The endocrine system
Endocrine examination
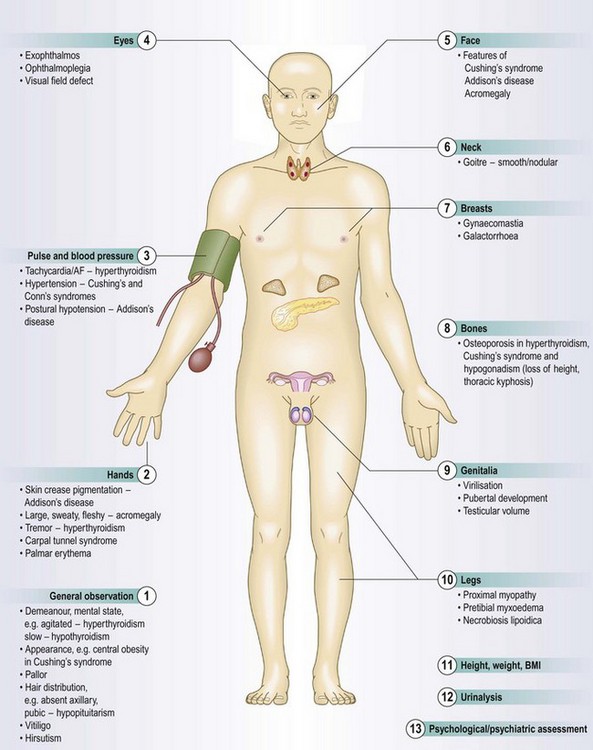
Anatomy
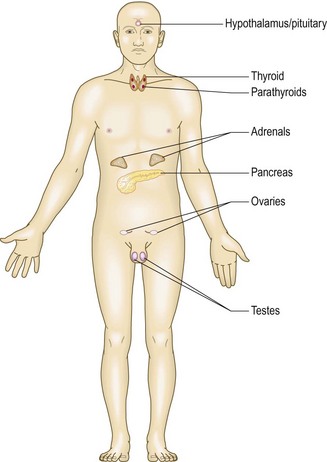
The main endocrine glands are the pituitary, thyroid, parathyroids, pancreas, adrenals and gonads: testes and ovaries (Fig. 5.1). These glands synthesise hormones which are released into the circulation and act at distant sites. Disease may result from excessive or inadequate production of hormones, or target organ hypersensitivity or resistance to the hormone. Although some endocrine glands, e.g. parathyroid glands and pancreas, respond directly to metabolic signals, most are controlled by hormones released from the pituitary gland. A wide variety of molecules act as hormones:
Symptoms and definitions
Symptoms of endocrine disturbance are frequently non-specific and affect many body systems (Box 5.1). Endocrine conditions may be detected by chance, e.g. glycosuria on screening, or if the clinician sees a patient after a significant time interval and notices diagnostic facial features, e.g. in acromegaly or hypothyroidism. Nevertheless, diagnosis often depends upon careful observation of a patient with non-specific symptoms prompting the recognition of specific features.
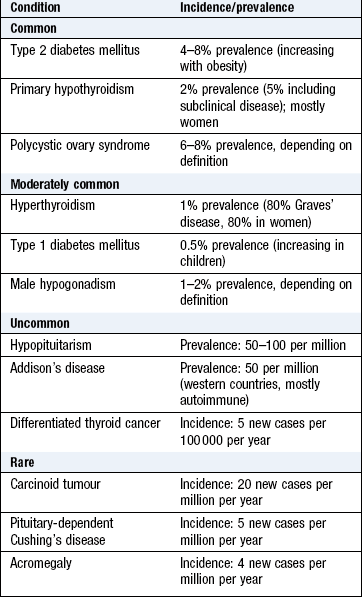
Apart from diabetes mellitus, thyroid disease and some reproductive conditions, endocrine disorders are uncommon. Most patients with tiredness, excessive sweating or sexual dysfunction, for example, do not have an underlying endocrine cause (Box 5.2).
Common presenting symptoms are:
• appetite and/or weight change – in hyper/hypothyroidism, diabetes mellitus, Cushing’s syndrome
• polydipsia (excessive thirst) and/or polyuria (passing >3 litres urine/day) – in diabetes mellitus, diabetes insipidus or hyperparathyroidism
• change in facial/body hair growth and distribution – in hypogonadism, hypopituitarism, adrenal insufficiency, androgen excess. Hirsutism is the excessive growth of thick terminal hair in an androgen-dependent distribution (upper lip, chin, chest, back, lower abdomen, thighs) in women
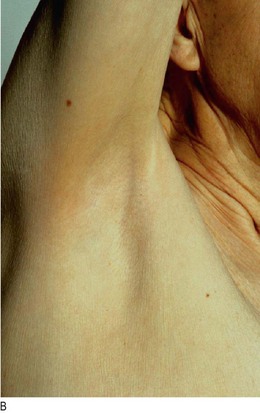
• change in skin and mucosal pigmentation and character: coarse dry skin in hypothyroidism; excessive pigmentation and/or vitiligo (areas of depigmented skin) in Addison’s disease (Fig. 5.17D); soft-tissue overgrowth and skin tags in acromegaly; acanthosis nigricans (velvety thickening and pigmentation of the major flexures, especially the axillae and groins: Fig. 5.11A) in obesity, and type 2 diabetes
• increased sweating in acromegaly and phaeochromocytoma
• temperature intolerance – in hyperthyroidism (heat) and hypothyroidism (cold)
• erectile dysfunction or loss of libido in hypogonadism
• gynaecomastia (breast tissue enlargement in men)
• galactorrhoea (breast milk production in men, or in women outwith pregnancy or breastfeeding) in pituitary adenomas producing hyperprolactinaemia
• primary or secondary amenorrhoea (p. 221) in pituitary or hypothalamic disease
• tiredness: can be a non-specific feature of diabetes mellitus, hypothyroidism or Addison’s disease.
The history
The thyroid
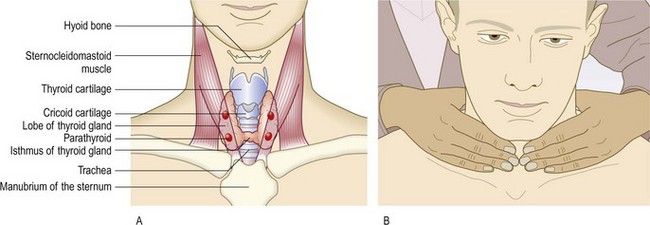
The thyroid is butterfly-shaped with two symmetrical lobes joined by a central isthmus that normally covers the second and third tracheal rings (Fig. 5.2A). The gland may extend into the superior mediastinum, or may occasionally be entirely retrosternal. Rarely, it is located higher in the neck along the line of the thyroglossal duct. If situated at the back of the tongue (lingual goitre), it may be visible through the open mouth.
Symptoms and definitions
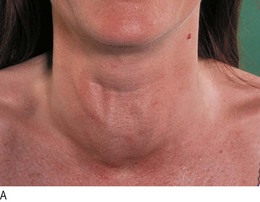
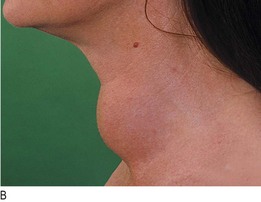
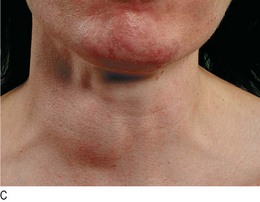
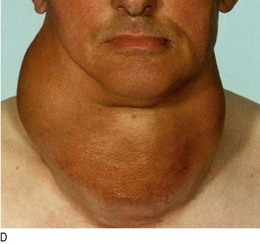
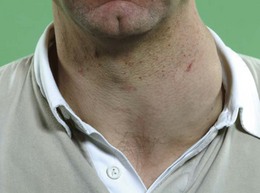
Goitre is enlargement of the thyroid gland. It is not necessarily associated with thyroid dysfunction and most patients with a goitre are euthyroid (Fig. 5.5).
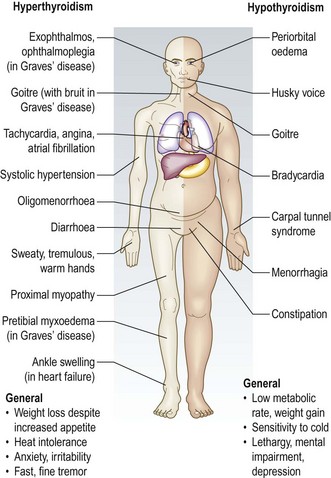
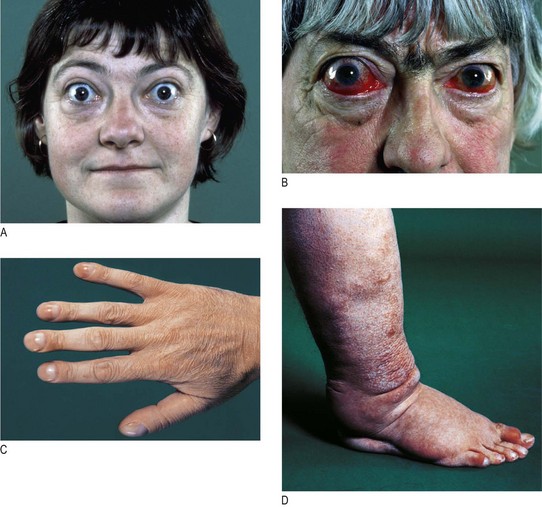
Hyperthyroidism (thyrotoxicosis) is a clinical state caused by increased levels of circulating levels of the thyroid hormones, T3 and T4. Graves’ disease is the commonest cause of hyperthyroidism. It is an autoimmune disease with a familial component, which is 5–10 times more common in women and usually presents between 20 and 50 years of age. It has specific extrathyroid features (Fig. 5.3):
• Exophthalmos (proptosis) is increased protrusion of the eyeball from the orbit. It is caused by an inflammatory infiltration of the orbital contents (the soft tissues and extraocular muscles, not the globe). It is usually bilateral. Exophthalmos may lead to diplopia (Fig. 5.4A&B) and other features of Graves’ ophthalmopathy: conjunctival oedema, conjunctivitis, corneal ulceration, ophthalmoplegia and optic atrophy (Ch. 12).
• Pretibial myxoedema is a raised, discoloured (usually pink or brown) indurated appearance over the lower legs (Fig. 5.4D). Note that, despite the name, it is associated with Graves’ disease, not hypothyroidism.
• Thyroid acropachy is a periosteal hypertrophy of the distal phalanges which looks like finger clubbing (Fig. 5.4C).
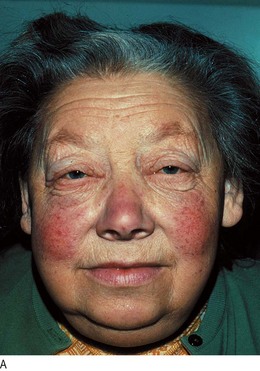
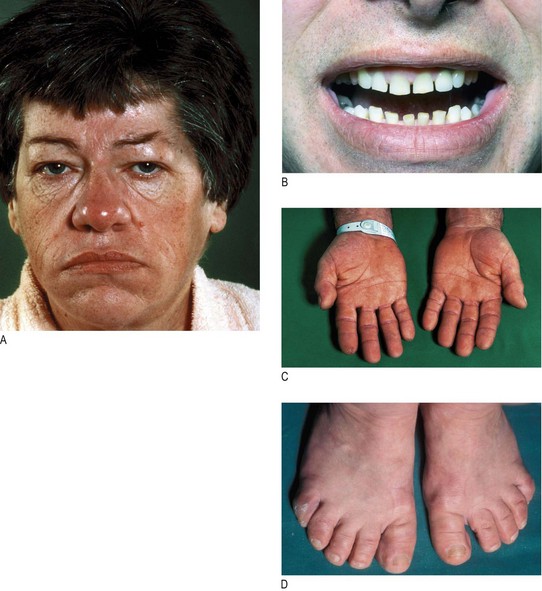
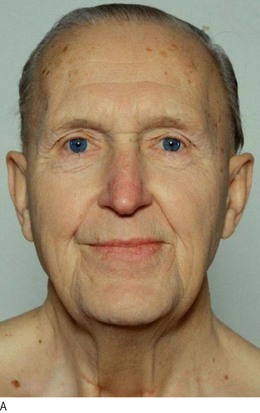
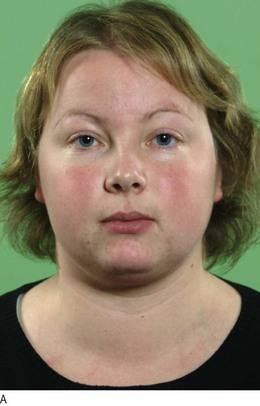
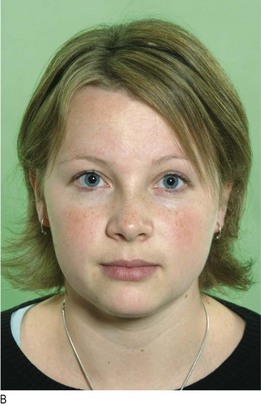
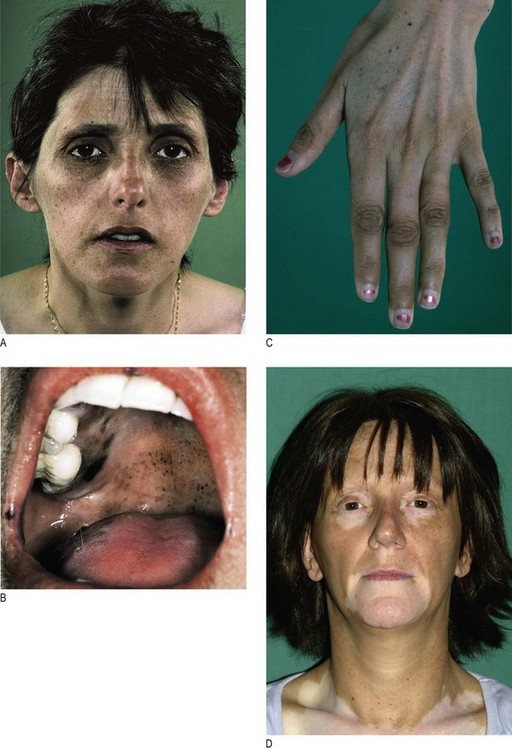
Hypothyroidism (Fig. 5.3) is caused by reduced levels of thyroid hormones and is usually due to autoimmune Hashimoto’s thyroiditis. Women are affected approximately six times more commonly than men. Many clinical features of hypothyroidism are produced by myxoedema (non-pitting oedema caused by tissue infiltration by mucopolysaccharides, chondroitin and hyaluronic acid) (Box 5.3 and Figs 5.3 and 5.7).
History
Normal findings: The normal thyroid gland is palpable in ~50% of women and 25% of men. Prominent skin folds may give a false impression of goitre. The thyroid (or a thyroglossal cyst) moves upwards on swallowing since it is enveloped in the pre-tracheal fascia, which is attached to the cricoid cartilage.
Shape, surface and consistency: Simple goitres are relatively symmetrical in their earlier stages but often become nodular with time. In Graves’ disease the surface of the thyroid gland is usually smooth and diffuse; it is irregular in uninodular or multinodular goitre (Fig. 5.5). Nodules in the substance of the gland may be large or small, and single or multiple, and are usually benign. A very hard consistency suggests malignancy. Large, firm lymph nodes near a goitre suggest thyroid cancer (Fig. 5.6). Diffuse tenderness is typical of viral thyroiditis. Localised tenderness may follow bleeding into a thyroid cyst.
The parathyroids
There are usually four parathyroid glands which lie posterior to the thyroid (Fig. 5.2A). Each is about the size of a pea and produces parathyroid hormone, a peptide which increases the level of calcium in the blood.
Symptoms and definitions
Parathyroid disease is commonly asymptomatic. In hyperparathyroidism, the commonest symptoms relate to hypercalcaemia: polyuria, polydipsia, renal stones, peptic ulceration, tender areas of bone fracture deformity (‘Brown tumours’: Fig. 5.8A), and confusion or psychiatric symptoms.
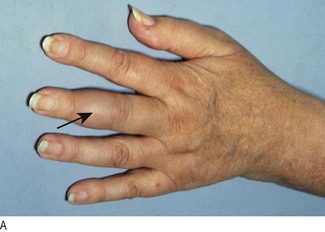
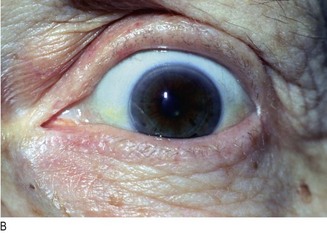
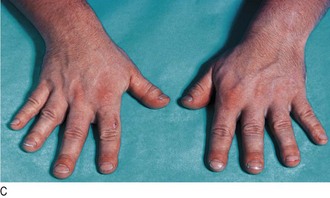
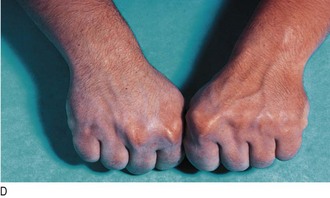
Fig. 5.8 Parathyroid disease.
(A) ‘Brown tumour’ of the phalanx (middle finger) in hyperparathyroidism. (B) Corneal calcification in hyperparathyroidism. (C) Pseudohypoparathyroidism: short metacarpals. (D) These are best seen when the patient makes a fist.
In hypoparathyroidism, hypocalcaemia may cause hyperreflexia or tetany (involuntary muscle contraction), most commonly in the hands or feet. Paraesthesiae of the hands and feet or around the mouth may occur. Hypoparathyroidism is most often caused by inadvertent damage to the glands during thyroid surgery.
Patients with the autosomal dominant condition pseudohypoparathyroidism have end-organ resistance to parathyroid hormone and typically have short stature, round face and shortening of some metacarpal bones.
History
• recent thyroid or neck surgery or irradiation
• polyuria, polydipsia or renal stones
Abnormal findings: Parathyroid tumours are very rarely palpable.
Findings in hyperparathyroidism may include altered mental state, dehydration, proximal muscle weakness, fractures and bony tenderness. In long-standing hypercalcaemia, corneal calcification (band keratopathy) may be present (Fig. 5.8B). Renal stones may produce haematuria on stix testing.
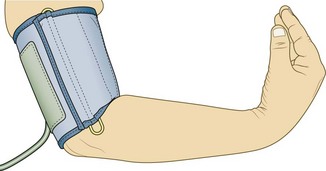
In moderate/severe hypocalcaemia, hyperreflexia and a positive Trousseau’s sign may be present. In pseudohypoparathyroidism the metacarpals of the ring and little fingers are shortened (Fig. 5.8C and D).
The pancreas
The pancreas lies behind the stomach on the posterior abdominal wall. Its endocrine functions include the production of insulin, glucagon, gastrin, somatostatin and vasoactive intestinal peptide. Its exocrine function is to produce alkaline secretions containing digestive enzymes.
Symptoms and definitions
Diabetes mellitus: This is characterised by hyperglycaemia due to absolute or relative insulin deficiency. Insulin-dependent patients are particularly susceptible to acute metabolic decompensation due to hypoglycaemia or ketoacidosis, both of which require prompt clinical and biochemical recognition and treatment.
• Type 1: severe insulin deficiency due to autoimmune destruction of the pancreatic islets.
• Type 2: commonly affects people who are obese and insulin-resistant, although impaired β-cell function is also important.
Diabetes mellitus may present with a classical triad of symptoms:
• Polyuria (and nocturia): due to osmotic diuresis caused by glycosuria.
• Thirst: due to the resulting loss of fluid and electrolytes.
• Weight loss: due to fluid depletion and breakdown of fat and muscle secondary to insulin deficiency.
Other common symptoms are tiredness, mood changes and blurred vision (due to glucose-induced changes in lens refraction). Bacterial and fungal skin infections are common because of the combination of hyperglycaemia, impaired immune resistance and tissue ischaemia. Itching of the genitalia (pruritus vulvae in women, balanitis in men) is due to Candida yeast infection (thrush).
Abnormal findings: Dehydration and Kussmaul respiration (hyperventilation with a deep, sighing respiratory pattern) are common in ketoacidosis.
Bacterial skin infections, e.g. cellulitis, boils, abscesses and fungal infections, may be seen. Acanthosis nigricans (Fig. 5.11A) occurs in hyperinsulinism and is seen frequently in patients with insulin-resistant type 2 diabetes. Necrobiosis lipoidica (a yellow indurated or ulcerated area surrounded by a red margin: Fig. 5.11B), due to collagen degeneration, may occur on the shins of some type 1 diabetic patients and often causes chronic ulceration. Xanthelasmata and xanthomata indicate significant hyperlipidaemia (Fig. 5.11C and Fig. 6.8).
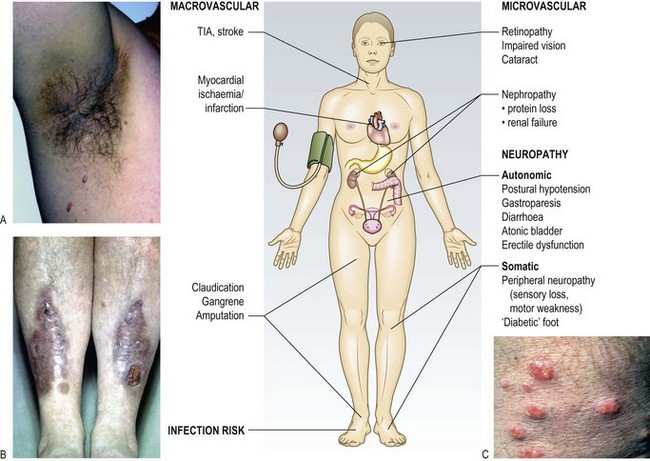
Fig. 5.11 Diabetes and the skin.
(A) Acanthosis nigricans. (B) Necrobiosis lipoidica. (C) Eruptive xanthomata.
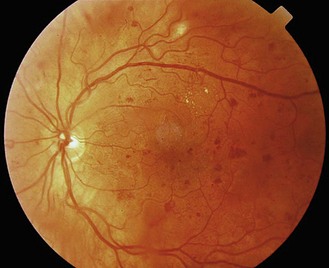
Microvascular, neuropathic and macrovascular complications of hyperglycaemia (Fig. 5.11) can occur in patients with any type of diabetes mellitus, and may be present at diagnosis in patients with slow-onset type 2 disease. Careful examination of the eyes, cardiovascular, neurological and renal systems, and feet is essential.
Glycosuria suggests hyperglycaemia and, if accompanied by ketonuria (and Kussmaul respiration: Ch. 7) indicates ketoacidosis. Proteinuria occurs in diabetic nephropathy. Detection of nitrite ± haematuria suggests (often occult) urinary infection (Box 5.4).
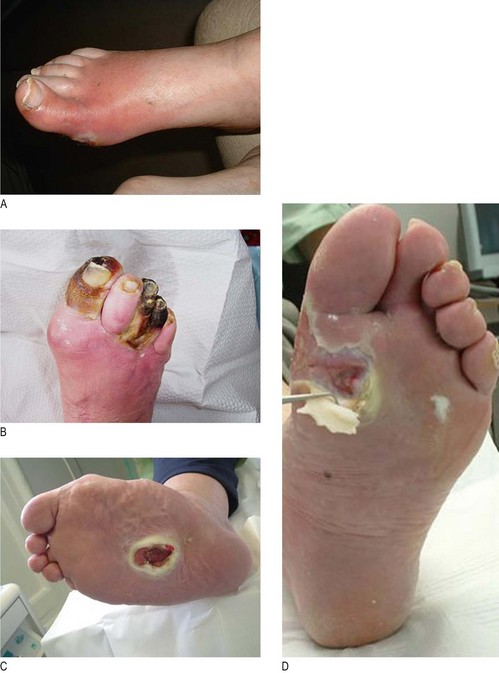
Abnormal findings: Hair loss and nail dystrophy occur with ischaemia, causing nutritional changes. There may be skin fissures or tinea infection (‘athlete’s foot’). The foot arch may be excessive in neuropathy or collapsed (rocker-bottom sole). Both conditions cause abnormal pressures and increase risk of plantar ulceration.
Warm feet occur in neuropathy and cold feet in ischaemia.
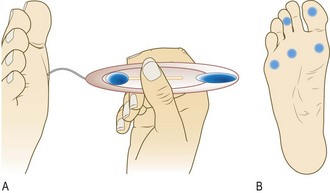
Sensory neuropathy is present if the patient cannot feel the monofilament in any of the sites. This means loss of protective pain sensation and is a good predictor of future ulceration.
Charcot’s arthropathy is disorganised foot architecture, acute inflammation, fracture and bone thinning, usually in a patient with neuropathy but relatively good vascular supply to the lower limb. It presents acutely as a hot, red, swollen foot often impossible to distinguish clinically from infection.
• Low – no risk factors (no sensation loss, peripheral vascular disease or other risk factors).
• Moderate – one risk factor present.
• High – previous ulceration or amputation, or more than one risk factor present.
• Active – ulceration, spreading infection, critical ischaemia, unexplained red, hot, swollen foot.
The pituitary
The pituitary gland is enclosed in the sella turcica in the base of the skull beneath the hypothalamus. It is bridged over by a fold of dura mater (diaphragma sellae) with sphenoidal air spaces below and the optic chiasm above. The pituitary has two lobes:
• Anterior: which secretes several hormones (adrenocorticotrophic hormone (ACTH), prolactin, growth hormone (GH), thyroid-stimulating hormone and gonadotrophins (luteinising hormone (LH) and follicle-stimulating hormone (FSH)).
• Posterior: an extension of the hypothalamus, which secretes vasopressin (antidiuretic hormone) and oxytocin.
History
Ask about the most common symptoms – headache and excessive sweating.
Has the patient (or more often a relative or friend) noticed changes in his facial features? Photographs taken years earlier can be helpful to identify changes and the onset of the condition.
Has the patient noticed an increase in shoe, ring or glove size (Box 5.5)?
Hypopituitarism: Anterior hypopituitarism is due to compression of the pituitary by a macroadenoma, infarction after childbirth (Sheehan’s syndrome), severe head trauma or cranial radiotherapy.
Apart from headache due to stretching of the diaphragma sellae and visual abnormalities, clinical presentation depends upon the deficiency of the specific anterior pituitary hormones involved. Individual or multiple hormones may be involved, so questioning in relation to the thyroid, adrenocortical and sexual function is needed.
The adrenals
The adrenals are small pyramidal organs lying immediately above the kidneys on their posteromedial surface. The adrenal medulla is part of the sympathetic nervous system and secretes catecholamines. The adrenal cortex secretes cortisol, mineralocorticoids and androgens.
Symptoms and definitions
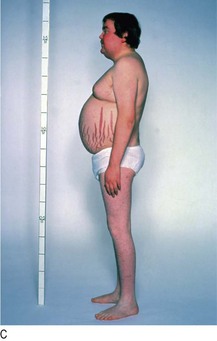
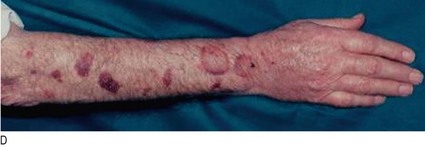
Cushing’s syndrome: Cushing’s syndrome is caused by excess exogenous or endogenous corticosteroid exposure. Most cases are iatrogenic due to side-effects of corticosteroid therapy. ‘Endogenous’ Cushing’s usually results from an ACTH-secreting pituitary microadenoma. Other causes include a primary adrenal tumour or ‘ectopic’ ACTH secretion.
The catabolic effects of steroids cause widespread tissue breakdown (particularly in skin, muscle and bone) with central accumulation of body fat. Proximal myopathy, fragility fractures, spontaneous purpura, skin thinning and susceptibility to infection are common (Fig. 5.16). Patients may be hypertensive.
The gonads
These glands secrete sex hormones (oestrogen and testosterone) in response to gonadotrophin (FSH and LH) release by the pituitary. They also contain the germ cells.
Symptoms and definitions
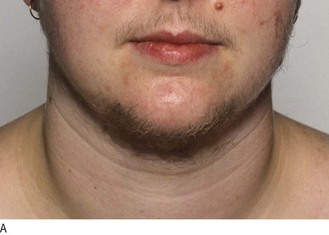
Klinefelter’s syndrome (47XYY) is the most common cause of primary hypogonadism in men (1 : 600 live male births). Diagnosis may be delayed until later life, by which time features of prolonged testosterone deficiency can be seen. Look for soft, finely wrinkled, hairless facial skin and gynaecomastia and examine the genitalia (pubic hair is often reduced/absent and the testes <3 ml in volume; Fig. 5.18).
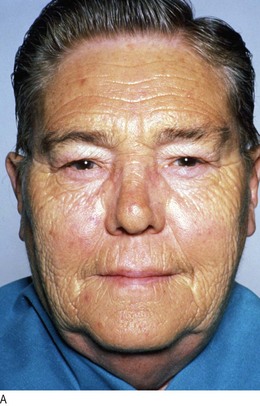
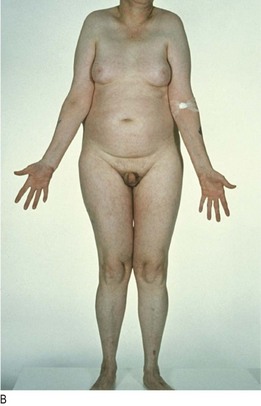
Fig. 5.18 Klinefelter’s syndrome.
(A) Hypogonadal facial skin. (B) Gynaecomastia, reduced pubic hair and small testes.
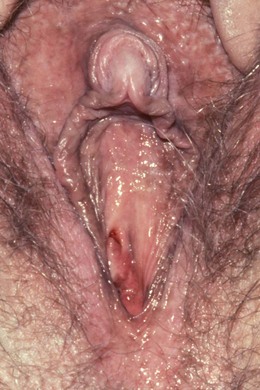
Hirsutism is common in women with polycystic ovary syndrome (Fig. 5.19). Virilisation is temporal recession of the scalp hair, deepening of the voice, breast atrophy, increased muscle bulk and clitoromegaly (Fig. 5.20). If present in women with a short history of severe hirsutism, it suggests a possible testosterone-secreting tumour.
Other endocrine disorders
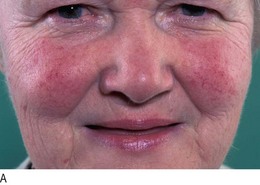
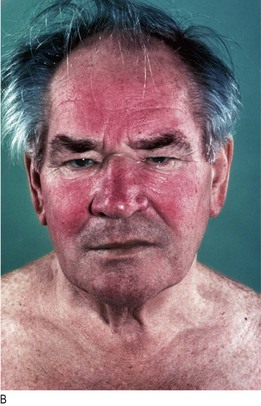
Liver metastases from mid-gut carcinoid tumour release vasoactive chemicals into the systemic circulation which cause flushing, diarrhoea and bronchospasm. Bending, exercise or even palpation of the enlarged liver may induce typical skin flushing. Permanent facial telangiectasia occurs after many years of carcinoid flushing (Fig. 5.21).
Putting it all together
Because of their wide diversity of clinical features, keep alert to the possibility of endocrine disease in non-specific presentations. Perhaps more than in any other area of medicine, pattern recognition is important.
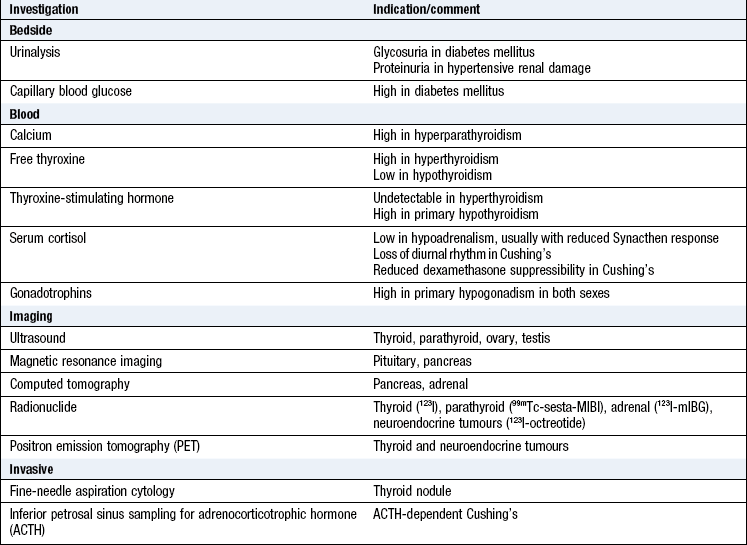
Investigations
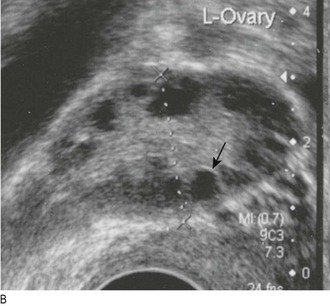
Measure serum hormone levels to assess over- or underactivity. Suppression tests can determine whether hormonal secretion is autonomous. Stimulation tests assess hormonal reserve (or lack of it in deficiency states). Modern imaging enables visualisation of small endocrine tumours, sometimes only millimetres in diameter (Box 5.7 and Fig. 5.22).
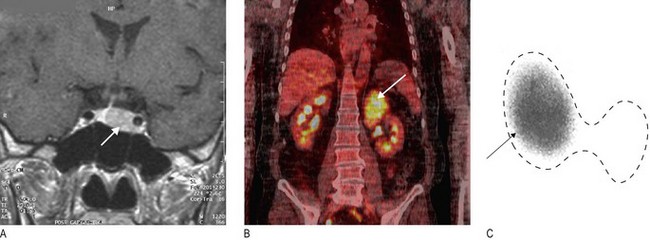
Fig. 5.22 Endocrine imaging.
(A) Magnetic resonance imaging showing pituitary macroadenoma (arrow). (B) Positron emission tomography-computed tomography scan showing an adrenal cancer (arrow). (C) 99mTechnetium radionuclide scan confirming unilateral toxic thyroid adenoma (arrowed) – dotted line shows outline of thyroid.