and Ren vessels which may account for the observed increase in miscarriages in PCOS patients (see Ch. 5).
Endometritis
Infection in the endometrium causes inflammation (called endometritis), which can increase risk of miscarriage by irritating the fetal membranes and causing premature contractions of the uterus. If there is a history of pelvic inflammation or infection (pelvic inflammatory disease or PID), then vigorous and persistent treatment must be applied to correct the condition before it contributes to future pregnancy loss. In cases of low-grade but chronic PID, antibiotics have limited effectiveness; acupuncture, especially the use of abdomen points, and strong Damp-Heat clearing herbal formulas, on the other hand, are usually quite effective (see Ch. 5).
Amenorrhea
Clearly amenorrhea and anovulation contribute in a very obvious way to infertility and sometimes the conditions which inhibit ovulation can also compromise a pregnancy should one occur (perhaps as a result of drug treatment to induce ovulation). For example, amenorrhea caused by extreme weight loss is often associated with significant under-nutrition. If an ovulation and a pregnancy should happen to occur in these circumstances, then the ability of the mother to sufficiently nourish her baby may be inadequate. From a TCM point of view, this situation would be described as Blood and Qi deficiency, a common cause of a small-for-dates fetus and sometimes of fetal death and miscarriage. Loss of periods related to drug use might create similar conditions and any closely following pregnancy will be at risk of miscarriage. The hormonal imbalances which lead to amenorrhea indicate a Kidney disorder in TCM terms (see Ch. 5) and until this is corrected, any pregnancies which might eventuate will be precarious.
Blocked tubes
Damage to the tubes which causes absolute obstruction creates sterility, but if this is overcome using IVF technology, the tubal pathology will have little impact on the outcome of the pregnancy and generally, the risk of miscarriage is lower in this category than in other types of IVF patients.
Other types of blockages in the fallopian tubes caused by mucus or secretions can be dealt with in a number of ways, including the mechanical clearing of the tubes, which occurs during a tube X-ray (HSG) or ultrasound (HyCoSy), or the application of acupuncture and the use of Damp-clearing herbs. However, if the Damp is not cleared adequately (e.g., if the tubes are cleared mechanically and there is no systemic treatment), then there is an increased risk of pre-implantation loss of the embryo because the endometrium may be too ‘slippery’ or fluid from the fallopian tubes may wash the embryo off the endometrial surface.
Fibroids and polyps
Fibroids which are large or numerous enough to occupy a significant part of the uterine cavity reduce the chances of falling pregnant and increase the risk of miscarriage if pregnancy does occur. This is because the available area for implantation of the embryo or adequate placental development on the uterine wall is reduced. Some late-stage miscarriages are attributed to the failure of placental development due to obstruction by fibroids. In the case of large and numerous fibroids, specialists will often recommend their removal before pregnancy is attempted. This sort of surgery is major and requires long recovery time, but in a young and healthy woman, will usually increase fertility and certainly reduce the risk of miscarriage. Some women choose to use Chinese medicine to address the problem of fibroids, with mixed results. If the woman has a strong constitution, has plentiful Qi and Blood, then strong Blood-moving treatment can be applied to encourage fibroid necrosis and shrinkage. Even if this is successful, the risk of the fibroids growing again during pregnancy is a real one.
If uterine polyps are discovered on ultrasound, they will usually be removed surgically before conception is attempted. There is some evidence that size of a polyp, especially as it approaches 2 cm, may be associated with increased miscarriage. Polyps may contribute to uterine inflammation which can have an IUD sort of effect and prevent implantation or successful placental development. Hysteroscopic polypectomy is a simple procedure, which carries little risk and may improve reproductive outcome in cases of women trying to conceive or undergoing ART.38
This is generally a quicker and simpler solution than using Chinese medicine, which in the case of removing pedunculated polyps, has limited success.
Other conditions associated with recurrent miscarriages
Diabetes
Diabetes is a disease that has classically been associated with recurrent pregnancy loss. However, it is only when there is poor blood sugar control in an insulin-dependent female diabetic that there is any increased likelihood of miscarriage. It appears that levels of blood sugar need to be stable at the time of ovulation and conception. If they are not, there is an increased risk of chromosomal abnormalities in the fetus or developmental abnormalities.39
Fortunately, these days, diabetes is usually adequately treated and thus is not a frequent contributor to miscarriages in the developed world.
Gestational diabetes is a more insidious form of diabetes, which becomes apparent only after the pregnancy is established. Even when it has resolved completely after the pregnancy, it is important to ensure blood sugar is well-regulated before considering another pregnancy: otherwise, there may be a persisting increased risk of a malfunction during cell division at ovulation, and the risk of creating an embryo with a chromosomal abnormality. Women with a history of gestational diabetes, are advised to follow a good diet before conceiving again.40
The same factors in diabetes which can put at risk cell division and create chromosomal defects in the fetus also operate in the male. Poorly-controlled blood sugar can affect cell division in the testes, leading to abnormalities of the sperm that result in infertility or increased miscarriage risk.41
Miscarriages associated with diabetes will, according to TCM analysis, often fall in the Kidney Yin Xu category. Mild blood sugar abnormalities are sometimes associated with PCOS and treatment of Spleen Qi deficiency and Damp accumulation may be relevant.
Thyroid disorders
Both infertility and miscarriage are more common when the thyroid gland is hypo- or hyperactive. Higher miscarriage rate, more frequent pre-term deliveries, increased hypertension, diabetic complications, higher risk for placental abruption, and adverse fetal effects have all been reported with thyroid dysfunction in pregnancy.
During pregnancy, a 30–40% increased need for thyroid hormones is the result of increased placental uptake, higher thyroid-binding globulin levels, and greater blood volume. Those with subclinical hypothyroidism and/or high-normal TSH levels at the beginning of pregnancy may not be able to meet these needs and may show signs of thyroid insufficiency during pregnancy. It is usually recommended that these women (and those with diagnosed hypothyroidism before they become pregnant) be treated prior to and during pregnancy.42
Uncontrolled hyperactivity of the thyroid during pregnancy is rare but can increase the risk of miscarriage.43 The mechanism is unknown but high levels of thyroid hormones increase body metabolism and temperature which might compromise the endometrium’s structure and function.
In TCM terms, we relate this increased metabolism to internal Heat from Yin deficiency. In Yin-deficient women, the endometrium is typically thin and not well nourished; thus, the embryo fails to develop and thrive. Strong Heat-clearing herbs given with Yin-nourishing herbs can often remedy this.
Women who are significantly hypothyroid (underacting thyroid) have more difficulty conceiving, but if they do there is a two-three times increased miscarriage risk.44
Early intervention with thyroid hormone medication (before pregnancy) reduces the risk, as do preventative measures taken with Chinese herbs and acupuncture to strengthen Kidney and Spleen Yang over a period of some months.
There is no conclusive evidence that thyroid disease in the male partner contributes to increased miscarriage rates; however, thyroid disease, especially hypothyroidism, has been shown to have a negative effect on semen quality.45
This and the fact that thyroid function is so important for controlling cell metabolism and cell division means that ensuring healthy thyroid function is an important part of preconception care in men and especially so if there have been previous miscarriages.
Hypothyroidism is a clinical condition which is often encountered as part of a Kidney Yang deficient picture in TCM terms. In men, Kidney Yang deficiency lowers libido, causes difficulty with erections, and is often related to poor sperm production or production of sperm that have defective motility.
Thyroid antibodies were discussed above in immune disorders.
Intestinal disorders
Disorders of the gut such as irritable bowel syndrome, celiac disease, Crohn’s disease, ulcerative colitis and candidiasis can compromise nutritional status by interfering with absorption of nutrients through the intestinal wall. Some nutrients are known to be important for fertility or fetal health and if intestinal disorders prevent adequate absorption, then supplementation may be important to prevent recurrent miscarriage.
Additionally, the drugs used to treat some of these diseases can affect fertility or the fetus. Some of these drugs suppress the immune system and some can damage the DNA.46
Either of these categories can cause damage to the gametes or the fetus. Such drugs must be withdrawn or replaced before pregnancy is attempted.
Celiac disease (a severe intolerance to gluten) seems to be in some cases related to hormonal abnormalities which are not found in other gut disorders. Many men with celiac disease have smaller than average testicles, low fertility, sexual dysfunction and partners with a history of miscarriage. It is not uncommon for celiac disease to first be diagnosed after recurrent miscarriages.47
Candidiasis is an overgrowth in the gut by Candida albicans, a benign yeast organism and normal gut inhabitant, which mutates to a fungal form and proliferates and invades the intestines and intestinal walls. According to Foresight, a British association which promotes pre-conception care, Candida infection is implicated in infertility, miscarriage and premature birth.48,49 Dietary interventions will be advised before conception for these disorders.
Renal disease
When renal disease is chronic, risk of miscarriage is increased. Treatment of Kidney Yin and Yang until the disease is cured or stabilized is advisable before conception is attempted.
Cardiovascular disease
Women with a family history of ischemic heart disease are more at risk of miscarriage.50 And conversely, women who suffer recurrent miscarriages are more likely to develop heart problems when they are older. In early pregnancy, the cardiovascular system must do a great deal to ensure that the pregnancy continues and part of preconception planning should be to ensure the cardiovascular system is in as good a shape as possible.
Treatment offered by TCM practitioners in early pregnancy often focuses on the Heart (to treat the Shen and the Bao vessel) and the Pericardium (which helps cardiovascular function).
Excess or low body weight
A relationship has been observed between obesity and miscarriage rates of pregnancies achieved with IVF.51 Weight loss is an important and low cost measure which is non-invasive and managed by patients themselves. Hence, IVF clinics with their patient’s interests at heart will insist that patients with unfavorable BMIs lose weight before attempting IVF. (See Chapter 5 (PCOS) and Chapter 9 for more discussion on weight loss and the role Chinese medicine can play.)
On the other hand, very low body weight is also considered a risk factor for miscarriage and dietary and lifestyle modification should address this before conception.52 Women with Yin deficiency and internal Heat fall into this category; appropriate lifestyle and treatment measures were discussed in Chapter 4.
Lifestyle and environmental causes
Lifestyle and environmental factors can contribute to infertility and to miscarriage and the impact of both of these needs to be considered for both female and male partners. Scientific evidence indicates extreme sensitivity of embryos and fetuses to environmental and occupational chemicals compared with adult responses.53
Stress
The way we live our lives not only affects fertility but also has an impact on how a pregnancy develops, e.g., stress is related to higher miscarriage rates.54 The effects of stress are discussed further in Chapter 12 (and also Ch. 11).
Diet
Diet is discussed in more detail in Chapter 12, however, we should note here that eating a good diet of fresh foods and taking supplements is associated with a lower miscarriage rate.53
Chemical exposure
Men: Historically, the fault for miscarriages always fell on the woman, i.e., it was thought she couldn’t ‘hold on to the baby’, and this is reflected in both Chinese and Western medical texts.
Then we came to understand the primary causative role chromosomal abnormality played in fetal loss and research showed how genetic abnormalities in the sperm, and not just the egg, are often implicated in miscarriages, especially if the male partner works in certain trades. For example, men who work with glues, solvents, and paints produce sperm which create fetuses that are two–three times more likely to miscarry than normal.5
Sperm can be affected by exposure to toxic chemicals at any time, but miscarriages are most likely if the sperm exposure happened in the 6 months before conception.55
Women: It has also been clearly demonstrated that chemical exposure affects women too, both in their ability to conceive and to hold on to the pregnancy. The chromosomes of the egg are vulnerable to damage by toxic chemicals during the time of maturation of the egg, and especially after it is released from the safe haven of the ovary at the time of ovulation, or at the time of conception and formation of the embryo.
Pharmacists or nurses who handle antineoplastic agents before or when they become pregnant are more likely to miscarry.56 Similarly, nurses who are exposed to sterilizing chemicals have a higher miscarriage rate.57 Female veterinarians who are exposed to anesthetics and pesticides have twice the miscarriage rate of the general population.58
Some other confirmed environmental causes of miscarriage include lead, mercury, organic solvents, and ionizing radiation.59,60
Household cleaners are also a cause of concern (see Ch. 12 for more discussion on the effect of environmental toxins).
Caffeine
Caffeine consumption during early pregnancy is clearly related to an increased risk of miscarriage of normal karyotype embryos, especially once daily intake reaches 200 mg (roughly 1.5 cups of coffee, 3 cups of tea or 5 sodas).61,62
Caffeine can easily cross the placental barrier. A fetus cannot metabolize caffeine, particularly in the early stages of pregnancy, so it has a direct effect on cells and tissues and may interfere with development. We know that high doses of caffeine have a vasoconstrictive effect and this could possibly reduce blood flow to the placenta and to the fetus.
Many women who have prepared for pregnancy with pre-conception programs will have already eliminated or reduced caffeine consumption before they conceive. If not, then cutting caffeine out (or down) is a sensible strategy for at least the first 3 or 4 months of pregnancy. Those women who suffer from pregnancy nausea will usually not need any persuading to eliminate coffee.
Alcohol
The effects of drinking during pregnancy are well known and are significant enough to deter most women from drinking.
But women who are attempting to conceive should be encouraged to avoid even very early exposure to alcohol. There is good evidence that even moderate alcohol consumption is associated with an increased risk of miscarriage.63
Smoking
Several studies have shown that women who smoke have a modest increase in their risk for miscarriage,64 hence women planning to conceive would be well advised to quit. Marijuana is thought to add to inflammatory processes that can contribute to early pregnancy loss, though this has not been confirmed in human studies.65
Mycotoxins
Mold contamination of food and environment is widespread. Some mycotoxins such as zearalenone mimic estrogen and have been described in connection with a number of reproductive disorders including miscarriage in animal studies.66 This and other mold toxins are common in our environment – either in our houses if they are damp or in our kitchens if food (especially grains) is kept for too long. While the effect of mycotoxins is unlikely to be a major concern for women who suffer repeated miscarriages, in the interests of improving the internal hormone environment eating fresh foods and not keeping foods for too long (in or out of the fridge) is to be recommended.
Patients living in damp houses could think about installing dehumidifiers if other more drastic measures, such as moving house or installing damp courses, are not practical.
Electromagnetic fields (EMF) and radiation
EMFs are impossible to avoid in modern daily life, but advice to women in the early stages of pregnancy to avoid excessive exposure is important. Miscarriage risk is increased two-fold by exposure to peak levels of ≥1.6 μT. The researchers speculate that EMF spikes (rather than overall exposure) could cause miscarriages by subtly disrupting cell-to-cell communication. The EMF load can be lessened by reducing exposure to such spikes from household gadgets in the early weeks of pregnancy. Vacuum cleaners, food mixers, and hairdryers can produce strong alternating magnetic fields; generally, those with strong motors are the worst culprit, so handing over some of the household chores for the 1st trimester might be an option many women would desire.67
X-rays of the abdomen or back in women increases the miscarriage rate, although the effect does not extend over several years, as it does with men. Early embryos are particularly sensitive, since their rapidly dividing cells are easily damaged by ionizing radiation. If genetic damage results, the embryo will not develop properly and will miscarry. A history of either abdominal or lower back X-rays on men increase risk of miscarriage in subsequent pregnancies.5
Clearly, assessing the environment at home and at work is important when investigating recurrent miscarriage. Ongoing exposures to chemicals at work, at home or related to hobbies or renovations must be discontinued well before pregnancy is attempted again. And exposure to radiation and EMFs limited where possible.
Psychological factors
A number of workers in this field feel that emotional traumas, leading to low self-esteem or feelings of guilt, may underlie some cases of recurrent miscarriage. There may be a history of incest or sexual assault. Previous abortions may also contribute to a tendency to miscarry if the woman felt ambivalent about the abortion and, especially, if the aborted pregnancy was with the same partner with whom she now wanted to have a baby. Severe stress or domestic abuse have also been linked with increased miscarriage.68
Population studies in China have observed that those who do ‘mental’ work have a higher rate of miscarriage than those who don’t; 38% compared with 15%.69
Chinese medicine describes a central role of the Heart when it is talking about emotional imbalance. The Heart is said to be the house of the spirit and when it is damaged, there can be many psychological manifestations – some of them deep in the subconscious, some of them manifesting in high levels of anxiety and a number of other clinical symptoms. As described in Chapter 2, the Heart also has a direct link with the Uterus and in fact, is of key importance in controlling the ‘opening and closing’ of the Uterus. Disturbed Heart Qi during pregnancy can lead to inappropriate opening of the Uterus and miscarriage.
Treatment to prevent miscarriage should always be mindful of the Heart and settling or calming the mind. Counseling or psychotherapy are usually effective methods of addressing unresolved issues from the past and acupuncture can be helpful in changing deeply held or unconscious body–mind patterns and in calming anxiety. Once a patient with a history of miscarriage becomes pregnant, regular acupuncture to calm the mind is recommended. Some research has indicated that just the act of monitoring early pregnancy seems to help reduce miscarriage rates in women with a history of pregnancy loss.70