CHAPTER 33 Neurological health
At the completion of this chapter and with some further reading, students should be able to:
• Describe the structure of the nervous system
• Describe the position of each part of the nervous system
• Describe the functions of the nervous system
• State the pathophysiological influences and effects associated with disorders of the nervous system
• Describe the major manifestations of nervous system disorders
• Briefly describe the specific disorders of the nervous system outlined in this chapter
• Apply principles of neurological assessment
• Demonstrate accurate documentation of a neurological assessment
• Discuss the nursing management of an acute neurological presentation
• State the diagnostic tests that may be used to assess nervous system function
• Assist in planning and implementing nursing care for the individual with a nervous system disorder
The nervous system is responsible for the coordination of all other systems. It provides a network for communication within the body, and between the body and its environment. The brain is informed of events occurring both within and outside the body by nerve impulses that originate at a large number of sensory receptors. The receptors, which may be nerve endings, single specialised cells or a group of cells forming a sense organ, convert the energy of a stimulus into impulses that pass to specific areas of the brain. An understanding of this complex and dynamic system underpins many aspects of client care, as almost all medical conditions can affect the human nervous system in some way.
The workings of the human brain, and indeed the entire nervous system, have both fascinated and mystified scientists for centuries. The knowledge that has been uncovered has enabled healthcare professionals to make more accurate assessments of clients, allowing implementation of safer and more effective treatments. While application of this knowledge has significantly improved the expected outcomes for many clients affected by disorders of the nervous system, there is still much research to be carried out to fully explain the workings of this intricate system.
This chapter focuses on the function and structure of the neurological system, pathophysiological influences and effects of disorders of the nervous system, neurological assessment and the care of a client with a nervous system disorder.
Here I was again, back in the doctor’s office trying to find an answer. I’ve just been so weak and lethargic. I actually went to the ophthalmologist and had my eyes tested because I started seeing two of everything! It is obviously stress; heaps of people have told me I took on too much—studying for my degree just after the wedding and while we are building the new house. But the other day when I collapsed in the kitchen because I couldn’t feel my legs any more, James put his foot down and here we are to get the results of my MRI scan. I feel as if I am wasting everyone’s time, I’m sure it’s just stress. MULTIPLE SCLEROSIS! My whole world began to crumble.
My God, Louise looked really upset when she heard about the MS. She just cracked up. But I’m sure she will be fine, always has been. I guess she will just need some vitamin tablets to get better, which will be good because next week we are going to be laying the driveway.
THE FUNCTION AND STRUCTURE OF THE NEUROLOGICAL SYSTEM
Nervous tissue
Neurons
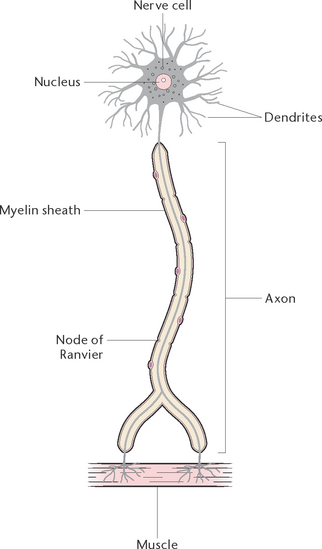
Neurons (Fig 33.1) are the primary components of the nervous system. Functioning alone, or as units, neurons detect internal and external changes and initiate body responses needed to maintain homeostasis. Each neuron is composed of a cell body, with projections forming dendrites, and one long axon. The dendrites are short-branched fibres, which receive impulses and conduct them towards the cell body of a neuron. The axon, which may vary in length from miniscule to over a metre, conducts impulses away from the cell body of a neuron. Generally, a neuron has only one axon but many dendrites. Axons leave the grey matter and become the fibres of the white matter. Each axon has a covering called a neurilemma, and most have a fatty sheath, the myelin sheath. The myelin sheath protects and insulates the axon and increases the transmission rate of nervous impulses. Neurons are bound together by a special type of connective tissue called neuroglia.
Neuroglia
The neuroglia includes many types of cells that support and protect the neurons. They play a role in regulating neuronal activity, and in providing neurons with nutrients. Neuroglia differ from neurons in that they are not capable of transmitting nerve impulses and never lose their ability to divide. The neuroglia in the central nervous system (CNS) are comprised mainly of two types of cells: astrocytes, cells with small cell bodies and processes like dendrites, which protect the neurons from harmful substances that may be in the blood by forming a living barrier between the capillary blood supply and the neurons; and oligodendrocytes in the CNS, which have few processes and produce the myelin sheath around the processes of the neurons. The Schwann cells in the CNS protect, nourish and form myelin.
Functions of neurons
Neurons have two major functional properties: irritability and conductivity. Irritability is the ability to respond to a stimulus and convert it into a nerve impulse. Conductivity is the ability to transmit the impulse to other neurons, muscles or glands. An impulse is a complex electrical and chemical signal transmitted along a nerve pathway in response to a stimulus. The speed of transmission varies with the size of the nerve fibre, and may be as much as 120 metres per second.
A synapse is the space between the terminal axon of one neuron and the dendrites of another. By means of a chemical substance (neurotransmitter) released by the axons, impulses are transmitted through this space from one neuron to another. Examples of neurotransmitters are acetylcholine and noradrenaline. Many different types of stimuli can excite neurons so that they become active and generate an impulse. Most neurons are excited by the neurotransmitters released by other neurons, but other stimuli can excite neurons. For example, sound excites some of the neuronal receptors of the ear, and pressure excites some cutaneous receptors of the skin. Receptors, or sensory nerve terminals, act as transducers, converting the energy of a stimulus into impulses that pass to the brain.
The nervous system can be divided into two primary divisions: the central nervous system, consisting of the brain and spinal cord; and the peripheral nervous system, consisting of nerves that connect the central nervous system with the body tissues.
The central nervous system
The central nervous system is composed of nervous tissue, which is commonly described as grey and white matter. Examination of a section of the brain reveals that it is grey on the outside and white on the inside. Microscopic examination reveals that the grey matter is composed of neuron cell bodies, and the white matter is made up of myelinated fibres.
The brain
The brain is a large organ weighing about 1.4 kg in the adult, held in position within the skull by membranes called the meninges. In most parts of the brain the outer portion, or cortex, consists of grey matter, while white matter forms the inner portion. The grey matter is convoluted to provide a greater surface area. The brain is divided into the:
The cerebrum
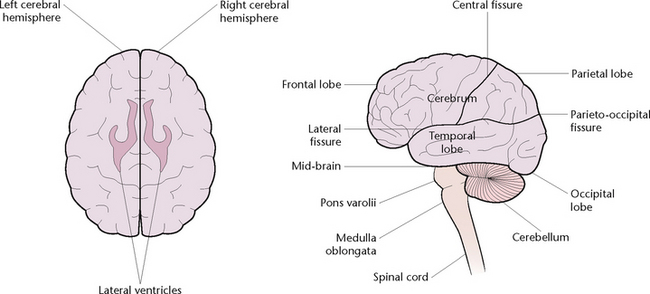
The cerebrum (Fig 33.2) is the largest part of the brain, filling the vault of the cranium from front to back. It is divided by fissures into the left and right hemispheres, and each hemisphere is further divided by fissures into four lobes:
1. The frontal lobe, responsible for voluntary motor function, motivation, aggression, personality, sense of smell and mood
2. The parietal lobe, which receives and evaluates sensory information
3. The temporal lobe, which receives input for smell and hearing and has an important role in memory
4. The occipital lobe, responsible for reception and integration of visual input.
The left hemisphere is usually associated with language, mathematical skills and reasoning. The right hemisphere is generally associated with skills such as artistic awareness and imagination. Within each hemisphere is a cavity called the lateral ventricle, which is concerned with the formation of cerebrospinal fluid.
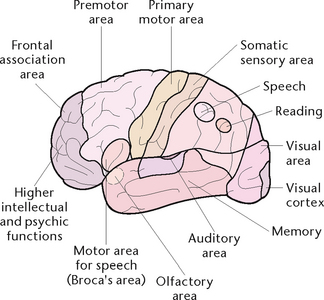
The cerebrum is divided into several areas, some of which are sensory and some of which are motor areas. The sensory areas of each hemisphere receive and interpret sensations from the opposite side of the body, including touch, temperature, pain, pressure and an awareness of the position of the body in its environment. The motor areas of each hemisphere control all voluntary movement on the opposite side of the body. The centres of special sense are located in the various lobes, including the centres for hearing, speech, smell, taste and sight (Fig 33.3).
The functions of the cerebrum are therefore to receive and interpret impulses from the sensory organs, to initiate and control the movements of skeletal muscles and to perform the higher levels of mental activity such as thinking, reasoning, intelligence, learning and memory.
The diencephalon
The thalami are two oval masses of grey matter that form the lateral walls of the third ventricle. Each thalamus is subdivided into a number of nuclei. Most sensory pathways (except smell) synapse here. The thalamus plays a role in the control of somatic motor activity and also influences mood and strong emotions.
The hypothalamus lies beneath the thalami, and the pituitary gland is closely connected to it. The hypothalamus controls all the activities of the autonomic nervous system, which is described later in this chapter. The hypothalamus is important in controlling the endocrine system, as it regulates pituitary gland function.
The brainstem
The midbrain. The midbrain is a short narrow segment connecting the cerebrum with the pons varolii. It is composed primarily of ascending and descending fibre tracts. Its functions are to provide a pathway for impulses passing between the cerebrum and spinal cord, and to receive stimuli that initiate eye and postural movements.
The pons varolii. The pons varolii is about 2.5 cm long, lying anterior to the cerebellum and above the medulla oblongata. It contains two respiratory centres, the pneumotaxic centre and the apneustic centre. Its functions are to act as a relay station from the cerebrum to the cerebellum, and to modify the activity of the medullary respiratory centres through the pneumotaxic and apneustic centres.
The medulla oblongata. The medulla oblongata is about 2.5–3.0 cm long, lying between the pons and the spinal cord. It provides the link between the brain and the spinal cord and contains the cardiac, respiratory, vasomotor and reflex centres. Its functions are:
• To provide a pathway where nerve fibres to and from the brain cross over to the opposite side
• To control heartbeat (through the cardiac centre)
• To control ventilation (through the respiratory centre)
• To control constriction and dilatation of blood vessels (through the vasomotor centre)
• To initiate the reflex actions of swallowing, vomiting, coughing and sneezing (through the reflex centres).
The cerebellum
The cerebellum lies behind the pons and medulla and below the occipital lobes of the cerebrum. Like the cerebrum, the cerebellum is divided into two hemispheres that have shallow convolutions in their surface of grey matter. Its functions are coordination of muscular activity and regulation of muscle tone, and maintenance of balance and posture.
Blood supply to the brain
The carotid and the vertebral arteries supply blood to the brain. These arteries branch and join up again, forming a circle of arteries at the base of the brain called the circle of Willis. From here smaller cerebral arteries branch off to supply each region of the brain. Blood returns from the brain via the jugular veins to the superior vena cava.
The blood–brain barrier is a barrier that prevents or delays the entry of certain substances into brain tissue. The relatively low permeability of the capillaries supplying the brain means that some substances are either completely or partially prevented from gaining access to brain tissue. The blood–brain barrier thus acts as a protective mechanism, preventing substances such as bilirubin, which could disrupt brain function, from crossing the barrier.
The spinal cord
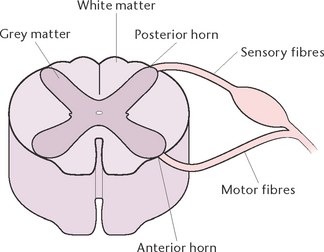
The spinal cord is a cylindrical structure that lies within a canal inside the vertebral column. It extends from an opening on the underside of the skull (the foramen magnum) to the level of the first or second lumbar vertebra. Below this level the vertebral canal is occupied by nerves from the lumbar and sacral segments of the cord; these constitute the cauda equina (‘horse’s tail’). The spinal cord, which is about 46 cm in length, consists of nervous tissue, with the white matter on the outside and the grey matter arranged roughly in an ‘H’ formation in the centre (Figs 33.4 and 33.5). The two anterior projections of grey matter are called the anterior horns, and the posterior projections are called the posterior horns. Sensory nerve fibres enter the posterior horns, and motor nerve fibres leave the anterior horns.
Leaving the spinal cord at intervals throughout its length are 31 pairs of spinal nerves. The functions of the spinal cord are:
• To receive sensory impulses from the tissues and convey them to the sensory areas of the brain via ascending (afferent) pathways
• To convey motor impulses from the brain to various parts of the body via descending (efferent) pathways
• To provide a pathway through which reflex actions take place.
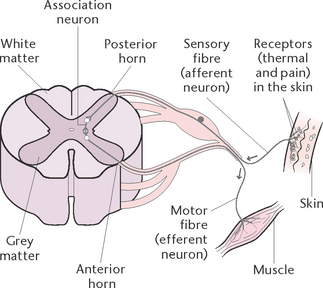
A reflex action, or arc, is an automatic motor response to a sensory stimulus without conscious involvement (Fig 33.6). Most reflex actions are protective in nature and take place more quickly than voluntary actions. The structures involved in a reflex action are:
• A sensory organ (e.g. the skin) to receive the stimulus
• A sensory (afferent) nerve fibre to carry the impulse to the posterior horn of the spinal cord
• An association neuron in the spinal cord to receive the impulse and transmit it directly to the anterior horn
• A motor (efferent) neuron in the anterior horn to receive the impulse and transmit it to the motor organ
• A motor organ (e.g. a muscle) to receive and respond to the stimulus.
An example of a reflex action is when the hand comes into contact with a very hot object. The skin on the hand receives the stimulus of heat, and an impulse travels from the sensory nerve endings in the skin to the posterior horn of the spinal cord. From there, the impulse is transmitted to the anterior horn, then passed along the motor nerves to the muscles of the shoulder, arm and hand. As a result, the hand is pulled rapidly away from the source of heat before the brain has even processed the information.
The meninges
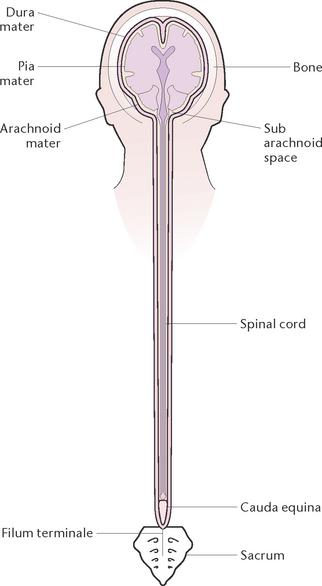
The meninges are the three membranes that cover the brain and the spinal cord. The individual membranes are:
1. The dura mater (meaning ‘hard mother’) is the tough outermost layer. It consists of two layers of fibrous connective tissue, with one layer forming the periosteum covering the inner surface of the skull bones, and the other layer covering the brain and spinal cord
2. The arachnoid mater (meaning ‘mother like a spider’s web’) is the middle layer. The name refers to the fact that it is so thin that, when viewed under a microscope, it resembles a spider’s web
3. The pia mater (meaning ‘gentle mother’) is the delicate innermost layer. It adheres closely to the surface of the brain and spinal cord, dipping down into all the convolutions and fissures. The pia mater is richly supplied with blood vessels that carry blood to the brain and spinal cord.
The subarachnoid space is the space between the arachnoid mater and pia mater, filled with cerebrospinal fluid in circulation. The functions of the meninges are to form a protective covering against physical injury around the brain and spinal cord, and to help secure the brain to the cranial vault.
Cerebrospinal fluid
Cerebrospinal fluid (CSF) is a clear watery fluid with a composition similar to plasma. It contains substances including water, glucose, sodium, chloride, potassium, protein and waste products such as urea. The CSF is formed from the blood and is produced by a combination of filtration and active secretory processes by the choroid plexus in the ventricles of the brain. CSF circulates in the subarachnoid space surrounding the brain and spinal cord. The total volume of the CSF is about 150 mL. The fluid is formed continuously in the ventricles at a rate of about 600–700 mL/day, and is reabsorbed into the blood at about the same rate. The normal CSF pressure when the body is horizontal is 5–10 mmHg. The functions of CSF are to:
The peripheral nervous system
The peripheral nervous system consists of the 12 pairs of cranial nerves, and 31 pairs of spinal nerves that leave the spinal cord. The peripheral nerves may be sensory, motor or mixed. Sensory (afferent) nerves carry impulses to the brain and spinal cord. Motor (efferent) nerves carry impulses from the brain and spinal cord to the muscles, organs and tissues. Mixed nerves are composed of both sensory and motor fibres and transmit impulses in both directions. The motor peripheral nervous system has two functional divisions:
• The somatic nervous system, which allows us to consciously, or voluntarily, control our skeletal muscles. This division is often called the voluntary motor system but it also includes involuntary reflexes
• The autonomic nervous system, which regulates events that are automatic, or involuntary, such as the activity of smooth and cardiac muscle and glands. The autonomic nervous system itself has two parts: the sympathetic and parasympathetic nervous systems (described further below) (Marieb 2012).
The cranial nerves
Twelve pairs of cranial nerves leave the brainstem. The numbers (Roman numerals are the convention), names and functions of the cranial nerves are:
I. Olfactory nerve: sensory—the nerve of smell
II. Optic nerve: sensory—the nerve of sight
III. Oculomotor nerve: motor—supplies the muscle of the eye
IV. Trochlear nerve: motor—supplies one of the eye muscles
V. Trigeminal nerve: mixed—sensory fibres receive stimuli from most of the skin of the head and face, the membranes of the nose and mouth, the orbits, the upper and lower jaws and teeth; motor fibres supply the muscles of mastication
VI. Abducent nerve: motor—supplies one of the eye muscles
VII. Facial nerve: mixed—sensory fibres convey the sensation of taste from the anterior portion of the tongue; motor fibres supply the muscles of facial expressions
VIII. Auditory nerve: sensory—the nerve of hearing and balance
IX. Glossopharyngeal nerve: mixed—sensory fibres convey taste sensations from the posterior part of the tongue; motor fibres supply the pharynx
X. Vagus nerve: mixed—controls secretion and movement of the internal organs (e.g. oesophagus, larynx, trachea, heart, stomach, intestines, pancreas, spleen, kidneys and blood vessels)
XI. Accessory nerve: motor—supplies the muscles of the neck, and also the pharynx and larynx
XII. Hypoglossal nerve: motor—supplies the tongue muscles (Marieb 2012).
The spinal nerves
The spinal nerves project out of the vertebral canal, one pair emerging below each vertebra, and one pair emerging between the cranium and the first cervical vertebra. The spinal nerves are mixed nerves, containing both sensory and motor fibres. They allow for sensation and movement in peripheral parts of the body not supplied by the cranial nerves, such as skin, muscles, bones and joints of the trunk and limbs. The spinal nerves are arranged in groups according to their region of origin in the cord. There are:
• Eight pairs of cervical nerves (C1–C8)
• Twelve pairs of thoracic nerves (T1–T12)
• Five pairs of lumbar nerves (L1–L5)
In some regions the nerves divide immediately after leaving the cord. These then branch and unite with each other to form what is called a plexus (meaning braid). The major plexuses are:
• The cervical plexus, which supplies the muscles of the neck and shoulders, and also gives rise to the phrenic nerves that supply the diaphragm
• The brachial plexus, which gives rise to the radial, median and ulna nerves, which supply the arm
• The lumbar plexus, which gives rise to the femoral nerve, which supplies the thigh muscles
The sciatic nerve is the largest nerve in the body, running over the hip posteriorly down the back of the thigh to the knee where it divides into the peroneal nerve and tibial nerve (Marieb 2012).
The autonomic nervous system
The autonomic nervous system is the division of the peripheral nervous system concerned with involuntary activity of the body. It supplies nerves to all the structures in the body that are not under conscious control. The autonomic nervous system consists of two divisions: the sympathetic and the parasympathetic nervous systems.
The sympathetic nervous system
The sympathetic nervous system arises from grey matter in the spinal cord from T1 through to L2. Sympathetic nerves then synapse in a chain of ganglia that lies on either side of the vertebral column, before reaching organs or tissues. A ganglion (plural ganglia) is a knot-like mass of cell bodies. Plexuses are formed by fibres from these ganglia; for example, the solar plexus lying behind the stomach and supplying the abdominal organs, and the cardiac plexus supplying the heart and lungs (Marieb 2012).
The parasympathetic nervous system
The parasympathetic nervous system consists of cranial nerves III, VII, IX and X and nerves that emerge from the sacral region of the spinal cord. The vagus nerve (cranial nerve X) is the largest autonomic nerve.
Functions of the autonomic nervous system
The functions of the autonomic nervous system are to control the movements of internal organs and the secretions of glands. The system provides dual control: the activity of an organ is stimulated by one set of nerves, and inhibited by the other set of nerves. This dual control achieves smooth rhythmic action of involuntary muscles and internal organs, maintaining a balance between activity and rest.
The sympathetic nerves are called adrenergic nerve fibres and release the neurotransmitter noradrenaline. These nerves can be affected by strong emotions such as anger, fear or excitement, and have a stimulating effect on most organs. The effect resembles that produced by adrenaline, a hormone secreted by the adrenal glands. This effect is called the ‘fright, fight or flight’ effect, in which the body responds to a fright either by preparing to fight or by running away. The response of the body includes:
• Dilation of the pupils of the eyes
• Increased force and rate of heartbeat, increasing circulation
• Increased blood pressure and constriction of arterioles in the skin and abdominal organs to divert blood to all skeletal muscles, heart, lungs and brain
• Dilation of the bronchi to allow more oxygen to enter
• Slowing of digestion so that the digestive organs can receive a reduced blood supply, enabling blood to be diverted to vital structures
• Increased production of sweat by sweat glands
• A rise in blood sugar level, as the liver is stimulated to release more glucose for increased energy needs.
The parasympathetic nerves are called cholinergic fibres and release the neurotransmitter acetylcholine. These nerves tend to slow down body processes, so that the end result of the antagonistic action of each division of the autonomic nervous system is a balance between acceleration and retardation. After the ‘fright’ or stressful situation is over, the parasympathetic nervous system returns things to normal. The digestive organs receive more blood, the glands increase their secretions, the heartbeat is decreased and the blood pressure falls. The effects of sympathetic and parasympathetic stimulation on various body organs are compared in Table 33.1.
Table 33.1 Effects of sympathetic and parasympathetic stimulation
| Organ | Sympathetic stimulation | Parasympathetic stimulation |
|---|---|---|
| Heart | ||
| Bronchi | Dilates bronchi, allowing more air to enter the lungs | Constricts bronchi, limiting air intake |
| Digestive system | Decreases activity of the system and constricts digestive system sphincters Inhibits production of saliva | |
| Urinary bladder | Relaxes bladder wall. Contracts internal sphincter muscle | Contracts bladder wall. Relaxes internal sphincter muscle |
| Eye | Dilates the pupil. Retracts the eyelids | Constricts the pupil. Closes the eyelids |
| Skin |
PATHOPHYSIOLOGICAL INFLUENCES AND EFFECTS OF DISORDERS OF THE NERVOUS SYSTEM
The pathophysiological changes that can disrupt normal function of part or all of the nervous system can be due to congenital or developmental disorders, infectious or inflammatory conditions, trauma, neoplasia, degenerative conditions and metabolic or endocrine disorders. Any pathophysiological change is capable of causing various types and degrees of dysfunction.
Aetiology of nervous system disorders
Congenital disorders
The central nervous system of the developing fetus is very vulnerable to damage. Factors that may cause nervous system damage include the passage of microorganisms and drugs across the placental barrier into the fetal circulation. Other factors that may cause nervous system defects and result in physical and intellectual deterioration include chromosomal abnormalities, metabolic disorders, cranial malformations and structural abnormalities. The central nervous system may also be damaged during the birth process; for example, by cerebral anoxia or cerebral haemorrhage.
Inflammatory and infectious conditions
Bacterial or viral infective processes affecting the central nervous system may result in the destruction of nervous tissue through the action of toxins released by the living microorganisms and from the material released from dead microorganisms, which stimulates the inflammatory process. Infection and inflammation of nervous tissue may result in altered behaviour, altered consciousness and sensory or motor deficits.
Trauma
Trauma to the nervous system may result from elements within the system or from external forces. Trauma occurring from elements within the nervous system includes: bleeding from an aneurysm or ruptured intracranial vessel; transient interruption of the cerebral blood flow, causing ischaemia; and occlusion of a cerebral blood vessel by a thrombus or embolus. The most common causative factors in these conditions are hypertension and atherosclerosis.
Trauma from external forces may be caused by a direct or an indirect injury. A direct acceleration brain injury occurs when the head is struck by a moving object, and a direct deceleration injury occurs when the head in motion strikes a stationary object. In an indirect brain injury, the traumatic force is transmitted to the head through an impact to another part of the body, such as the neck or buttocks.
In open head trauma, a penetrating injury damages the integrity of the skull and/or meninges and brain. Infection may occur, as the injury allows the entry of microorganisms. A closed head injury is non-penetrating, with generally no disruption to the integrity of the cerebral meninges. Closed head injuries can result in jarring, bruising or tearing of brain tissue, which can cause haemorrhage, cranial nerve damage and cerebral oedema. An important event in closed head injury is known as coup and contrecoup. The coup injury is cerebral bruising resulting from impact to the skull, and contrecoup refers to the rebound effect of the injury, the movement of the brain opposite to the site of impact.
The nervous system response to trauma, which may cause more damage than the actual injury, results in oedema, bleeding and increased intracranial pressure. These factors destroy nervous tissue by compression or restriction of the circulation.
The spinal cord may be damaged as a result of a crushing or penetrating injury, dislocation of the spinal column, prolapsed intravertebral discs or neoplasia. In addition to tearing of, and pressure on, the spinal cord tissues, damage may be caused by haemorrhage, oedema or disruption of the blood supply to the spinal cord.
Damage to the peripheral nerves may result in loss of sensory and/or motor function (Marieb & Hoehn 2010).
Neoplasia
Tumours of the nervous system, which may be either benign or malignant, cause symptoms related to pressure, destruction of nervous tissue, oedema and disruption of the blood supply. The neurological manifestations of a tumour affecting the nervous system depend on the location of the tumour and on its rate of growth.
Degenerative conditions
The causes of degenerative disorders of the nervous system are varied and involve atrophy of neurons and nerve fibres. The course of a degenerative disorder is generally gradual and progressive over many years. The effects of degenerative disorders include: progressive muscular atrophy; impaired speech, chewing, swallowing and breathing; deterioration of intellectual capacity; impaired motor function; and dementia.
Metabolic and endocrine disorders
Nervous system dysfunction may result from the effects of certain metabolic and endocrine disorders. Some nutritional deficiencies may affect nerve cells, resulting in their damage or death. For example, degeneration of the posterior and lateral columns of the spinal cord may occur from the vitamin B12 deficiency of pernicious anaemia. Disorders of cortical function, leading to confusion or coma, may result from a deficiency of thiamine (vitamin B1).
Specific endocrine disorders such as hypothyroidism result in decreased metabolic rate, and hypothermia can develop. If the body temperature falls below 30°C, unconsciousness will result. Myxoedema coma is characterised by exaggeration of the signs and symptoms of hypothyroidism, with neurological impairment leading to loss of consciousness.
Major manifestations of nervous system disorders
The manifestations of a nervous system disorder will vary depending on the type and severity of the disorder.
Headaches, or cephalalgia
Headaches, or cephalalgia, are common in a variety of disorders and situations ranging from functional disturbances of blood vessels to tension and stress. In neurological disorders, headaches are one of the most common symptoms. Headaches can result from compression, traction, displacement or inflammation of the cranial periosteum, the dura mater, cerebral arteries or branches of the cranial nerves. Headaches may also occur as a result of tension within extracranial structures such as muscles, air sinuses and blood vessels. Headaches are commonly classified as vascular, tension or traction–inflammatory.
Vascular headaches include migraine, cluster headaches, hypertension headaches and headaches resulting from temporal arteritis. Although the mechanisms of migraine are not completely understood, migraine appears to result from an inherited predisposition and seems to be precipitated by trigger factors such as stress, abrupt falls in oestrogen levels, low blood glucose levels and dietary intake. One theory is that migraine results from spasm of intracranial blood vessels and dilation of extracranial blood vessels. The classic characteristics of migraine headache include throbbing and a tendency for the attacks to be unilateral. Some attacks are preceded by a variety of visual disturbances, such as loss of half of the visual field or flashing lights across the visual fields. Some individuals experience vertigo, nausea and vomiting.
Cluster headaches are a rapid succession of attacks over several days, followed by remission. Previously thought to be caused by histamine sensitisation, cluster headaches are now considered to have a vascular cause. Headaches associated with severe hypertension may be intense and similar to those caused by intracranial lesions. Temporal arteritis causes severe, throbbing headaches in the region of the temporal artery and is sometimes accompanied by visual loss.
Tension headaches are caused by prolonged contraction (tension) of the neck, head or facial muscles. Tension headaches are frequently associated with psychological factors such as anxiety or depression. The pain tends to be bilateral and, unlike vascular headaches, is not throbbing in character.
Traction–inflammatory headaches: headaches of this type are related to increased intracranial pressure, which causes irritation of, and traction on, blood vessels and the dura mater within the skull. Inflammation of the meninges (meningitis) can also result in severe headache. Headaches of intracranial origin related to increased intracranial pressure vary from mild to excruciating depending on the location and cause, such as a tumour, lesion or cerebral oedema.
Sensory changes
Sensory changes, which can result from disorders of the brain, spinal cord or peripheral nerves, include alterations in the sense of touch, pain, temperature sensitivity and the loss of a sense of position. The loss of these sensations may be partial or complete. Common sensory disturbances include neuritis and neuralgia. Neuritis, characterised by pain and tenderness along the path of a nerve, can progress to complete loss of sensory and motor function. Neuralgia is characterised by severe stabbing pain, and can be caused by a variety of disorders affecting the nervous system. Other sensory changes that may accompany nervous system disorders include a loss of taste or smell, visual changes and hearing loss.
Motor changes
Alterations in motor function include localised or generalised weakness, with difficulty in moving normally. Muscle tone may be abnormally increased or decreased. A pronounced increase in tone is referred to as rigidity. Spasticity of muscles is an increased resistance to passive stretch, with rapid flexion of a joint. Abnormal movements include:
• Twitching: localised spasmodic contraction of a single muscle group
• Tremor: rhythmic quivering movements resulting from involuntary alternating contraction and relaxation of opposing groups of muscles
• Myoclonus: spasm of a muscle or a group of muscles
• Dystonia: intense irregular muscle spasms
• Athetosis: slow, writhing involuntary movements of the extremities
• Chorea: involuntary, purposeless, rapid jerky movements
• Dyskinesia: involuntary twitching of the limbs or facial muscles.
Symptoms of ataxia, a condition characterised by impaired ability to coordinate movement, may be caused by a lesion in the spinal cord or cerebellum. Dizziness or vertigo, when the individual is unable to maintain normal balance in a standing or seated position, may also be related to a disorder of the nervous system. Unusual gait or stance may result from motor or sensory deficits caused by a disorder of the nervous system, such as Parkinson’s disease. Paralysis, a symptom of motor disturbances, can occur in varying degrees with many nervous system disorders. Upper motor neuron lesions, in which the reflex area remains intact, generally cause spastic paralysis. Flaccid paralysis generally occurs in lower motor neuron lesions, which disrupt the reflex area.
Reflex changes
Reflex changes can provide evidence of damage to the nervous system. The absences of normal reflexes, or the presence of abnormal reflexes, generally indicate nervous system dysfunction. Reflexes are classed as either superficial (cutaneous) or deep tendon (muscle stretch). Superficial reflexes are elicited when a stimulus is applied to the skin surface or to mucous membrane. Deep tendon reflexes are elicited when a stimulus is applied to a tendon, bone or joint.
Altered awareness, personality or level of consciousness
A neurological disorder that results in altered brain structure may cause impairment of a person’s cognitive functions. They may experience difficulty in being able to think, remember, reason or understand. The person may also be confused in that orientation to time, place and person is impaired. Signs of reduced alertness or responsiveness may also be shown. Brain damage, for example as a result of a head injury, can cause a confused state characterised by fluctuating disorientation and incoherence.
Cerebral impairment may also cause mood changes and/or inappropriate emotional responses. Diffuse brain damage such as that caused by a large cerebral infarction may result in emotional instability or lability (a tendency to show alternating states of happiness and sadness that seem to be inappropriate). The person may also show signs of emotional flatness or apathy, demonstrated by a reactive absence of emotions. Alternatively, the client may become euphoric.
Damage to the brain can also result in altered states of consciousness, ranging from drowsiness and difficulty in being aroused by normal stimuli, to coma. More information on assessment of level of consciousness is provided later in this chapter.
ASSESSING NEUROLOGICAL STATUS
Assessment is of prime importance in the care of a client with a neurological disorder. The nurse must recognise changes that indicate a change in condition, as changes can occur rapidly and dramatically or develop over a period of days or weeks.
Intracranial pressure
Intracranial pressure is the pressure exerted by the CSF within the ventricles of the brain. However, it is more accurate to think in terms of intracranial ‘pressures’ rather than a single pressure, as the rigid skull is filled with brain tissue, intravascular blood and CSF. If any one of these three components increases in volume without a reciprocal change in volume of the other two, intracranial pressure will rise. Increased intracranial pressure affects the cerebral perfusion pressure, causing hypoxia, ischaemia, irreversible neurological damage and even death. Unless increased intracranial pressure is treated, the outcome will be herniation of a portion of the cerebrum through the tentorium, with pressure being exerted on the brainstem. The brainstem will then herniate through the foramen magnum, the only opening in the closed cranial vault.
Common causes of increased intracranial pressure include: space-occupying masses such as tumours, haematomas, abscesses or cerebral oedema; conditions that increase cerebral blood volume; and conditions that increase CSF. It is very important to identify early signs of increased intracranial pressure so that actions can be implemented to prevent or minimise irreversible brain damage. The manifestations of increased intracranial pressure include:
• Early signs and symptoms: deterioration in the level of consciousness (confusion, restlessness, lethargy), pupillary dysfunction, motor weakness such as hemiparesis and possible headaches
• Later signs and symptoms: continued deterioration in the level of consciousness (coma), possible vomiting, hemiplegia, decortication, decerebration, increasing systolic blood pressure, bradycardia and decreasing or irregular ventilations.
Neurological assessment
Neurological assessment includes checking the level of consciousness, the pupils, motor function, sensory function and the vital signs. The frequency with which assessment is performed and documented depends on the client’s condition and on the healthcare institution’s policy (see Procedural Guideline 33.1).
Procedural Guideline 33.1 Performing a neurological assessment
| Review and carry out the standard steps for all nursing procedures/interventions |
Adapted from Berman et al 2012; Crisp & Taylor 2009
Level of consciousness
The level of consciousness is a most important factor in neurological assessment, providing valid information about changes in neurological status. Change can occur slowly over the course of many days, or it can occur rapidly in a few minutes or hours. The rapidity of change is an indicator of the severity of the neurological problem. The client’s level of consciousness is evaluated by providing stimuli and observing the response. Sound and pain are the major stimuli used. Speaking to the client is the most common method of applying an auditory stimulus, while painful stimuli are reserved for the client with obviously decreased levels of consciousness. When spoken to, a fully conscious client should reply with an appropriate verbal response. A person with a decreased level of consciousness may respond in a puzzled way or may not respond at all, showing no response even when someone speaks directly into their ear (Crisp & Taylor 2009).
Painful tactile stimuli
Painful tactile stimuli may be necessary to arouse the semi-comatose client. Painful stimuli can be provided by exerting firm digital pressure on the nail beds, the Achilles tendon or the gastrocnemius muscle. Response to painful stimuli can be classified into:
• Purposeful, when the client winces, pushes the assessor away or withdraws the affected body part
• Non-purposeful, when the client moves the stimulated body part only slightly, or when the application of painful stimuli causes an extensor response (a contraction of muscles) only
• Unresponsive: when the individual shows no sign of reacting to painful stimuli.
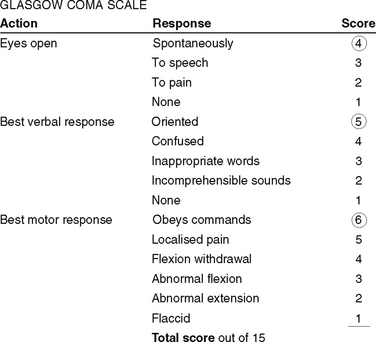
The Glasgow Coma Scale (GCS) (Fig 33.7) was originally designed to assess the level of consciousness in people with head injuries but is now used in a variety of settings. It has gained increasing acceptance as an accurate and effective means of evaluating levels of consciousness. Using the GCS, a score of 15 reflects a fully alert, well-oriented person, while a score of 8 or less is considered to indicate coma. The lowest possible score of 3 is indicative of brain death. The GCS is standardised world wide.
Evaluation of the pupils
Evaluating the pupils provides vital information about the brain and raised intracranial pressure. The findings in one pupil are compared with the findings in the other, and the differences between the two pupils are documented. The pupils are assessed for size, shape and reaction to light. Normally the pupils are equal in size (average diameter of 3.5 mm), round and they constrict briskly when light is shone into the eye. A pupil gauge may be used to estimate the size of each pupil. Abnormal responses of a pupil to light may be described as sluggish, non-reactive or fixed. Generally, any change in a pupil’s size, shape or reaction is indicative of an intracranial change.
Assessment of motor function
Assessment of motor function usually focuses on the arms and legs, and the identification of significant changes is important for denoting improvement, stabilisation or deterioration in the client’s condition. The techniques used to evaluate motor function depend on the client’s level of consciousness. In the conscious client, the assessment can be made by observing motor responses to directions; for example, by asking the client to squeeze the assessor’s hands. If the client is unconscious or is unable to provide accurate responses, the assessor must rely on observational skills to evaluate motor function.
Assessment of the vital signs
Assessing the vital signs (see Ch 18) provides data concerning vital functions of the body. The client’s temperature, pulse, ventilations and blood pressure are monitored and documented at a frequency that depends on their condition. Data from neurological assessments are documented according to the healthcare institution’s policy. Many institutions use a special neurological assessment chart, similar to the one illustrated in Figure 33.7.
DIAGNOSTIC TESTS
Specific tests may be performed for diagnostic purposes or to aid in evaluation of a client’s condition.
The neurological examination
The purpose of the neurological examination is to determine the presence or absence of disease in the nervous system by assessing cerebral, cranial nerve, motor, sensory and reflex function. Evaluation of cerebral function is performed by assessing the client’s general behaviour and cognitive functions, such as orientation to time and place, concentration, memory, vocabulary and abstract reasoning. Evaluation of the cranial nerves involves assessing:
• The olfactory nerve: the sense of smell is tested by obstructing one nostril while testing the other. A variety of substances is placed near the unobstructed nostril and the client is asked to identify the odour of each
• The optic nerve: each eye is tested to assess visual acuity and visual fields. The fundus of each eye is assessed by ophthalmoscopic examination
• The oculomotor, trochlear and abducens nerves: these three nerves are generally tested together, as they supply the various muscles that rotate the eyeball. The ophthalmoscope is used during the assessment; the pupils are observed for size, shape and equality, and movement of the eyes is evaluated by requesting the client to follow a finger through the six cardinal areas of vision
• The trigeminal nerve: the sensory component of this nerve is tested with the client’s eyes closed. Test tubes of warm and cold water are brought into contact with the skin of the face to check temperature perception. Touching the face with a wisp of cotton checks perception of light touch. Pain perception is evaluated either by applying pressure or by touching areas of the face with the point of a pin. The motor component of the trigeminal nerve is evaluated by asking the client to clench and unclench the teeth, and by observing their ability to open the mouth against resistance. The corneal reflex is assessed by lightly stroking the cornea with a wisp of cotton. If the corneal reflex is intact, the client will automatically blink
• The facial nerve: the sensory component of this nerve is assessed by placing sweet, salty, sour and bitter substances on various areas of the tongue, and asking the client to identify each taste. The motor component of the facial nerve is assessed by requesting the client to perform specific facial movements such as smiling, closing the eyes, pursing the lips and wrinkling the forehead
• The acoustic nerve: generally, unless the client has a history of vertigo, only the hearing branch of this nerve is assessed. A series of hearing tests is performed, and hearing in both ears is compared. For a more precise assessment of hearing acuity, a tuning fork is used
• The glossopharyngeal and vagus nerves: these nerves are usually tested together, as they are closely related both anatomically and functionally. A series of tests is performed to assess the gag and swallowing reflexes
• The spinal accessory nerve: this nerve is tested by evaluating the strength of the trapezius and sternocleidomastoid muscles; for example, by requesting the client to shrug the shoulders against resistance and by asking them to turn their head to one side and push their chin against the assessor’s hand
• The hypoglossal nerve: the strength and movement of the tongue muscles are evaluated by testing the client’s ability to protrude the tongue, and also by requesting them to push their tongue against a tongue depressor.
Evaluation of motor function
Evaluating motor function involves assessing the client’s gait, posture, muscle strength and tone, balance and coordination. The assessor observes for abnormalities and compares the findings on both sides of the body for asymmetry.
Evaluation of sensory function
Evaluating sensory function involves assessing the client’s ability to perceive various sensations with their eyes closed. Assessment includes testing of sensitivity to touch, pain, temperature, testing of joint motion and position and assessment of discriminative function and vibratory sensation.
Evaluation of reflexes
Evaluation of reflexes involves testing the two types of reflex to assess the integrity of the motor and sensory systems.
The superficial reflexes
These include the upper abdominal, lower abdominal, gluteal and plantar reflexes. The abdominal and gluteal reflexes are evaluated by applying a stimulus to the skin surface; for example, stroking with a finger or pointed object and observing for muscle contraction. The plantar reflex is evaluated by stroking the sole of the foot, with one continuous movement from the heel to the toes. Normally, the big toe curls downwards in response to this stimulus. An abnormal response, Babinski’s sign, when there is dorsiflexion of the big toe and fanning of the other toes, indicates upper motor neuron disease.
The deep tendon reflexes
These include the biceps, triceps, quadriceps and Achilles tendons. Deep tendon reflexes are elicited by using a percussion hammer and observing the response, as follows:
• The biceps reflex is tested with the arm partially flexed at the elbow and the palm down. When the hammer is applied to the biceps tendon, the elbow should flex
• The triceps reflex is tested with the arm partially flexed at the elbow and the palm directed towards the body. When the hammer is applied to the triceps tendon, the elbow should extend
• The quadriceps reflex is tested with the knee flexed. When the patellar tendon is struck with the hammer, the knee should extend
• The Achilles reflex is tested with the knee flexed. When the Achilles’ tendon is struck with the hammer, the foot should plantar flex.
Radiographic examination
X-ray
Plain x-ray films of the skull may be performed to detect fractures, to aid in the diagnosis of pituitary tumours or to detect congenital abnormalities. X-ray films of the spine may be performed to detect trauma to the vertebral column or to aid in the diagnosis of conditions that cause motor or sensory impairment.
Computerised tomography scan
Computerised tomography (CT) is commonly used to diagnose intracranial and spinal cord lesions. It is usually non-invasive but a contrast dye is sometimes administered to visualise blood vessels or to define lesions. The client lies on an x-ray table, with the head immobilised and face uncovered. The head is moved into the scanner, and a moveable frame revolves around it while x-ray films are taken. If a contrast agent is used the client may feel warm and experience a transient headache, a salty taste and nausea.
Myelogram
A myelogram involves fluoroscopy and radiography to evaluate the spinal cord and vertebral column after injection of a contrast medium into the subarachnoid space. A needle is inserted, most often in the lumbar area, into the subarachnoid space and about 10 mL of CSF is removed. Contrast medium is then injected through the needle and the client is positioned to allow the medium to flow through the subarachnoid space. A series of x-ray films are taken, after which the contrast medium may be either withdrawn or allowed to remain in the CSF. Water-soluble agents are allowed to remain, as they will eventually be excreted by the kidneys.
Angiography
Cerebral angiography involves injecting a radio-opaque contrast medium into an artery for radiological visualisation of the intracranial and extracranial blood vessels. Common injection sites are the carotid or femoral arteries, with x-ray films taken at various intervals after injection of the medium. Cerebral angiography may be performed using either local or general anaesthetic. Digital subtraction angiography is a computer-assisted radiographic procedure for visualising extracranial and intracranial vessels and involves injection of a contrast medium through a catheter into the superior vena cava. Cerebral vessels are visualised on a screen, and pictures taken.
Pneumoencephalography
Pneumoencephalography is performed infrequently since the advent of the CT scan. Pneumoencephalography allows radiographic examination of the cerebral ventricles after injection of air or oxygen into the subarachnoid space.
Magnetic resonance imaging (MRI)
An MRI is a non-invasive procedure in which the individual is placed in a strong magnetic field and is subjected to precise computer-programmed bursts of radio pulse waves. The sharpness and detail of the images produced assist diagnosis by providing identification of abnormalities and can detect neurological disorders with structural changes, for example, stroke, tumour, infection. MRI is contraindicated in clients with pacemakers, metallic aneurysm clips and some metallic prostheses.
Positron emission tomography (PET) scanning
PET scanning is a non-invasive nuclear imaging technique used to detect biochemical and physiological abnormalities. The client is injected with a nuclide that reacts with electrons and produces gamma-ray photons. A scanner detects the gamma rays and codes this data into a computer. Radioisotopes evaluate cellular metabolism, and may show a typical pattern for Alzheimer’s disease, and can be used to differentiate tumour reoccurrence from radiation necrosis. The computer then reconstructs cross-sectional images of the tissues being examined. PET is not widely available.
Electroencephalography (EEG)
An electroencephalogram (EEG) is a recording of the electrical activity of the brain (brainwaves). Surface electrodes are attached to the scalp with a paste and transmit the brain’s electrical impulses to a machine that records them as brainwaves on strips of paper. Brainwaves are recorded while the client is at rest, after hyperventilation, with photic stimulation, after a sensory stimulus and during sleep (see Clinical Interest Box 33.1).
CLINICAL INTEREST BOX 33.1 Care of the client undergoing an EEG
Explain the procedure to the client, emphasising the importance of cooperation
Withhold fluids, foods and medications (as prescribed) that may stimulate or depress brainwaves. These include anticonvulsants, tranquillisers, depressants and caffeine-containing foods (e.g. coffee, tea, colas and chocolate). Medications are usually withheld for 24–48 hours before the test
Help the client to wash their hair before the test
The test is painless and will be performed while the client sits in a comfortable chair or lies on a stretcher
The electrodes are applied to the scalp with a thick paste
During the test the client will first be asked to breathe in and out deeply for a few minutes, then to close their eyes while a light is flashed on them and, finally, to lie quietly with eyes closed
After the test, the nurse will help the client wash the paste out of their hair
Cerebrospinal fluid analysis
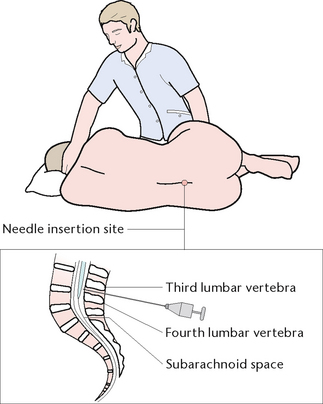
A sample of CSF is generally obtained by lumbar puncture (Fig 33.8) or, less commonly, by cisternal puncture. A lumbar puncture may be performed for either diagnostic or therapeutic purposes. The diagnostic indications include:
• Examination of CSF for the presence of blood or microorganisms
• Injection of air, oxygen or radio-opaque material to visualise parts of the central nervous system radiologically
Therapeutic indications include introduction of spinal anaesthesia for surgery, and intrathecal injection of medications.
For the procedure the client assumes a lateral position, with their back curled and their knees flexed as close to their chest as possible. The head should be bent forward so that the chin touches their chest. After preparation of the site, the medical officer inserts a spinal needle with a stylus (a fine probe) between the third and fourth lumbar vertebrae into the subarachnoid space. When the stylus is removed, CSF should drip from the needle. If the lumbar puncture is being performed for diagnostic purposes, a manometer may be attached to the needle to measure CSF pressure. Samples of CSF are then collected for visual and laboratory examination. When the procedure is completed, the needle is withdrawn and an adhesive dressing applied over the puncture site.
Queckenstedt’s test
Queckenstedt’s test is sometimes performed as part of the lumbar puncture if an obstruction of the spinal subarachnoid space is suspected. While the lumbar puncture needle is in place, an assistant manually compresses both jugular veins for 10 seconds. The CSF pressure is read and recorded at 5-second intervals and again after release of jugular pressure. Normally, occlusion of the veins of the neck causes an immediate rise in spinal fluid pressure; if the vertebral canal is blocked, no rise occurs. The test is contraindicated if the client has increased intracranial pressure or cerebral bleeding, because brainstem herniation or further bleeding can occur.
Cisternal puncture
A cisternal puncture may be performed to obtain a sample of CSF when a lumbar puncture is contraindicated. A needle, with stylus, is inserted into the cisterna magnum and a sample of CSF withdrawn. Cisternal puncture is a potentially dangerous procedure because the needle is positioned close to the brainstem.
Further investigations
Echoencephalography (ECHO)
An echoencephalogram (ECHO) is a test that uses pulsating ultrasonic waves to indicate deviation of the cerebral midline structures. Since the advent of computerised tomography, echoencephalography is used infrequently.
Electromyography
This procedure involves recording the electrical activity of a muscle and peripheral nerve and may be performed to aid in diagnosis of neuromuscular disorders. Needle electrodes are inserted into the muscle to be examined, and recordings are made of the electrical activity of the muscle at rest and during contraction.
Nerve conduction studies
These studies involve application of an electrical stimulus to peripheral nerves, and measurement of their response by means of an oscilloscope.
Caloric testing for vestibular function
Caloric testing is a diagnostic procedure designed to evaluate the vestibular portion of the eighth cranial (acoustic) nerve. The underlying principle of the procedure is that thermal stimulation of the vestibular end organs with warm and cold water will elicit the oculovestibular reflex. This reflex, if intact, results in induced nystagmus and eye movement in response to cold or warm water irrigation of the external auditory canal. Each external meatus is irrigated for up to 3 minutes with both cold and warm water, with a pause of at least 5 minutes between irrigations. Irrigation with cold water should result in slow nystagmic eye movements on the same side, followed by rapid nystagmus to the opposite side. Irrigation with warm water should produce rapid nystagmus on the same side.
SPECIFIC DISORDERS OF THE NERVOUS SYSTEM
Disorders of the nervous system may be congenital or genetic, due to multiple causes, degenerative, infectious or inflammatory, immunological, neoplastic, obstructive or traumatic.
Congenital disorders
Structural congenital abnormalities include anencephaly, spinal cord defects and hydrocephalus.
Anencephaly
Anencephaly is the failure of normal development of the brain (cerebral hemispheres and cerebellum) and scalp. The precise cause is unknown, and babies with the disorder do not live.
Spinal cord defects
These include spina bifida, meningocele and myelo-meningocele. These conditions are the result of incomplete closure of the neural tube during the first 3 months of embryonic development. Causes are thought to include maternal exposure to viruses, radiation and other environmental factors.
In severe forms, spina bifida involves incomplete closure of one or more of the vertebrae, causing protrusion of the spinal contents in an external sac. In spina bifida with meningocele, the sac contains meninges and CSF. In spina bifida with myelomeningocele the sac contains meninges, CSF and a portion of the spinal cord or nerve roots. Manifestations of congenital spinal cord defects vary and include a depression, dimple or tuft of hair on the skin over the spinal defect. The more severe defects cause neurological dysfunction such as paralysis of the legs, bowel and bladder incontinence and hydrocephalus.
Hydrocephalus
Hydrocephalus is an excessive accumulation of CSF within the ventricles of the brain. It may result from an obstruction in CSF flow or from faulty absorption of CSF. The condition can also occur as a result of cerebral injury or disease. In infants, the obvious manifestation of hydrocephalus is abnormal enlargement of the head. Other characteristics include distended scalp veins, thin and fragile scalp skin, downward displacement of the eyes, a shrill high-pitched cry, irritability and abnormal muscle tone of the legs.
Genetic disorders
Hereditary genetic defects include muscular dystrophy, Huntington’s chorea and neurofibromatosis.
Muscular dystrophy
Muscular dystrophy is a group of congenital disorders characterised by progressive wasting and weakness of muscles. Duchenne’s muscular dystrophy, which begins to manifest between the ages of 3 and 5 years, is the most common and severe form. Initially it affects the leg and pelvic muscles but there is progressive involvement of all voluntary muscles. Later in the disease, progressive weakening of cardiac and respiratory muscles results in heart or respiratory failure. Early manifestations of Duchenne’s muscular dystrophy include a waddling gait, lordosis (increased curvature of the lumbar spine) and marked difficulty rising from a supine to a standing position. As the disease progresses, facial, oropharyngeal and respiratory muscles become involved.
Huntington’s chorea
Huntington’s chorea is a disorder in which degeneration of the cerebral cortex and basal ganglia causes chronic progressive choreiform movements and mental deterioration. Onset is generally in early middle age, and the individual gradually develops progressively severe choreiform movements and dementia. The movements usually begin slowly, with facial grimacing and jerking arm actions. Over time, the movements become frequent, erratic and violent, affecting the trunk and lower limbs. Dementia may be mild at first but eventually severely disrupts the personality.
Neurofibromatosis
Neurofibromatosis is characterised by a variety of congenital abnormalities and the condition is usually classified according to which parts of the nervous system are affected. In the peripheral form, multiple cutaneous and subcutaneous nodules of varying size occur. Subcutaneous nodules may attach to the peripheral portion of the nerve, causing pain or pressure and, rarely, sensory loss in the distribution of the affected nerve. Neuromas, which are an overgrowth of subcutaneous tissue, may reach enormous sizes and commonly affect the face, scalp, neck and chest. Neurological symptoms may appear if the tumours cause pressure on the brain or spinal cord.
Disorders of multiple cause
Cerebral palsy
Cerebral palsy comprises a group of neuromotor disorders resulting from prenatal, perinatal or postnatal cerebral hypoxia or damage. The incidence of cerebral palsy is highest in premature infants or in infants who have experienced a difficult birth resulting in cerebral damage. Causative factors include: chromosomal abnormalities; prenatal factors such as maternal infections, exposure to harmful chemicals or malnutrition; perinatal factors such as premature birth or instrumental delivery causing cerebral anoxia; and postnatal factors such as trauma, infection or malnutrition causing cerebral damage.
The manifestations of cerebral palsy range from mild muscle incoordination to severe spasticity. The spastic form of the disorder is characterised by rapid alternating muscle contraction and relaxation, muscle weakness and underdevelopment and muscle contraction in response to manipulation. The athetoid form of cerebral palsy is characterised by grimacing, writhing and jerking involuntary movements, which become more severe during stress. Ataxic cerebral palsy is characterised by disturbed balance, incoordination, muscle weakness and tremor. In addition to the range of motor deficits, the individual may experience sensory deficits such as speech, visual or hearing impairment. Intellectual disability accompanies cerebral palsy in about 40% of cases.
Cerebral aneurysm
A cerebral aneurysm is an abnormality of the wall of a cerebral artery that results in a localised dilation. If the aneurysm ruptures, blood enters the subarachnoid space or cerebral tissue. Causative factors include congenital defects in the arterial walls, sclerotic changes in blood vessels, hypertension and cerebral trauma. Manifestations of a cerebral aneurysm do not generally appear until the aneurysm ruptures. The most common symptom of rupture is the sudden onset of a severe headache, which may be accompanied by nausea and vomiting, motor deficits, visual disturbances and loss of consciousness. A cerebral aneurysm may be detected before it ruptures if the individual shows signs of oculomotor nerve compression, eyelid ptosis and a pupil that is sluggish or non-reactive.
Transient ischaemic attacks
Transient ischaemic attacks (TIAs) are recurrent episodes of neurological deficit. The attacks, which may last from seconds to hours, are generally considered to be warning signs of an impending thrombotic cerebrovascular accident (stroke). The characteristics of a TIA, which may be caused by micro-emboli or arteriole spasm, are various symptoms of neurological dysfunction followed by a return of normal function. Symptoms include double vision, slurred or thick speech, unilateral loss of vision, staggering or uncoordinated gait, unilateral weakness or numbness, dizziness and falling because of leg weakness.
Trigeminal neuralgia
Trigeminal neuralgia is a painful disorder of one or more branches of the trigeminal nerve that produces paroxysmal attacks of excruciating facial pain. While the cause is often unknown, the disorder may be associated with other neurological conditions such as aneurysms, cerebral tumours or multiple sclerosis. The individual experiences excruciating burning pain, which generally occurs suddenly in response to a stimulus, such as a draft of cold air, drinking hot or cold fluids, brushing the teeth or speaking or laughing. The frequency of attacks varies from many times a day to several times a month or year.
Intellectual disability
Intellectual disability is a syndrome of incomplete intellectual development associated with impaired learning and social adjustment. The causes include:
• Prenatal factors such as metabolic disorders, chromosomal abnormalities, cranial malformation, maternal infections, malnutrition or anoxia
• Perinatal factors such as prematurity, anoxia or intracranial haemorrhage
• Postnatal factors such as cerebral injury, central nervous system infections, anoxia, neoplasms, degenerative diseases, cerebral haemorrhage, nutritional deficiencies and emotional deprivation.
Manifestations include poor motor development, impaired concepts of space and time, learning difficulties, inappropriate behaviour and difficulty with social interactions.
Peripheral neuritis
Peripheral neuritis (polyneuritis) is the degeneration of peripheral nerves, resulting in muscle weakness and atrophy, sensory loss and decreased or absent tendon reflexes. Causes include chronic intoxication (alcohol, arsenic, lead), metabolic and inflammatory disorders (diabetes mellitus, rheumatoid arthritis), nutrient deficiencies (thiamine) and infectious diseases (meningitis or Guillain–Barré syndrome). Manifestations usually develop slowly, beginning with leg pains and numbness or tingling in the feet and hands. As the disease progresses the individual experiences flaccid paralysis, muscle wasting, pain of varying intensity and loss of reflexes in the legs and arms. Footdrop, ataxic gait and inability to walk will eventually occur.
Guillain–Barré syndrome
Guillain-Barré Syndrome (GBS) is an acute inflammatory polyneuropathy disease (Schub et al 2011). It is characterised by rapid and progressive neuromuscular paralysis (Schub et al 2011). There is no known cause of GBS; however, up to two-thirds of clients who are diagnosed with this condition have a 1- to 3-week previous history of upper respiratory or gastrointestinal infection (Lugg 2010). What happens in GBS is antiganglioside antibodies attack Schwann cells of the myelin sheath, causing demyelination, usually of the peripheral nerves which in turn halts nerve conduction (Schub et al 2011). Clients with GBS will initially complain of decreased function, weakness and deceased sensation in their arms and legs, with or without pain (Lugg 2010). This rapidly develops into muscle weakness, commencing distally then travelling to proximal with decreased reflexes and sensations (Lugg 2010). For some clients the disease progression will stop here; they will experience difficulty walking but will be able to be discharged to home (Lugg 2010). Others will progress to total paralysis. Thirty per cent of clients with GBS will require mechanical ventilation due to respiratory dysfunction (Lugg 2010). The disease progression is usually 4–8 weeks and is confirmed with a lumbar puncture, electromyography and nerve conduction studies. Treatment of GBS is supportive, Schwann cells will re-myelinate and most clients can expect a full recovery (Schub et al 2011). When caring for the client with GBS the nurse should assess airway and breathing, refer to speech pathology and maintain the client as nil by mouth until otherwise ordered, ensure adequate analgesia, perform pressure area care and take steps to reassure the client.
Bell’s palsy
Bell’s palsy is a disorder of the seventh cranial nerve that produces unilateral facial weakness or paralysis. An inflammatory reaction occurs in or around cranial nerve VII, resulting in nerve compression and the onset of flaccid facial paralysis. Factors responsible for the inflammatory reaction include infection, prolonged exposure to cold temperature and local trauma. The seventh cranial nerve can also be affected by other conditions such as a cerebral tumour, meningitis or a middle-ear infection. Manifestations are unilateral facial weakness, which is sometimes associated with pain around the angle of the jaw or behind the ear. On the affected side the mouth droops and the individual is unable to wrinkle the forehead, close the eyelid or smile. There may be excessive watering from the affected eye and drooling of saliva from the affected side of the mouth.
Seizure disorders
Seizure disorders may be primary and idiopathic, or secondary and symptomatic of a central nervous system disorder. The most common type of seizure disorder is epilepsy. Seizures may be focal (partial), or generalised. Focal seizures generally affect a specific body part, and the symptoms of an attack depend on the location of the cerebral focus. For example, the focal motor seizure occurs from a lesion in the motor cortex or strip. Typically it causes stiffening or jerking in one extremity that is accompanied by numbness or tingling.
Absence, or petit mal, seizures last only a few seconds. They generally begin with a brief change in the level of consciousness, which is indicated by a blank stare, eyelid fluttering or head nodding or a pause in conversation. The individual generally retains posture and returns to pre-seizure activity without difficulty. This type of epilepsy usually occurs in childhood and may continue into early adolescence. Some partial seizures may progress to become generalised seizures. These are termed as secondary generalised seizures.
Although seizures may result from a nervous system disorder, they may be caused by many other factors and are often idiopathic. The common classification of seizures is given in Table 33.2.
Table 33.2 Common classification of seizures
| 1 | Focal (partial) seizures |
| About 60% of people with epilepsy have focal (partial) seizures. These seizures can often be subtle or unusual, and may go unnoticed or be mistaken for anything from intoxication to daydreaming. Seizure activity starts in one area of the brain and may spread to other regions of the brain. | |
| Types of focal (partial) seizures are: | |
|
• Focal seizure—awareness retained (formerly simple partial seizures) • Focal dyscognitive seizures—awareness altered (formerly complex partial seizures) • Focal seizures evolving to a bilateral convulsive seizure (formerly secondarily generalised tonic-clonic*) |
|
| 2 | Generalised seizures |
| Generalised seizures are the result of abnormal activity in both hemispheres of the brain simultaneously. Because of this, consciousness is lost at the onset of the seizure. There are many types of generalised seizures: | |
| 3 | Unknown |
| This a grouping of seizures that cannot be diagnosed as either a focal or generalised seizure and are thus grouped as unknown. | |
Epilepsy Action Australia (nd) Seizure types and classifcation. Available: http://www.epilepsy.org.au/about-epilepsy/understanding-epilepsy/seizure-types-classifcation
Most people will only have one or two seizure type(s), which may vary in severity. A person with severe epilepsy or significant damage to the brain may experience several different seizure types.
* Note: Sometimes a seizure starts as a focal (partial) seizure and then becomes a generalised seizure—almost always a tonic-clonic seizure.
The most common generalised seizure is referred to as a tonic–clonic, or grand mal, seizure or convulsion. This type of seizure usually consists of three phases:
1. Aura. The aura (which is not always experienced) is a warning of an impending seizure. An aura is a sensation (e.g. a specific taste or smell) experienced by the individual immediately before a seizure. The seizure commonly begins with a loud cry, which is caused by air being forced out through the vocal cords that are in spasm
2. Tonic–clonic (convulsive) phase. The individual then loses consciousness and may fall. The muscles become rigid, then alternate between episodes of muscle spasm and relaxation (tonus and clonus), resulting in jerky spasmodic body movements. Tongue biting, incontinence of urine, laboured breathing, apnoea and cyanosis may occur
3. Post-convulsive phase. The seizure generally stops within 2–5 minutes, when abnormal electrical conduction in the brain ceases. The individual regains consciousness but may be dazed and confused or fall asleep. Automatisms are more commonly associated with complex partial seizures.
Status epilepticus is a condition in which the individual experiences continuous seizures without regaining consciousness in between. It is generally accompanied by respiratory distress.
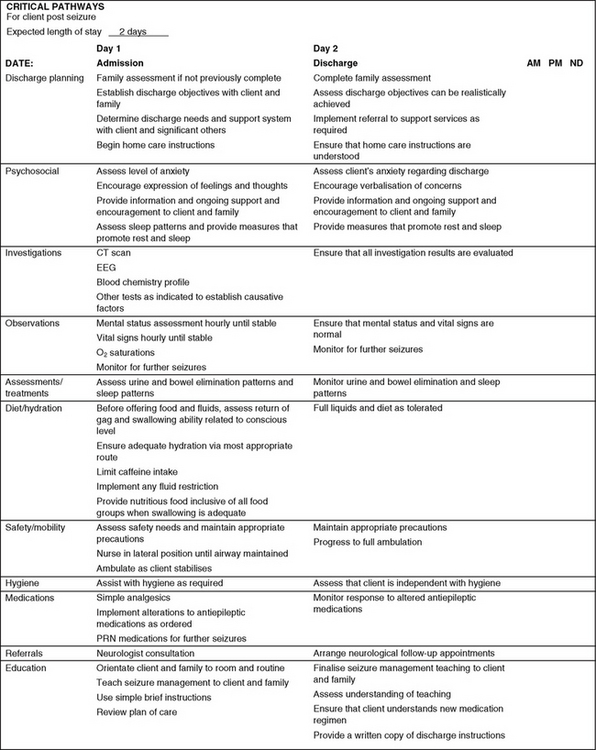
Figure 33.9 shows a sample nursing critical pathway for managing a client after a seizure, and Clinical Interest Box 33.2 provides an outline of teaching for home care of clients in relation to seizures.
CLINICAL INTEREST BOX 33.2 Teaching for home care of clients affected by generalised seizures
Teaching must be planned around a systematic assessment of the needs of both the client and their significant others. Significant others need to be included so that they can learn seizure management, care and observations. The importance of safety and maintenance of a patent airway should be stressed. The following recommendations assist the client and significant others to adjust:
• Correct misconceptions, fears and myths about epilepsy
• Encourage both the client and their significant others to express their feelings
• Provide the name and location of community and national resources; for example, the Epilepsy Foundation of Victoria (www.epinet.org.au). Facilitate socialisation with others facing the same issues
• Stress the importance of follow-up care and keeping medical appointments
• Refer the client to employment or vocational counselling as needed
• Review any state and local laws that apply to people with seizure disorders. Usually a driver’s licence can be reinstated after a 2-year seizure-free period and a letter from a medical practitioner
• Stress the importance of wearing a medical alert bracelet and carrying a medical alert card at all times
• Emphasise the importance of aura identification and plan action to take
• Emphasise the importance of taking anticonvulsant medication as prescribed, even when seizures no longer occur
• Avoid physical and emotional stress
• Help clients develop a positive focus on life
• In general, alcohol should be avoided and caffeine limited
• Discuss factors that may trigger a seizure (fatigue, abrupt stopping of medication, flashing video games)
Degenerative disorders
Parkinson’s disease
Parkinson’s disease is a degenerative process of nerve cells in the basal ganglia and substantia nigra. The substantia nigra is an area in the basal ganglia considered necessary for motor control. Although the precise cause of the disorder is unknown, research has demonstrated that a dopamine deficiency prevents affected brain cells from functioning normally. Dopamine is a neurotransmitter that plays a role in the transmission of nerve impulses between synapses. Factors implicated in the development of Parkinson’s disease include cerebral atherosclerosis and long-term therapy with drugs such as haloperidol and phenothiazine.
Manifestations of Parkinson’s disease are related to disturbances of movement: tremor, muscle rigidity and dyskinesia. The most common initial symptom is tremor; for example, ‘pill-rolling’ movements of the fingers, and to-and-fro head tremors. Tremors are aggravated by fatigue and stress, and decrease when the individual performs a purposeful activity or is asleep. The person experiences difficulty in initiating voluntary movement and loss of posture control, so that walking is with the body bent forwards. The gait consists of short shuffling steps that are slowly initiated. Facial expression becomes mask-like, and the voice is commonly high-pitched and monotone. The person’s intelligence is not affected.
Amyotrophic lateral sclerosis
Amyotrophic lateral sclerosis, which is the most common form of motor neuron disease, is a progressive degenerative condition that is generally fatal within 3–10 years after onset. The disease affects the upper and lower motor neurons of the central nervous system, resulting in progressive muscular atrophy, progressive bulbar palsy and upper motor neuron deficits. While the cause is unknown, the disease is thought to result from viral, metabolic, toxic, infectious and immunological factors. Manifestations include skeletal muscle weakness and atrophy and impaired speech, chewing, swallowing and breathing. The cause of death is commonly respiratory muscle weakness and bulbar palsy causing respiratory failure.
Alzheimer’s disease
Alzheimer’s disease is a progressive degenerative disorder that causes cerebral atrophy and dementia. Although the precise cause is unknown, several theories propose that the disorder may result from a genetic factor, immunological dysfunction, a toxin or a virus. Recent research has focused on the role of neurotransmitters and on the effect of a deficiency of acetylcholine in the brain as a cause of the condition. Manifestations of the disease generally occur in three stages:
1. Memory loss, decline in judgment and logic, disorientation, global aphasia, irritability, mood swings and agitation
2. Neglect of hygiene, inability to carry out deliberate voluntary movements (apraxia), inability to recognise the nature or use of objects (agnosia), repetition of a motor or verbal action (perseveration) and seizures
Delirium is a common mental disorder affecting older adults. The characteristics of delirium are listed in Clinical Interest Box 33.3. The acute condition is often misdiagnosed as a form of dementia and the underlying cause therefore being missed. A history of the client’s behaviour before delirium developed is essential in early recognition of the condition.
CLINICAL INTEREST BOX 33.3 Clinical criteria for delirium
• Delirium is an acute disturbance of consciousness that is accompanied by a change in cognition. It cannot be accounted for by a preexisting or evolving dementia. Delirium develops over a short period of time, usually hours to days, and tends to fluctuate during the course of the day. It is usually a direct physiological consequence of a general medical condition.
• There is reduced clarity of awareness of the environment
• Ability to focus, sustain or shift attention is impaired
• Person is easily distracted by irrelevant stimuli
• There is an accompanying change in cognition (memory impairment, disorientation or language disturbance)
• Recent memory is most commonly affected
• Disorientation is usually shown, with a person disoriented to time or place
• Language disturbance may involve impaired ability to name objects or ability to write; speech may be rambling
• Perceptual disturbances may include misinterpretations, illusions or hallucinations
(Crisp & Taylor 2009:673)
Immunological disorders
Multiple sclerosis
Multiple sclerosis is a disorder characterised by progressive demyelination of nerve fibres in the spinal cord and brain. Patches of demyelination throughout the central nervous system result in varied neurological dysfunction. The cause is unknown, but the disease is thought to result from viral or immunological factors. Manifestations vary depending on the areas of the central nervous system that are affected. Some clients experience mild exacerbations, with long remission periods, while others have frequent relapses, with increasing residual deficits. The most common initial symptoms are fatigue, motor weakness and visual disturbances. Other characteristic changes include numbness and tingling sensations, intention tremor, gait ataxia, paralysis, urinary disturbances and emotional lability. Clinical Interest Box 33.4 provides a teaching plan for the client as well as their significant others.
CLINICAL INTEREST BOX 33.4 Teaching checklist—the client with multiple sclerosis
In formulating a teaching plan it is important that the client’s significant others are included. The following aspects may be considered:
• Facilitate access to the Multiple Sclerosis Society of Australia (www.msaustralia.org.au)
• Ensure that the client understands the clinical course of multiple sclerosis. Dispel any myths
• Identify strategies to manage symptoms such as dysphagia or altered cognitive responses
• Plan strategies for preventing complications such as pressure ulcers or depression
• Identify strategies for minimising fatigue
• Explain how to prevent injury
• Discuss ways to adapt to sexual dysfunction
• Develop strategies to control bowel and bladder function
• Explain benefits of continued physical activity and exercise
• Identify ways to minimise immobility and spasticity
• Describe the medication regimen and possible adverse effects.
Myasthenia gravis
Myasthenia gravis is a chronic neuromuscular disorder that affects voluntary muscles and is characterised by fluctuating muscle weakness that is exacerbated by exercise. The disease is considered to be autoimmune in origin, resulting in an acetylcholine-receptor deficiency. The thymus gland is also thought to be involved in the disease because the gland is abnormal and remains active after puberty in clients with myasthenia gravis.
Manifestations include progressive weakness of certain voluntary muscles, with some improvement in muscle function after rest. The eye muscles are most commonly affected, with drooping of the eyelids (ptosis) and double vision (diplopia). Other affected muscles include those involved with facial expression, speech, chewing and swallowing. The client may experience problems with saliva, nasal regurgitation and choking. The shoulder and neck muscles may be affected so that the head tends to fall forwards. Weakened respiratory muscles make breathing difficult and predispose the person to respiratory tract infections.
Infectious and inflammatory conditions
Meningitis
Meningitis is inflammation of the meninges and can be caused by viruses, bacteria or fungi. The inflammation may involve one or all three layers of the meninges. Meningitis often begins when the causative organism enters the subarachnoid space, then the infection spreads because of the open communication over the brain’s convexity. The accumulation of exudate from the inflammatory process over the convexities or in the ventricles can obstruct the flow of CSF. Aseptic meningitis is thought to occur from meningeal irritation resulting from encephalitis, leukaemia, lymphoma or the presence of blood in the subarachnoid space. The major manifestations of meningitis are severe headaches, pyrexia, irritability, neck rigidity, photophobia and pain in the back and limbs. Other manifestations are alterations in mental status, altered levels of consciousness and restlessness. Vomiting may occur, and cranial nerve involvement causes visual disturbances, pupil abnormalities, strabismus and vertigo. There may be generalised seizures due to cerebral oedema.
Encephalitis
Encephalitis is inflammation of the brain tissue caused by viruses, bacteria, fungi or protozoans. Endemic encephalitis begins in a non-human host or reservoir from which the virus is transmitted to humans, for example, through mosquito bites. After the pathogen gains access to the central nervous system via the bloodstream or along nerves, the white matter and meninges develop non-suppurative inflammation, and diffuse cerebral oedema results. Initial manifestations are headaches, pyrexia, vomiting, malaise and muscular aches and pains. These are often followed by alterations in the level of consciousness, confusion, motor and sensory deficits, hyperirritability and meningeal signs.
Brain abscess
A brain abscess is a collection of pus, usually occurring in the temporal lobes or the cerebellum. A brain abscess is accompanied by cerebral oedema and congestion. Most brain abscesses develop secondary to a primary source of infection such as mastoiditis or otitis media; or they may develop from a septic focus in the respiratory tract or, less often, from a pelvic or cardiac source. A small percentage result from a penetrating head wound such as a gunshot injury.
Manifestations include headache, pyrexia, vomiting, alterations in the level of consciousness, and local or generalised seizures. Other features differ according to the site of the abscess and include motor, sensory and speech disturbances.
Myelitis
Myelitis is the term that applies to a group of infective and non-infective processes that affect the spinal cord. Myelitis can be due to viruses, occur secondary to meningeal inflammation or be of unknown aetiology. The most common viral diseases causing myelitis are poliomyelitis and herpes zoster. Manifestations include a sudden onset of motor paresis, accompanied by other neurological deficits such as loss of sensory and sphincter functions.
Herpes zoster
Herpes zoster is a viral disorder that causes inflammation of the posterior root ganglia. The condition develops from reactivation of the varicella virus, the virus responsible for chickenpox. There is also evidence of a relationship between herpes zoster and certain systemic infections, neoplasms and immunosuppressive therapy. Manifestations include mild to severe neuralgic pain in the affected nerve root distribution. The pain, which may be burning, tingling, dull or sharp, may occur with or be followed by skin reddening and eruption of vesicles. The vesicles become pustules and develop a crust within 1–2 weeks. If infection or ulceration accompanies the vesicles, permanent scarring may result.
Occasionally, herpes zoster involves the cranial nerves, especially the trigeminal or oculomotor nerve. Trigeminal involvement causes eye pain and, possibly, corneal damage and impaired vision. Oculomotor involvement may result in conjunctivitis or ptosis. Rarely, herpes zoster leads to generalised central nervous system infection. Post-herpetic neuralgia can persist for months or years, and the skin may remain hypersensitive to touch.
Poliomyelitis
Poliomyelitis is an acute infectious disease caused by one of the three poliomyelitis viruses, which generally enter the body through the mouth or nose, multiply in the bloodstream and travel to the central nervous system. The viruses are then spread along neural pathways and destroy cells in the anterior horns of the spinal cord. The brainstem may also be damaged. The incidence of acute anterior poliomyelitis has decreased dramatically in the western world since the introduction of vaccination in 1955.
The virus may cause only a minor illness, or there may be signs and symptoms of viral meningitis and paralysis. The extent of paralysis depends on the location of the affected neurons. The initial manifestations of paralytic poliomyelitis include pyrexia, headaches, vomiting, irritability and pains in the neck, back, arms and legs. About 5–7 days after onset, the individual experiences weakness of various muscles, paraesthesia, hypersensitivity to touch and resistance to neck flexion. If the disease affects the brainstem, the muscles involved in swallowing, chewing and ventilation are affected.
Neoplastic and obstructive disorders
Tumours of the nervous system may be benign or malignant, and primary or metastatic. Tumours may arise in the brain tissue, the meninges, the skull, in the peripheral and cranial nerves or in the spinal cord. Brain tissue (cerebral) tumours include astrocytomas and glioblastomas. Meningiomas usually arise from the arachnoid layer of the meninges and do not invade the brain. Skull tumours, which are rare, may be either osteomas (benign) or sarcomas (malignant). Peripheral and cranial nerve tumours include acoustic neuromas, schwannomas and neuroblastomas. Spinal cord tumours may be either extradural or intradural.
Manifestations of nervous system tumours are related to invasion or compression of surrounding neural structures. Brain tumours may produce symptoms as a consequence of increased intracranial pressure; for example, from cerebral oedema. The neurological manifestations of a brain tumour depend on the location of the tumour and its rate of growth. The clinical features associated with a brain tumour include headaches, vomiting, papilloedema (swelling of the optic disc and distension of the retinal vessels), personality or behavioural changes, seizures, visual or hearing defects, dizziness, ataxia and hemiparesis. Manifestations of spinal cord tumours are related to spinal cord compression and include pain, paraplegia or quadriplegia, which may be slowly progressive or acute.
Traumatic disorders
Despite being well protected by bone, meninges and CSF, the brain and spinal cord are frequently injured. Serious cerebral or spinal cord damage can result from a variety of factors such as motor vehicle accidents, sports accidents and penetrating injuries such as gunshot wounds. Cerebral injury may be classified as concussion, contusion, laceration, haematomas and tentorial herniation.
Concussion
Concussion results from a blow to the head and is characterised by a loss of consciousness for less than 5 minutes and memory loss of events preceding and following the injury. Other features include headaches, confusion, dizziness, visual disturbances, vomiting and irritability.
Contusion
Contusion is bruising of the brain that disrupts normal nerve function in the bruised area and which may be associated with haemorrhage or oedema. Manifestations include drowsiness, confusion, behavioural changes, loss of consciousness, hemiparesis, unequal pupil response and decorticate or decerebrate posturing. With decorticate posturing the individual demonstrates hyperflexion of the upper extremities and hyperextension of the lower extremities (Fig 33.10A). With decerebrate posturing, both the upper and lower extremities are hyper-extended (Fig 33.10B).
Laceration
Laceration is tearing of the brain tissue, followed by intracerebral bleeding. Manifestations include prolonged unconsciousness, immediate neurological deficits and deterioration of the individual’s condition.
Haematomas
Haematomas are collections of coagulated blood and, in the brain, may be epidural, subdural or intracerebral. An epidural haematoma results from haemorrhage in the epidural space between the skull and the dura mater. A subdural haematoma results from an accumulation of blood in the subdural space, between the arachnoid and dura mater. An intracerebral haematoma is a collection of blood within the brain tissue.
Manifestations of cerebral haematomas vary according to the location and whether the haematoma develops rapidly or slowly. Typically an epidural haematoma causes immediate loss of consciousness, followed by a lucid interval that eventually gives way to a rapidly progressive decrease in the level of consciousness. Accompanying features include hemiparesis, severe headaches, unilateral pupil dilation and signs of increased intracranial pressure (decreasing pulse and ventilation rate, increasing systolic blood pressure). Manifestations of a subdural haematoma may not occur until days after the injury. Common features include headaches, drowsiness, confusion, slow responses and seizures. Pupillary changes and motor deficits commonly occur. Manifestations of intracerebral haematoma include neck rigidity, photophobia, nausea and vomiting, dizziness, decreased ventilation rate and seizures.
Cerebral herniation
Increased pressure in the cranial cavity can cause damage to the brain through hypoxia, ischaemia and infarction. Unrelieved or untreated raised pressure results in cerebral herniation. When pressure builds up in one area of the brain, brain tissue will begin to move into an area of lower pressure.
Tentorial herniation occurs when part of the temporal lobe herniates through the tentorial hiatus. Typical signs of this form of herniation are pupil dilation and hemiplegia.
Tonsillar herniation or ‘coning’ occurs when part of the cerebellum and/or brainstem herniates through the foramen magnum. Typical signs of this type of herniation are neck rigidity, dysfunction of the cardiac and respiratory drive and abnormal posturing. Irreversible brain damage and death can occur rapidly.
Spinal cord damage
Spinal cord damage may occur from traumatic injuries as a result of motor vehicle or sports accidents, gunshot or stab wounds or falls from high places. Fractures and dislocations can occur anywhere along the spinal column and, if the spinal cord is injured, may result in temporary or permanent damage.
Peripheral nerve damage
Peripheral nerve damage can result from pressure, compression, constriction or traction on a nerve, or as a consequence of skeletal fractures, lacerations or penetrating wounds. Nerve damage can also result from an injection of a toxic or metabolic substance into the nerve. The peripheral nerves most commonly injured are the radial, axillary and ulnar nerves and the brachial plexus. Manifestations include loss of motor function, loss of sensation and muscle atrophy. Depending on which nerve is damaged, there may be foot drop, wrist drop, limited range of motion or paralysis.
CARE OF THE CLIENT WITH A NERVOUS SYSTEM DISORDER
Although specific nursing actions and medical management vary depending on the disorder, the main aims of care are to:
• Maintain fluid and nutritional status
• Prevent and manage alterations in elimination
• Promote effective communication
• Prevent complications of immobility
• Provide psychological support
• Provide a suitable environment
Each client presents specific nursing problems for which an individualised nursing care plan must be developed, implemented and evaluated.
Promoting a clear airway
Disorders of the nervous system may affect the client’s ability to breathe normally, to cough effectively or to prevent the tongue from obstructing the airway. Altered levels of consciousness, decreased motor function or disrupted cranial nerve function may impair the client’s ability to maintain a clear airway. To ensure a patent airway the client’s nose, mouth and respiratory tract must be clear, allowing adequate oxygen and carbon dioxide exchange.
• The client should be assisted into a position that will promote effective breathing. A sitting or upright position provides better lung expansion, which improves breathing and lessens the risk of respiratory tract infection
• The client is instructed to take deep breaths hourly and to cough and expectorate mucus frequently. Chest physiotherapy (e.g. percussion) may be necessary to help mobilise secretions
• If the client’s ability to chew and swallow is impaired, care must be taken when food, fluids or oral medications are being consumed
• Suction equipment should be readily available if the client is at risk of choking or unable to expectorate secretions effectively
• Active or passive range-of-motion (ROM) exercises and 2–4-hourly position changes help to mobilise respiratory tract secretions
• An adequate fluid input is provided to keep respiratory tract secretions moist.
• The client should be nursed in a lateral recumbent position to promote drainage of secretions and to prevent the tongue from obstructing the airway. Positioning on alternate sides 2-hourly should be carried out to prevent pooling of secretions in the lungs
• Oronasopharyngeal suction should be performed to keep the upper airway free of accumulated secretions. Mouth and nasal care should be performed 2–4-hourly for the same purpose (information on oronasopharyngeal suctioning is provided in Ch 23)
• Chest percussion and postural drainage may be prescribed to help remove retained secretions, particularly if the cough reflex is impaired
• The individual may require mechanical assistance for adequate ventilation. A tracheostomy or endotracheal tube may be inserted and mechanical ventilation provided (information on tracheostomy care and mechanical ventilation is provided in Ch 23)
• Eye care is essential for the unconscious client. If the client’s corneal reflex is absent, keep the eyes moist with artificial tears and protect the eye with a protective shield. These should be ordered by a medical officer.
Maintaining nutritional and fluid status
A client with a neurological disorder may have deficits that interfere with an adequate intake of food and fluid, such as:
• Altered level of consciousness
• Diminished or absent swallowing or gag reflex
• Inability to feed themself; for example, if there is paralysis of the arm(s)
• Paralysis of the muscles of mastication and/or the tongue
• Loss of appetite due to altered sensory function; for example, sight, smell, taste.
Information on assisting the client to meet nutritional and fluid needs is provided in Chapters 24 and 28. Specific nursing activities to assist the individual with a nervous system disorder include:
• Providing appropriate devices to facilitate the cutting and eating of food
• Ensuring that suction equipment is readily available should it be needed; for example, if the client’s swallowing or gag reflexes are impaired
• Assisting the client who is unable to feed themself
• Placing the food into the unaffected side of the mouth if the client has any facial weakness. If able to feed themself, the client should be advised to feed in this manner
• Preparing food for the client who has motor deficits; for example, cutting meat, spreading butter, pouring fluids
• Redirecting the client’s attention to eating if they become distracted or are unable to concentrate at mealtimes
• Assisting with the care of the client who is being provided with nutrition and fluids by alternative methods; for example, tube feeding or total parenteral nutrition
• Keeping a record of fluid input and output if the client has difficulty in feeding themself or swallowing, or if they are receiving dehydrating medications or intravenous solutions to reduce or prevent increased intracranial pressure.
Preventing and managing alterations in elimination
Many disorders affecting the nervous system can result in constipation, retention of urine or incontinence. Factors that contribute to altered patterns of elimination include loss of sphincter control, diminished awareness of the need to empty the bladder or bowel, altered levels of consciousness and impaired mental status, with resulting incontinence. (Information on the prevention and management of constipation, retention of urine and incontinence is provided in Chapters 29 and 30.)
Promoting effective communication
Disorders of the nervous system may affect the ability of clients to express themselves verbally or non-verbally, and the ability to understand the spoken or written word. (General information on communication can be found in Ch 6.) The ability to communicate may be impaired by factors that include:
• Damage to the speech centres in the brain
• Damage to the temporal lobes, which hinders the perception and interpretation of stimuli
• Damage to the cranial nerves responsible for movement of the lips, tongue, pharynx and larynx
• Limited motor function that hinders non-verbal communication actions (e.g. facial expressions and gestures)
The two major terms used to describe communication deficits are dysphasia (difficulty in communicating), and aphasia (loss of the ability to communicate).
Aphasia
Aphasia is subdivided into three major classifications.
1. Expressive aphasia (Broca’s aphasia): inability to express oneself verbally or in writing. The degree of difficulty can range from mild hesitancy in flow of speech to limitation of expression to ‘yes’ and ‘no’. The ability to understand the spoken and written word remains intact
2. Receptive aphasia (Wernicke’s aphasia): inability to understand the spoken word. Although the client hears the sounds of speech, comprehension of speech is impaired. The client can speak but makes many errors when using words and is often unaware of the imperfect messages. The ability to comprehend the written word is also impaired
3. Global aphasia: a combination of both expressive and receptive aphasia. The client neither understands what they hear or read, nor can they convey their thoughts in speech or writing.
The loss or impairment of the ability to communicate is devastating and frustrating to the client and to their significant others, often resulting in fear and depression. Although the speech therapist will be the key person in the treatment of a client with a communication problem, the nurse must be aware of prescribed therapy so that it can be continued when the speech therapist is not with the client. The nurse should assume a calm, reassuring and supportive manner that conveys a sense of acceptance of the client’s behaviour. Table 33.3 provides guidelines that can be used when working with a client with aphasia.
Table 33.3 Assisting the aphasic client
| Expressive aphasia | Receptive aphasia |
|---|---|
| Stimulate conversation and ask open-ended questions | Speak slowly and distinctly, using a common vocabulary and simple sentences |
| Allow the client time to find the words to express themself | Stand within the client’s line of vision, so that lip movements can be observed |
| Be supportive and accepting as the client deals with the frustration of finding the right words | Use simple gestures as an added cue |
| Accept self-expression (e.g. pointing or gestures) | Repeat or rephrase any instructions if they are not understood |
| Provide charts or books with pictures of common objects so that the client can point when they cannot say the word | Speak in a normal voice |
| Reassure the client that speech skills can be relearned, given time | Divide any tasks into small units, working with the client to accomplish the task |
| Give praise for achievements and progress |
Communication with the unconscious client is very important because, although the client appears to be completely unaware of their environment, it is impossible to determine their awareness of any stimulus. Many clients have recovered from unconsciousness and given accurate details of events or conversations that took place in their presence while they were unconscious. Therefore the nurse should assume that some stimuli will penetrate the complexities of unconsciousness. Stimuli can be provided by talking to the client, by touch and by playing a radio or CDs. The client should be told what the nurse will be doing—orient the client to time, place and person and describe the surroundings. Coma arousal is a technique whereby the unconscious individual is continuously exposed to a variety of stimuli, such as sounds, touch and smells in an attempt to increase the level of consciousness.
Promoting safety
The client with a nervous system disorder is often susceptible to injury because of factors such as impaired consciousness or awareness, reduced mobility, impaired motor and sensory functions and reflexes. The client is most at risk of skin breakdown, physical injuries or infection.
Maintaining skin integrity
The nurse should assess the client for potential skin problems and implement nursing measures to prevent skin breakdown from pressure, extremes of temperature, and physical trauma, as follows:
• The skin is kept clean and dried to prevent irritation and possible breakdown. Very dry skin should be lubricated with a suitable oil or cream to prevent cracking and breakdown
• A protective cream or lotion may be applied to the genital area and buttocks if the client is incontinent. Wet or soiled linen must be replaced immediately
• The client’s position is changed every 2–4 hours to protect the skin from irritation and prolonged pressure. Pressure-relieving aids may be used
• The skin is assessed every 2 hours for colour, temperature, dryness and the signs of impaired circulation. Any signs of skin breakdown are reported immediately so that appropriate actions can be implemented to prevent further deterioration
• Precautions must be taken to avoid injury to the skin by hot, cold, sharp or rough objects. The client is always moved correctly and gently to avoid damage to the skin.
Preventing physical injuries
A client who has impaired motor, sensory or intellectual function must be protected from accidents and injuries. Protective measures include:
• Maintaining the bed in a low position when not providing direct care at the bedside
• Using alarms that are triggered when the client attempts unsafe activities (e.g. standing from chair unaccompanied)
• Accompanying the client when ambulating if they are unsteady or disoriented
• Providing walking aids and handrails as a means of support and to promote greater safety
• Providing an uncluttered environment and adequate lighting
• Placing the client’s requirements, including the call bell, within reach
• Supervising clients who are at risk of falling while performing the activities of daily living.
Preventing infection
A client with a nervous system disorder that impairs mobility, motor function or level of consciousness is prone to infection. When a person is ill, the body’s natural defence mechanisms are stressed and therefore less able than usual to resist the invasion of pathogenic microorganisms. The two most common types of infection that may occur are urinary tract infection due to urinary stasis or catheterisation, and respiratory tract infection resulting from inadequate lung expansion, pooling of secretions in the lungs, the presence of an artificial airway or mechanical ventilation.
Measures to prevent a urinary tract infection include ensuring that:
• The client receives an adequate fluid input
• Whenever possible, an external urinary drainage device or intermittent catheterisation is used rather than an indwelling catheter
• If an indwelling catheter is unavoidable, measures to prevent cross-infection are implemented. These measures include maintaining a sterile closed drainage system, performing meatal and perineal care, maintaining dependent drainage, maintaining strict aseptic care and using correct handwashing technique, which is the most effective way of preventing cross infection. (Further information on maintaining an indwelling catheter is provided in Ch 29.)
Measures to prevent a respiratory tract infection include ensuring that:
• When possible, the client is nursed in a sitting or upright position to promote maximal lung expansion
• The client performs 4-hourly deep breathing and coughing exercises
• If necessary, suction is used to remove oral and nasopharyngeal secretions
• Aseptic techniques are implemented when caring for an artificial airway.
Promoting mobility and preventing the complications of immobility
Many nervous system disorders impair physical mobility through motor deficits, cerebellar dysfunction, alterations in sensory perception and changes in conscious or mental status. Prolonged lack of physical exercise and movement can lead to many complications, including pulmonary stasis, urinary stasis, venous stasis, decubitus ulcers, constipation and contractures. Impaired mobility varies from reductions in range of motion, or unsteady gait, to total immobility. Maintaining muscle tone and preventing orthopaedic disabilities are of prime importance when caring for a client with impaired mobility.
• Active or passive range-of-motion exercises should be performed every 4 hours
• The client should be repositioned every 2 hours to maintain correct body alignment. Weak or paralysed body parts must be carefully positioned to prevent deformity. Limb splints are often used to maintain joints in normal anatomical position. These must be checked regularly to detect any areas of pressure
• Specific exercises, such as lifting hand weights, may be prescribed to strengthen a weakened limb
• As soon as the client’s condition permits, balancing and sitting exercises are implemented. If the client has been immobile for a prolonged period it is necessary to progress slowly to prevent orthostatic hypotension
• Once the client is able to balance and sit, transfer activities are started; for example, from bed to chair
• When the client is able to stand and balance in an upright position, ambulation is started
• For the client who is unable to ambulate, wheelchair mobility may be achieved.
The client’s age, severity of illness, other neurological deficits, chronic conditions or complications contribute to progress. Client attitude and motivation are also important factors in regaining mobility. Frequent assessment provides evaluation of the client’s needs so that rehabilitation can progress towards the greatest level of independence. More information on preventing the complications of immobility is provided in Chapter 26.
Providing psychological support
Many clients who have a nervous system disorder will suffer neurological deficits resulting in loss of independence, mobility, sensory function or speech. As a result, the client’s body image and self-concept may be greatly altered and they may experience emotional lability, depression, anxiety, frustration or hostility. The client may undergo personality changes, which may be functional or organic in origin. They may require a lengthy period to regain what were once automatically performed skills involved in the activities of daily living, or they may have to come to terms with the realisation that some skills may never be regained. The emotional shock to a client who experiences paralysis can be devastating. The nurse has an important role in providing emotional and psychological support for the client and their significant others. Some of the key aspects related to supporting the client are as follows:
• During the period of dependence, it is important that dignity is preserved. Sensitivity is needed when dealing with any problems associated with loss of control (e.g. incontinence or loss of social restraint)
• Positive feedback should be provided for accomplishments no matter how minor they may appear
• Adequate information about the disease process and its management should be provided, and the client should be encouraged to participate in decision making regarding care
• Client needs should be anticipated to decrease frustration. As much self-care as practicable should be allowed, as a return to independence is the ultimate goal of care. The client’s significant others should be allowed to be involved in care, if they so wish
• The client and their significant others should be encouraged to express their feelings and anxieties. If the client is experiencing a communication problem, appropriate methods of communicating should be developed. Time, patience and understanding are necessary to allow them to come to terms with the effects and implications of the disease
• The client should be encouraged to participate in activities of interest that will help to promote a feeling of self-worth. The occupational therapist and physiotherapist generally assist the client to find activities that interest them and that will also provide exercise for weak or paralysed muscles.
Providing a suitable environment
The immediate physical environment should be adapted to meet the client’s specific needs. Items should be arranged to promote safety; for example, adequate lighting, the call bell within easy reach and the bed adjusted to a suitable height. If the person is experiencing sensory deprivation (a lack of sensory input from the environment), the nurse can provide multi-sensory stimuli. Sensory input can be provided by talking to the person, playing a radio or recordings of the voices of the client’s significant others, by touch and by reality orientation. Reality orientation is a process of making the client aware of their environment, for example, the date, time, people, place and objects.
Conversely, the client may experience sensory overload, particularly if critically ill and the condition requires the use of equipment such as a mechanical ventilation or cardiac monitor, or if they are receiving the constant stimuli of nursing care. Sensory overload occurs when sustained multisensory experiences are perceived as confusing or irritating by the client. The manifestations of sensory overload are confusion, disorientation, restlessness, agitation, panic and possible hallucinations. Every effort should be made to control and moderate the intensity of stimuli, for example, reducing tactile and environmental stimuli.
When the client is to be discharged from hospital, the physical home environment should be evaluated and the delivery of any necessary equipment arranged so that the activities of daily living can be accomplished and independence maintained. The physiotherapist and occupational therapist arrange for the home use of ambulatory equipment and identify special needs and alterations in the client’s environment that could be beneficial to support their independence.
Providing diagnostic test care
Preparation of the client for, and care after, diagnostic tests is part of the nurse’s role. The nurse must refer to the healthcare institution’s policy manual for information about preparation of the individual for specific diagnostic tests. Preparation includes a general explanation of the procedure to reinforce the information provided to the client by the medical officer. Other preparation may include dietary or fluid restrictions, administration of prescribed medications, assisting the client into a specific position, skin preparation and measurement of baseline vital and neurological signs.
Postprocedural care may include assessing vital and neurological signs, measuring and recording fluid input and output, administering prescribed medications and assessing the client for signs and symptoms such as headaches, back pain, neck rigidity, nausea or vomiting, elevated temperature or voiding difficulty.
Promoting rehabilitation and independence
Rehabilitation is an integral part of care and is a dynamic process in which the client is assisted to achieve optimal potential. Throughout the client’s illness, all care is directed towards the maintenance of optimal function and prevention of complications to promote as much independence as possible. Rehabilitation of a client with a nervous system disorder includes helping with relearning the activities of daily living, management of neuromuscular and impaired perception and communication deficits, bladder and bowel retraining and educating the client and their significant others in preparation for discharge from hospital. (Information on rehabilitation is provided in Ch 38.)
CARE OF THE UNCONSCIOUS CLIENT
Consciousness is defined as a state of awareness of self and the surroundings. Consciousness implies an ability to perceive sensory stimuli and to respond appropriately to them. Unconsciousness is defined as an abnormal state in which the client is unresponsive to sensory stimuli. There are degrees of unconsciousness that vary in length and severity, ranging from a brief episode of unconsciousness in the form of fainting, to a prolonged and deep coma.
Causes of impaired consciousness
Impaired consciousness arises from widespread damage to both cerebral hemispheres or from disruption of the reticular activating system in the upper brainstem. Loss of consciousness may result from a cerebral tumour, abscess, haemorrhage, haematoma, laceration, bruising or ischaemia, or from metabolic processes that depress or interrupt the function of both cerebral hemispheres; for example, hypoxia, hypoglycaemia or toxic agents.
Outcome of unconsciousness
The ultimate outcome of unconsciousness varies from full recovery of brain function, through a wide range of disabilities, to irreversible coma and death. The development of sophisticated monitoring techniques and life-support systems has increased the survival rate for comatose clients with severe brain damage. A small percentage of clients emerge from deep coma to a state of wakefulness without awareness, never regaining any recognisable mental function.
Persistent vegetative state
Persistent vegetative state is a term used to describe a chronic condition occurring after severe cerebral damage. It is characterised by intact autonomic functions, generally intact reflexes, presence of a sleep–wakefulness cycle, spontaneous eye opening to verbal stimuli, no localising motor responses to verbal stimuli and no intact cognitive functions or awareness of self or of the environment.
Brain death
Brain death is a state of irreversible brain damage characterised by absence of cognitive functions and awareness of self and the environment, inability to maintain vital functions and the absence of isoelectric activity on EEG. In brain death (or brainstem death) the higher cortical functions cease, consciousness and awareness are lost, as is voluntary control of movement and all brainstem function. Some functions are not completely dependent on the integrity of the brainstem; for example, heart rate continues, though this is usually for a limited time as the client requires ventilatory support. If brainstem function can be shown to have ceased, then there is no prospect of recovery. The basic criteria for diagnosing brain death usually include:
• No motor response in cranial nerve distribution
• No respiratory response to hypercapnia
• Absence of brainstem reflexes
Before considering a brain death diagnosis there is a need to exclude that brain dysfunction is the result of structural or metabolic disease, rather than the result of depressant drugs, alcohol, poisoning or hypothermia.
Brain death is a controversial legal, ethical and medical dilemma, but it is considered ethical and legal to terminate life support in clients diagnosed as brain dead.
Management of an unconscious client
When a client is unconscious a high standard of care must be provided, with the objectives of maintaining and restoring body function and preventing complications. Medical management involves establishing a patent airway and providing adequate ventilation, controlling intracranial pressure and establishing the cause of unconsciousness and, if possible, reversing it. Nursing care of the unconscious client requires the following practices.
Maintaining a patent airway
With the absence of cough and swallowing reflexes, secretions accumulate in the posterior pharynx and upper trachea. An oral artificial airway may be sufficient to maintain patency, or tracheostomy or endotracheal intubation and mechanical ventilation may be necessary. To prevent airway obstruction:
• The client is positioned on alternate sides every 2–4 hours to prevent secretions accumulating in the airways on one side. The neck should be maintained in a neutral position
• Dentures and partial plates are removed
• Nasal and oral care is provided to keep the upper airway free of accumulated secretions and debris
• Oronasopharyngeal suction equipment may be necessary to aspirate secretions
• Chest percussion and postural drainage may be prescribed to assist in the removal of tenacious secretions.
Monitoring neurological function
The client’s neurological signs are monitored at intervals determined by their condition. The results are documented and compared with previous assessments. Information on assessment of neurological function is provided earlier in this chapter.
Positioning
The client is generally nursed in a lateral position with a small pillow placed under the head and neck to maintain the head in a neutral position. The upper arm is positioned on a pillow to maintain the shoulder in alignment, and the upper leg is supported on a pillow to maintain alignment of the hip. The client’s position is changed so that they lie on alternate sides every 2–4 hours. If hemiplegia is present the client may be positioned on the affected side for brief periods, but care must be taken to prevent injury to soft tissue and nerves, oedema or disruption of the blood supply. Because vasomotor tone is decreased in the affected areas, such adverse effects can develop rapidly from improper positioning. If the correct position is maintained, secretions are able to drain from the client’s mouth, the tongue is less likely to obstruct the airway and postural deformities can be prevented.
Meeting hygiene needs
Care of the skin involves keeping it clean and dry and protected from damage. Areas of the skin, particularly over the bony prominences, should be assessed regularly for the signs of impaired blood circulation and irritation that contribute to the formation of decubitus ulcers. Dry skin may be lubricated with a suitable cream or lotion to prevent cracking and breakdown, and a water-repellent substance may be used to protect the skin against excreta or perspiration. The male should receive a facial shave as part of his daily hygiene care; the client’s nails are kept short and clean; and the hair is brushed, combed and washed as necessary.
Care of the mouth involves cleansing all areas at 2–4-hourly intervals to prevent a build-up of plaque, development of caries and development of a focus of infection. To prevent aspiration of fluid while oral hygiene is being performed, the client’s head is turned to one side and suction equipment made available throughout the procedure. The lips are lubricated with a suitable water-based substance.
Care of the nose involves cleansing the nostrils to keep them free of dried mucus. Cottonwool-tipped applicators and saline solution may be used to remove mucus and dried crusts, and a thin coating of cream may be applied to the rim of the nostrils.
Care of the eyes involves swabbing the eyes with moistened cotton wool to remove secretions, the instillation of artificial tears (or antibiotic eye drops if prescribed) and protecting the eyes from corneal abrasions. If the eyelids do not close fully, the use of eye shields or pads may be necessary to protect the corneas. (See Ch 32 for more information on care of the eye.)
Meeting nutritional and fluid needs
The nutritional and fluid needs of the client must be regularly assessed and met to maintain body function, support tissue repair and combat infection. The dietitian prescribes a nutritional program based on consideration of the individual’s energy needs, requirements for tissue repair, loss of fluid and basic life functions. Methods of administering nutritional and fluid support to the unconscious client include total parenteral nutrition, and enteral feedings administered via a nasogastric, nasojejunal or gastrostomy tube. Parenteral nutrition is only used if there is a long-term gut absorption problem, as the aim is to normalise gut function as soon as possible. Fluid input may be restricted to a specific amount of fluid in a 24-hour period. The purpose of fluid restriction is to control increased intracranial pressure by keeping the client slightly under-hydrated. As fluid input is correlated with output, an accurate input and output record must be maintained.
Meeting elimination needs
Because an unconscious client is incontinent, an external urinary drainage appliance or an indwelling catheter (IDC) may be used to manage urinary drainage. Both methods are used to keep the skin dry, as urinary incontinence can quickly lead to skin breakdown. Urinary drainage devices also enable accurate calculation of urinary output. Long-term IDC is avoided whenever possible due to risk of infection. Frequent checks and meticulous skin care is preferable. (Information on care of the client with a urinary drainage device is provided in Ch 29.)
Constipation and faecal impaction are common complications in an unconscious client because immobility and lack of a normal diet inhibit peristalsis. A program is established whereby aperients and rectal suppositories are administered to promote regular bowel evacuation. The frequency of bowel actions and the amount and nature of the faeces are documented (see Ch 30).
Promoting safety
Providing and maintaining a safe environment is of prime importance because an unconscious client is unable to perceive or react to safety hazards. Clinical Interest Box 33.5 suggests alternative routes for measuring temperature when a client is in a state of altered consciousness.
CLINICAL INTEREST BOX 33.5 Altered consciousness and taking temperature
Temperature should never be taken orally in clients with altered conscious state. For an oral temperature reading to be taken safely and accurately, the client must be able to close their lips completely and understand the importance of not biting the thermometer. Measure temperature via the tympanic or axillary routes; of these, tympanic is more accurate and therefore preferred.
Preventing complications
Because the unconscious client is not mobile, they are at risk of developing any of the complications associated with immobility (muscle contractures, decubitus ulcers or venous, pulmonary or urinary stasis). Information on preventing these complications is provided in Chapter 26.
Providing sensory stimulation
The extent to which an unconscious client may be aware of what is happening to and around them cannot usually be determined; the nurse should therefore assume that the brain is receiving some sensory input. When the duration of coma extends into weeks or months, it may seem meaningless to keep explaining each activity to a client who gives no sign of comprehension. However, on regaining consciousness some clients have been able to describe accurately events that happened to and around them while they were unconscious. Although they were unable to communicate their feelings they were able to discriminate between the gentle caring manner of some people and the inattentive ways of others. Some clients have reported that they longed for someone to talk to them rather than about them.
The nurse should therefore act as though the client is conscious and demonstrate respect for them as a person. All activities should be explained to them, privacy during procedures should be ensured and they should be treated with dignity. Family members and friends should be encouraged to talk to and touch the unconscious client. They should be encouraged to perform certain activities for the client, such as combing the hair or applying skin lotion. Other sensory stimuli can be provided by playing a radio or CDs, or by placing perfumed flowers in the room.
Recovery from unconsciousness is a gradual process that tends to vary with each individual. Rehabilitation after a prolonged period of unconsciousness includes protecting the client from orthostatic hypotension. When able to tolerate a vertical position, an ambulation program is developed, unless neurological deficits make it infeasible. (Information on rehabilitation nursing is provided in Ch 38.)
Management of the client with impaired motor function
Disturbance of motor function is common among clients who experience disorders of the brain, spinal cord or peripheral nerves, such as cerebral haemorrhage, spinal cord injury or peripheral neuritis. While this chapter addresses the care of a client who has experienced a stroke or a spinal cord injury, the principles of care can be applied to clients who experience impaired motor function from other causes. Some terms relating to impaired motor function are:
• Paresis: incomplete paralysis or muscle weakness
• Paralysis: loss or impairment of the ability to move part(s) of the body. Paralysis may be complete or incomplete, spastic or flaccid, symmetric or asymmetric, temporary or permanent
• Hemiplegia: unilateral paralysis, or paralysis of one side of the body. Because nerves cross in the pyramidal tract before descending to the spinal cord, damage to one side of the brain causes hemiplegia on the opposite side of the body
• Paraplegia: paralysis of the lower limbs and, sometimes, paralysis of the lower trunk and sphincters. Paralysis may be complete or incomplete, spastic or flaccid, temporary or permanent
• Quadriplegia (tetraplegia): paralysis of the arms and legs and of the body below the level of injury to the spinal cord.
Stroke
A stroke, also known as a cerebrovascular accident (stroke) or brain attack, is one of the leading causes of death in the western world, and each year many thousands of clients survive a stroke but are left with permanent disabilities. A stroke is a sudden impairment of cerebral circulation, which causes cerebral infarction. The two types of stroke are ischaemic and haemorrhagic. In an ischaemic stoke, cerebral blood flow is suddenly impaired by a thrombus or embolus. In a haemorrhagic stroke, the rupture of a cerebral blood vessel causes bleeding into the subarachnoid space or brain tissue.
Manifestations of a stroke vary depending on the artery involved, and consequently the area of brain it supplies, and the severity of damage to cerebral tissue.
Table 33.4 lists the clinical features resulting from specific cerebral artery occlusion or rupture. If the stroke occurs in the left hemisphere, it produces symptoms on the right side of the body. If it occurs in the right hemisphere, the left side of the body is affected.
Table 33.4 Manifestations of cerebrovascular accidents according to vessel involved
A thrombotic stroke, the most common type, is associated with atherosclerosis, which causes narrowing of the lumen of arteries. A thrombus forms in one of the cerebral arteries, occluding the vessel and resulting in cerebral ischaemia. An embolic stroke occurs when an embolus, which may be part of a thrombus, fat or other substance, is carried to the brain and occludes a cerebral blood vessel. A haemorrhagic stroke, which is often associated with hypertension, occurs when a cerebral blood vessel ruptures, spilling blood into the brain tissue. Rupture of an artery may result from a degenerative change in the arterial wall, or from an anatomical defect such as an aneurysm.
Clinical Scenario Box 33.1
Gary is a 45-year old-male. He presented to the emergency department after a fall from a first floor window last night. He had been out drinking at a work function and had forgotten his house keys. His wife called an ambulance this morning as Gary was very agitated and appeared to have a weakness in his left arm and leg. She also noticed some blood loss on the pillow from a gash on Gary’s head.
Risk factors
Educational programs have been developed to inform the general public about stroke and prevention. Many factors have been identified as predisposing a person to a stroke and, by increasing public awareness, those at risk can seek medical advice to have any preexisting conditions managed, thus reducing the risk of stroke. Risk factors include:
Manifestations of a stroke
In all cases of stroke, areas of the brain are deprived of an adequate oxygen supply. If the blood supply is impaired for an extended period, the involved cerebral tissue may become necrotic, resulting in permanent neurological deficits. In instances of ischaemia, temporary neurological impairment may result. The particular type and degree of neurological deficits depend on the area of the brain involved (see Table 33.4). Table 33.5 lists a comparison of manifestations associated with right- and left-sided hemiplegia.
Table 33.5 Manifestations of stroke
| Left-sided stroke | Right-sided stroke |
|---|---|
| Right-sided hemiplegia (left stroke) | Left-sided hemiplegia (right stroke) |
| Aphasia—expressive, receptive or global | Spatial–perceptual defcits |
| Intellectual impairment | Tends to be distractible; impulsive behaviour |
| Slow behaviour | Appears to be unaware of defcits; poor judgment |
| Defects in right visual felds | Defects in left visual felds |
Care of the client who has had a stroke
Medical management involves control of cerebral oedema and subsequent increased intracranial pressure, surgical intervention if indicated and drug therapy; for example, thrombolytic medication such as tissue plasminogen activator (TPA) may be given to clients experiencing a non-haemorrhagic stroke. Nursing care of the client involves:
Care during the acute phase
The acute phase begins when the client is admitted, and continues until their condition is stable. Nursing care is directed towards maintaining a patent airway and monitoring vital and neurological signs.
Maintaining a patent airway. This involves positioning the client on their side, administering oxygen as prescribed and suctioning secretions from the airway. Care must be taken when performing oronasopharyngeal suction, as suction applied for longer than 15 seconds at a time may increase intracranial pressure.
Recording fluid input and output. This information should be kept to monitor kidney function and to evaluate fluid and electrolyte balance.
Vital and neurological signs. These signs should be assessed frequently, for example every 15–30 minutes, to detect changes in the client’s condition. Information on neurological assessment is provided earlier in this chapter. If the client is unconscious, the principles of care described previously should be incorporated.
Care after the acute phase
Detailed information about the nursing measures necessary to meet the client’s basic needs for hygiene, safety, elimination, nutrition and fluids, psychological support, mobility and rehabilitation are provided elsewhere in this text. Clinical Interest Box 33.6 provides some suggestions which can facilitate self-care after stroke.
CLINICAL INTEREST BOX 33.6 Devices to facilitate self-care after stroke
The following list identifies useful items that may assist neurologically impaired clients to perform self-care more easily and safely after a stroke or other disorders.
• Plate guards to prevent food from being pushed off plate
The main aims of care for a client who has experienced a stroke are to:
• Assist in meeting hygiene needs
• Monitor vital and neurological signs
• Maintain muscle tone and prevent contractures
• Prevent venous stasis (thrombus and embolus formation)
• Prevent and manage alterations in elimination (e.g. incontinence, retention of urine, constipation)
• Maintain nutritional and fluid status
• Establish an adequate means of communication
• Promote reorientation of a confused client
• Enhance self-concept and body image
• Institute a rehabilitation program aimed at achieving an optimal level of independence.
Rehabilitation
Rehabilitation of the client begins on admission to hospital and continues for as long as necessary including after discharge home. In some healthcare institutions the client may be transferred to a rehabilitation unit after the acute phase of their illness. The focus of rehabilitation is directed at helping the client to relearn lost skills and to become as independent as possible. The client and their significant others are made aware of the plan and goals of the rehabilitative phase, and their active participation is encouraged. Recovery from a stroke is a slow process; therefore the nurse must provide support and positive feedback so that the client does not become discouraged. Rehabilitation of the client includes:
• Encouraging participation in their own care as much as possible
• Teaching them to perform the activities of daily living with regard to ways of compensating for any disabilities
• Teaching and assisting with performance of transfer activities (e.g. bed to chair)
• Assisting in the regaining of any lost communication skills
• Encouraging expression of feelings, to decrease anxiety and to allow for correction of any misunderstood information
• Developing a bladder and bowel retraining program (if necessary).
More information on rehabilitation nursing is provided in Chapter 38.
Planning for discharge
Discharge planning is directed at facilitating the transition from the healthcare institution to the home environment. Discharge planning involves assessing the client and the family, identifying specific needs, planning to implement ways of meeting those needs and evaluating the discharge process and the results. After the client is discharged home, they and the family must have contact with support services, such as the district nurse, whom they can rely on for continued help and support.
Spinal cord injury
Injuries involving the spinal cord result most often from motor vehicle accidents, falls, sporting and industrial accidents and firearm or stab wounds. Injuries to the vertebral column and spinal cord result from forces applied directly or indirectly to the head, neck or trunk. Apart from direct tearing of the spinal cord, the main damage is caused by haemorrhage, oedema and disruption of the blood supply to the cord. Additional compression can result if bony fragments or disc material press on the spinal cord.
Manifestations of spinal cord damage depend on the degree and site of the injury. Complete spinal cord transection causes a total loss of motor and sensory function below the level of injury. With cervical cord transection there is paralysis of all four extremities (quadriplegia/tetraplegia). There are varying degrees of arm and ventilatory paralysis, depending on the injury level. With thoracic cord transection, down to the level of the second lumbar vertebra, there is paralysis of the lower extremities (paraplegia). There is often some loss of intercostal muscle function and loss of bladder and bowel function. With transection in the region of lumbar vertebrae there is loss of a combination of sensory, motor, bowel and bladder function.
Complete cord transection results in immediate flaccid paralysis, loss of sensation and loss of reflexes below the level of injury. As paralysis subsides, reflexes usually return and flaccidity changes to involuntary spastic movements. Recovery of any motor or sensory function is rare when there has been complete paralysis of these functions for several days. With incomplete spinal-cord injuries, degrees of motor and sensory deficit below the level of damage vary. The client may experience temporary paralysis, with function returning when any oedema subsides.
Clinical Scenario Box 33.2
Mr Ken Nyugen is a 56-year-old male who has been admitted to the acute medical ward with an ischaemic stroke. He initially presented by ambulance after being found slumped in a chair at home by his daughter. On initial presentation to the emergency department the following assessment data was obtained:
HR 50 regular (12 lead ECG RBBB—old)
SpO2 92% RA—coarse crackles right lower lobe
• Detail how you would perform your physical assessment of the client.
• What risk factors does Mr Nguyen have in relation to his stroke and how do the risk factors contribute to stroke?
• What are some indications of dysphagia?
• What is your management plan for Mr Nguyen? What medical interventions will be required?
Damage to the spinal cord and nerve roots results from:
• Compression by displaced bone or ligaments, extruded disc or haematoma formation
• Excessive stretching, crushing, shearing or severance of neural tissue
There are four possible vectors (forces) that can be applied to the spinal column to cause injury:
1. Flexion: excessive flexion (hyperflexion) tends to produce compression of the vertebral bodies, with disruption of the posterior ligaments and the intervertebral discs. Hyperflexion injuries are caused by hyperflexion of the head and neck, as in sudden deceleration of a vehicle
2. Extension: excessive extension (hyperextension) usually causes fractures of the posterior elements of the vertebral column and disruption of the anterior ligaments. Hyperextension injuries are caused by hyperextension of the head and neck, as may occur in a rear-end vehicular accident
3. Rotation (lateral flexion): excessive rotation is most likely to produce rupture of the ligaments, fracture and fracture dislocation of the vertebral facets. Rotational injuries are caused by extreme lateral flexion or rotation of the head and neck
4. Compression: compression can result in fractures of the vertebral body and arch, and rupture of the supporting ligaments. Compression injuries are caused by vertical pressure as occurs when a person falls from a height and lands on their feet or buttocks.
Classification of spinal cord injuries
Spinal cord injuries can be classified by the type of injury and by syndromes:
• Concussion: severe shaking of the spinal cord that causes temporary loss of function lasting about 24–48 hours
• Contusion: bruising of the spinal cord, which includes bleeding into the cord
• Laceration: an actual tear in the spinal cord
• Transection: severing of the cord—may be complete or incomplete
• Haemorrhage: bleeding into or around the cord. Escaped blood is an irritant to the delicate tissue
• Anterior cord syndrome: due to injury of the anterior part of the spinal cord and associated with flexion injuries and fracture dislocations of the vertebrae. Manifestations include loss of pain and temperature sensation and motor function below the level of the injury. The sensations of light touch, position and vibration remain intact
• Posterior cord syndrome: a rare syndrome in which the senses of position and vibration are involved
• Central cord syndrome: due to injury and/or oedema to the central cord in the cervical region (e.g. as a result of hyperextension injuries). Manifestations include a greater loss of motor function in the upper limbs (rather than the lower), bladder dysfunction and varying degrees of sensory impairment
• Brown-Séquard syndrome: results from open penetrating wounds that produce transverse hemisection of the cord. Manifestations include loss of pain and temperature sensation on the side opposite the injury, and loss of motor function, light touch, position and vibratory sensation on the side of the injury.
Manifestations of spinal cord injury
Generally, the degree of damage to the spinal cord at any level is described as incomplete or complete transection. Incomplete transection of the cord produces loss or impairment of sensation and motor function that reflects the specific nerve tracts that have been damaged. Complete transection of the cord results in permanent loss of voluntary movement, sensation, reflex and autonomic function below the level of injury.
Spinal shock
Spinal shock is an immediate response to an acute spinal cord injury and is the temporary suppression of reflexes controlled by the segments below the level of injury. After a period that may vary from hours to months, the spinal neurons gradually regain their excitability. Subsequent return of some function results from decompression of the cord as oedema resolves.
Functional loss from spinal cord injury
The different functions and dysfunctions associated with spinal cord injuries at specific levels are listed in Table 33.6. The effects of spinal cord injury on sexual response vary depending on the level and degree of injury. Sexual function is controlled by spinal levels S2, S3 and S4. Knowledge of the physiology of alterations in sexual response after spinal cord injury is incomplete, and significant individual differences exist. People with complete loss of sensation in the genitalia may still experience orgasm in response to sensations produced by stimulation of other areas of the body in which sensation is intact. Sexual pleasure can also be increased by psychological stimuli, such as memory, sight, sound and odour. Physical stimulation of the genitalia may produce reflex erection of the penis and vaginal lubrication, even though there is no sensory awareness of stimulation.
Care of the client with spinal cord injury
Management of the client at the scene of the accident is critical to the ultimate neurological outcome. The basic objectives of first aid management at the scene are to:
• Prevent further spinal cord damage from torsion, flexion or extension of the unstable spine
• Transport the client rapidly and safely to an appropriate facility.
• Subsequent management of the individual involves emergency department care, early management, post-acute and long-term management.
Initial management
On arrival of the client in the accident and emergency department, the medical officer assesses the client, and x-rays are taken to determine the extent of the injuries. The medical officer develops a plan of care that may include immediate surgery or a non-surgical approach with traction and immobilisation and insertion of a nasogastric tube, indwelling urinary catheter and intravenous infusion. Generally, glucocorticoid steroids are prescribed to reduce cord swelling.
Early management
After initial assessment and stabilisation of the client, they are admitted to the intensive care or spinal unit. A client with less severe injuries may be admitted to a general ward. Medical management will depend on the type of spinal cord injury and any associated injuries. Treatment may be surgical, non-surgical or a combination of both approaches. Surgical management may take the form of decompression laminectomy, fusion of vertebrae, open or closed reduction of fractures or dislocations or the insertion of rods. Non-surgical management involves immobilisation of the spine (Fig 33.11) using skeletal tongs with traction, halo traction, a cervical collar or a device designed to maintain thoracic or lumbar alignment, such as a fibreglass body jacket.
Nursing care of the client with a spinal cord injury
Nursing management will vary according to the client’s injury and whether a surgical or non-surgical approach is selected. However, the major aspects of care are directed towards maintaining respiratory function, immobilisation and alignment of the spine, preventing complications, meeting basic needs, providing psychological support and rehabilitation.
Respiratory care
A client with a spinal cord injury can develop varying degrees of respiratory difficulty, depending on the level of spinal injury. The client will require a plan of care directed at preventing pulmonary complications. Intubation and mechanical ventilation will be required if there is impairment of respiratory muscle function. The program of care includes:
Immobilisation and alignment of the spine
After alignment of the spine has been achieved, immobilisation serves to maintain alignment and promotes healing at the site of injury. For most thoracic, lumbar or sacral injuries the client remains confined to bed, with the back positioned and supported to achieve hyperextension of the spine at the site of injury. A bed with a firm mattress and steel base and correctly positioned pillows are necessary to maintain the prescribed posture.
Skeletal traction
When the injury involves dislocation or fracture-dislocation of the cervical or high thoracic spine, skeletal traction is commonly used to accomplish alignment and immobilisation (see Fig 33.11). Skeletal traction may be achieved by means of cervical tongs, such as Crutchfield tongs, or by the halo device. The halo device may also be incorporated with the use of a body vest or jacket to stabilise the spine, thereby allowing the individual to be ambulatory. When skeletal traction is used, the client may be nursed on a firm mattress and fracture board, or on a special bed such as a Stryker frame.
After skeletal traction has been established, pain is decreased and the client’s comfort is enhanced. Turning can be carried out using a special technique (as described in Ch 21) to allow for skin care and a change of position. Alternatively, a client may be lifted in a Jordan frame for hygiene purposes. Management of the client in cervical skeletal traction includes:
• Checking the traction equipment every 2–4 hours to ensure safety and integrity of the treatment
• Inspecting, cleansing and dressing the pin sites according to the institution’s policy (e.g. every 4–8 hours)
• Changing the client’s position every 2 hours to prevent the complications of immobility. The ‘log-rolling’ technique or the Stryker frame is used to turn the individual to maintain the vertebral column in neutral position
• Using various devices (e.g. pillows, a foot board, a cervical roll) to maintain good body alignment. When the client lies supine, the arms and legs are positioned in extension with support to maintain the feet in dorsiflexion. The hands are placed in a functional position and a cervical roll is used to maintain hyperextension of the neck. When the client is in a lateral position, the arms and legs are positioned in extension, and pillows are placed to support this position.
Preventing complications
Because prolonged immobility can lead to various complications, specific preventive measures must be implemented. (Information on preventing the complications associated with immobility is provided in Ch 26.)
Meeting basic needs
Clients with impaired motor and sensory function require assistance to meet their needs for hygiene, safety, elimination, nutrition and fluids, temperature regulation and pain relief. (Information on assisting clients to meet these basic needs is provided in other chapters.)
Providing psychological support
A severe spinal cord injury has a devastating effect on the client and their significant others, and they will experience a range of emotional responses, from the time of injury and through the rehabilitation process. The client will have to adapt to the loss of motor function and sensory deprivation, both of which severely threaten self-concept and body image. It is important that the nurse is aware of the impact that the injury has on the client’s emotional and psychological equilibrium. The nurse must be sensitive to the emotional and psychological response of the client to the injury, and be supportive as they deal with the impact of the injury. The nurse can help to support the client by:
• Establishing a climate of trust
• Accepting behaviour, without being judgmental
• Encouraging expression of feelings
• Listening empathetically and attentively
• Allowing the client to make decisions and maintain control
• Providing information as necessary
• Supporting a positive self-concept and self-esteem
• Informing the client that it will take time to adjust to the disability.
Promoting rehabilitation
In most instances of spinal cord injury the client will require long-term rehabilitation. Rehabilitation after spinal cord injury is a lifelong process of learning to live with a disability. The client and family together with the healthcare team members contribute to the development of the rehabilitative plans. (Information on rehabilitation is provided in Ch 38.)
Summary
The nervous system is a complex system, responsible for communication within the body and between the body and its environment. It is divided into two primary divisions: the central nervous system and the peripheral nervous system.
Nervous tissue is commonly described as grey and white matter. The grey matter is composed of cells and the white matter is made up of fibres. Neurons are the primary components of nervous tissue, which are bound together by neuroglia. Neurons have two functional properties, irritability and conductivity. This means that neurons are able to respond to a stimulus, convert it into an impulse and transmit the impulse to other neurons, muscles or glands. Impulses are transmitted through spaces, called synapses, between neurons.
The central nervous system consists of the brain and the spinal cord. The brain is a large organ composed of the cerebrum, diencephalon, brainstem and cerebellum. Each part of the brain has specific functions. The spinal cord lies within a canal inside the vertebral column, extending from the base of the skull to the first or second lumbar vertebra. The spinal cord receives sensory impulses, conveys motor impulses and is the centre through which reflex actions take place. The meninges are three membranes that cover the brain and spinal cord to protect them against physical injury. Cerebrospinal fluid is a clear watery fluid produced in the ventricles of the brain, which circulates in the subarachnoid space surrounding the brain and spinal cord. It protects the brain and spinal cord and provides a medium for the exchange of nutrients and waste products.
The peripheral nervous system consists of 12 pairs of cranial nerves and 31 pairs of spinal nerves. The nerves of the peripheral nervous system may be: sensory, carrying impulses to the brain and spinal cord; motor, carrying impulses away from the brain and spinal cord; or mixed. The motor nervous system is divided into somatic and autonomic nervous system divisions. The autonomic nervous system division is composed of the sympathetic nervous system and the parasympathetic nervous system. It is the section of the peripheral nervous system concerned with the involuntary activity of the body. Sympathetic nerves have a stimulating effect on most organs, while parasympathetic nerves tend to slow down body processes.
Normal function of the nervous system may be impaired as a result of congenital disorders, inflammatory or infectious conditions, trauma, neoplasia, degenerative conditions or metabolic and endocrine disorders. The major manifestations of nervous system disorders are headaches, sensory changes, motor changes, reflex changes, altered states of awareness or consciousness and seizures. Disorders of the nervous system can be classified as those occurring from congenital or hereditary defects, from multiple causes, degenerative disorders, immunological disorders, infectious or inflammatory conditions, neoplastic or obstructive disorders and trauma.
Diagnostic tests used to assess nervous system function include the neurological examination, radiographic examination, magnetic resonance imaging and electroencephalography. Care of the individual with a nervous system disorder includes promoting a clear airway, maintaining fluid and nutritional status, preventing and managing alterations in elimination, promoting effective communication, promoting safety, promoting mobility, preventing the complications of immobility, providing psychological support, assessing neurological status, providing a suitable environment and promoting rehabilitation.
1. A 48-year-old man has been brought into the emergency department after a fall on his head at work. He says he was knocked out for about 10 minutes, but now seems alert and orientated. What type of injury is he most likely to have sustained? What discharge instructions would you give this client’s family? How would you modify these instructions if this client lives alone?
2. A 21-year-old client has been admitted to the rehabilitation ward after complete transection of his spinal cord at C7 level, in a motor vehicle accident. What motor and sensory function would you expect the client to have? The client says he is looking forward to learning to use special equipment. Do you think his emotional response is appropriate? How would you respond? What elimination issues may emerge? How would you deal with these?
3. Mr Traynor, 59, has recently been diagnosed with early-stage Parkinson’s disease. Mrs Traynor is quite concerned about the progression of the disease—whether Mr Traynor can still be employed, if he can be left alone for several hours at a time and what medications he will be required to take. How would you respond to her concerns? Is there other information that would be helpful to the Traynors? How can they find more information about Parkinson’s disease?
4. Mr Hong is a 50-year-old police constable. He has been troubled by recurrent atrial fibrillation, and treated with an anticoagulant. Mr Hong was on a ladder cleaning the gutters of his house when he fell and hit his head. Although shaken, after his wife made him a cup of tea and after a short rest, he felt well enough to continue with his task. However, over the next few days, Mrs Hong began noticing several behavioural changes in her husband. He seemed vague and forgetful at times. Finally, when she found him urinating in the freshly set fireplace, he was convinced to seek medical assistance. An MRI showed a subdural haematoma. Mr Hong was booked in for evacuation of the clot via burr holes. His surgery was highly successful and Mrs Hong was most grateful that she could confidently set her fire.
Before surgery, the nurse taking care of Mr Hong made the following nursing diagnoses:
1. What is the function of the peripheral nervous system?
2. What is the function of the autonomic nervous system?
3. What are the major manifestations of nervous system disorders?
4. What are the components of a neurological assessment?
5. What are the main aims of nursing care of the client with a nervous system disorder?
6. What is the nursing management of an unconscious client?
7. What are the types of stroke? What are the risk factors? What are the manifestations?
8. What is the nursing management of a client with spinal cord injury?
References and Recommended Reading
Ankner GM. Case Studies in Medical–Surgical Nursing. Clifton Park, NY: Thomson Delmar Learning, 2007.
Ankner GM. Medical–Surgical Nursing. Clifton Park, NY: Thomson Delmar Learning, 2008.
Berman A, Snyder S, Kozier B, et al. Kozier and Erb’s Fundamentals of Nursing, 2nd edn. Pearson, Frenchs Forest, NSW, 2012.
Brunner LS, Smeltzer SCOC. Brunner & Suddarth’s textbook of medical–surgical nursing. Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins, 2010.
Crisp J, Taylor C. Potter & Perry’s Fundamentals of Nursing, 3rd edn., Sydney: Elsevier, 2009.
Marieb E. Human Anatomy and Physiology, 6th edn. San Francisco: Benjamin Cummings, 2010.
Marieb E. Essentials of Human Anatomy and Physiology, 10th edn. San Francisco: Pearson Benjamin Cummings, 2012.
Marieb E, Hoehn K. Human Anatomy and Physiology, 8th edn. San Francisco: Pearson Benjamin Cummings, 2010.
McCance KL, Huether SE, Brashers VL, et al. Understanding Pathophysiology. Sydney: Elsevier, 2011.
LeMone P, Burke K, Dwyer T, et al. Medical-Surgical Nursing: Critical Thinking in Client Care. Pearson, Frenchs Forest, NSW, 2010.
Lugg J. Recognising and managing Guillain-Barré syndrome. Emergency Nurse. 2010;18(3):27–30.
Neighbors M, Jones R. Human Diseases, 2nd edn. NY: Delmar/Thomson, 2006.
Patton KT, Thibodeau GA. Anatomy and Physiology, 7th edn. Mosby Elsevier, 2010.
Schub T, Caple C, Pravikoff D. Guillain-Barré Syndrome. CINAHL Information Systems, 2011.
Seeley R, Stephens T, Tate P. Anatomy and Physiology, 8th edn. DuBuque, IA: McGraw-Hill, 2008.
Thibodeau GA. Structure and Function of the Body. St Louis: Mosby, 2008.
Waterhouse C. An audit of nurses’ conduct and recording of observations using the Glasgow Coma Scale. British Journal of Neuroscience Nursing. 2008;4(10):492–499.
ABC Online. Health Matters Library, www.abc.net.au/health/library.
Epilepsy Foundation of Victoria, www.epinet.org.au.
Multiple Sclerosis Society of Australia, www.msaustralia.org.au.
National Institute of Neurological Disorders and Stroke, www.ninds.nih.gov.
Parkinson’s Australia website, www.parkinsons.org.au.
Stroke Foundation, www.strokefoundation.com.au.
The Better Health Channel, www.betterhealth.vic.gov.au.